Principles of dose finding studies in cancer: a comparison of trial designs
|
|
|
- Britton Moody
- 6 years ago
- Views:
Transcription
1 Cancer Chemother Pharmacol (2013) 71: DOI /s REVIEW ARTICLE Principles of dose finding studies in cancer: a comparison of trial designs Thomas Jaki Sally Clive Christopher J. Weir Received: 25 October 2012 / Accepted: 12 December 2012 / Published online: 9 January 2013 Ó The Author(s) This article is published with open access at Springerlink.com Abstract Purpose One key aim of Phase I cancer studies is to identify the dose of a treatment to be further evaluated in Phase II. We describe, in non-statistical language, three classes of dose-escalation trial design and compare their properties. Methods We review three classes of dose-escalation design suitable for Phase I cancer trials: algorithmic approaches (including the popular 3? 3 design), Bayesian model-based designs and Bayesian curve-free methods. We describe an example from each class and summarize the advantages and disadvantages of the design classes. Results The main benefit of algorithmic approaches is the simplicity with which they may be communicated: it may be for this reason alone that they are still employed in the Thomas Jaki, Sally Clive, Christopher J. Weir made equal contributions to the development of this manuscript. The views expressed in this publication are those of the authors and not necessarily those of the UK National Health Service, the UK National Institute for Health Research or the UK Department of Health. T. Jaki Medical and Pharmaceutical Statistics Research Unit, Lancaster University, Lancaster, UK S. Clive Edinburgh Cancer Centre, Western General Hospital, Edinburgh, UK C. J. Weir (&) Medical Research Council Hub for Trials Methodology Research, Centre for Population Health Sciences, University of Edinburgh Medical School, Teviot Place, Edinburgh EH8 9AG, UK Christopher.Weir@ed.ac.uk vast majority of Phase I trials. Model-based and curve-free Bayesian approaches are preferable to algorithmic methods due to their superior ability to identify the dose with the desired toxicity rate and their allocation of a greater proportion of patients to doses at, or close to, that dose. Conclusions For statistical and practical reasons, algorithmic methods cannot be recommended. The choice between a Bayesian model-based or curve-free approach depends on the previous information available about the compound under investigation. If this provides assurance about a particular model form, the model-based approach would be appropriate; if not, the curve-free method would be preferable. Keywords 3? 3 design Bayesian method Clinical trial, Phase I Continual reassessment method CRM Curve free Introduction Ethical considerations [1] require the use of efficient trial designs in order to optimize the balance of risk versus benefit for participants. In Phase I cancer studies, this would include minimizing the numbers of patients allocated to ineffective or excessively toxic doses, while addressing the principal aim of identifying the best dose of a treatment to recommend for further evaluation in a Phase II trial. In this article, we focus on the identification of the maximum tolerated dose (MTD), which remains a key factor in this decision. In practice, additional aspects such as the biological level of anti-cancer activity of a dose would also be considered. The 3? 3 trial design [2, 3], which has been widely implemented, has substantial limitations: we describe two alternative classes of dose-escalation strategy,
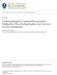
2 1108 Cancer Chemother Pharmacol (2013) 71: using specific examples [4 6] drawn from the many designs available to illustrate their superiority to the 3? 3 design on several relevant study design criteria. Phase I studies play an extremely important role in the development of a cancer treatment as the agent is often given to humans for the first time. As a result, conservative approaches that tend to start at doses much lower than the anticipated highest safe dose and slowly approach the dose of interest from below are usually employed. The population studied is not necessarily the population to be treated and the questions are many despite the subjects being few. Consequently much uncertainty about dose, safety and efficacy will remain afterward. These studies are, however, critical to successful drug development as the decision on whether to continue and the design of any subsequent trials depend on the outcome of this first study. Phase I dose-escalation studies in cancer traditionally enroll late stage patients for whom other therapies have failed. Due to the narrow therapeutic index of cytotoxic drugs and the variable toxicities that may occur at the therapeutic dose of newer targeted anti-cancer drugs, the MTD has been considered a reasonable basis on which to determine an appropriate dose for further clinical use. Hence, in addition to investigating the pharmacokinetics, toxicities and biological activity of a drug, Phase I cancer studies aim to find the MTD, the highest dose that can safely be administered. More precisely, one seeks the dose that has an acceptable risk of dose-limiting toxicity (DLT). In this context, a DLT is a serious adverse event that impairs usual activities and requires therapeutic intervention [7 9]. Late toxicities or lower graded, cumulative or additive toxicities that do not individually meet the DLT criteria also contain information on the safety and activity of a drug; however, the designs used to date do not take account of such events [10]. Advances in this area would clearly have potential to enhance decision making at the end of Phase I. Commonly the dose at which the probability of a DLT is p (for 0 \ p \ 1) is called the TD100p. For example, the TD25 would refer to the dose associated with a 25 % toxicity risk. The rationale for seeking the TD100p is to ensure a safe dose is identified for further study and is based on the common assumption, specifically for cytotoxic compounds, that efficacy increases with toxicity. The latter implies that finding the highest tolerable dose will ensure that the most efficacious dose is investigated subsequently. First, cycle toxicity is a critical and immediate measure that can guide the decision on whether the dose may be escalated safely, and the use of this rather than later efficacy outcomes ensures minimal trial duration. A key ingredient of any dose-escalation study is the set of doses to be explored. Figure 1 illustrates four different dose schedules for a given, hypothetical, dose toxicity relationship. Each graph depicts dose versus toxicity risk and assumes an increasing relationship between them. The arrows indicate the doses available and it is assumed that a toxicity risk of 25 % is acceptable. Figure 1a has very low risk of toxicity for the lower two doses while the upper two doses have a toxicity risk close to 100 %. Such a dose schedule therefore only allows the conclusion that the TD25 lies somewhere between the middle two doses; neither of the doses available is, however, close to the desired toxicity risk. In Fig. 1b, all the doses lie above the desired toxicity level. In this situation, not only does none of the doses have an acceptable toxicity risk, but we cannot even be sure that any dose of the compound is safe. Similarly, if all doses were below the desired TD25, we would not know if any dose corresponded to the TD25 and hence whether a biologically active dose had been attained. Figure 1c shows the advantage of allowing many different doses. It is clear that such a dose schedule allows much more accurate TD25 estimation as the interval between doses is much smaller. While adding doses to allow for more accurate estimation is appealing, doing so requires a different dose-escalation strategy to the commonly employed methods in order to limit the sample size and avoid many patients receiving doses well below those expected to have either toxicity or efficacy. Figure 1d represents an ideal situation where many doses are available, but excessively toxic or ineffective doses represented by lighter shaded arrows are explored less often or possibly even skipped altogether. Traditionally, dose escalation starts at a low dose defined preclinically and slowly escalates dose in decreasing increments according to a predetermined strategy (the modified Fibonacci sequence, in which the dose increments for succeeding dose levels are 100, 67, 50, 40 % then 33 % for all subsequent levels [11]). Alternative escalation strategies [12] include accelerated titration designs [3], pharmacokinetically guided dose escalation [13] and continual reassessment or Bayesian methods [4, 14 16] which have been successfully incorporated into Phase I trial design [17, 18]. From here on, we assume that a sensible selection of doses is available but stress that inclusion of more potential doses within the range of interest may allow more accurate estimation of the highest tolerable dose. To avoid wasting patients at doses that are no longer of interest based on the data gathered so far in the trial, skipping doses [6] or the use of single patients at early dose levels [3] could be considered. There exists a vast literature on dose-escalation methods for Phase I trials in cancer, yet very few of them have been used in practice. By far the most popular approach to dose escalation is the 3? 3 design [2] which, according to Le Tourneau et al. [12], was used in 96.7 % of Phase I trials published in 2007 and A similar finding was made by Rogatko et al. [19] when they investigated the use of
3 Cancer Chemother Pharmacol (2013) 71: (a) (b) toxicity toxicity TD25 dose (c) TD25 dose (d) toxicity toxicity TD25 dose Fig. 1 Schematic illustration of different problems in finding the TD25, the dose at which the underlying risk of dose-limiting toxicity is 25 %. a Four doses, none of which matches the target toxicity rate; (b) six doses, all lying above the desired toxicity level; (c) many TD25 dose doses, allowing accurate estimation of the TD25; (d) many doses, with increased efficiency through less frequent use of excessively toxic or ineffective doses Bayesian designs in Phase I cancer trials. Only 20 (1.6 %) of 1,235 trials followed a Bayesian design despite the existence of around 100 publications demonstrating the statistical properties of such designs. There are three general approaches to dose finding studies in cancer. We will introduce their main features and compare their advantages and disadvantages. In particular, we will show that the most popular design in practice has severe shortcomings when it comes to identifying the dose of interest. Design alternatives Algorithmic approaches Rule-based dose-escalation methods include the Storer upand-down design [3] and the frequently applied 3? 3 design (Fig. 2). Although several variants of this longestablished approach have been published, the earliest source is a book chapter arising from the proceedings of a clinical pharmacology course held in Brussels in May 1972 [2]. The main principle of algorithmic designs is that a small group of patients is treated at a given dose and, dependent on the observed number of toxicities, a decision is made on to whether to study a further group of patients at the next dose up the scale, to study more patients at the same dose or to stop the trial. The 3? 3 design, for example, enters three patients into the trial one at a time at intervals of seven days or more and treats them at the chosen starting dose. The core features of this design, as outlined by Storer [3], are: (a) (b) (c) If no dose-limiting toxicity (DLT) occurs in the first cycle of any of the initial group of 3 patients treated at a dose, the dose should be escalated for the next group of patients. If two or more of the 3 patients treated at a given dose experience a DLT, the trial should stop. If one patient of the 3 treated at a given dose level experiences a DLT, a further 3 patients are treated at
4 1110 Cancer Chemother Pharmacol (2013) 71: Fig. 2 Schematic display of one version of the 3? 3 design New cohort at new dose level: Enrol 3 patients DLT=0/3 DLT=1/3 DLT>1/3 Go to next higher dose level or same dose level if already at highest dose level Enrol 3 additional patients at the same dose level Go to next lower dose level or declare MTD at next lower dose level if 6 patients already tested there DLT=1/6 DLT>1/6 Go to next higher dose level or declare MTD otherwise Go to next lower dose level or declare MTD at next lower dose level if 6 patients already tested there the same dose level. If a DLT has occurred in exactly one of these 6 patients, escalation may continue as in (a); otherwise, the trial should stop. A frequent variation allows the dose to be reduced if more than one DLT is observed within the first three patients studied at a particular dose. Following completion of the trial according to this design, the MTD is defined as either the actual dose at which the trial was stopped or the next lower dose, possibly depending on the frequency and severity of toxicity observed in the patients evaluated in the final group [3]. A number of adaptations of this design attempt to reduce the number of patients treated at the lowest dose levels [20]. Such accelerated titration designs [18, 21] include singlepatient dose levels and more rapid dose escalation (e.g., dose doubling) until the first DLT is observed, after which the dose-escalation scheme would then revert to the modified Fibonacci sequence. Model-based Bayesian methods Bayesian modeling combines prior knowledge of the drug with the observed data from the current trial to provide updated information about the distribution of the trial outcome of interest. Bayesian methods have been incorporated into a number of early phase clinical trial designs, the best known being the continual reassessment method (CRM) [4, 5]. In contrast to the algorithmic approach of the 3? 3 design, the continual reassessment method aims to identify the dose at which the proportion of patients experiencing a DLT reaches a specific target level (e.g., 25 %). Furthermore, the investigator performs repeated analyses on all of the data gathered to date hence the term continual reassessment rather than simply observing the data recorded at the current dose, as is the case for the 3? 3 design. The CRM uses a one-parameter Bayesian model which assumes that the probability of toxic response increases with dose: as we move from one dose up to the next higher dose, the toxicity risk at the higher dose is greater than or equal to that at the previous dose. Before the trial has commenced, Bayesian modeling requires a prior distribution for the dose toxicity curve parameters to be specified [22], representing the expected shape of the dose toxicity relationship. In the original version of the CRM, a simple one-parameter prior distribution is recommended; subsequent developments allow the prior to be informed by data (such as information from pre-clinical studies) or expert opinion (see for example [23] for alternatives). The model may be updated as soon as new data become available on previously included patients. Following this the next patient, or group of patients, is treated at the dose, based on the evidence to date, that has an estimated probability of toxicity closest to the target level.
5 Cancer Chemother Pharmacol (2013) 71: Once all patients have been treated and followed up, the MTD is taken to be the dose at which the estimated toxicity probability is closest to the target level. Although the originally proposed CRM method allows for the initial dose to be above the lowest available dose level, in practice, a modified version that enforces dose escalation to start from the lowest dose [24] is usually employed. Stopping rules have been developed for the CRM [25] to allow early discontinuation of the trial in the situation where all doses are found to be excessively toxic. Alternative Bayesian model-based approaches include escalation with overdose control (EWOC) designs [16] and the TITE-CRM extension of the CRM which allows the trial to be completed more quickly by incorporating time to toxicity event data [26]. Curve-free Bayesian approaches This class of escalation strategies includes work by Gasparini and Eisele [27] and Whitehead et al. [6] and aims to minimize the number of assumptions within the dose toxicity modeling. No assumption is made about the form of the relationship between dose and toxicity except that, as in the CRM, the probability of toxic response increases with dose. The risk of toxicity is modeled directly, resulting in an easy to interpret table of probabilities for each risk level. The possible levels of toxicity risk at a dose are described qualitatively as very safe, safe, ideal, risky or toxic. The numerical probability value that corresponds to each of these descriptors depends on the target toxicity level. The ideal risk category has exactly the target toxicity probability, while the safe and very safe categories have progressively lower risks of toxicity and the risky and toxic categories have progressively higher risks. For example, in a study aiming to identify the dose which has toxicity rate 25 %, the descriptors very safe, safe, ideal, risky and toxic might be assigned the probability values 0.05, 0.15, 0.25, 0.4 and 0.65, respectively. The prior distribution summarizing previous knowledge of the expected risk at each dose level, required under the Bayesian framework, is informed by investigator opinion. As data accumulate during the trial, the updated probabilities of each risk level being associated with each dose are calculated. The dose to be allocated to the next patient enrolled in the trial is selected to avoid doses that have anything other than a small chance of being toxic and to target the dose that has the greatest chance of being ideal. Table 1 illustrates the probabilities of each level of toxicity during a hypothetical trial. Here, 25 % is the target toxicity rate, and dose level 7 is the one with the highest probability of having that toxicity rate. At the end of the trial, one of three approaches may be used to determine which dose to take forward for further study. The first method bases the decision on the final table of updated risk level probabilities. If the dose with a toxicity risk of 25 % was being sought, then the dose with the highest probability of having a toxicity risk of 25 % would be recommended. In the second, perhaps more realistic, strategy, the table of updated risk level probabilities would form just part of the information being considered by investigators when deciding what dose to recommend. The complete study data set will contain far more information than DLT occurrences: pharmacokinetic and clinical data and the expert opinion of investigators could also inform the recommendation. The third approach would be to take the data set and apply any appropriate method of statistical analysis, independently of the dose allocation method used in the trial. Discussion The merits and shortcomings of the three classes of doseescalation procedures introduced above will now be discussed. A broad range of important criteria, including statistical and practical aspects, to consider when evaluating a dose-escalation procedure will be considered under five headings. The weighting for each of the criteria will depend on the specific trial and consequently it is unlikely that each point will carry equal weight across all trials. We have summarized this in Table 2 where we have graded the performance of the dose-escalation procedure for each item under the five headings qualitatively as poor, intermediate, good or not applicable. Statistical properties We expect a good statistical procedure to estimate a specific measure of toxicity and that the precision of this estimate can be gauged. Moreover, we want additional information (i.e., additional patients) to increase the precision in the estimate. Both the model-based and curve-free approach aim to estimate a clear cut measure of toxicity: the dose at which a certain proportion of patients is expected to experience a toxic event. Both methods also quantify the precision of the estimated dose and this precision increases as the sample size increases: they have good statistical properties. Furthermore, were complete information to be available on toxicity of every dose for each patient, the CRM model-based design has performance very close to that of the best design that could exist theoretically [28]. The algorithmic approach, in contrast, tries to find the MTD which is difficult to quantify. As a consequence of
6 1112 Cancer Chemother Pharmacol (2013) 71: Table 1 Example of risk level probabilities generated by the Bayesian curve-free approach Dose level Risk of toxicity 5 % very safe 15 % safe 25 % ideal 40 % risky 65 % toxic Bold value indicates the dose level with the highest probability of having the ideal toxicity rate Table 2 Characteristics of dose-escalation strategies Issues to consider Algorithmic Model based Curve free 1. Statistical properties 1a Does method provide estimate of a relevant parameter and allow Poor Good Good the precision of the estimate to be quantified? 1b Does precision increase with sample size? Poor Good Good 1c Reliably arrives at correct decision on dose with target toxicity risk Poor Good Good 2. Simplicity 2a Non-technical explanation of method Good Poor Intermediate 2b Statistical complexity Not applicable Intermediate Poor 3. Intuitive dose recommendations Good Intermediate Good 4. Flexibility 4a Target toxicity rate Poor Good Good 4b Accommodating underlying shape of dose response Poor Good Good 4c Dose skipping Poor Good Good 5. Impact of number of doses in schedule Poor Good Good this loose definition, it is also impossible to obtain a measure of precision for the MTD. Furthermore, the algorithmic nature of the method means that additional data do not feature in the estimated MTD and the decision about whether a dose is the MTD only depends on what has been observed at this dose level: no learning from the doses above or below is possible. Consequently, algorithmic approaches have very poor statistical properties: the 3? 3 design correctly identifies the dose with toxicity rate closest to the target level less frequently than model-based designs [29] and over the course of the trial exposes many additional patients to doses above or below that optimal dose. Only 35 % of patients are treated at the optimal dose with the 3? 3 design compared to 55 % for Bayesian adaptive designs [19]. We gain insight into this poor performance of the algorithmic design by quantifying the evidence when one out of a group of three patients has experienced a DLT: the 95 % confidence interval (CI) around the best estimate of 33 % for the toxicity rate ranges from 0.8 to 90.6 %, illustrating that little has been learned about the true rate. There is not substantially more evidence even when two of six patients studied at a dose experience a DLT: the corresponding 95 % CI for the toxicity rate is (4.3, 77.7 %). Simplicity The ideal method would be easy to describe to clinicians and be straightforward statistically. The latter criterion does not apply to the algorithmic approach as it is not a statistically derived method. It is, however, the simplest to explain to non-statisticians and may be used without the involvement of a statistician. The Bayesian model-based approach is of moderate statistical complexity, but is easily implemented in practice, in part due to software being readily available (e.g., the R package CRM [30]). A particular challenge that does remain is specifying the prior distributions, which we believe is best done in consultation
7 Cancer Chemother Pharmacol (2013) 71: with a statistician. Finally, the curve-free Bayesian method is relatively simple to explain to non-statisticians (though much more complex than the 3? 3 design) as it directly estimates the risk of each dose rather than using a specific model. The price for this conceptual simplicity is a much more involved statistical process. The contrast between the model-based and the curvefree approaches is that the former requires the dose toxicity model to be specified in advance of the study through discussion between the clinicians and a statistician. Nevertheless, it can still consistently identify the dose that has the desired toxicity rate, even when the model has been misspecified [4, 31]. The curve-free approach only assumes non-decreasing risk of toxicity as dose increases. Although this assumption is often reasonable, the curve-free approach depends on it while a model-based approach could allow for decreases in toxicity risk provided that this was specified in the model. Intuitive dose recommendations The optimal dose-escalation method would recommend doses for subsequent patients or for Phase II trials with which an experienced investigator would be comfortable. In general, all three approaches perform well although it does depend on the exact implementation: the originally proposed CRM [4] does sometimes give a counterintuitive dose recommendation [23] but subsequent modifications have been developed [24] to overcome this. Flexibility In particular, we are interested whether any target toxicity rate can be used, how robust the method is to variations in the true dose toxicity relationship and whether the method can skip doses. The algorithmic approach fairs poorly on all three counts. In its design, the MTD rather than a certain toxicity rate is sought, while dose skipping is prohibited. The dose recommendation only depends on the current dose and hence the underlying dose toxicity relationship is not exploited. The model-based approach on the other hand caters for any toxicity level and, depending on the exact implementation, can allow dose skipping. In addition, any model can be used although it is clear that specifying the correct model before starting the study will sometimes be difficult. As an alternative to modeling the dose toxicity relationship, the model-based approach may also be used in a continual reassessment of pharmacokinetic data [13, 18], pharmacodynamic data [32, 33] or toxicity and efficacy data in combination [34]. The Bayesian curve-free approach may also be applied to combined toxicity and efficacy data [35] (and indeed pharmacodynamic data) if these are binary. As well as allowing any target toxicity rate and dose skipping, the biggest advantage of the curvefree approach is that it is suitable for any underlying dose toxicity relationship provided toxicity increases with dose. This implies that, unlike the model-based approach, the form of the relationship does not have to be specified in advance. Both the model-based and Bayesian curve-free approaches permit single-patient dose cohorts, which can dramatically improve the trial design efficiency. Impact of number of doses in schedule As illustrated in Fig. 1c, a large number of doses allow more precise estimation of the dose of interest although it potentially comes at a price of many patients being treated at sub-optimal doses. With the algorithmic approach, the decision about a dose only depends on what has been observed at this dose level: it does not make use of the information from any of the previous dose levels. In consequence, a large number of doses increase the chance of selecting too safe a dose as even a very safe dose may result in two out of six patients having a DLT [as noted above, the toxicity rate confidence interval in that scenario would be (4.3, 77.7)]. The situation is exacerbated by disallowing skipping of doses and thereby enforcing assessment of every dose incrementally. In contrast, both the model-based and curve-free methods allow dose skipping and use data from all patients in estimating risk of toxicity at each dose level, and so perform well when many doses are available. Conclusion Overall the main benefit of the algorithmic approach is the simplicity of communicating the method and incorporating it into trial protocols and it may be for this reason alone that it is still employed in the vast majority of Phase I trial designs. On the grounds of statistical and other practical considerations, however, it cannot be recommended. The model-based and curve-free approaches have similar merits and are preferable to algorithmic methods due to their superior ability to identify the dose with the desired toxicity rate. Although it is desirable to involve a statistician in the planning of a Phase I oncology trial, Bayesian modelbased methods can readily be implemented by a numerate scientist or clinician. The decision whether a model-based approach is to be used will largely depend on the previous information available about the compound under investigation. Substantial evidence from preclinical studies or studies in different indications regarding the shape of the dose response curve would motivate use of the modelbased approach over the curve-free method. If there is sufficient evidence of high enough quality from previous
8 1114 Cancer Chemother Pharmacol (2013) 71: studies, the model-based approach will be slightly superior to the curve-free one, but if not, resulting in the wrong model, it will perform less well. Acknowledgments This work was supported by a United Kingdom (UK) National Institute for Health Research Career Development Fellowship [NIHR-CDF to T.J.]. C.J.W. was supported in part by the UK Medical Research Council Edinburgh Hub for Trials Methodology Research. The authors thank Professor David Cameron, Professor Duncan Jodrell and two independent reviewers for their constructive suggestions on this manuscript. Conflict of interest interest. The authors have declared no conflicts of Open Access This article is distributed under the terms of the Creative Commons Attribution License which permits any use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited. References 1. Joffe S, Miller FG (2006) Rethinking risk-benefit assessment for phase I clinical trials. J Clin Oncol 24: Carter SK (1973) Study design principles for the clinical evaluation of new drugs as developed by the chemotherapy programme of the National Cancer Institute. In: Staquet MJ (ed) The design of clinical trials in cancer therapy. Futura Publishing Co, Mount Kisco, pp Storer BE (1989) Design and analysis of phase I clinical trials. Biometrics 45: O Quigley J, Pepe M, Fisher L (1990) Continual reassessment method: a practical design for phase I clinical trials in cancer. Biometrics 46: O Quigley J, Chevret S (1991) Methods for dose finding studies in cancer clinical trials: a review and results of a Monte Carlo study. Stat Med 10: Whitehead J, Thygesen H, Whitehead A (2010) A Bayesian dosefinding procedure for phase I clinical trials based only on the assumption of monotonicity. Stat Med 29: Geller NL (1984) Design of phase I and II clinical trials in cancer: a statistician s view. Cancer Invest 2: Eastern Cooperative Oncology Group (2012) org/general/ctc.pdf. Accessed 10 Dec National Cancer Institute (2012) Common terminology criteria for adverse events v Accessed 10 Dec Postel-Vinay S, Gomez-Roca C, Molife LR et al (2011) Phase I trials of molecularly targeted agents: should we pay more attention to late toxicities? J Clin Oncol 29: Hansen HH, Selawry OS, Muggia FM et al (1971) Clinical studies with 1-(2-chloroethyl)-3-cyclohexyl-1-nitrosourea (NSC 79037). Cancer Res 31: Le Tourneau C, Lee JJ, Siu LL (2009) Dose escalation methods in phase I cancer trials. J Natl Cancer Inst 101: Collins JM, Zaharko DS, Dedrick RL et al (1986) Potential roles for preclinical pharmacology in phase I clinical trials. Cancer Treat Rep 70: Tighiouart M, Rogatko A, Babb JS (2005) Flexible Bayesian methods for cancer phase I clinical trials: dose escalation with overdose control. Stat Med 24: Rinaldi DA, Kuhn JG, Burris HA et al (1999) A phase I evaluation of multitargeted antifolate (MTA, LY231514), administered every 21 days, utilizing the modified continual reassessment method for dose escalation. Cancer Chemother Pharmacol 44: Babb J, Rogatko A, Zacks S (1998) Cancer phase I clinical trials: efficient dose escalation with overdose control. Stat Med 17: Dees EC, Whitfield LR, Grove WR et al (2000) A Phase I and pharmacologic evaluation of the DNA intercalator CI-958 in patients with advanced solid tumors. Clin Cancer Res 6: Clive S, Webb DJ, MacLellan J et al (2001) Forearm blood flow and local responses to peptide vasodilators: a NOVEL pharmacodynamic measure in the phase I trial of Antagonist G, a neuropeptide growth factor antagonist. Clin Cancer Res 7: Rogatko A, Schoeneck D, Jonas W et al (2007) Translation of innovative designs into phase I trials. J Clin Oncol 25: Simon RM, Freidlin B, Rubinstein LV et al (1997) Accelerated titration designs for phase I clinical trials in oncology. J Natl Cancer Inst 89: Gadgeel SM, Wozniak A, Boinpally RR et al (2005) Phase I clinical trial of BMS , a derivative of epothilone B, using accelerated titration 2B design. Clin Cancer Res 11: Tighiouart M, Rogatko A (2006) Dose finding in oncology parametric methods. In: Gail M, Krickeberg K, Samet J, Tsiatis A, Wong W (eds) Dose finding in drug development. Springer, New York, pp Neuenschwander B, Branson M, Gsponer T (2008) Critical aspects of the Bayesian approach to phase I cancer trials. Stat Med 27: Goodman SN, Zahurak ML, Piantadosi S (1995) Some practical improvements in the continual reassessment method for phase I studies. Stat Med 14: Zohar S, Chevret S (2001) The continual reassessment method: comparison of Bayesian stopping rules for dose-ranging studies. Stat Med 20: Cheung YK, Chappell R (2000) Sequential designs for phase I clinical trials with late-onset toxicities. Biometrics 56: Gasparini M, Eisele J (2000) A curve-free methods for phase I clinical trials. Biometrics 56: O Quigley J, Paoletti X, Maccario J (2002) Non-parametric optimal design in dose finding studies. Biostatistics 3: Iasonos A, Wilton AS, Riedel ER et al (2008) A comprehensive comparison of the continual reassessment method to the standard 3? 3 dose escalation scheme in phase I dose-finding studies. Clin Trials 5: Mo Q (2012) Accessed 10 Dec Shen LZ, O Quigley J (1996) Consistency of continual reassessment method under model misspecification. Biometrika 83: Calvert AH, Plummer R (2008) The development of Phase I cancer trial methodologies: the use of pharmacokinetic and pharmacodynamic end points sets the scene for Phase 0 cancer clinical trials. Clin Cancer Res 14: Mandrekar SJ, Cui Y, Sargent DJ (2007) An adaptive phase I design for identifying a biologically optimal dose for dual agent drug combinations. Stat Med 26: Zhang W, Sargent DJ, Mandrekar S (2006) An adaptive dosefinding design incorporating both toxicity and efficacy. Stat Med 25: Whitehead J, Thygesen H, Whitehead A (2011) Bayesian procedures for phase I/II clinical trials investigating the safety and efficacy of drug combinations. Stat Med 30:
Non-parametric optimal design in dose finding studies
 Biostatistics (2002), 3, 1,pp. 51 56 Printed in Great Britain Non-parametric optimal design in dose finding studies JOHN O QUIGLEY Department of Mathematics, University of California, San Diego, CA 92093,
Biostatistics (2002), 3, 1,pp. 51 56 Printed in Great Britain Non-parametric optimal design in dose finding studies JOHN O QUIGLEY Department of Mathematics, University of California, San Diego, CA 92093,
Bayesian Approaches to Phase I Clinical Trials:
 Bayesian Approaches to Phase I Clinical Trials: Methodological and Practical Aspects Design of Experiments in Healthcare Isaac Newton Institue of Mathematical Sciences August 2011, Cambridge UK Beat Neuenschwander
Bayesian Approaches to Phase I Clinical Trials: Methodological and Practical Aspects Design of Experiments in Healthcare Isaac Newton Institue of Mathematical Sciences August 2011, Cambridge UK Beat Neuenschwander
PubH 7470: STATISTICS FOR TRANSLATIONAL & CLINICAL RESEARCH
 PubH 7470: STATISTICS FOR TRANSLATIONAL & CLINICAL RESEARCH PHASE I CLINICAL TRIALS: CONTINUAL REASSESSMENT METHOD (CRM) When designing cancer clinical trials for development and evaluation of therapeutic
PubH 7470: STATISTICS FOR TRANSLATIONAL & CLINICAL RESEARCH PHASE I CLINICAL TRIALS: CONTINUAL REASSESSMENT METHOD (CRM) When designing cancer clinical trials for development and evaluation of therapeutic
What does a modified-fibonacci dose-escalation actually correspond to?
 Penel and Kramar BMC Medical Research Methodology 2012, 12:103 RESEARCH ARTICLE Open Access What does a modified-fibonacci dose-escalation actually correspond to? Nicolas Penel 1,2* and Andrew Kramar 1,2
Penel and Kramar BMC Medical Research Methodology 2012, 12:103 RESEARCH ARTICLE Open Access What does a modified-fibonacci dose-escalation actually correspond to? Nicolas Penel 1,2* and Andrew Kramar 1,2
Page 78
 A Case Study for Radiation Therapy Dose Finding Utilizing Bayesian Sequential Trial Design Author s Details: (1) Fuyu Song and (2)(3) Shein-Chung Chow 1 Peking University Clinical Research Institute, Peking
A Case Study for Radiation Therapy Dose Finding Utilizing Bayesian Sequential Trial Design Author s Details: (1) Fuyu Song and (2)(3) Shein-Chung Chow 1 Peking University Clinical Research Institute, Peking
Impact of model complexity on adaptive dose-finding methods
 Impact of model complexity on adaptive dose-finding methods Alexia Iasonos, Ph.D. Memorial Sloan Kettering Cancer Center Nolan A. Wages, Ph.D. University of Virginia Outline Objectives of Phase I or early
Impact of model complexity on adaptive dose-finding methods Alexia Iasonos, Ph.D. Memorial Sloan Kettering Cancer Center Nolan A. Wages, Ph.D. University of Virginia Outline Objectives of Phase I or early
An Adaptive Oncology Dose Finding Trial Using the Time-to-Event Continual Reassessment Method Incorporating Cycle Information
 An Adaptive Oncology Dose Finding Trial Using the Time-to-Event Continual Reassessment Method Incorporating Cycle Information Bo Huang, PhD Oncology Business Unit Pfizer Inc. PhRMA KOL Adaptive Design
An Adaptive Oncology Dose Finding Trial Using the Time-to-Event Continual Reassessment Method Incorporating Cycle Information Bo Huang, PhD Oncology Business Unit Pfizer Inc. PhRMA KOL Adaptive Design
Establish the Maximum Tolerated Dose in Phase-I Trials using 3+3 Method
 Establish the Maximum Tolerated Dose in Phase-I Trials using 3+3 Method Anup Pillai Cytel, Pune, India Vienna 11 th - 14 th October 2015 1 Agenda Ø Introduction to Phase-1 trials Ø Dose Escalation Studies
Establish the Maximum Tolerated Dose in Phase-I Trials using 3+3 Method Anup Pillai Cytel, Pune, India Vienna 11 th - 14 th October 2015 1 Agenda Ø Introduction to Phase-1 trials Ø Dose Escalation Studies
Coherence in early phase dose-finding studies Ken Cheung Dept of Biostatistics Columbia University
 Coherence in early phase dose-finding studies Ken Cheung Dept of Biostatistics Columbia University Agenda Motivation Phase I cancer trials The conventional method ( 3+3 ) Literature: review & critique
Coherence in early phase dose-finding studies Ken Cheung Dept of Biostatistics Columbia University Agenda Motivation Phase I cancer trials The conventional method ( 3+3 ) Literature: review & critique
Improving Safety of the Continual Reassessment Method via a Modified Allocation Rule
 arxiv:1807.05781v1 [stat.me] 16 Jul 2018 Improving Safety of the Continual Reassessment Method via a Modified Allocation Rule Pavel Mozgunov and Thomas Jaki Department of Mathematics and Statistics, Lancaster
arxiv:1807.05781v1 [stat.me] 16 Jul 2018 Improving Safety of the Continual Reassessment Method via a Modified Allocation Rule Pavel Mozgunov and Thomas Jaki Department of Mathematics and Statistics, Lancaster
Bayesian Designs for Clinical Trials in Early Drug Development
 Vol. 3, No. 6, June 007 Can You Handle the Truth? Bayesian Designs for Clinical Trials in Early Drug Development By St. Clare Chung and Miklos Schulz Introduction A clinical trial is designed to answer
Vol. 3, No. 6, June 007 Can You Handle the Truth? Bayesian Designs for Clinical Trials in Early Drug Development By St. Clare Chung and Miklos Schulz Introduction A clinical trial is designed to answer
Cancer phase I trial design using drug combinations when a fraction of dose limiting toxicities is attributable to one or more agents
 Cancer phase I trial design using drug combinations when a fraction of dose limiting toxicities is attributable to one or more agents arxiv:1709.00918v3 [stat.me] 22 Aug 2018 José L. Jiménez 1, Mourad
Cancer phase I trial design using drug combinations when a fraction of dose limiting toxicities is attributable to one or more agents arxiv:1709.00918v3 [stat.me] 22 Aug 2018 José L. Jiménez 1, Mourad
Model-based Designs in Oncology Dose Finding Studies
 Cytel Workshop 2015 Model-based Designs in Oncology Dose Finding Studies Ling Wang Overview of Oncology Dose Finding Studies Oncology is a special therapeutic area in which dose finding studies, including
Cytel Workshop 2015 Model-based Designs in Oncology Dose Finding Studies Ling Wang Overview of Oncology Dose Finding Studies Oncology is a special therapeutic area in which dose finding studies, including
Daniel Sabanés Bové (presented by Giuseppe Palermo)
 Model-based D/E designs: Current status and next steps Basel Biometrics Society Seminar, 26 June 2017 Daniel Sabanés Bové (presented by Giuseppe Palermo) Background of early phase clinical trials Main
Model-based D/E designs: Current status and next steps Basel Biometrics Society Seminar, 26 June 2017 Daniel Sabanés Bové (presented by Giuseppe Palermo) Background of early phase clinical trials Main
Understanding the Continual Reassessment Method for Dose Finding Studies: An Overview for Non-Statisticians
 Johns Hopkins University, Dept. of Biostatistics Working Papers 3-3-2005 Understanding the Continual Reassessment Method for Dose Finding Studies: An Overview for Non-Statisticians Elizabeth Garrett-Mayer
Johns Hopkins University, Dept. of Biostatistics Working Papers 3-3-2005 Understanding the Continual Reassessment Method for Dose Finding Studies: An Overview for Non-Statisticians Elizabeth Garrett-Mayer
Adaptive Design for Clinical Trials
 Adaptive Design for Clinical Trials Mark Chang Millennium Pharmaceuticals, Inc., Cambridge, MA 02139,USA (e-mail: Mark.Chang@Statisticians.org) Abstract. Adaptive design is a trial design that allows modifications
Adaptive Design for Clinical Trials Mark Chang Millennium Pharmaceuticals, Inc., Cambridge, MA 02139,USA (e-mail: Mark.Chang@Statisticians.org) Abstract. Adaptive design is a trial design that allows modifications
Continual Reassessment Method for First-in-Human Trial: From Design to Trial Implementation
 Continual Reassessment Method for First-in-Human Trial: From Design to Trial Implementation Inna Perevozskaya Statistical Research and Consulting Center, Pfizer in collaboration with Lixin Han, Infinity
Continual Reassessment Method for First-in-Human Trial: From Design to Trial Implementation Inna Perevozskaya Statistical Research and Consulting Center, Pfizer in collaboration with Lixin Han, Infinity
Interactive Software Isotonic Design using Normalized Equivalent Toxicity Score (ID-NETS TM) for Cancer Phase I Clinical Trials
 Interactive Software Isotonic Design using Normalized Equivalent Toxicity Score (ID-NETS TM) for Cancer Phase I Clinical Trials Zhengjia Chen, Emory University Zhibo Wang, Emory University Haibin Wang,
Interactive Software Isotonic Design using Normalized Equivalent Toxicity Score (ID-NETS TM) for Cancer Phase I Clinical Trials Zhengjia Chen, Emory University Zhibo Wang, Emory University Haibin Wang,
A likelihood-based approach to selecting doses with acceptable toxicity in a standard phase I algorithm
 A likelihood-based approach to selecting doses with acceptable toxicity in a standard phase I algorithm Cody Chiuzan, Elizabeth Garrett-Mayer Department of Public Health Sciences Medical University of
A likelihood-based approach to selecting doses with acceptable toxicity in a standard phase I algorithm Cody Chiuzan, Elizabeth Garrett-Mayer Department of Public Health Sciences Medical University of
Bayesian modelling for combination dose-escalation trial that incorporates pharmacokinetic data
 Bayesian modelling for combination dose-escalation trial that incorporates pharmacokinetic data Daniel Lorand (Oncology Early Clinical Biostatistics, Novartis) Basel Biometrics Society Seminar - April
Bayesian modelling for combination dose-escalation trial that incorporates pharmacokinetic data Daniel Lorand (Oncology Early Clinical Biostatistics, Novartis) Basel Biometrics Society Seminar - April
ORGANIZATION AND ROLE OF A PHASE I ONCOLOGY UNIT. Dr Philippe CASSIER Centre Léon Bérard, Lyon
 ORGANIZATION AND ROLE OF A PHASE I ONCOLOGY UNIT Dr Philippe CASSIER Centre Léon Bérard, Lyon Outline Cancer & Oncology Drug development in oncology Specificity of phase I trials in oncology Study design
ORGANIZATION AND ROLE OF A PHASE I ONCOLOGY UNIT Dr Philippe CASSIER Centre Léon Bérard, Lyon Outline Cancer & Oncology Drug development in oncology Specificity of phase I trials in oncology Study design
Novel Bayesian Adaptive Designs for Early Phase Oncology Clinical Trials
 Novel Bayesian Adaptive Designs for Early Phase Oncology Clinical Trials A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Kristen M. Cunanan IN PARTIAL FULFILLMENT
Novel Bayesian Adaptive Designs for Early Phase Oncology Clinical Trials A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Kristen M. Cunanan IN PARTIAL FULFILLMENT
Dose Finding & Strategies for Novel Combination Development
 Dose Finding & Strategies for Novel Combination Development Drug Development Paradigm in Oncology NAM NCPF & Forum on Drug Discovery 12-13 December 2016 Steven Piantadosi, M.D., Ph.D. Phase One Foundation
Dose Finding & Strategies for Novel Combination Development Drug Development Paradigm in Oncology NAM NCPF & Forum on Drug Discovery 12-13 December 2016 Steven Piantadosi, M.D., Ph.D. Phase One Foundation
A toxicity-dependent feasibility bound for the Escalation with Overdose Control approach in phase I cancer trials
 A toxicity-dependent feasibility bound for the Escalation with Overdose Control approach in phase I cancer trials Graham Wheeler 1,2 Michael Sweeting 3 Adrian Mander 2 1 Cancer Research UK & UCL Cancer
A toxicity-dependent feasibility bound for the Escalation with Overdose Control approach in phase I cancer trials Graham Wheeler 1,2 Michael Sweeting 3 Adrian Mander 2 1 Cancer Research UK & UCL Cancer
BIOSTATISTICAL METHODS
 BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH Phase 0 Trials: EARLY-PHASE CLINICAL TRIALS Steps to New Drug Discovery Get idea for drug target Develop a bioassay Screen chemical compounds
BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH Phase 0 Trials: EARLY-PHASE CLINICAL TRIALS Steps to New Drug Discovery Get idea for drug target Develop a bioassay Screen chemical compounds
BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH
 BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH Phase 0 Trials: EARLY-PHASE CLINICAL TRIALS CLINICAL PHASE Clinical Studies: Class of all scientific approaches to evaluate Disease Prevention,
BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH Phase 0 Trials: EARLY-PHASE CLINICAL TRIALS CLINICAL PHASE Clinical Studies: Class of all scientific approaches to evaluate Disease Prevention,
BAYESIAN DATA AUGMENTATION DOSE FINDING WITH CONTINUAL REASSESSMENT METHOD AND DELAYED TOXICITY
 BAYESIAN DATA AUGMENTATION DOSE FINDING WITH CONTINUAL REASSESSMENT METHOD AND DELAYED TOXICITY BY SUYU LIU, GUOSHENG YIN,1 AND YING YUAN,2 MD Anderson Cancer Center and University of Hong Kong A major
BAYESIAN DATA AUGMENTATION DOSE FINDING WITH CONTINUAL REASSESSMENT METHOD AND DELAYED TOXICITY BY SUYU LIU, GUOSHENG YIN,1 AND YING YUAN,2 MD Anderson Cancer Center and University of Hong Kong A major
Novel Methods for. Early Phase Clinical Trials
 Novel Methods for Early Phase Clinical Trials Amy Louise Cotterill, B.Sc., M.Sc. Submitted for the degree of Doctor of Philosophy at Lancaster University. August 21, 2015 Novel Methods for Early Phase
Novel Methods for Early Phase Clinical Trials Amy Louise Cotterill, B.Sc., M.Sc. Submitted for the degree of Doctor of Philosophy at Lancaster University. August 21, 2015 Novel Methods for Early Phase
Draft agreed by Scientific Advice Working Party 5 September Adopted by CHMP for release for consultation 19 September
 23 January 2014 EMA/CHMP/SAWP/757052/2013 Committee for Medicinal Products for Human Use (CHMP) Qualification Opinion of MCP-Mod as an efficient statistical methodology for model-based design and analysis
23 January 2014 EMA/CHMP/SAWP/757052/2013 Committee for Medicinal Products for Human Use (CHMP) Qualification Opinion of MCP-Mod as an efficient statistical methodology for model-based design and analysis
The Promise and Challenge of Adaptive Design in Oncology Trials
 THE POWER OFx Experts. Experience. Execution. The Promise and Challenge of Adaptive Design in Oncology Trials Clinical oncology trials are more complex and time consuming than those in any other therapeutic
THE POWER OFx Experts. Experience. Execution. The Promise and Challenge of Adaptive Design in Oncology Trials Clinical oncology trials are more complex and time consuming than those in any other therapeutic
BOIN: A Novel Platform for Designing Early Phase Clinical Tri
 BOIN: A Novel Platform for Designing Early Phase Clinical Trials Department of Biostatistics The University of Texas, MD Anderson Cancer Center Outline Introduction Bayesian optimal interval (BOIN) designs
BOIN: A Novel Platform for Designing Early Phase Clinical Trials Department of Biostatistics The University of Texas, MD Anderson Cancer Center Outline Introduction Bayesian optimal interval (BOIN) designs
3+3 Consensus Meeting Introducing Model Based Dose Escalation in a Pharmaceutical Environment. James Matcham Head, ECD Biometrics 3 rd December 2014
 3+3 Consensus Meeting Introducing Model Based Dose Escalation in a Pharmaceutical Environment James Matcham Head, ECD Biometrics 3 rd December 2014 Agenda Background Challenge Actions Outcome 2 JMatcham
3+3 Consensus Meeting Introducing Model Based Dose Escalation in a Pharmaceutical Environment James Matcham Head, ECD Biometrics 3 rd December 2014 Agenda Background Challenge Actions Outcome 2 JMatcham
A Life-cycle Approach to Dose Finding Studies
 A Life-cycle Approach to Dose Finding Studies Rajeshwari Sridhara, Ph.D. Director, Division of Biometrics V Center for Drug Evaluation and Research, USFDA This presentation reflects the views of the author
A Life-cycle Approach to Dose Finding Studies Rajeshwari Sridhara, Ph.D. Director, Division of Biometrics V Center for Drug Evaluation and Research, USFDA This presentation reflects the views of the author
Single and Double Agent Oncology Dose-Escalation Designs in East 6.4: A communication tool. Shaping the Future of Drug Development
 Shaping the Future of Drug Development Single and Double Agent Oncology Dose-Escalation Designs in East 6.4: A communication tool Pantelis Vlachos, Ph.D. Cytel Inc. Geneva Agenda What s new? Single- Agent
Shaping the Future of Drug Development Single and Double Agent Oncology Dose-Escalation Designs in East 6.4: A communication tool Pantelis Vlachos, Ph.D. Cytel Inc. Geneva Agenda What s new? Single- Agent
Flexible early-phase design for combination therapies
 Flexible early-phase design for combination therapies Nolan A. Wages, PhD Associate Professor Department of Public Health Sciences University of Virginia May 30, 2018 Nolan A. Wages, PhD (UVA) The 2nd
Flexible early-phase design for combination therapies Nolan A. Wages, PhD Associate Professor Department of Public Health Sciences University of Virginia May 30, 2018 Nolan A. Wages, PhD (UVA) The 2nd
A robust Bayesian dose-finding design for phase I/II clinical trials
 Biostatistics (2016), 17,2,pp. 249 263 doi:10.1093/biostatistics/kxv040 Advance Access publication on October 20, 2015 A robust Bayesian dose-finding design for phase I/II clinical trials SUYU LIU Department
Biostatistics (2016), 17,2,pp. 249 263 doi:10.1093/biostatistics/kxv040 Advance Access publication on October 20, 2015 A robust Bayesian dose-finding design for phase I/II clinical trials SUYU LIU Department
Bayesian Designs for Early Phase Clinical Trials
 Bayesian Designs for Early Phase Clinical Trials Peter F. Thall, PhD Department of Biostatistics M.D. Anderson Cancer Center Fourteenth International Kidney Cancer Symposium Miami, Florida, November 6-7,
Bayesian Designs for Early Phase Clinical Trials Peter F. Thall, PhD Department of Biostatistics M.D. Anderson Cancer Center Fourteenth International Kidney Cancer Symposium Miami, Florida, November 6-7,
What s New in GCP? FDA Draft Guidance Details FIH Multiple Cohort Trials
 Vol. 14, No. 10, October 2018 Happy Trials to You What s New in GCP? FDA Draft Guidance Details FIH Multiple Cohort Trials While multiple, concurrently accruing patient cohorts in first-in-human (FIH)
Vol. 14, No. 10, October 2018 Happy Trials to You What s New in GCP? FDA Draft Guidance Details FIH Multiple Cohort Trials While multiple, concurrently accruing patient cohorts in first-in-human (FIH)
PRACTICAL EXTENSIONS OF THE CONTINUAL REASSESSMENT METHOD AMBER R. SALTER
 PRACTICAL EXTENSIONS OF THE CONTINUAL REASSESSMENT METHOD by AMBER R. SALTER INMACULADA B. ABAN, CHAIR GARY CUTTER CHARITY MORGAN JOHN O QUIGLEY JOHN RINKER A DISSERTATION Submitted to the graduate faculty
PRACTICAL EXTENSIONS OF THE CONTINUAL REASSESSMENT METHOD by AMBER R. SALTER INMACULADA B. ABAN, CHAIR GARY CUTTER CHARITY MORGAN JOHN O QUIGLEY JOHN RINKER A DISSERTATION Submitted to the graduate faculty
Advanced Designs of Cancer Phase I and Phase II Clinical Trials
 Georgia State University ScholarWorks @ Georgia State University Mathematics Dissertations Department of Mathematics and Statistics Spring 5-13-2013 Advanced Designs of Cancer Phase I and Phase II Clinical
Georgia State University ScholarWorks @ Georgia State University Mathematics Dissertations Department of Mathematics and Statistics Spring 5-13-2013 Advanced Designs of Cancer Phase I and Phase II Clinical
Three Methods for Phase I/II Clinical Trials, with Application to Allogeneic
 Three Methods for Phase I/II Clinical Trials, with Application to Allogeneic Stem Cell Transplantation Peter F. Thall, PhD Biostatistics Department M.D. Anderson Cancer Center Workshop on Clinical Trial
Three Methods for Phase I/II Clinical Trials, with Application to Allogeneic Stem Cell Transplantation Peter F. Thall, PhD Biostatistics Department M.D. Anderson Cancer Center Workshop on Clinical Trial
arxiv: v1 [stat.ap] 8 Jan 2014
![arxiv: v1 [stat.ap] 8 Jan 2014 arxiv: v1 [stat.ap] 8 Jan 2014](/thumbs/88/115075223.jpg) The Annals of Applied Statistics 2013, Vol. 7, No. 4, 2138 2156 DOI: 10.1214/13-AOAS661 c Institute of Mathematical Statistics, 2013 arxiv:1401.1706v1 [stat.ap] 8 Jan 2014 BAYESIAN DATA AUGMENTATION DOSE
The Annals of Applied Statistics 2013, Vol. 7, No. 4, 2138 2156 DOI: 10.1214/13-AOAS661 c Institute of Mathematical Statistics, 2013 arxiv:1401.1706v1 [stat.ap] 8 Jan 2014 BAYESIAN DATA AUGMENTATION DOSE
The Promise of Novel Clinical Trial Designs. Michael Parides, Ph.D. Mount Sinai School of Medicine
 The Promise of Novel Clinical Trial Designs Michael Parides, Ph.D. Mount Sinai School of Medicine Productivity New Drug Approvals (NMEs) R&D Spending (billions) $12 $13 $13 $15 $49 $38 $39 $43 $30 $32
The Promise of Novel Clinical Trial Designs Michael Parides, Ph.D. Mount Sinai School of Medicine Productivity New Drug Approvals (NMEs) R&D Spending (billions) $12 $13 $13 $15 $49 $38 $39 $43 $30 $32
Research Article Escalation with Overdose Control Using Ordinal Toxicity Grades for Cancer Phase I Clinical Trials
 Journal of and Statistics Volume 22, Article ID 37634, 8 pages doi:.55/22/37634 Research Article Escalation with Overdose Control Using Ordinal Toxicity Grades for Cancer Phase I Clinical Trials Mourad
Journal of and Statistics Volume 22, Article ID 37634, 8 pages doi:.55/22/37634 Research Article Escalation with Overdose Control Using Ordinal Toxicity Grades for Cancer Phase I Clinical Trials Mourad
Oncology New Drug Development. Tomoyuki Kakizume Novartis Pharma K.K. Oncology Biometrics and Data Management Dept.
 Novartis: Challenging to Accelerate Oncology New Drug Development Tomoyuki Kakizume Novartis Pharma K.K. Oncology Biometrics and Data Management Dept. Bayesian Clinical Trials in Novartis Oncology Phase
Novartis: Challenging to Accelerate Oncology New Drug Development Tomoyuki Kakizume Novartis Pharma K.K. Oncology Biometrics and Data Management Dept. Bayesian Clinical Trials in Novartis Oncology Phase
Jim Bolognese, Cytel Inc. 05Nov2015
 Modified Toxicity Probability Intervals (mtpi), Bayesian Logistic Regression Modeling (BLRM), Continual Reassessment Method (CRM) via EAST6.3.1 vs. T-statistic (Tstat) Design via COMPASS for finding MTD
Modified Toxicity Probability Intervals (mtpi), Bayesian Logistic Regression Modeling (BLRM), Continual Reassessment Method (CRM) via EAST6.3.1 vs. T-statistic (Tstat) Design via COMPASS for finding MTD
Models for Computer-Aided Trial & Program Design
 Models for Computer-Aided Trial & Program Design Terrence Blaschke, M.D. VP, Methodology and Science Pharsight Corporation & Professor of Medicine & Molecular Pharmacology Stanford University MODELS What
Models for Computer-Aided Trial & Program Design Terrence Blaschke, M.D. VP, Methodology and Science Pharsight Corporation & Professor of Medicine & Molecular Pharmacology Stanford University MODELS What
PART I. Clinical Trials COPYRIGHTED MATERIAL
 PART I Clinical Trials COPYRIGHTED MATERIAL CHAPTER 1 Phase I Clinical Trials Anastasia Ivanova Department of Biostatistics, University of North Carolina, Chapel Hill, North Carolina Nancy Flournoy Department
PART I Clinical Trials COPYRIGHTED MATERIAL CHAPTER 1 Phase I Clinical Trials Anastasia Ivanova Department of Biostatistics, University of North Carolina, Chapel Hill, North Carolina Nancy Flournoy Department
Statistical Methods for Bayesian Adaptive Early-Phase Clinical Trial Designs
 Statistical Methods for Bayesian Adaptive Early-Phase Clinical Trial Designs by Jin Zhang A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy (Biostatistics)
Statistical Methods for Bayesian Adaptive Early-Phase Clinical Trial Designs by Jin Zhang A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy (Biostatistics)
A Latent Contingency Table Approach to Dose Finding for Combinations of Two Agents
 Biometrics 65, 866 875 September 2009 DOI: 10.1111/j.1541-0420.2008.01119.x A Latent Contingency Table Approach to Dose Finding for Combinations of Two Agents Guosheng Yin and Ying Yuan Department of Biostatistics,
Biometrics 65, 866 875 September 2009 DOI: 10.1111/j.1541-0420.2008.01119.x A Latent Contingency Table Approach to Dose Finding for Combinations of Two Agents Guosheng Yin and Ying Yuan Department of Biostatistics,
Formalizing Study Design & Writing Your Protocol. Manish A. Shah, MD Weill Cornell Medicine Center for Advanced Digestive Care
 TWIST: Formalizing Study Design & Writing Your Protocol Manish A. Shah, MD Weill Cornell Medicine Center for Advanced Digestive Care Presented by the Joint Clinical Trials Office/Quality Assurance Unit
TWIST: Formalizing Study Design & Writing Your Protocol Manish A. Shah, MD Weill Cornell Medicine Center for Advanced Digestive Care Presented by the Joint Clinical Trials Office/Quality Assurance Unit
Package pocrm. R topics documented: March 3, 2018
 Package pocrm March 3, 2018 Type Package Title Dose Finding in Drug Combination Phase I Trials Using PO-CRM Version 0.11 Date 2018-03-02 Author Nolan A. Wages Maintainer ``Varhegyi, Nikole E. (nev4g)''
Package pocrm March 3, 2018 Type Package Title Dose Finding in Drug Combination Phase I Trials Using PO-CRM Version 0.11 Date 2018-03-02 Author Nolan A. Wages Maintainer ``Varhegyi, Nikole E. (nev4g)''
Continuous Safety Monitoring in Large Phase I Cancer Clinical Trials with Multiple Expansion Cohorts
 Continuous Safety Monitoring in Large Phase I Cancer Clinical Trials with Multiple Expansion Cohorts Masha Kocherginsky, PhD 1 Theodore Karrison, PhD 2 1 Northwestern University and 2 The University of
Continuous Safety Monitoring in Large Phase I Cancer Clinical Trials with Multiple Expansion Cohorts Masha Kocherginsky, PhD 1 Theodore Karrison, PhD 2 1 Northwestern University and 2 The University of
Guiding dose escalation studies in Phase 1 with unblinded modeling
 Guiding dose escalation studies in Phase 1 with unblinded modeling Andreas Krause Lead Scientist Modeling & Simulation Andreas.Krause@idorsia.com Basel Biometrics Section (BBS) Seminar: Innovative model-based
Guiding dose escalation studies in Phase 1 with unblinded modeling Andreas Krause Lead Scientist Modeling & Simulation Andreas.Krause@idorsia.com Basel Biometrics Section (BBS) Seminar: Innovative model-based
Bayesian interval dose-finding designs: Methodology and Application
 Bayesian interval dose-finding designs: Methodology and Application May 29, 2018 Conflict of Interests The U-Design webtool is developed and hosted by Laiya Consulting, Inc., a statistical consulting firm
Bayesian interval dose-finding designs: Methodology and Application May 29, 2018 Conflict of Interests The U-Design webtool is developed and hosted by Laiya Consulting, Inc., a statistical consulting firm
Adaptive Designs for Identifying Optimal Biological Dose for Molecularly Targeted Agents
 Adaptive Designs for Identifying Optimal Biological Dose for Molecularly Targeted Agents Yong Zang, J Jack Lee and Ying Yuan Department of Biostatistics, The University of Texas M. D. Anderson Cancer Center,
Adaptive Designs for Identifying Optimal Biological Dose for Molecularly Targeted Agents Yong Zang, J Jack Lee and Ying Yuan Department of Biostatistics, The University of Texas M. D. Anderson Cancer Center,
SEARS: A Seamless Dose Escalation/Expansion with Adaptive Randomization Scheme
 SEARS: A Seamless Dose Escalation/Expansion with Adaptive Randomization Scheme Haitao Pan 1,2, Fang Xie 4, Ping Liu 5, Jielai Xia 1,, Yuan Ji 3, March 7, 2012 1 Department of Health Statistics, Fourth
SEARS: A Seamless Dose Escalation/Expansion with Adaptive Randomization Scheme Haitao Pan 1,2, Fang Xie 4, Ping Liu 5, Jielai Xia 1,, Yuan Ji 3, March 7, 2012 1 Department of Health Statistics, Fourth
Genomics And Pharmacogenomics In Anticancer Drug Development And Clinical Response (Cancer Drug Discovery And Development)
 Genomics And Pharmacogenomics In Anticancer Drug Development And Clinical Response (Cancer Drug Discovery And Development) Strategies for modern biomarker and drug - Oct 3, 2014 Sequencing the cancer genome
Genomics And Pharmacogenomics In Anticancer Drug Development And Clinical Response (Cancer Drug Discovery And Development) Strategies for modern biomarker and drug - Oct 3, 2014 Sequencing the cancer genome
SIMULATION EXPERIMENT PLATFORM FOR EVALUATING CLINICAL TRIAL DESIGNS, WITH APPLICATIONS TO PHASE I DOSE-FINDING CLINICAL TRIALS.
 SIMULATION EXPERIMENT PLATFORM FOR EVALUATING CLINICAL TRIAL DESIGNS, WITH APPLICATIONS TO PHASE I DOSE-FINDING CLINICAL TRIALS by Yuanyuan Wang BS, University of Science and Technology of China, China,
SIMULATION EXPERIMENT PLATFORM FOR EVALUATING CLINICAL TRIAL DESIGNS, WITH APPLICATIONS TO PHASE I DOSE-FINDING CLINICAL TRIALS by Yuanyuan Wang BS, University of Science and Technology of China, China,
Disclaimer This presentation expresses my personal views on this topic and must not be interpreted as the regulatory views or the policy of the FDA
 On multiplicity problems related to multiple endpoints of controlled clinical trials Mohammad F. Huque, Ph.D. Div of Biometrics IV, Office of Biostatistics OTS, CDER/FDA JSM, Vancouver, August 2010 Disclaimer
On multiplicity problems related to multiple endpoints of controlled clinical trials Mohammad F. Huque, Ph.D. Div of Biometrics IV, Office of Biostatistics OTS, CDER/FDA JSM, Vancouver, August 2010 Disclaimer
Optimizing Phase 1 and 2 Clinical Trials Design. Stephanie Green and Tao Wang
 Optimizing Phase 1 and 2 Clinical Trials Design Stephanie Green and Tao Wang 1 Phase 1 options OUTLINE Improve efficiency over 3+3 Use other designs if standard assumptions are not met Phase 1 2 strategy
Optimizing Phase 1 and 2 Clinical Trials Design Stephanie Green and Tao Wang 1 Phase 1 options OUTLINE Improve efficiency over 3+3 Use other designs if standard assumptions are not met Phase 1 2 strategy
PHASE 1, MULTICENTER, OPEN-LABEL STUDY OF SINGLE-AGENT BISPECIFIC ANTIBODY T CELL ENGAGER GBR 1342 IN RELAPSED/REFRACTORY MULTIPLE MYELOMA
 PHASE 1, MULTICENTER, OPEN-LABEL STUDY OF SINGLE-AGENT BISPECIFIC ANTIBODY T CELL ENGAGER GBR 1342 IN RELAPSED/REFRACTORY MULTIPLE MYELOMA JOSHUA RICHTER 1 ; OLA LANDGREN 2 ; JOHN KAUH 3 ; JONATHAN BACK
PHASE 1, MULTICENTER, OPEN-LABEL STUDY OF SINGLE-AGENT BISPECIFIC ANTIBODY T CELL ENGAGER GBR 1342 IN RELAPSED/REFRACTORY MULTIPLE MYELOMA JOSHUA RICHTER 1 ; OLA LANDGREN 2 ; JOHN KAUH 3 ; JONATHAN BACK
A Constrained Optimum Adaptive Design for Dose Finding in Early Phase Clinical Trials
 A Constrained Optimum Adaptive Design for Finding in Early Phase Clinical Trials Iftakhar Alam Barbara Bogacka Steve Coad School of Mathematical Sciences Queen Mary University of London m.alam@qmul.ac.uk
A Constrained Optimum Adaptive Design for Finding in Early Phase Clinical Trials Iftakhar Alam Barbara Bogacka Steve Coad School of Mathematical Sciences Queen Mary University of London m.alam@qmul.ac.uk
When to Stop Dose Escalation: MTD, MLD or?
 When to Stop Dose Escalation: MTD, MLD or? Henri CAPLAIN First Joint Annual Meeting, AGAH Club Phase 1 STRASBOURG, France 1 So called MTD STOP FIM No MTD? 2 WHY WE NEED TO REACH THE MAXIMUM TOLERATED DOSE
When to Stop Dose Escalation: MTD, MLD or? Henri CAPLAIN First Joint Annual Meeting, AGAH Club Phase 1 STRASBOURG, France 1 So called MTD STOP FIM No MTD? 2 WHY WE NEED TO REACH THE MAXIMUM TOLERATED DOSE
S9 Nonclinical Evaluation for Anticancer Pharmaceuticals
 S9 Nonclinical Evaluation for Anticancer Pharmaceuticals This draft guidance, when finalized, will represent the Food and Drug Administration's (FDA's) current thinking on this topic. It does not create
S9 Nonclinical Evaluation for Anticancer Pharmaceuticals This draft guidance, when finalized, will represent the Food and Drug Administration's (FDA's) current thinking on this topic. It does not create
Methods in Clinical Cancer Research Workshop Format for Protocol Concept Synopsis Sheet (blank) SYNOPSIS
 B Methods in Clinical Cancer Research Workshop Format for Protocol Concept Synopsis Sheet (blank) elow is the format to follow for the concept sheet for protocols. It is based on the International Committee
B Methods in Clinical Cancer Research Workshop Format for Protocol Concept Synopsis Sheet (blank) elow is the format to follow for the concept sheet for protocols. It is based on the International Committee
Recommendation on elements required to support the medical plausibility and the assumption of significant benefit for an orphan designation
 2 March 2010 EMA/COMP/15893/2009 Final Committee for Orphan Medicinal Products (COMP) Recommendation on elements required to support the medical plausibility and the assumption of significant benefit for
2 March 2010 EMA/COMP/15893/2009 Final Committee for Orphan Medicinal Products (COMP) Recommendation on elements required to support the medical plausibility and the assumption of significant benefit for
The Integrated Web Portal for Escalation with Overdose Control (EWOC)
 Send Orders of Reprints at reprints@benthamscience.net 18 The Open Medical Informatics Journal, 2013, 7, 18-23 Open Access The Integrated Web Portal for Escalation with Overdose Control (EWOC) Haibin Wang
Send Orders of Reprints at reprints@benthamscience.net 18 The Open Medical Informatics Journal, 2013, 7, 18-23 Open Access The Integrated Web Portal for Escalation with Overdose Control (EWOC) Haibin Wang
BIOSTATISTICAL METHODS
 BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH Combination Chemotherapy: DESIGNING CLINICAL RESEARCH Use of a combination of two therapeutics, especially drug-drug combination (called combination
BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH Combination Chemotherapy: DESIGNING CLINICAL RESEARCH Use of a combination of two therapeutics, especially drug-drug combination (called combination
Adaptive Model-Based Designs in Clinical Drug Development. Vlad Dragalin Global Biostatistics and Programming Wyeth Research
 Adaptive Model-Based Designs in Clinical Drug Development Vlad Dragalin Global Biostatistics and Programming Wyeth Research 2007 Rutgers Biostatistics Day February 16, 2007 Outline Definition and general
Adaptive Model-Based Designs in Clinical Drug Development Vlad Dragalin Global Biostatistics and Programming Wyeth Research 2007 Rutgers Biostatistics Day February 16, 2007 Outline Definition and general
The BEST Platform. A Modular Early-Phase Platform for Seamless Dose Finding and Cohort Expansion Laiya Consulting, Inc. 2018
 The BEST Platform A Modular Early-Phase Platform for Seamless Dose Finding and Cohort Expansion Laiya Consulting, Inc. 2018 Introduction The Bayesian early-phase seamless transformation (BEST) platform
The BEST Platform A Modular Early-Phase Platform for Seamless Dose Finding and Cohort Expansion Laiya Consulting, Inc. 2018 Introduction The Bayesian early-phase seamless transformation (BEST) platform
Genitope Corporation. Summary of MyVax Personalized Immunotherapy Phase 3 Clinical Trial Results
 Genitope Corporation Summary of MyVax Personalized Immunotherapy Phase 3 Clinical Trial Results Introduction In December 27, Genitope Corporation ( Genitope ) obtained data indicating that its pivotal
Genitope Corporation Summary of MyVax Personalized Immunotherapy Phase 3 Clinical Trial Results Introduction In December 27, Genitope Corporation ( Genitope ) obtained data indicating that its pivotal
Adaptive Design Improvements in the. and. Correspondence Author: Bradley P. Carlin
 Adaptive Design Improvements in the Continual Reassessment Method for Phase I Studies JULIE M. HEYD Medtronic, Inc., 800 53rd Avenue N.E. N300, Minneapolis, Minnesota 55421, U.S.A. and BRADLEY P. CARLIN
Adaptive Design Improvements in the Continual Reassessment Method for Phase I Studies JULIE M. HEYD Medtronic, Inc., 800 53rd Avenue N.E. N300, Minneapolis, Minnesota 55421, U.S.A. and BRADLEY P. CARLIN
Genomics And Pharmacogenomics In Anticancer Drug Development And Clinical Response (Cancer Drug Discovery And Development) READ ONLINE
 Genomics And Pharmacogenomics In Anticancer Drug Development And Clinical Response (Cancer Drug Discovery And Development) READ ONLINE to modify patients' exposure to drugs based on their genomic drug-response
Genomics And Pharmacogenomics In Anticancer Drug Development And Clinical Response (Cancer Drug Discovery And Development) READ ONLINE to modify patients' exposure to drugs based on their genomic drug-response
Comparative Oncology Program
 The Problem: Non-Integrated Cancer Drug Development A Solution: Integration of Informative Non-Clinical Models of Cancer With Clinical Drug Development Efforts Companion Animal Malignancies as Comparative
The Problem: Non-Integrated Cancer Drug Development A Solution: Integration of Informative Non-Clinical Models of Cancer With Clinical Drug Development Efforts Companion Animal Malignancies as Comparative
IDSA is pleased to offer the following comments on specific priority areas identified by FDA:
 October 31, 2018 Shashi Malhotra Office of Acquisitions & Grants Services (OAGS) Food and Drug Administration Telephone: 240-402-7592 Email: Shashi.Malhotra@fda.hhs.gov SUBJECT: NOT-FD-18-16: Development
October 31, 2018 Shashi Malhotra Office of Acquisitions & Grants Services (OAGS) Food and Drug Administration Telephone: 240-402-7592 Email: Shashi.Malhotra@fda.hhs.gov SUBJECT: NOT-FD-18-16: Development
Consultation on proposals for a new Cancer Drugs Fund (CDF) operating model: Q&A
 Consultation on proposals for a new Cancer Drugs Fund (CDF) operating model: Q&A NHS England INFORMATION READER BOX Directorate Medical Commissioning Operations Patients and Information Nursing Trans.
Consultation on proposals for a new Cancer Drugs Fund (CDF) operating model: Q&A NHS England INFORMATION READER BOX Directorate Medical Commissioning Operations Patients and Information Nursing Trans.
Statistical Issues in Clinical Trial Design
 Statistical Issues in Clinical Trial Design Kenneth R. Hess, PhD Corresponding author Kenneth R. Hess, PhD Department of Biostatistics and Applied Mathematics, The University of Texas M.D. Anderson Cancer
Statistical Issues in Clinical Trial Design Kenneth R. Hess, PhD Corresponding author Kenneth R. Hess, PhD Department of Biostatistics and Applied Mathematics, The University of Texas M.D. Anderson Cancer
Technical Guidance on Development of In Vitro Companion Diagnostics and Corresponding Therapeutic Products
 Administrative Notice December 26, 2013 To: Division of Pharmaceutical Affairs, Prefectural Health Department (Bureau) From: Evaluation and Licensing Division, Pharmaceutical and Food Safety Bureau Ministry
Administrative Notice December 26, 2013 To: Division of Pharmaceutical Affairs, Prefectural Health Department (Bureau) From: Evaluation and Licensing Division, Pharmaceutical and Food Safety Bureau Ministry
Estimation of Relative Potency from Bioassay Data that Include Values below the Limit of Quantitation
 Estimation of Relative Potency from Bioassay Data that Include Values below the Limit of Quantitation FRANCIS BURSA, KELLY J. FLEETWOOD, KARIE J. HIRST, AND ANN YELLOWLEES Experimental data may include
Estimation of Relative Potency from Bioassay Data that Include Values below the Limit of Quantitation FRANCIS BURSA, KELLY J. FLEETWOOD, KARIE J. HIRST, AND ANN YELLOWLEES Experimental data may include
Cost-effectiveness and cost-utility analysis accompanying Cancer Clinical trials. NCIC CTG New Investigators Workshop
 Cost-effectiveness and cost-utility analysis accompanying Cancer Clinical trials NCIC CTG New Investigators Workshop Keyue Ding, PhD. NCIC Clinical Trials Group Dept. of Public Health Sciences Queen s
Cost-effectiveness and cost-utility analysis accompanying Cancer Clinical trials NCIC CTG New Investigators Workshop Keyue Ding, PhD. NCIC Clinical Trials Group Dept. of Public Health Sciences Queen s
Exploratory clinical trials workshop
 Exploratory clinical trials workshop Yves Donazzolo, Grenoble / Lyon Dominique Tremblay, Paris AGAH / Club Phase I meeting Lyon, April 28 & 29, 2009 Topics Introduction Definitions Nonclinical safety studies
Exploratory clinical trials workshop Yves Donazzolo, Grenoble / Lyon Dominique Tremblay, Paris AGAH / Club Phase I meeting Lyon, April 28 & 29, 2009 Topics Introduction Definitions Nonclinical safety studies
Basic Principles for Conducting Phase I Trials in the Japanese Population Prior to Global Clinical Trials
 Administrative Notice October 27, 2014 To: Prefectural Health Department (Bureau) Evaluation and Licensing Division, Pharmaceutical and Food Safety Bureau, Ministry of Health, Labour and Welfare Basic
Administrative Notice October 27, 2014 To: Prefectural Health Department (Bureau) Evaluation and Licensing Division, Pharmaceutical and Food Safety Bureau, Ministry of Health, Labour and Welfare Basic
PHASE 1, MULTICENTER, OPEN-LABEL STUDY OF SINGLE-AGENT BISPECIFIC ANTIBODY T CELL ENGAGER GBR 1342 IN RELAPSED/REFRACTORY MULTIPLE MYELOMA
 PHASE 1, MULTICENTER, OPEN-LABEL STUDY OF SINGLE-AGENT BISPECIFIC ANTIBODY T CELL ENGAGER GBR 1342 IN RELAPSED/REFRACTORY MULTIPLE MYELOMA JOSHUA RICHTER 1 ; MARTIN WERMKE 2 ; JOHN KAUH 3 ; JONATHAN BACK
PHASE 1, MULTICENTER, OPEN-LABEL STUDY OF SINGLE-AGENT BISPECIFIC ANTIBODY T CELL ENGAGER GBR 1342 IN RELAPSED/REFRACTORY MULTIPLE MYELOMA JOSHUA RICHTER 1 ; MARTIN WERMKE 2 ; JOHN KAUH 3 ; JONATHAN BACK
31 Mar Two Bayesian designs for first-in-human trials in cancer. Nedjad Losic March 31, 2017
 Two Bayesian designs for first-in-human trials in cancer Nedjad Losic March 31, 2017 2 1 Agenda Two Bayesian designs for first-inhuman trials in cancer Quick intro to first-in-human trials in cancer Continual
Two Bayesian designs for first-in-human trials in cancer Nedjad Losic March 31, 2017 2 1 Agenda Two Bayesian designs for first-inhuman trials in cancer Quick intro to first-in-human trials in cancer Continual
3 Phases of Investigation
 Part I: The scientific setting - December 30, 2009, 1 3 Phases of Investigation As discussed in Chapter 1, science is adversarial; scientists should consider all possible hypotheses, and only eliminate
Part I: The scientific setting - December 30, 2009, 1 3 Phases of Investigation As discussed in Chapter 1, science is adversarial; scientists should consider all possible hypotheses, and only eliminate
Bayesian Dose-Finding in Phase I/II Clinical Trials Using Toxicity and Efficacy Odds Ratios
 Biometrics 62, 777 787 September 2006 DOI: 10.1111/.1541-0420.2006.00534.x Bayesian Dose-Finding in Phase I/II Clinical Trials Using Toxicity and Efficacy Odds Ratios Guosheng Yin, Yisheng Li, and Yuan
Biometrics 62, 777 787 September 2006 DOI: 10.1111/.1541-0420.2006.00534.x Bayesian Dose-Finding in Phase I/II Clinical Trials Using Toxicity and Efficacy Odds Ratios Guosheng Yin, Yisheng Li, and Yuan
An Introduction to Clinical Research and Development
 Bay Clinical R&D Services An Introduction to Clinical Research and Development The Complex Process by which New Drugs are Tested in Humans Anastassios D. Retzios, Ph.D. Outline of Presentation What is
Bay Clinical R&D Services An Introduction to Clinical Research and Development The Complex Process by which New Drugs are Tested in Humans Anastassios D. Retzios, Ph.D. Outline of Presentation What is
U. Lorch, K. Berelowitz, C. Ozen, A. Naseem, E. Akuffo & J. Taubel
 The practical application of adaptive study design in early phase clinical trials: a retrospective analysis of time savings U. Lorch, K. Berelowitz, C. Ozen, A. Naseem, E. Akuffo & J. Taubel European Journal
The practical application of adaptive study design in early phase clinical trials: a retrospective analysis of time savings U. Lorch, K. Berelowitz, C. Ozen, A. Naseem, E. Akuffo & J. Taubel European Journal
Session 2 summary Designs & Methods. Pairwise comparisons approach. Dose finding approaches discussed: Guiding principles for good dose selection
 Session 2 summary Designs & Methods Pairwise comparisons approach Dose finding approaches discussed: PK/PD Modeling (Adaptive) MCPMod Model Averaging Bayesian Adaptive Dose Ranging Emax Dose Response Model
Session 2 summary Designs & Methods Pairwise comparisons approach Dose finding approaches discussed: PK/PD Modeling (Adaptive) MCPMod Model Averaging Bayesian Adaptive Dose Ranging Emax Dose Response Model
Parametric non-mixture cure models for schedule finding of therapeutic agents
 Appl. Statist. (2009) 58, Part 2, pp. 225 236 Parametric non-mixture cure models for schedule finding of therapeutic agents Changying A. Liu and Thomas M. Braun University of Michigan, Ann Arbor, USA [Received
Appl. Statist. (2009) 58, Part 2, pp. 225 236 Parametric non-mixture cure models for schedule finding of therapeutic agents Changying A. Liu and Thomas M. Braun University of Michigan, Ann Arbor, USA [Received
Merging the Science of Quantitative Pharmacology into Routine Patient Care: Focus on Digital Tools
 Merging the Science of Quantitative Pharmacology into Routine Patient Care: Focus on Digital Tools Janel Long-Boyle, PharmD, PhD Associate Professor of Clinical Pharmacy UCSF School of Pharmacy Disclosure(s)
Merging the Science of Quantitative Pharmacology into Routine Patient Care: Focus on Digital Tools Janel Long-Boyle, PharmD, PhD Associate Professor of Clinical Pharmacy UCSF School of Pharmacy Disclosure(s)
Bios 6648: Design & conduct of clinical research
 Bios 6648: Design & conduct of clinical research Section 3 - Essential principle (randomization) 3.4 Trial monitoring: Interim decision and group sequential designs Bios 6648- pg 1 (a) Recruitment and
Bios 6648: Design & conduct of clinical research Section 3 - Essential principle (randomization) 3.4 Trial monitoring: Interim decision and group sequential designs Bios 6648- pg 1 (a) Recruitment and
Best practice in dose finding studies. Rudolf Koehne-Volland Head of Biostatistics & CEO Metronomia Clinical Research GmbH
 Best practice in dose finding studies Rudolf Koehne-Volland Head of Biostatistics & CEO Metronomia Clinical Research GmbH Best practice s in dose 13-Oct-2016 finding 2 Best practice in dose finding studies
Best practice in dose finding studies Rudolf Koehne-Volland Head of Biostatistics & CEO Metronomia Clinical Research GmbH Best practice s in dose 13-Oct-2016 finding 2 Best practice in dose finding studies
MEDICINES CONTROL COUNCIL
 MEDICINES CONTROL COUNCIL FIXED DOSE COMBINATION PRODUCTS (FDC Products) FOR HIV/AIDS, TUBERCULOSIS, and MALARIA This guideline is intended to provide recommendations to applicants wishing to submit applications
MEDICINES CONTROL COUNCIL FIXED DOSE COMBINATION PRODUCTS (FDC Products) FOR HIV/AIDS, TUBERCULOSIS, and MALARIA This guideline is intended to provide recommendations to applicants wishing to submit applications
Crowe Critical Appraisal Tool (CCAT) User Guide
 Crowe Critical Appraisal Tool (CCAT) User Guide Version 1.4 (19 November 2013) Use with the CCAT Form version 1.4 only Michael Crowe, PhD michael.crowe@my.jcu.edu.au This work is licensed under the Creative
Crowe Critical Appraisal Tool (CCAT) User Guide Version 1.4 (19 November 2013) Use with the CCAT Form version 1.4 only Michael Crowe, PhD michael.crowe@my.jcu.edu.au This work is licensed under the Creative
Animal Research Ethics Committee. Guidelines for Submitting Protocols for ethical approval of research or teaching involving live animals
 Animal Research Ethics Committee Guidelines for Submitting Protocols for ethical approval of research or teaching involving live animals AREC Document No: 3 Revised Guidelines for Submitting Protocols
Animal Research Ethics Committee Guidelines for Submitting Protocols for ethical approval of research or teaching involving live animals AREC Document No: 3 Revised Guidelines for Submitting Protocols
How to implement the recently released EMA guideline on First-in-Human trials?
 How to implement the recently released EMA guideline on First-in-Human trials? Academic Clinical Investigation Centers Perspective Pr D. DEPLANQUE National Coordinator of the French Clinical Investigation
How to implement the recently released EMA guideline on First-in-Human trials? Academic Clinical Investigation Centers Perspective Pr D. DEPLANQUE National Coordinator of the French Clinical Investigation
Pharmacokinetics in clinical oncology
 Pharmacokinetics in clinical oncology Carlos Ochoa Biostatistics Journal Club Zurich, 27 March 2013 Pharmacokinetics in clinical oncology Anticancer drug effects: Shrink tumour size Slow tumour growth
Pharmacokinetics in clinical oncology Carlos Ochoa Biostatistics Journal Club Zurich, 27 March 2013 Pharmacokinetics in clinical oncology Anticancer drug effects: Shrink tumour size Slow tumour growth
The flexible bivariate continual reassessment method
 University of Iowa Iowa Research Online Theses and Dissertations Summer 2015 The flexible bivariate continual reassessment method Mitchell Alan Thomann University of Iowa Copyright 2015 Mitchell Alan Thomann
University of Iowa Iowa Research Online Theses and Dissertations Summer 2015 The flexible bivariate continual reassessment method Mitchell Alan Thomann University of Iowa Copyright 2015 Mitchell Alan Thomann
