SEED Coagulation. Sysmex Educational Enhancement and Development April 2014
|
|
|
- Matthew Domenic Poole
- 6 years ago
- Views:
Transcription
1 SEED Coagulation Sysmex Educational Enhancement and Development April 2014 The Thrombin Time Test and Reptilase Test what is their role in coagulation testing? Baseline screening tests of coagulation The bulk of prothrombin time (PT) and activated partial thromboplastin time (APTT) test requests worldwide are for the monitoring of anticoagulant therapy. There are however a number of instances where such baseline tests are performed with no indication that a specific haemostatic disorder is present. The main indication for such requests is to evaluate whether a patient who is scheduled to undergo elective surgery or invasive procedure is at risk of bleeding. Screening tests are also the starting point of investigation of patients that present with a clinical history of a suspected bleeding diathesis. In such instances, the thrombin time (TT) and reptilase test (RT) are a valuable adjunct to interpretation of results and for guiding more definitive testing where indicated. The principle of the thrombin time The thrombin time, although not strictly speaking a screening test, is a commonly performed test that is widely available. It is a very simple clot-based test that involves only the addition of exogenous thrombin (the reagent) to platelet poor plasma which triggers the conversion of fibrinogen to fibrin. The thrombin time therefore measures the rate of fibrin clot formation after the addition of a standard amount of thrombin to citrated plasma. The test exclusively measures the conversion of fibrinogen to fibrin. Any prolongation of the thrombin time is therefore directly related to this reaction; either in the form of a fibrinogen abnormality or the presence of any substance that may inhibit this reaction, most notably heparin (Fig. 1). The conversion of fibrinogen to fibrin The addition of thrombin initiates the cleavage of fibrinopeptide A and fibrinopeptide B from the N-terminal ends of the alpha and beta chains of the fibrinogen molecule. This action of thrombin converts fibrinogen into fibrin monomers. These fibrin monomers each of which is comprised of a so-called E-domain and two D-domains align to form fibrin dimers and then polymers. These fibrin polymers in turn are stabilised through the process of cross linkage mediated via activated factor XIII to form an insoluble fibrin clot. This cross linkage takes the form of a covalent bond which irreversibly binds the D-domains of two adjacent fibrin molecules to each other (Fig. 2). The resultant fibrin is insoluble and forms a clot. The time taken for clot formation is recorded as the thrombin time. In health, the process of clot formation is finely balanced with the simultaneous initiation of clot breakdown, socalled fibrinolysis to ensure that the blood vessel lumen is not occluded. The process of fibrinolysis is mediated via the enzyme plasmin which has the ability to cleave both fibrin and fibrinogen into a heterogeneous mixture of so-called fibrin(ogen) degradation products (FDPs). The covalent bond formed between two D-domains is however resistant to plasmin degradation. FDPs containing 2 such D-domains are referred to as D-dimers and are exclusively produced from cross-linked fibrin. Any interference with the polymerisation process will affect the thrombin time.
2 2 Fig. 1 Schematic representation of the clotting pathways highlighting the components that are tested by the thrombin time. Thrombin is excluded as the test is activated by the addition of the test reagent which contains exogenous thrombin. Pink arrows indicate the activation effects of thrombin additional to its conversion of fibrinogen to fibrin. The green arrow indicates the inhibitory effect on thrombin by heparin/antithrombin complex. Fig. 2 Schematic representation of fibrin polymerisation.
3 3 The thrombin time test method The test sample is platelet poor plasma obtained from whole blood which has been collected with citrate as the anticoagulant (the same as for all routine clot-based tests of haemostasis). The test reagent containing thrombin, which can be of human or bovine origin, is added to platelet poor plasma at 37 C. The time taken (in seconds) for the clot to form, is recorded. The test can be performed manually in a water bath or set up on an automated coagulation analyser. Interpretation of thrombin time Normal values for thrombin time are highly dependent on the concentration of thrombin used as well as the clot detection principle of the analyser. The concentration of thrombin is not uniform in commercially available thrombin time reagents, the package inserts of which confirm that the expected values are accordingly different. To illustrate this, published thrombin time reference range values sometimes do not even overlap; for example seconds, in contrast to seconds. Consequently, it is critically important that thrombin time results are interpreted strictly only against local laboratory established reference ranges. A prolonged thrombin time is considered abnormal. If a shortened thrombin time is obtained, the possibility of an activated sample must be excluded before this result is accepted as biologically representative of the patient s clinical status. Causes of prolonged thrombin times These can be divided into 3 broad categories. 1. A problem with fibrinogen 2. Anything interfering with fibrin polymerisation 3. Anything inhibiting the reaction by interfering with thrombin a. Fibrinogen abnormalities i. Quantitative abnormalities As the thrombin time measures the conversion of fibrinogen to fibrin, an adequate amount of fibrinogen must be present in the patient plasma. Patients with absent fibrinogen or a reduced concentration of fibrinogen will manifest a prolonged or unclottable thrombin time, depending on the severity. Generally speaking, fibrinogen levels need to be below 1 g/l before the thrombin time will become abnormal. Fibrinogen deficiencies can be either congenital or acquired. The inherited deficiencies are termed afibrinogenaemia, where fibrinogen is absent or severely reduced (generally <0.2 g/l), or hypofibrinogenaemia if reduced. Acquired deficiencies of fibrinogen are observed in disseminated intravascular coagulopathy, following thrombolytic therapy for life threatening thrombosis, liver disease and in certain malignancies. ii. Quantitative abnormalities A functional abnormality of fibrinogen may likewise manifest with a prolonged thrombin time. This can occur as a result of impaired thrombin activation of fibrinogen, i.e. reduced conversion of fibrinogen to fibrin, or due to impaired fibrin polymerisation, leading to clot instability (see below). These conditions, called dysfibrinogenaemias, are rare and can be either genetically inherited or acquired. Acquired dysfibrinogenaemias occur most commonly in the context of liver disease. The thrombin time in neonates is commonly prolonged because of the presence of foetal fibrinogen. Although the concentration of fibrinogen is normal, there is an increase in carbohydrate content which delays polymerisation similar to what is observed in the acquired dysfibrinogenaemia of liver disease. In this context it is imperative to ensure that the reference range used is age specific. Infants less than 6 months old can be expected to have a thrombin time that is approximately 2 3 seconds longer than the normal adult reference range. iii. Other causes Very rarely, patients with amyloidosis may present with a prolonged thrombin time due to the inhibition of conversion of fibrinogen to fibrin by the presence of abnormal circulating proteins. This in essence would manifest similarly to a quantitative deficiency of fibrinogen.
4 4 b. Interference with fibrin polymerisation i. Dysfibrinogenaemias and FDPs As the end point of detection of the thrombin time is clot formation, anything that will interfere with the stability of the clot may cause a prolongation of the clotting time. As previously described, the fibrin polymer is progressively built up from individual evenly sized and structurally identical fibrin monomers. The presence of any structural variants, as in dysfibrinogenaemia, or FDPs such as D-dimers, which contain only part of the structure, may result in an unstable clot if these are incorporated into the growing polymer. A very high concentration of D-dimers may result in a prolonged thrombin time. The aetiology of the impairment of fibrinogen, which is produced in the liver, in acquired dysfibrinogenaemias associated with liver disease, is a structural defect caused by an increased carbohydrate content which interferes with fibrin polymerisation. ii. Other causes Paradoxically, a very high fibrinogen (> 14 g/l), but not elevated levels associated with the acute phase response, can be associated with a prolonged thrombin time which is thought to occur because the excess fibrinogen interferes with the assembly of fibrin. The presence of abnormal circulating proteins, such as paraproteins observed in myeloma may interfere with fibrin polymerisation and cause a prolonged thrombin time. Hypoalbuminaemia (albumin <30 g/l) may also interfere with fibrin polymerisation and cause a prolongation of the thrombin time. c. Thrombin inhibition i. Heparin As the thrombin time is initiated by the addition of exogenous thrombin, it is insensitive to deficiencies of all upstream clotting factors that are involved in the generation of endogenous thrombin. The assay is however sensitive to any substances present in the patient plasma that may inhibit the exogenous thrombin added to the plasma as a reagent. Even a very small amount of heparin, whether given therapeutically or introduced as a contaminant during blood collection from a heparinized central intravenous (IV) line, will result in a thrombin time that invariably will fail to clot. The test is so exquisitely sensitive to heparin that one of the commonest uses of the thrombin time is to confirm the presence of heparin when this is suspected to be present and is interfering with the interpretation of other coagulation tests. As such it is most commonly used as a quality control check to establish the presence or absence of unfractionated heparin in a sample prior to undertaking more complex tests of coagulation rather than for the investigation of clinically suspected abnormalities of fibrinogen. The reptilase test, which has a similar test principle to thrombin time, is used to confirm that the cause of prolongation of a thrombin time is indeed heparin (see below). Low molecular weight heparins will generally not affect the thrombin time unless the patient has been significantly overdosed. ii. Other anticoagulant drugs The direct thrombin inhibitors hirudin, argatroban and the new oral agent dabigatran all cause a prolongation of the thrombin time. The thrombin time shows a linear dose response to these drugs although most commercially available thrombin time assays will be too sensitive to provide any quantitative information. A normal thrombin time would generally exclude the presence of a direct thrombin inhibitor whereas a markedly prolonged or unclottable thrombin time cannot differentiate between sub-therapeutic, therapeutic or supra-therapeutic levels. Rivaroxaban, being a direct factor Xa inhibitor has no effect on the thrombin time. Warfarin also has no effect on the thrombin time as it exerts its anticoagulant action by impeding the synthesis of functional prothrombin, and other vitamin K dependent clotting factors, as these are all upstream from the test reaction. iii. Rare antibodies Patients previously exposed to bovine thrombin, may develop inhibitors that prolong bovine-based thrombin times, and if there is cross-reactivity to human thrombin, may also prolong the thrombin times where the thrombin reagent is
5 5 of human origin. Patients may be exposed to bovine thrombin in the form of tissue glue. Tissue glue is a unique adhesive material that is being used with increasing frequency in a variety of surgical situations to rapidly secure haemostasis, independent of the patient s own coagulation status, in anatomically vulnerable sites. In practice, it is a twocomponent system in which a solution of concentrated fibrinogen and factor XIII are combined with a solution of thrombin and calcium in order to form a clot, simulating the final stage of the clotting cascade. Once the thrombin, calcium, fibrinogen and factor XIII are all combined, a fibrin clot forms in seconds. Heparin-like anticoagulants have been reported, albeit rarely, in patients with malignant neoplasms and will manifest with a prolonged thrombin time. Causes of shortened thrombin times In very rare instances, a shortened thrombin time may be observed. The commonest cause of this would be the use of colloidal fluids, such as dextran or hydroxyethyl starch, as circulatory volume expanders during surgery. In such cases the clotting times are shortened although clot strength has been shown to be weaker. All other causes of a prolonged thrombin time would also affect the reptilase time. There is only one scenario that would give rise to the combination of a normal thrombin time with a prolonged reptilase time, namely elevated fibrinogen levels. This is commonly observed as plasma samples submitted for coagulation testing are frequently received from patients that have had an acute thrombosis which would elicit an acute phase reaction, and hence a rise in fibrinogen. Even mildly elevated levels of fibrinogen (4 7 g/l) commonly cause a prolongation of the reptilase time, in contrast to the thrombin time where this is only manifest with extreme hyperfibrinogenaemia (> 14 g/l). The reason for this difference is not clear but it is well documented that the reptilase times revert back to normal once the fibrinogen levels normalise. As for thrombin time, reference ranges for reptilase time are dependent on the assay system and hence local reference ranges must be used for interpretation. Such a reference should be established from plasma obtained from normal individuals with confirmed normal fibrinogen levels. When using such reference values, about 30% of patients with an elevated fibrinogen level will have a prolonged reptilase time, depending on the degree of fibrinogen elevation. The reptilase time The reptilase test, also known as the atroxin time, is very similar in principle to the thrombin time in that it assesses the conversion of fibrinogen to fibrin. The difference is that in the reptilase test, thombin is replaced with the thrombinlike enzyme reptilase which is purified from the venom of the snake Bothrops atrox. This enzyme, like thrombin converts fibrinogen to fibrin. The difference however is that it cleaves only fibrinopeptide A, and not fibrinopeptide B, from fibrinogen. The main difference that is observed is that this assay is insensitive to the presence of heparin and other drugs that act as thrombin inhibitors. A sample in which the thrombin time is prolonged, a normal reptilase time would (in most cases) be consistent with the presence of unfractionated heparin or one of the newer direct thrombin inhibitor drugs. A prolonged thrombin time is therefore commonly associated with a normal reptilase time. What are the indications for thrombin time and reptilase time testing? A thrombin time test is generally a test that the laboratory will perform if the baseline PT and APTT are abnormal. As the commonest cause of prolongation of both PT and APTT is heparin, the thrombin time is performed as a quick test to exclude this possibility. If heparin (or heparin like substances and other thrombin inhibitors) is the cause of the prolonged thrombin time, the normal reptilase time will confirm this. The reptilase time is therefore generally only ever indicated if the thrombin time is abnormal. Thrombin time testing is also commonly performed as part of a panel of tests to determine the possible cause of the underlying hypercoagulability in patients with thrombosis. In this case, the aim is two-fold.
6 6 Firstly, to exclude heparin as above, as its presence would interfere with other assays and make them inconclusive. In such cases, the plasma may have to be treated with a special enzyme called hepzyme to eliminate this interference before commencing with additional tests. More commonly however, further testing will be delayed until such time that the patient is no longer heparinised and a fresh blood sample submitted to the laboratory. Secondly, the thrombin time is used to assess for dysfibrinogenaemia, which may manifest as thrombosis, although it is an infrequent finding accounting for less than 1% of cases. Whilst the thrombin time is generally prolonged in deficiencies of fibrinogen and the dysfibrinogenaemias, in such cases a Clauss fibrinogen test, which is sensitive to both quantitative and functional abnormalities, would generally be more informative. In dysfibrinogenaemia, the Clauss fibrinogen result (an activity assay) would be lower than an antigen based fibrinogen assay (e.g. ELISA), whereas both would be low in a deficiency of fibrinogen with normal structure and function. If a dysfibrinogenaemia is suspected, the fibrinogen activity-antigen ratio is used for confirmation in most cases. Liver function tests would support an acquired aetiology whereas family studies and more specialized investigations are required to confirm an inherited abnormality. What tests does Sysmex have on offer? Sysmex has reagents and controls available for thrombin time and reptilase time for manual testing or for automated testing (Tab. 1). Test protocols are available for all Sysmex coagulation analysers. Sysmex only provides a normal control for these tests. As a general rule, it is not considered necessary to perform an abnormal control for thrombin time and reptilase time tests as these are primarily used to see if there is heparin contamination in the sample in which case the thrombin usually fails to clot, and the reptilase time is normal. If a laboratory wishes to include an abnormal control this can be sourced from another company. The laboratory however will have to establish its own target range as values may vary significantly from one testing platform to the next. Take home message The thrombin time and reptilase time are basic coagulation tests that evaluate fibrin formation from fibrinogen in plasma. The thrombin time is most commonly used to exclude the presence of heparin before commencing more extensive coagulation tests which would otherwise be difficult to interpret. The advantage of the reptilase time is that it is insensitive to heparin and other inhibitors of thrombin. Causes of prolonged thrombin and reptilase times include fibrinogen abnormalities and anything that may interfere with fibrin polymerisation. The thrombin time and reptilase time are used for screening for dysfibrinogenaemia but it must be noted that both are susceptible to a high rate of false positivity as they are nonspecific tests. If dysfibrinogenaemia is suspected on the basis of a prolonged thrombin and/or reptilase time, this must be confirmed with a fibrinogen activity:antigen ratio determination. Thrombin Time Reptilase Time Reagent Test Thrombin (OWHM135) or Batroxobin reagent (OUOV215) Thromboclotin (281007) Normal Control Control Plasma N (ORKE415) or Control Plasma N (ORKE415) or Citrol 1 (291070) Citrol 1 (291070) Calibrator Not required Not required Tab. 1 Thrombin time and reptilase time reagents available from Sysmex
7 7 References [1] Favaloro EJ and Lippi G. (2013): The new oral anticoagulants and the future of haemostasis laboratory testing. Biochemia Medica 22: [2] Curvers J. et al. (2012): Measuring direct thrombin inhibitors with routine and dedicated coagulation assays. Which assay is helpful? Am J Clin Pathol 138: [3] Cunningham MT et al. (2002): Laboratory diagnosis of dysfibrinogenemia. Arch Pathol Lab Med 126(4): [4] Van Cott EM et al. (2002): Elevated fibrinogen in an acute phase reaction prolongs the reptilase time but typically not the thrombin time. Am J Clin Pathol 118: Compiled by Dr Marion Münster Sysmex Europe GmbH Bornbarch 1, Norderstedt, Germany, Phone Fax info@sysmex-europe.com
Sysmex Educational Enhancement and Development No
 SEED Haematology Sysmex Educational Enhancement and Development No 3 2014 The Thrombin Time test and Reptilase test what is their role in coagulation testing? The purpose of this newsletter is to provide
SEED Haematology Sysmex Educational Enhancement and Development No 3 2014 The Thrombin Time test and Reptilase test what is their role in coagulation testing? The purpose of this newsletter is to provide
Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems.
 Test Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems. Karen A. Moffat BEd, MSc, ART, FCSMLS(D) Technical Specialist, Coagulation, HRLMP Assistant Professor, Department of
Test Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems. Karen A. Moffat BEd, MSc, ART, FCSMLS(D) Technical Specialist, Coagulation, HRLMP Assistant Professor, Department of
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues
 Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Sysmex Educational Enhancement & Development
 Sysmex Educational Enhancement & Development SEED-Africa Newsletter No 9 2011 Quality control in coagulation testing Basic Coagulation The purpose of this newsletter is to provide an overview of internal
Sysmex Educational Enhancement & Development SEED-Africa Newsletter No 9 2011 Quality control in coagulation testing Basic Coagulation The purpose of this newsletter is to provide an overview of internal
Activated Protein C Resistance vs Factor V Leiden assay: Which is the most cost effective?
 Activated Protein C Resistance vs Factor V Leiden assay: Which is the most cost effective? Rajiv K. Pruthi, M.B.B.S Co-Director, Special Coagulation Laboratory & Director, Mayo Comprehensive Hemophilia
Activated Protein C Resistance vs Factor V Leiden assay: Which is the most cost effective? Rajiv K. Pruthi, M.B.B.S Co-Director, Special Coagulation Laboratory & Director, Mayo Comprehensive Hemophilia
Coagulopathy Case-2. Andy Nguyen, M.D. 2009
 Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY
 LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
Session 1 Topics. Vascular Phase of Hemostasis. Coagulation Pathway. Action of Unfractionated Heparin. Laboratory Monitoring of Anticoagulant Therapy
 ~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
EDUCATIONAL COMMENTARY STRAIGHT TALK ABOUT THE D-DIMER
 EDUCATIONAL COMMENTARY STRAIGHT TALK ABOUT THE D-DIMER Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits
EDUCATIONAL COMMENTARY STRAIGHT TALK ABOUT THE D-DIMER Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits
Princess Alexandra Hospital Emergency Department. Clinical Procedure. 1 Introduction
 Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
Clinical Procedure. ROTEM Trauma, Resuscitation. Princess Alexandra Hospital Emergency Department. 1 Introduction
 Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides.
 These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
DOACs: When and how to measure their anticoagulant effect
 DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
Laboratory investigation in the Bleeding Patient. Dr Craig Taylor Consultant Haematologist May 2016
 Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
EDUCATIONAL COMMENTARY D-DIMER UPDATE
 EDUCATIONAL COMMENTARY D-DIMER UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits see the Continuing
EDUCATIONAL COMMENTARY D-DIMER UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits see the Continuing
Basic coagulation applications and case studies
 Basic coagulation applications and case studies Jing Jin Clinical laboratory Scientist (MLS, ASCP) - Coagulation/Hematology Stanford University Hospital and Clinics 1 Agenda Overview about 3 major phases
Basic coagulation applications and case studies Jing Jin Clinical laboratory Scientist (MLS, ASCP) - Coagulation/Hematology Stanford University Hospital and Clinics 1 Agenda Overview about 3 major phases
Laboratory Monitoring of Anticoagulation
 Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
TSOAC Case Study 1. Question. TSOAC Case Study 1 Continued
 TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
General Principles of. Hemostasis. Kristine Krafts, M.D.
 General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
Local vasoconstriction. is due to local spasm of the smooth muscle (symp. reflex) can be maintained by platelet vasoconstrictors
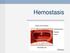 Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Disclosure (s) Relevant financial relationship(s) None Off-label usage None Change in slide set You betcha! (YES!) 2015 MFMER slide-1
 Disclosure (s) Relevant financial relationship(s) None Off-label usage None Change in slide set You betcha! (YES!) 2015 MFMER slide-1 Learning Objectives Explain the concept of thrombophilia Recognize
Disclosure (s) Relevant financial relationship(s) None Off-label usage None Change in slide set You betcha! (YES!) 2015 MFMER slide-1 Learning Objectives Explain the concept of thrombophilia Recognize
Coagulation Mechanisms Dr. Nervana Bayoumy
 Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
DOAC s and Implications on Laboratory Results. Kandice Kottke-Marchant, MD, PhD Cleveland Clinic
 DOAC s and Implications on Laboratory Results Kandice Kottke-Marchant, MD, PhD Cleveland Clinic Anticoagulants Heparin Low Molecular Weight Heparins enoxaparin, fragmin Heparin pentasaccharide - fondaparinux
DOAC s and Implications on Laboratory Results Kandice Kottke-Marchant, MD, PhD Cleveland Clinic Anticoagulants Heparin Low Molecular Weight Heparins enoxaparin, fragmin Heparin pentasaccharide - fondaparinux
Coagulation Cascade. TF-VIIa. Tissue Factor + VII. XIIa. Prothrombin. XIa. IXa. VIIIa. Thrombin. XL- Fibrin. XIII Monomer. Fibrinogen.
 Coagulation Cascade Intrinsic Pathway Extrinsic Pathway Contact Activation XIIa XI XIa Prekallikrein HMW Kininogen IX IXa Ca 2+ Anticoagulation proteins: Protein C, Protein S, Antithrombin III, TFPI TF
Coagulation Cascade Intrinsic Pathway Extrinsic Pathway Contact Activation XIIa XI XIa Prekallikrein HMW Kininogen IX IXa Ca 2+ Anticoagulation proteins: Protein C, Protein S, Antithrombin III, TFPI TF
Hypercoagulation. CP Conference 11/14/2006
 Hypercoagulation CP Conference 11/14/2006 Overview Hypercoagulation: poorly understood phenomena No definite cause is identified in > 40% of cases Three major factors in thrombus formation (Rudolf Virchow,
Hypercoagulation CP Conference 11/14/2006 Overview Hypercoagulation: poorly understood phenomena No definite cause is identified in > 40% of cases Three major factors in thrombus formation (Rudolf Virchow,
Laboratory Testing Issues for Protein C, Protein S and Antithrombin Assays
 Laboratory Testing Issues for Protein C, Protein S and Antithrombin Assays Richard A. Marlar Ph.D. University of Oklahoma THSNA Meeting- Chicago, IL April 14-16, 2016 DISCLOSURE Richard A. Marlar, PhD
Laboratory Testing Issues for Protein C, Protein S and Antithrombin Assays Richard A. Marlar Ph.D. University of Oklahoma THSNA Meeting- Chicago, IL April 14-16, 2016 DISCLOSURE Richard A. Marlar, PhD
Pharmacology Lecture 5. Anticoagulants
 Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
WORTHAM LABORATORIES, INC. DRAFT Thrombin Reagent
 WORTHAM LABORATORIES, INC. DRAFT Thrombin Reagent Intended Use Wortham Laboratories Thrombin Reagent is intended for thrombin to convert fibrinogen in the quantitative determination of fibrinogen in plasma
WORTHAM LABORATORIES, INC. DRAFT Thrombin Reagent Intended Use Wortham Laboratories Thrombin Reagent is intended for thrombin to convert fibrinogen in the quantitative determination of fibrinogen in plasma
UW Medicine Alternative Monitoring for Antithrombotic Agents
 Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
Use of Chromogenic Assay of Factor X to Accept or Reject INR Results in Warfarin Treated Patients
 CM&R Rapid Release. Published online ahead of print July 22, 2009 as Use of Chromogenic Assay of Factor X to Accept or Reject INR Results in Warfarin Treated Patients Michael J. Sanfelippo, MS, MT ASCP;
CM&R Rapid Release. Published online ahead of print July 22, 2009 as Use of Chromogenic Assay of Factor X to Accept or Reject INR Results in Warfarin Treated Patients Michael J. Sanfelippo, MS, MT ASCP;
2 Thomas G. DeLoughery
 Tests of Hemostasis and Thrombosis 2 Thomas G. DeLoughery A routine laboratory test once well-established is often slavishly adhered to, with little further thought about how it originated, why it is done
Tests of Hemostasis and Thrombosis 2 Thomas G. DeLoughery A routine laboratory test once well-established is often slavishly adhered to, with little further thought about how it originated, why it is done
Human D- dimer ELISA Kit
 Product Manual Human D- dimer ELISA Kit Catalog Numbers PRB- 5048 PRB- 5048-5 96 assays 5 x 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Thrombosis is the local coagulation
Product Manual Human D- dimer ELISA Kit Catalog Numbers PRB- 5048 PRB- 5048-5 96 assays 5 x 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Thrombosis is the local coagulation
Special Coagulation - APC Resistance. DiaPharma Group, Inc. Customer Service: Technical Support:
 Special Coagulation - APC Resistance DiaPharma Group, Inc. Customer Service: 1.800.526.5224 Technical Support:1.800.447.3846 www.diapharma.com 1 Review of Hemostasis Overview Pathways of coagulation, anticoagulation,
Special Coagulation - APC Resistance DiaPharma Group, Inc. Customer Service: 1.800.526.5224 Technical Support:1.800.447.3846 www.diapharma.com 1 Review of Hemostasis Overview Pathways of coagulation, anticoagulation,
Guideline on core SmPC for human fibrinogen products
 23 July 2015 EMA/CHMP/BPWP/691754/2013 Rev 1 Committee for Medicinal Products for Human Use (CHMP) Draft Agreed by Blood Products Working Party 27 November 2013 Adoption by CHMP for release for consultation
23 July 2015 EMA/CHMP/BPWP/691754/2013 Rev 1 Committee for Medicinal Products for Human Use (CHMP) Draft Agreed by Blood Products Working Party 27 November 2013 Adoption by CHMP for release for consultation
Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity
 Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity Abhishek Gulati What is enoxaparin? Low molecular weight heparin anticoagulant Used to minimise the
Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity Abhishek Gulati What is enoxaparin? Low molecular weight heparin anticoagulant Used to minimise the
Using TEG in the ED, OR, and ICU. Don H. Van Boerum, MD, FACS
 Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
Blood transfusion in special situations and poly-trauma. Dr Marina Karakantza Consultant Haematologist in Transfusion Medicine, LTHT
 Blood transfusion in special situations and poly-trauma Dr Marina Karakantza Consultant Haematologist in Transfusion Medicine, LTHT Uncontrolled bleeding is a major preventable cause of death in trauma
Blood transfusion in special situations and poly-trauma Dr Marina Karakantza Consultant Haematologist in Transfusion Medicine, LTHT Uncontrolled bleeding is a major preventable cause of death in trauma
Coagulation in perspective: Blood management. Objectives
 Coagulation in perspective: Blood management Julie Wegner, PhD jawrbl@gmail.com Objectives To gain a basic understanding of the following: 1. Coagulation components and processes Why patients bleed. 2.
Coagulation in perspective: Blood management Julie Wegner, PhD jawrbl@gmail.com Objectives To gain a basic understanding of the following: 1. Coagulation components and processes Why patients bleed. 2.
Novel Anti-coagulant Agents. David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan
 Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Hematotoxin producing snakes in Thailand พญ.ม ชฌ มา รอดเช อ พญ.อ สร ย หาญอ ท ยร ศม
 Hematotoxin producing snakes in Thailand พญ.ม ชฌ มา รอดเช อ พญ.อ สร ย หาญอ ท ยร ศม Hematotoxin producing snakes Pit vipers (Crotalinae) Malayan pit viper (Calloselasma rhodostoma) Green pit viper (Trimeresurus
Hematotoxin producing snakes in Thailand พญ.ม ชฌ มา รอดเช อ พญ.อ สร ย หาญอ ท ยร ศม Hematotoxin producing snakes Pit vipers (Crotalinae) Malayan pit viper (Calloselasma rhodostoma) Green pit viper (Trimeresurus
Note: The taller 100 x 13 mm tube is not designed to run on the ACL TOP. Plasma after centrifugation of these tubes must be placed in sample cups.
 Created Revised Reviewed Approved Lupus Insensitive aptt on the ACL TOP HEM 4.15.1 7/13/2012 4/11/2013 4/11/2013 4/11/2013 I. PRINCIPLE The activated partial thromboplastin time is a global screening procedure
Created Revised Reviewed Approved Lupus Insensitive aptt on the ACL TOP HEM 4.15.1 7/13/2012 4/11/2013 4/11/2013 4/11/2013 I. PRINCIPLE The activated partial thromboplastin time is a global screening procedure
Laboratory Monitoring of Unfractionated Heparin Therapy
 1 PATHOLOGY & LABORATORY MEDICINE December, 2015 Laboratory Monitoring of Unfractionated Heparin Therapy On November 18, 2015, the Thrombosis and Hemostasis Laboratory transitioned from the aptt to the
1 PATHOLOGY & LABORATORY MEDICINE December, 2015 Laboratory Monitoring of Unfractionated Heparin Therapy On November 18, 2015, the Thrombosis and Hemostasis Laboratory transitioned from the aptt to the
With Stago, discover an outstanding Routine range
 In Haemostasis, There s routine... and then there s Routine With Stago, discover an outstanding Routine range An optimal Routine range for guaranteed satisfaction 1 Comprehensive range Stago s extensive
In Haemostasis, There s routine... and then there s Routine With Stago, discover an outstanding Routine range An optimal Routine range for guaranteed satisfaction 1 Comprehensive range Stago s extensive
ANEMIA. Oral iron. IV iron gluconate (order set #233)
 PREVENTION ANEMIA Oral iron IV iron gluconate (order set #233) TRANSEXAMIC ACID Efficacy of IV TXA in Reducing Blood Loss After Elective C-section: Prospective, Randomized, Double-blind, Placebo Controlled
PREVENTION ANEMIA Oral iron IV iron gluconate (order set #233) TRANSEXAMIC ACID Efficacy of IV TXA in Reducing Blood Loss After Elective C-section: Prospective, Randomized, Double-blind, Placebo Controlled
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS
 Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
Adv Pathophysiology Unit 4 Page 1 of 10. Learning Objectives for this file:
 Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
Index. Autoimmune thrombocytopenic purpura (AITP), 100, 102, 105, 108, 187 Automated platelet counters, , 108
 A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
Manejo de la transfusión de plaquetas. Ileana López-Plaza, MD
 Manejo de la transfusión de plaquetas Ileana López-Plaza, MD Thrombocytopenia Common in ICU setting 25-38% with< 100,000/µL 2-3 % with < 10,000/µL Common etiologies Drug-induced: heparin, antibiotics,
Manejo de la transfusión de plaquetas Ileana López-Plaza, MD Thrombocytopenia Common in ICU setting 25-38% with< 100,000/µL 2-3 % with < 10,000/µL Common etiologies Drug-induced: heparin, antibiotics,
Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015
 + Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
+ Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
PROTHROMBIN TIME WHY USE LOW ISI (HIGH SENSITIVITY)
 PROTHROMBIN TIME WHY USE LOW ISI (HIGH SENSITIVITY) PROTHROMBIN TIME DEFINITION The Prothrombin time is the functional determination of the extrinsic coagulation pathway. It is a widely used laboratory
PROTHROMBIN TIME WHY USE LOW ISI (HIGH SENSITIVITY) PROTHROMBIN TIME DEFINITION The Prothrombin time is the functional determination of the extrinsic coagulation pathway. It is a widely used laboratory
If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom
 If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom Heparin Discovered 1916, commercial available 1935 Heparin Is there an alternative, not really
If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom Heparin Discovered 1916, commercial available 1935 Heparin Is there an alternative, not really
Lina Al-Lawama. Rama Al-Ashqar. Malik Al-Zohlof
 2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
iccnet CHSA Clinical Protocol - HEPARIN
 Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
Managing the Risks Associated with Anticoagulant Therapy. Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde
 Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Marcia L. Zucker, Ph.D. ZIVD LLC
 Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 Picture courtesy of Helena Laboratories 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway
Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 Picture courtesy of Helena Laboratories 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway
LABORATORY APPROCH TO THE BLEEDING PATIENT
 Anne Winkler, MD Emory University School of Medicine, Atlanta Georgia Assistant Professor, Pathology & Laboratory Medicine Medical Director, Transfusion Service, Grady Health System Assistant Director,
Anne Winkler, MD Emory University School of Medicine, Atlanta Georgia Assistant Professor, Pathology & Laboratory Medicine Medical Director, Transfusion Service, Grady Health System Assistant Director,
Critical aspects in routine coagulation testing
 Pure & Appl. Chem., Vol. 68, No. 10, pp. 1867-1871,1996, Printed in Great Britain. 0 1996 IUPAC Critical aspects in routine coagulation testing A. D'Angelo, P. Della Valle, L. Crippa, E. Pattarini, S.
Pure & Appl. Chem., Vol. 68, No. 10, pp. 1867-1871,1996, Printed in Great Britain. 0 1996 IUPAC Critical aspects in routine coagulation testing A. D'Angelo, P. Della Valle, L. Crippa, E. Pattarini, S.
Haemostasis. The function of haemostasis is: to prevent blood loss from injured vessels. to stop bleeding. to prevent thrombosis
 Haemostasis Haemostasis The function of haemostasis is: to prevent blood loss from injured vessels to stop bleeding to prevent thrombosis Haemostasis blood endothelium basement membrane subendothelium
Haemostasis Haemostasis The function of haemostasis is: to prevent blood loss from injured vessels to stop bleeding to prevent thrombosis Haemostasis blood endothelium basement membrane subendothelium
New Anticoagulants Linda Liu, M.D.
 Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
Emergency and Perioperative Hemostasis Testing: Which Assays Provide Helpful Information. Wayne Chandler, MD Laboratory Medicine Seattle Children s
 Emergency and Perioperative Hemostasis Testing: Which Assays Provide Helpful Information Wayne Chandler, MD Laboratory Medicine Seattle Children s Emergency Hemostasis Testing Patients actively bleeding
Emergency and Perioperative Hemostasis Testing: Which Assays Provide Helpful Information Wayne Chandler, MD Laboratory Medicine Seattle Children s Emergency Hemostasis Testing Patients actively bleeding
Changes in coagulation and tissue plasminogen activator after the treatment of cerebral infarction with lumbrokinase
 Clinical Hemorheology and Microcirculation 23 (2000) 213 218 213 IOS Press Changes in coagulation and tissue plasminogen activator after the treatment of cerebral infarction with lumbrokinase Lirong Jin
Clinical Hemorheology and Microcirculation 23 (2000) 213 218 213 IOS Press Changes in coagulation and tissue plasminogen activator after the treatment of cerebral infarction with lumbrokinase Lirong Jin
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs
 Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
Anticoagulation in VTE The Haematologist s Perspective. Dr. M.D. Maina FRCP Edin.
 Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Primary hemostasis. Vascular endothelium Vasoconstriction : local tissue factor, nervous system
 Primary hemostasis Vascular endothelium Vasoconstriction : local tissue factor, nervous system Platelet Plug Platelet Adhesion Platelet Activation Platelet Aggregation Platelet Plug Formation Secondary
Primary hemostasis Vascular endothelium Vasoconstriction : local tissue factor, nervous system Platelet Plug Platelet Adhesion Platelet Activation Platelet Aggregation Platelet Plug Formation Secondary
Introduction Hemostasis: Tourniquet Test & Bleeding Time. Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO
 Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
R.Li, C.Swaelens, F.Vandermijnsbrugge, B.Cantinieaux BSTH Laboratory of haematology, Porte de Hal,
 Institut J. Bordet Normal with Actin-FS avoids intrinsic pathway factors assays in the presence of an isolated prolongation of (Platelin-LS) without hemorrhagic history R.Li, C.Swaelens, F.Vandermijnsbrugge,
Institut J. Bordet Normal with Actin-FS avoids intrinsic pathway factors assays in the presence of an isolated prolongation of (Platelin-LS) without hemorrhagic history R.Li, C.Swaelens, F.Vandermijnsbrugge,
Use of ROTEM from the Laboratory Perspective. A/Prof David Roxby SA Pathology
 Use of ROTEM from the Laboratory Perspective A/Prof David Roxby SA Pathology What s the Problem? Constant changes in treatment recommendations Lack of good evidence to guide practice Variations in clinical
Use of ROTEM from the Laboratory Perspective A/Prof David Roxby SA Pathology What s the Problem? Constant changes in treatment recommendations Lack of good evidence to guide practice Variations in clinical
Disclosures. Thromboelastography. TEG Methodology. TEG Output. Thromboelastography (TEG): Basics & Clinical Applications
 Thromboelastography (TEG): Basics & Clinical Applications Paula J. Santrach MD Associate Professor, Laboratory Medicine Mayo Clinic Rochester, MN Disclosures Relevant financial relationships NONE Off label
Thromboelastography (TEG): Basics & Clinical Applications Paula J. Santrach MD Associate Professor, Laboratory Medicine Mayo Clinic Rochester, MN Disclosures Relevant financial relationships NONE Off label
FACTOR XIII DEFICIENCY IN PAKISTAN
 FACTOR XIII DEFICIENCY IN PAKISTAN Pages with reference to book, From 67 To 69 Aamir Nadeem Shaikh, Mohammad Khurshid ( Department of Pathology, The Aga Khan University Hospital, Karachi. ) ABSTRACT Patients
FACTOR XIII DEFICIENCY IN PAKISTAN Pages with reference to book, From 67 To 69 Aamir Nadeem Shaikh, Mohammad Khurshid ( Department of Pathology, The Aga Khan University Hospital, Karachi. ) ABSTRACT Patients
OERMATAN SULFATE: A NEW CONCEPT IN ANTITHROMBOTIC THERAPY
 OERMATAN SULFATE: A NEW CONCEPT IN ANTITHROMBOTIC THERAPY by JOANNE VAN RYN-McKENNA, B.Sc., M.Sc. A Thesis Submitted to the School of Graduate Studies in Partial Fulfilment of the Requirements for the
OERMATAN SULFATE: A NEW CONCEPT IN ANTITHROMBOTIC THERAPY by JOANNE VAN RYN-McKENNA, B.Sc., M.Sc. A Thesis Submitted to the School of Graduate Studies in Partial Fulfilment of the Requirements for the
DEPARTMENT OF CLINICAL LABORATORY SCIENCES SCHOOL OF HEALTH TECHNOLOGY AND MANAGEMENT THE UNIVERSITY AT STONY BROOK STONY BROOK, NEW YORK
 DEPARTMENT OF CLINICAL LABORATORY SCIENCES SCHOOL OF HEALTH TECHNOLOGY AND MANAGEMENT THE UNIVERSITY AT STONY BROOK STONY BROOK, NEW YORK 11794-8205 COAGULATION COMPETENCY EVALUATION FORM STUDENT NAME:
DEPARTMENT OF CLINICAL LABORATORY SCIENCES SCHOOL OF HEALTH TECHNOLOGY AND MANAGEMENT THE UNIVERSITY AT STONY BROOK STONY BROOK, NEW YORK 11794-8205 COAGULATION COMPETENCY EVALUATION FORM STUDENT NAME:
Laboratory Investigation of Challenging Cases. Laura A. Worfolk, Ph.D Scientific Director, Coagulation
 Laboratory Investigation of Challenging Cases Laura A. Worfolk, Ph.D Scientific Director, Coagulation Coagulation Cascade XII XIIa XI HMWK/Prekallikrein XIa VII Injury IX X IXa VIII Xa X TF TF/VIIa Prothrombin
Laboratory Investigation of Challenging Cases Laura A. Worfolk, Ph.D Scientific Director, Coagulation Coagulation Cascade XII XIIa XI HMWK/Prekallikrein XIa VII Injury IX X IXa VIII Xa X TF TF/VIIa Prothrombin
P. W. HOWIE M.D., M.R.C.O.G. first method of activation is the intrinsic system. Hageman factor, which in turn activates a series of
 Postgraduate Medical Journal (May 1979) 55, 362-366 Blood clotting and fibrinolysis in pregnancy P. W. HOWIE M.D., M.R.C.O.G. MRC Unit of Reproductive Biology, Edinburgh Summary During normal pregnancy,
Postgraduate Medical Journal (May 1979) 55, 362-366 Blood clotting and fibrinolysis in pregnancy P. W. HOWIE M.D., M.R.C.O.G. MRC Unit of Reproductive Biology, Edinburgh Summary During normal pregnancy,
Coagulation. Coagulation Limited CGL, CGDF Surveys & Anatomic Pathology Education Programs. Coagulation 117
 www.cap.org Coagulation Analytes/procedures in bold type are regulated for proficiency testing by the Centers for Medicare & Medicaid Serviced (CMS). Coagulation Limited CGL, CGDF Analyte CGL CGDF New
www.cap.org Coagulation Analytes/procedures in bold type are regulated for proficiency testing by the Centers for Medicare & Medicaid Serviced (CMS). Coagulation Limited CGL, CGDF Analyte CGL CGDF New
Differential effects of the direct thrombin inhibitor dabigatran etexilate vs warfarin on platelet function
 Differential effects of the direct thrombin inhibitor dabigatran etexilate vs warfarin on platelet function Giulia Renda 1, Gelsomina Malatesta 1, Valentina Bucciarelli 1, Alessia Napoleone 1, Loredana
Differential effects of the direct thrombin inhibitor dabigatran etexilate vs warfarin on platelet function Giulia Renda 1, Gelsomina Malatesta 1, Valentina Bucciarelli 1, Alessia Napoleone 1, Loredana
Haemostasis Reagents product list 2018
 Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch Product # ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Product name
Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch Product # ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Product name
Type of intervention Treatment; secondary prevention. Economic study type Cost-effectiveness analysis.
 Coagulation disorders induced by L-asparaginase: correction with and without fresh-frozen plasma Glasmacher A, Kleinschmidt R, Unkrig C, Mezger J, Scharf R E Record Status This is a critical abstract of
Coagulation disorders induced by L-asparaginase: correction with and without fresh-frozen plasma Glasmacher A, Kleinschmidt R, Unkrig C, Mezger J, Scharf R E Record Status This is a critical abstract of
Table of Contents. Introduction. Worldwide Market and Technology Overview
 Table of Contents Introduction Worldwide Market and Technology Overview A. Major Routine and Special Coagulation Tests 1. Introduction 2. Activated Partial Thromboplastin Time (APTT) 3. Alpha-2 Antiplasmin
Table of Contents Introduction Worldwide Market and Technology Overview A. Major Routine and Special Coagulation Tests 1. Introduction 2. Activated Partial Thromboplastin Time (APTT) 3. Alpha-2 Antiplasmin
Human Plasmin Activity Assay ELISA Kit
 Human Plasmin Activity Assay ELISA Kit Catalog No. CSI12527A 1 x 96 tests CSI12527B 5 x 96 tests Intended Use: Background: Assay Principle: Reagents Provided: This human plasmin activity assay is for the
Human Plasmin Activity Assay ELISA Kit Catalog No. CSI12527A 1 x 96 tests CSI12527B 5 x 96 tests Intended Use: Background: Assay Principle: Reagents Provided: This human plasmin activity assay is for the
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency Evaluation of Medicines for Human Use London, 29 July 2004 CPMP/BPWG/1089/00 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON THE CLINICAL INVESTIGATION OF PLASMA
European Medicines Agency Evaluation of Medicines for Human Use London, 29 July 2004 CPMP/BPWG/1089/00 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON THE CLINICAL INVESTIGATION OF PLASMA
Apheresis Anticoagulant Removal. Oluwatoyosi Onwuemene, MD MS May 6th, 2017
 Apheresis Anticoagulant Removal Oluwatoyosi Onwuemene, MD MS May 6th, 2017 Talk Outline Case presentation Factors associated with drug removal TPE s effects on hematologic parameters Anticoagulant properties
Apheresis Anticoagulant Removal Oluwatoyosi Onwuemene, MD MS May 6th, 2017 Talk Outline Case presentation Factors associated with drug removal TPE s effects on hematologic parameters Anticoagulant properties
Sign up to receive ATOTW weekly -
 BLOOD PHYSIOLOGY PART 2 ANAESTHESIA TUTORIAL OF THE WEEK 231 11 TH JULY 2011 Dr Karen Hayes Royal Devon & Exeter Correspondence to: kmhayes@hotmail.co.uk QUESTIONS Before continuing, try to answer the
BLOOD PHYSIOLOGY PART 2 ANAESTHESIA TUTORIAL OF THE WEEK 231 11 TH JULY 2011 Dr Karen Hayes Royal Devon & Exeter Correspondence to: kmhayes@hotmail.co.uk QUESTIONS Before continuing, try to answer the
UvA-DARE (Digital Academic Repository) Factor XI as target for antithrombotic therapy van Montfoort, M.L. Link to publication
 UvA-DARE (Digital Academic Repository) Factor XI as target for antithrombotic therapy van Montfoort, M.L. Link to publication Citation for published version (APA): van Montfoort, M. L. (2014). Factor XI
UvA-DARE (Digital Academic Repository) Factor XI as target for antithrombotic therapy van Montfoort, M.L. Link to publication Citation for published version (APA): van Montfoort, M. L. (2014). Factor XI
Dr. Susan Louw Haematopathologist NHLS / WITS / SASTH
 Dr. Susan Louw Haematopathologist NHLS / WITS / SASTH Since 1948 Initially a research tool Utility in management of bleeding and thrombosis Guide clotting factor replacement, platelet / blood transfusions
Dr. Susan Louw Haematopathologist NHLS / WITS / SASTH Since 1948 Initially a research tool Utility in management of bleeding and thrombosis Guide clotting factor replacement, platelet / blood transfusions
Marilyn Johnston Hemostasis Reference Laboratory Hamilton,Ontario
 Marilyn Johnston Hemostasis Reference Laboratory Hamilton,Ontario None Discovered in 1916 Named from the Latin word for liver, hepar 1939, heparin requires a plasma cofactor First used in humans in 1940
Marilyn Johnston Hemostasis Reference Laboratory Hamilton,Ontario None Discovered in 1916 Named from the Latin word for liver, hepar 1939, heparin requires a plasma cofactor First used in humans in 1940
Marcia L. Zucker, Ph.D. ZIVD LLC
 Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway X II Xa LMWH & DXaI IIa (thrombin) Hirudin
Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway X II Xa LMWH & DXaI IIa (thrombin) Hirudin
Pre-analytics in coagulation lab: why struggle for better results?
 Pre-analytics in coagulation lab: why struggle for better results? Valdas Banys, MD, PhD Vilnius University Faculty of Medicine Vilnius University Hospital Santariskiu Klinikos, Center of Laboratory Medicine
Pre-analytics in coagulation lab: why struggle for better results? Valdas Banys, MD, PhD Vilnius University Faculty of Medicine Vilnius University Hospital Santariskiu Klinikos, Center of Laboratory Medicine
Antithrombosis Management for Pediatric VAD and Beyond
 Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
General News. Product Notes
 TO: HELENA POC DISTRIBUTORS FROM: HELENA POINT OF CARE SUBJECT: ROUND-UP/INTERNATIONAL DATE: 8/31/2009 ATTN: ROUNDUP READERS CLINICAL TRIAL SITES NEEDED! As Helena POC continues development of Cascade
TO: HELENA POC DISTRIBUTORS FROM: HELENA POINT OF CARE SUBJECT: ROUND-UP/INTERNATIONAL DATE: 8/31/2009 ATTN: ROUNDUP READERS CLINICAL TRIAL SITES NEEDED! As Helena POC continues development of Cascade
Section 8. To introduce the basic theory and principles of collecting blood for Intraoperative Cell Salvage (ICS)
 Section 8 Practicalities Blood Collection Aim To introduce the basic theory and principles of collecting blood for Intraoperative Cell Salvage (ICS) Learning Outcomes To identify the equipment used for
Section 8 Practicalities Blood Collection Aim To introduce the basic theory and principles of collecting blood for Intraoperative Cell Salvage (ICS) Learning Outcomes To identify the equipment used for
ROZAIMAH ZAIN-HAMID. Department of Pharmacology and Therapeutics Faculty of Medicine, Universitas Sumatera Utara
 ROZAIMAH ZAIN-HAMID Department of Pharmacology and Therapeutics Faculty of Medicine, Universitas Sumatera Utara Drugs Used in Disorders of Coagulation Fibrinolytic drugs Anti-thrombotic thrombotic drugs
ROZAIMAH ZAIN-HAMID Department of Pharmacology and Therapeutics Faculty of Medicine, Universitas Sumatera Utara Drugs Used in Disorders of Coagulation Fibrinolytic drugs Anti-thrombotic thrombotic drugs
HaematologY. Dr Tom Bate Again!
 HaematologY Dr Tom Bate Again! THE FRCA What you need to know Blood Groups ~30 blood group systems recognised (ISBT) ABO, Rhesus, Lewis, Kell, Duffy, Kidd MNS system, Kell system The ABO antigens are the
HaematologY Dr Tom Bate Again! THE FRCA What you need to know Blood Groups ~30 blood group systems recognised (ISBT) ABO, Rhesus, Lewis, Kell, Duffy, Kidd MNS system, Kell system The ABO antigens are the
Sysmex CS-2500 Hemostasis System Unrestricted Siemens Healthcare Diagnostics Inc All rights reserved.
 Excel with Confidence Sysmex CS-2500 Hemostasis System Unrestricted Siemens Healthcare Diagnostics Inc. 2015 All rights reserved. General Lab Challenges Test Volume Financial Performance Accuracy Reliability
Excel with Confidence Sysmex CS-2500 Hemostasis System Unrestricted Siemens Healthcare Diagnostics Inc. 2015 All rights reserved. General Lab Challenges Test Volume Financial Performance Accuracy Reliability
Disseminated Intravascular Coagulopathy
 REVIEW ARTICLE Disseminated Intravascular Coagulopathy Lt Col Rajat Kumar Introduction Disseminated Intravascular Coagulopathy (DIC) is an acquired disorder which, in its mildest form is only an aberration
REVIEW ARTICLE Disseminated Intravascular Coagulopathy Lt Col Rajat Kumar Introduction Disseminated Intravascular Coagulopathy (DIC) is an acquired disorder which, in its mildest form is only an aberration
Managing Coagulation Abnormalities Linda Liu, M.D.
 Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
2009 LAP Audioconference Series. Simple Tests, Tough Problems Patient Care and Laboratory Inspection in Coagulation
 2009 LAP Audioconference Series Simple Tests, Tough Problems Patient Care and Laboratory Objectives: After participating in this session, you will be able to: to describe patient care and accreditation
2009 LAP Audioconference Series Simple Tests, Tough Problems Patient Care and Laboratory Objectives: After participating in this session, you will be able to: to describe patient care and accreditation
ANTICOAGULANT THERAPY ANTICOAGULANT THERAPY REVISITED Thrombosis is a complication of underaggressive anticoagulant therapy
 ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
Automated Coagulation Analyser product list 2018
 Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Automated Coagulation
Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Automated Coagulation
NEW INITIATIVES. Factor XIII, Fibrinolysis, Heparin. Piet Meijer. ECAT Foundation. Leiden The Netherlands
 NEW INITIATIVES Factor XIII, Fibrinolysis, Heparin Piet Meijer ECAT Foundation Leiden The Netherlands DISCLOSURE Relevant Financial Relationship(s) None Off Label Usage None Pilot study on Fibrinolytic
NEW INITIATIVES Factor XIII, Fibrinolysis, Heparin Piet Meijer ECAT Foundation Leiden The Netherlands DISCLOSURE Relevant Financial Relationship(s) None Off Label Usage None Pilot study on Fibrinolytic
Marcia L. Zucker, Ph.D. ZIVD LLC
 Marcia L. Zucker, Ph.D. ZIVD LLC 1 Explain why ACTs from different systems are not the same Develop a plan for switching from one ACT system to another Describe why ACT and aptt are not interchangeable
Marcia L. Zucker, Ph.D. ZIVD LLC 1 Explain why ACTs from different systems are not the same Develop a plan for switching from one ACT system to another Describe why ACT and aptt are not interchangeable
