Category Storage Shelf Life Additional Criteria
|
|
|
- Sarah Adams
- 6 years ago
- Views:
Transcription
1 CE Update [blood banking/transfusion medicine] Blood Components for Hemostasis Jun Teruya, MD, DSc, and Glenn Ramsey, MD From the Department of Pathology, Northwestern University Medical School, Chicago. On completion of this article, the reader will be able to describe the clinical indications and dosages for transfusing platelets, plasma, and cryoprecipitate. Blood banking/transfusion medicine exam 0102 questions and the corresponding answer form are located after the Your Lab Focus section. Transfusion of platelets, plasma, or cryoprecipitate Use of plasma to provide clotting factors Plasma products used to treat thrombotic thrombocytopenic purpura Blood Components for Hemostasis* The guiding principle of blood component therapy is to provide the specific product needed by each patient. Platelets, plasma, and cryoprecipitate each have different indications for various types of coagulopathies. The clinical condition, the presence of bleeding or an invasive procedure, the platelet count, and coagulation testing are all factors in determining which hemostatic blood components to transfuse. Table 1 [T1] lists the blood components used for hemostasis. Category Storage Shelf Life Additional Criteria T1 Platelets 20 C-24 C with continuous gentle agitation 5 d Maximum time without agitation 24 h Platelet pooled or open system 20 C-24 C with continuous gentle agitation 4 h, unless otherwise specified Platelets, pheresis 20 C-24 C with continuous gentle agitation 5 d Maximum time without agitation 24 h FFP 18 C or less 12 mo Frozen within 8 h of collection in CPD, CP2D, CPDA-1 65 C or less 7 y Frozen within 6 h of collection in ACD FFP thawed 1 C-6 C 24 h Thaw at 30 C-37 C or FDAapproved microwave device Thawed plasma 1 C-6 C More than 24 h, less than 5 d Closed system Liquid plasma 1 C-6 C 5 d after expiration of RBCs Plasma frozen within 24 h 18 C or less 12 mo Solvent/detergent-treated 18 C or less 12 mo from manufacture; pooled plasma manufacturer states expiration date on label Solvent/detergent-treated 20 C -24 C 24 h pooled plasma, thawed Cryoprecipitated AHF 18 C or less 12 mo Thaw FFP at 1 C-6 C, refreeze cryoprecipitate within 1 h Cryoprecipitated AHF, thawed 20 C-24 C Open system or pooled: as soon as possible or 4 h Single unit or pooled prior to freezing: 6 h Plasma, cryoprecipitate 18 C or less 12 mo reduced Plasma cryoprecipitate 1-6 C 24 h reduced, thawed 31 ACD, acid citrate dextrose; AHF, antihemophilic factor; CP2D, citriate phosphate 2-dextrose; CPD, citrate phosphate dextrose; CPDA-1, CPD adenine; FDA, US Food and Drug Administration; FFP, fresh-frozen plasma. *From American Association of Blood Banks Standards for Blood Banks and Transfusion Services. 1 Plasma separated from the blood of an individual donor. FFP from which cryoprecipitate has been removed
2 32 your lab focus Platelet Transfusion Product Options Platelets are transfused either as random-donor platelets from whole-blood donations or as plateletpheresis units collected by apheresis. Random-donor units are somewhat less expensive per dose, but compared with plateletpheresis units they expose the recipient to more donors, are more prone to bacterial contamination, and are more cumbersome to reduce the number of leukocytes before storage. Plateletpheresis units are commonly produced with reduction of leukocytes techniques and are convenient to issue without pooling. The possibility of bacterial contamination and growth at the room temperature of platelet storage currently limits the shelf life of platelets to 5 days. If bacteria can be prevented or destroyed through sterilization in the future, platelet additives may be able to significantly extend the storage period [T1]. Platelet transfusions are administered when hemostasis is needed in the settings of thrombocytopenia or platelet dysfunction. 2 The risk of bleeding from a profoundly low platelet count has been reassessed in recent years [T2]. Formerly, platelet counts less than /µl ( /L) were thought to cause spontaneous hemorrhage. However, recent studies have revised this threshold. Serious bleeding does not usually occur until the patient s platelet count is less than /µl ( /L); therefore, prophylactic platelet transfusions are recommended for severe thrombocytopenia to this degree. Patients with platelet counts between 10 and /µl (10 and /L) may also be at risk if they have conditions causing increased platelet turnover, such as high fever or severe infection. For patients who are bleeding or who have an impending invasive procedure, a platelet count of more than /µl ( /L) is usually sought. For bleeding in critical anatomic sites such as the central nervous system or the airway, higher platelet counts may be needed. Patients receiving large amounts of RBCs and other fluids may develop dilutional thrombocytopenia after more than 1 blood volume of transfusions. Thrombocytopenia and Bleeding Risks Platelet Count Platelet dysfunction in the setting of bleeding or invasive procedures often requires treatment. Common causes of platelet dysfunction include antiplatelet medications, uremia, and cardiopulmonary bypass. Assessment of platelet dysfunction can be difficult. The bleeding-time test is a poor predictor of bleeding risk. Newer in vitro measurements of platelet activity are under investigation to augment the traditional clinical picture of systemic microvascular bleeding. 3 The first line of treatment is usually the drug desmopressin acetate (DDAVP), which may improve platelet function by stimulating the release of von Willebrand factor (vwf) into the blood from endothelial cells. However, if this does not control bleeding sufficiently, platelet transfusions may be needed. Platelet transfusions are usually avoided in patients with thrombotic thrombocytopenic purpura (TTP) because they may worsen the condition. In immune thrombocytopenic purpura, platelet transfusions are usually given only in bleeding emergencies because the autoantibodies promptly remove the transfused platelets from the circulation. The typical platelet dose for adults is 1 standard plateletpheresis unit or its equivalent of approximately 5 to 6 random-donor units. The minimum required content of these units is platelets, but about platelets are usually provided. This should be enough to increase the averagesized adult s platelet count by 30 to /µl (30 to /L), in the absence of refractoriness. Small children are given 1 random-donor unit per 10 to 15 kg Risk of Bleeding /µl or more ( /L or more) Bleeding with surgery, trauma, and invasive procedures unlikely /µl ( /L) Spontaneous bleeding unlikely; bleeding likely with surgery, trauma, and invasive procedures /µl ( /L) Risk of spontaneous bleeding < /µl (< /L) High risk of spontaneous bleeding T2 of body weight. Patients who need recurrent platelet transfusions should receive leukocyte-reduced RBCs and platelets to reduce their risk of HLA alloimmunization. A debate has emerged recently about the merits of higher or lower doses of platelets. In many plateletpheresis donations, a higher platelet content, or even 2 minimum-content products, can be obtained. Transfusions averaging platelets have been investigated as a way to increase platelet counts or to maintain the increase over a longer period of time. 4 On the other hand, the concept of more frequent transfusions with smaller amounts of platelets, such as 3 randomdonor units, has been proposed to reduce total platelet requirements while maintaining hemostatic platelet levels. 5 Further studies of this issue are anticipated. Physicians usually attempt to achieve a threshold platelet count; refractoriness is defined in terms of the percentage of the predicted platelet increment achieved for a given platelet content and body size. The platelet response is best assessed within 15 to 60 minutes after the transfusion. The patient s response is considered refractory when each of at least 2 transfusions fails to achieve one third to one half of the expected increment. For a 70-kg patient receiving a dose of platelets, this would be an increment of less than /µl ( /L). Refractoriness has many causes: active bleeding, splenomegaly, severe infection or fever, disseminated intravascular coagulation, platelet autoantibodies, and drug antibodies. ABO-incompatible platelet transfusions average about two thirds of the regular platelet count rise and, in some patients, yield poor responses
3 because of high anti-a/b levels. Plateletspecific antibodies develop in a small number of patients. However, immune refractoriness is often due to HLA antibodies. Diagnosis is made by HLA antibody testing. In alloimmunized patients, platelet crossmatching or HLA-matched platelets may improve transfusion responses. Plasma Transfusion Product Options Fresh frozen plasma (FFP) is prepared by centrifugation within 8 hours of whole blood collection in citrate phosphate dextrose adenine, citrate phosphate dextrose, and citrate phosphate 2-dextrose and 6 hours in acid citrate dextrose. It is stored at 18 C or less for up to 12 months. It should be thawed at 30 C to 37 C and can be used as FFP for up to 24 hours after thawing. FFP contains all the proteins including labile coagulation factors at the same level as they circulate in vivo. Twenty-four hours after thawing, it can be used as thawed plasma, which contains a somewhat reduced amount of labile factor V and factor VIII, for 5 days after thawing. Liquid plasma is prepared by centrifuge of a whole blood unit at any time and stored at 1 C to 6 C until use. Liquid plasma contains a reduced amount of labile coagulation factor V and factor VIII. According to National Institutes of Health guidelines published in 1993, FFP should be administered only to increase the level of clotting factors in patients with a demonstrated deficiency [T3]. 6 Deficiency of coagulation factors can be measured by prothrombin time (PT) and activated partial thromboplastin time (aptt) for extrinsic pathway and intrinsic pathway, respectively. Patients with TTP may benefit from FFP transfusion. Especially for patients with idiopathic TTP, who are considered to have autoantibody against the cleavage enzyme of unusually large vwf, plasma exchange with FFP is the only efficacious treatment. Clinicians should not transfuse FFP for volume expansion, as a nutritional supplement, or prophylactically with massive blood transfusion and following cardiopulmonary bypass. Factor-specific concentrates or recombinant factors are marketed for factor VII, VIII, or IX deficiencies. In the United States, antithrombin concentrate and alpha 1 - antitrypsin are approved for their respective congenital deficiencies. FFP should not be used if a specific coagulation factor or protein is available since the latter is sterilized. Unless the PT or aptt exceeds 1.5 to 1.8 times control values, FFP is rarely indicated since clinically significant bleeding is not common. However, because factor sensitivity of PT and aptt reagents varies between manufacturers, there is no definite threshold. For example, when the factor XI level is 10% of normal, the aptt in use at our institution (reference range, seconds) is 34.2 seconds. Because a 30% level of factor XI is usually needed to obtain hemostasis during surgery, a normal aptt does not always guarantee that the factor XI is sufficient. One unit of FFP is usually 200 to 250 ml. The FFP transfusion must be ABOcompatible [T4]. It can be given without regard to Rh type, and crossmatching is not required. The following formula is used to calculate dosage for specific factor replacement in adults: Body Weight (kg) 70 ml/kg = Total Blood Volume (ml) Total Blood Volume (ml) (100 Hematocrit)/100 = Total Plasma Volume (ml) for Plasma Transfusion Indication Coagulation Factor or Protein Deficiency Comments T3 Replacement of single factor Factors V, X, and XI, protein C, and protein S Factors VIIa, VIII, IX, antithrombin, and alpha 1 - deficiencies in which a specific factor antitrypsin concentrates are on market concentrate is unavailable Immediate reversal of warfarin effect Factors II, VII, IX, and X, protein C and protein S If the patient can wait 10 h, administer parenteral vitamin K Vitamin K deficiency associated with Factors II, VII, IX, and X, protein C and protein S It is commonly associated with a prolonged use of active bleeding antibiotics Acute disseminated intravascular All coagulation factors, protein C, protein S, coagulation and antithrombin Liver disease All coagulation factors (except factor VIII), The goal should be to correct or prevent bleeding protein C, protein S, and antithrombin complications, not to achieve a normal prothrombin time Dilutional coagulopathy All coagulation factors and proteins It is seen in massive transfusion of more than 1 blood volume and intensive daily pheresis with 5% albumin Thrombotic thrombocytopenic Congenital deficiency of von Willebrand factor Usually used as replacement fluid for plasma purpura/hemolytic uremic syndrome cleavage enzyme or autoantibody to the enzyme exchange 33
4 Total Plasma Volume (ml) (Desired Level Patient Level) U/mL = Needed Factor Level (U) (1 U/mL is 100%) For example, if a 100-kg patient, who is known to hemorrhage, with low factor XI of 5% is going to surgery and needs a 50% level, it is calculated as follows: 100 kg 70 ml/kg = 7,000 ml 7,000 ml (100 40)/100 = 4,200 ml 4,200 ml ( ) U/mL = 1,890 U Assuming 1 U of FFP contains 1 U/mL (100%) of factor XI, 1,890 U/1 U/mL = 1,890 ml Assuming 1 U of FFP is 250 ml, 1,890 ml/250 ml = 7.56 U Patient and Plasma ABO Types Recipient ABO First Choice Second Choice O O A, B, AB A A AB B B AB AB AB None Biologic Data for Coagulation Factors and Inhibitors Coagulation Factors Biological Half-Life Levels to Achieve and Inhibitors for Hemostasis Fibrinogen 3-4 d 100 mg/dl (1.0 g/l) T4 T5 34 Therefore, 8 U of FFP should be given usually every 24 hours. Table 5 [T5] shows the biological half-lives and hemostatic levels for each major coagulation factor and inhibitor. Cryoprecipitated Antihemophilic Factor (CRYO) CRYO contains factor VIII, fibrinogen, fibronectin, vwf, and factor XIII in 8 to 15 ml made from the FFP of 1 whole-blood donation. CRYO is recommended for hypofibrinogenemia with bleeding, von Willebrand disease, and hemophilia A when factor VIII concentrate is not available. 7 For mild type 1 von Willebrand disease, DDAVP is a preferred choice of treatment. Because some sterile factor VIII concentrates such as Humate-P (Centeon [M]) contain a significant amount of vwf, CRYO is not widely used to treat von Willebrand disease. A lyophilized vwf product may be on the market soon. Coagulopathy associated with uremia can be treated with CRYO, but DDAVP is usually the first-line therapy. One or 2 U of CRYO is also used for fibrin glue or fibrin sealant during surgery. CRYO and thrombin are applied to the bleeding surface simultaneously, where fibrinogen is converted to fibrin by the action of thrombin. To avoid potential donor exposures, the patient s own CRYO can be harvested for this Factor II 2-5 d 40%-50% of normal ( ) Factor V h 10%-30% ( ) Factor VII 4-7 h 10%-20% ( ) Factor VIII 9-18 h 30%-100% ( ) Factor IX h 20%-60% ( ) Factor X h 10%-40% ( ) Factor XI h 20%-30% ( ) Factor XIII 12 d 10% (0.10) Von Willebrand factor h 20%-50% Protein C 3-5 h 60% Protein S 42 h 60% Antithrombin h 60% use. Virally inactivated fibrinogen concentrate also has been licensed recently for this purpose. One unit contains an average of 250 mg of fibrinogen, with a minimum fibrinogen content of 150 mg, according to the standards of the American Association of Blood Banks. 1 When the patient s fibrinogen level is below 80 to 100 mg/dl (0.8 to 1.0 g/l), CRYO transfusion is usually indicated. One unit of CRYO per 10 kg body weight usually increases plasma fibrinogen level by 50 mg/dl (0.5 g/l) in the absence of continued consumption or massive bleeding. Although 6 to 8 U of CRYO constitute a typical adult transfusion dose, a larger dose of CRYO may be needed for patients with active disseminated intravascular coagulation and increased fibrinolytic activity. One unit of CRYO should contain a minimum factor VIII content of 80 U but is no longer used as a primary source of factor VIII since sterile factor VIII, both concentrate and recombinant, is available. Cryoprecipitate-Reduced Plasma The plasma recovered after removal of cryoprecipitate is the preferred replacement component for plasma exchange for TTP, since it contains far less vwf than plasma. In these conditions, deficiency of a vwf cleavage enzyme leads to the accumulation of large vwf multimers, which causes platelet activation and aggregation. When cryoprecipitate-reduced plasma is used as the replacement fluid in intensive plasma exchange, monitoring the aptt is required since it contains little factor VIII.
5 Conclusions Each blood component should be transfused based on clinical symptoms and laboratory test results. Surgical bleeding can be corrected without giving blood components. To avoid unnecessary transfusion, rapid turnaround time and accurate results for PT, aptt, fibrinogen, and platelet count are necessary. If platelet function can be measured within a reasonable time, unnecessary platelet transfusion for suspected platelet dysfunction can be avoided. It is suggested that clinicians, the blood bank, and the hematology-coagulation laboratory communicate with each other. Such communication can reduce unnecessary blood transfusion and wastage of blood components. 1. Standards for Blood Banks and Transfusion Services. 19th ed. Bethesda, MD: American Association of Blood Banks; Herman JH. Platelet transfusion therapy. In: Mintz PD, ed. Transfusion Therapy: Clinical Principles and Practice. Bethesda, MD: AABB Press;1999: Francis J, Francis D, Larson L, et al. Can the platelet function analyzer (PFA)-100 test substitute for the template bleeding time in routine clinical practice? Platelets. 1999;10: Klumpp TR, Herman JH, Gaughan JP, et al. Clinical consequences of alterations in platelet transfusion dose: a prospective, randomized, double-blind trial. Transfusion. 1999;39: Hersh JK, Hom EG, Brecher ME. Mathematical modeling of platelet survival with implications for optimal practice in the chronically platelet transfusion dependent patient. Transfusion. 1998;38: National Institutes of Health. Transfusion Alert: for the Use of Red Blood Cells, Platelets, and Fresh Frozen Plasma. Bethesda, MD: National Institutes of Health; August NIH Publication a. 7. College of American Pathologists. Practice parameter for the use of fresh-frozen plasma, cryoprecipitate, and platelets. JAMA. 1994;271:
Blood Component Preparation and Therapeutic Utilization
 Blood Component Preparation and Therapeutic Utilization Prof. A. Pourazar Immunohematologist and Transfusion medicine School of Medicine, Isfahan University Of Medical Science IRAN Red Blood cells, Platelets
Blood Component Preparation and Therapeutic Utilization Prof. A. Pourazar Immunohematologist and Transfusion medicine School of Medicine, Isfahan University Of Medical Science IRAN Red Blood cells, Platelets
Blood Product Utilization
 Who gets what & when Why not to give blood? Volume Expander For specific number (except as related to procedures) To patients with religious objections to blood transfusions Blood given only when necessary
Who gets what & when Why not to give blood? Volume Expander For specific number (except as related to procedures) To patients with religious objections to blood transfusions Blood given only when necessary
Clinical Use of Plasma for Transfusion. Irma Szymanski, MD Professor of Pathology, Emerita University of Massachusetts Medical School
 Clinical Use of Plasma for Transfusion Irma Szymanski, MD Professor of Pathology, Emerita University of Massachusetts Medical School PLASMA PRODUCTS FOR TRANSFUSION Fresh Frozen Plasma (FFP) Thawed Plasma
Clinical Use of Plasma for Transfusion Irma Szymanski, MD Professor of Pathology, Emerita University of Massachusetts Medical School PLASMA PRODUCTS FOR TRANSFUSION Fresh Frozen Plasma (FFP) Thawed Plasma
Manejo de la transfusión de plaquetas. Ileana López-Plaza, MD
 Manejo de la transfusión de plaquetas Ileana López-Plaza, MD Thrombocytopenia Common in ICU setting 25-38% with< 100,000/µL 2-3 % with < 10,000/µL Common etiologies Drug-induced: heparin, antibiotics,
Manejo de la transfusión de plaquetas Ileana López-Plaza, MD Thrombocytopenia Common in ICU setting 25-38% with< 100,000/µL 2-3 % with < 10,000/µL Common etiologies Drug-induced: heparin, antibiotics,
Managing Massive Transfusions in diverse Patient Populations in a Non-Metropolitan Area
 Managing Massive Transfusions in diverse Patient Populations in a Non-Metropolitan Area SHAUNA M.M. STURGILL, LAURIE GILLARD LEARNING OBJECTIVES 1. Compare and contrast massive transfusion protocols for
Managing Massive Transfusions in diverse Patient Populations in a Non-Metropolitan Area SHAUNA M.M. STURGILL, LAURIE GILLARD LEARNING OBJECTIVES 1. Compare and contrast massive transfusion protocols for
Platelet Refractoriness: The Basics. Martin H. Bluth, MD, PhD
 Platelet Refractoriness: The Basics Martin H. Bluth, MD, PhD Complete Toxicology Laboratories, LLC Objectives Define platelet refractoriness and associated conditions that may cause platelet refractoriness.
Platelet Refractoriness: The Basics Martin H. Bluth, MD, PhD Complete Toxicology Laboratories, LLC Objectives Define platelet refractoriness and associated conditions that may cause platelet refractoriness.
Blood transfusion in special situations and poly-trauma. Dr Marina Karakantza Consultant Haematologist in Transfusion Medicine, LTHT
 Blood transfusion in special situations and poly-trauma Dr Marina Karakantza Consultant Haematologist in Transfusion Medicine, LTHT Uncontrolled bleeding is a major preventable cause of death in trauma
Blood transfusion in special situations and poly-trauma Dr Marina Karakantza Consultant Haematologist in Transfusion Medicine, LTHT Uncontrolled bleeding is a major preventable cause of death in trauma
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs
 Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
ANEMIA. Oral iron. IV iron gluconate (order set #233)
 PREVENTION ANEMIA Oral iron IV iron gluconate (order set #233) TRANSEXAMIC ACID Efficacy of IV TXA in Reducing Blood Loss After Elective C-section: Prospective, Randomized, Double-blind, Placebo Controlled
PREVENTION ANEMIA Oral iron IV iron gluconate (order set #233) TRANSEXAMIC ACID Efficacy of IV TXA in Reducing Blood Loss After Elective C-section: Prospective, Randomized, Double-blind, Placebo Controlled
Local vasoconstriction. is due to local spasm of the smooth muscle (symp. reflex) can be maintained by platelet vasoconstrictors
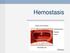 Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Blood Component Therapy and Apheresis
 Blood Component Therapy and Apheresis Dr. Debasish Gupta Program Director, CHF International TRANSFUSION THERAPY Used primarily to treat two conditions Inadequate oxygen carrying capacity because of anemia
Blood Component Therapy and Apheresis Dr. Debasish Gupta Program Director, CHF International TRANSFUSION THERAPY Used primarily to treat two conditions Inadequate oxygen carrying capacity because of anemia
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY
 LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
Index. Autoimmune thrombocytopenic purpura (AITP), 100, 102, 105, 108, 187 Automated platelet counters, , 108
 A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
Coagulation Mechanisms Dr. Nervana Bayoumy
 Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Home truths... the clinical use of components in the UK. Jonathan Wallis. Platelets, FFP, Cryoprecipitate
 Home truths... the clinical use of components in the UK Platelets, FFP, Cryoprecipitate Jonathan Wallis Mar-01 Mar-02 Mar-03 Mar-04 Mar-05 Mar-06 Mar-07 Mar-08 Mar-09 Mar-10 Mar-11 Mar-12 E&N.Wales Platelet
Home truths... the clinical use of components in the UK Platelets, FFP, Cryoprecipitate Jonathan Wallis Mar-01 Mar-02 Mar-03 Mar-04 Mar-05 Mar-06 Mar-07 Mar-08 Mar-09 Mar-10 Mar-11 Mar-12 E&N.Wales Platelet
Primary hemostasis. Vascular endothelium Vasoconstriction : local tissue factor, nervous system
 Primary hemostasis Vascular endothelium Vasoconstriction : local tissue factor, nervous system Platelet Plug Platelet Adhesion Platelet Activation Platelet Aggregation Platelet Plug Formation Secondary
Primary hemostasis Vascular endothelium Vasoconstriction : local tissue factor, nervous system Platelet Plug Platelet Adhesion Platelet Activation Platelet Aggregation Platelet Plug Formation Secondary
LABORATORY DIAGNOSIS OF BLEEDING DISORDERS
 LABORATORY DIAGNOSIS OF BLEEDING DISORDERS Primary & Secondary Hemostasis Disorders http://.columbia.edu/itc/hs/medical/selective/advclinicalpathology/2004/lecture/lab%20diagnosis%20of%20bleeding%20disorders.ppt
LABORATORY DIAGNOSIS OF BLEEDING DISORDERS Primary & Secondary Hemostasis Disorders http://.columbia.edu/itc/hs/medical/selective/advclinicalpathology/2004/lecture/lab%20diagnosis%20of%20bleeding%20disorders.ppt
Disclosures. Thromboelastography. TEG Methodology. TEG Output. Thromboelastography (TEG): Basics & Clinical Applications
 Thromboelastography (TEG): Basics & Clinical Applications Paula J. Santrach MD Associate Professor, Laboratory Medicine Mayo Clinic Rochester, MN Disclosures Relevant financial relationships NONE Off label
Thromboelastography (TEG): Basics & Clinical Applications Paula J. Santrach MD Associate Professor, Laboratory Medicine Mayo Clinic Rochester, MN Disclosures Relevant financial relationships NONE Off label
EDUCATIONAL COMMENTARY MASSIVE TRANSFUSION PROTOCOL
 EDUCATIONAL COMMENTARY MASSIVE TRANSFUSION PROTOCOL Commentary provided by: Kathleen Trudell MLS (ASCP) CM SBBCM University of Nebraska Medical Center Division of Medical Laboratory Science College of
EDUCATIONAL COMMENTARY MASSIVE TRANSFUSION PROTOCOL Commentary provided by: Kathleen Trudell MLS (ASCP) CM SBBCM University of Nebraska Medical Center Division of Medical Laboratory Science College of
Vein-to-Vein: Creating New Products to Optimize Patient Outcomes
 Vein-to-Vein: Creating New Products to Optimize Patient Outcomes BETH H. SHAZ, MD CHIEF MEDICAL AND SCIENTIFIC OFFICER EXECUTIVE VICE PRESIDENT NEW YORK BLOOD CENTER N Y B C. O R G S A V E A L I F E N
Vein-to-Vein: Creating New Products to Optimize Patient Outcomes BETH H. SHAZ, MD CHIEF MEDICAL AND SCIENTIFIC OFFICER EXECUTIVE VICE PRESIDENT NEW YORK BLOOD CENTER N Y B C. O R G S A V E A L I F E N
Platelet Factor IV- Heparin Antibodies. Presenter: Michael J. Warhol, M.D.
 Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
Coagulation in perspective: Blood management. Objectives
 Coagulation in perspective: Blood management Julie Wegner, PhD jawrbl@gmail.com Objectives To gain a basic understanding of the following: 1. Coagulation components and processes Why patients bleed. 2.
Coagulation in perspective: Blood management Julie Wegner, PhD jawrbl@gmail.com Objectives To gain a basic understanding of the following: 1. Coagulation components and processes Why patients bleed. 2.
What Can We Learn from Animal Models of Coagulopathy and Bleeding (about plasma transfusion)?
 Test What Can We Learn from Animal Models of Coagulopathy and Bleeding (about plasma transfusion)? William Sheffield Associate Director, Research CBS Centre for Innovation, and Professor, Pathology and
Test What Can We Learn from Animal Models of Coagulopathy and Bleeding (about plasma transfusion)? William Sheffield Associate Director, Research CBS Centre for Innovation, and Professor, Pathology and
Alberta Health Services - Edmonton Zone Massive Hemorrhage Protocol
 This document applies to all Covenant and AHS sites. Client Resource 23: Alberta Health Services - Edmonton Zone Regional Laboratory Services This document is applicable at site(s): GNH MIS RAH SGH UAH
This document applies to all Covenant and AHS sites. Client Resource 23: Alberta Health Services - Edmonton Zone Regional Laboratory Services This document is applicable at site(s): GNH MIS RAH SGH UAH
Introduction Hemostasis: Tourniquet Test & Bleeding Time. Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO
 Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
General Principles of. Hemostasis. Kristine Krafts, M.D.
 General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
Platelet transfusion therapy. Orieji Illoh, M.D. January 23, 2007
 Platelet transfusion therapy Orieji Illoh, M.D. January 23, 2007 The Eighteenth Century Transfusions were done only sporadically, and were generally animal to human. Transfusion was generally thought of
Platelet transfusion therapy Orieji Illoh, M.D. January 23, 2007 The Eighteenth Century Transfusions were done only sporadically, and were generally animal to human. Transfusion was generally thought of
CLOTTING FACTOR REPLACEMENT THERAPY
 CLOTTING FACTOR REPLACEMENT THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage
CLOTTING FACTOR REPLACEMENT THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage
Platelet type bleeding: (vwd) - Petechiae, purpura, ecchymoses, bruising - Menorrhagia, hematuria, occult GI bleed - Gingival bleeding, epistaxis
 1 Nadanotes.com 2 Nadanotes.com 3 Nadanotes.com Platelet type bleeding: (vwd) - Petechiae, purpura, ecchymoses, bruising - Menorrhagia, hematuria, occult GI bleed - Gingival bleeding, epistaxis Clotting
1 Nadanotes.com 2 Nadanotes.com 3 Nadanotes.com Platelet type bleeding: (vwd) - Petechiae, purpura, ecchymoses, bruising - Menorrhagia, hematuria, occult GI bleed - Gingival bleeding, epistaxis Clotting
Clinical Policy: Humate-P (Antihemophiliac Factor/von Willebrand Factor Complex Human) Reference Number: CP.MP.404
 Clinical Policy: (Antihemophiliac Factor/von Willebrand Factor Complex Human) Reference Number: CP.MP.404 Effective Date: January 2008 Last Review Date: 12/16 See Important Reminder at the end of this
Clinical Policy: (Antihemophiliac Factor/von Willebrand Factor Complex Human) Reference Number: CP.MP.404 Effective Date: January 2008 Last Review Date: 12/16 See Important Reminder at the end of this
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues
 Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
The Role Of Point of Care Coagulation Testing (POCCT) in Patient Blood Management. Elham Khalaf Adeli
 The Role Of Point of Care Coagulation Testing (POCCT) in Patient Blood Management Elham Khalaf Adeli Overview PBM, bleeding management, Coagulation POC Testing Review of laboratory conventional coagulation
The Role Of Point of Care Coagulation Testing (POCCT) in Patient Blood Management Elham Khalaf Adeli Overview PBM, bleeding management, Coagulation POC Testing Review of laboratory conventional coagulation
Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems.
 Test Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems. Karen A. Moffat BEd, MSc, ART, FCSMLS(D) Technical Specialist, Coagulation, HRLMP Assistant Professor, Department of
Test Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems. Karen A. Moffat BEd, MSc, ART, FCSMLS(D) Technical Specialist, Coagulation, HRLMP Assistant Professor, Department of
Alternative Haemostatic Agents in the Management of Obstetric Haemorrhage
 Alternative Haemostatic Agents in the Management of Obstetric Haemorrhage Clinical Associate Professor Nolan McDonnell School of Medicine and Pharmacology, School of Women s and Infants Health University
Alternative Haemostatic Agents in the Management of Obstetric Haemorrhage Clinical Associate Professor Nolan McDonnell School of Medicine and Pharmacology, School of Women s and Infants Health University
CURRENT COURSE OFFERINGS
 The American Red Cross offers regular educational opportunities as a convenient way for healthcare providers to receive relevant blood banking and transfusion medicine information. The bi-monthly sessions,
The American Red Cross offers regular educational opportunities as a convenient way for healthcare providers to receive relevant blood banking and transfusion medicine information. The bi-monthly sessions,
Antihemophilic Products
 Antihemophilic Products Factor IX Only AlphaNine SD Alprolix Kit BEBULIN VH BeneFIX RT Mononine Profilnine SD Additional Antihemophilic Products ATryn Corifact FEIBA Kcentra NovoSeven RT RiaSTAP RIXUBIS
Antihemophilic Products Factor IX Only AlphaNine SD Alprolix Kit BEBULIN VH BeneFIX RT Mononine Profilnine SD Additional Antihemophilic Products ATryn Corifact FEIBA Kcentra NovoSeven RT RiaSTAP RIXUBIS
Recombinant Factor VII vs Cryoprecipitate. Dr. M. Truter Moderator: Prof. Pretorius
 Recombinant Factor VII vs Cryoprecipitate Dr. M. Truter Moderator: Prof. Pretorius Discussion with Dr. J. Potgieter (Haematology) No articles on Recombinant factor VII vs Cryoprecipitate Different indications
Recombinant Factor VII vs Cryoprecipitate Dr. M. Truter Moderator: Prof. Pretorius Discussion with Dr. J. Potgieter (Haematology) No articles on Recombinant factor VII vs Cryoprecipitate Different indications
Prior Authorization Criteria Hemophilia/Blood Factor Products
 Prior Authorization Criteria Hemophilia/Blood Factor Products All requests for Hemophilia/Blood Factor Products require a prior authorization and will be screened for medical necessity and appropriateness
Prior Authorization Criteria Hemophilia/Blood Factor Products All requests for Hemophilia/Blood Factor Products require a prior authorization and will be screened for medical necessity and appropriateness
Using TEG in the ED, OR, and ICU. Don H. Van Boerum, MD, FACS
 Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
PROVINCIAL BLOOD COORDINATING PROGRAM DEFINITIONS NLBCP-063
 Government of Newfoundland and Labrador Department of Health and Community Services Provincial Blood Coordinating Program PROVINCIAL BLOOD COORDINATING PROGRAM DEFINITIONS Office of Administrative Responsibility
Government of Newfoundland and Labrador Department of Health and Community Services Provincial Blood Coordinating Program PROVINCIAL BLOOD COORDINATING PROGRAM DEFINITIONS Office of Administrative Responsibility
Transfusion & Non-transfusion Approaches to Bleeding
 Transfusion & Non-transfusion Approaches to Bleeding Maureane Hoffman, MD, PhD Professor of Pathology, Duke University and Director, Transfusion Service and Hematology Laboratory Durham Veterans Affairs
Transfusion & Non-transfusion Approaches to Bleeding Maureane Hoffman, MD, PhD Professor of Pathology, Duke University and Director, Transfusion Service and Hematology Laboratory Durham Veterans Affairs
Princess Alexandra Hospital Emergency Department. Clinical Procedure. 1 Introduction
 Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
Clinical Procedure. ROTEM Trauma, Resuscitation. Princess Alexandra Hospital Emergency Department. 1 Introduction
 Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
PLATELET GUIDANCE DOCUMENT
 Government of Newfoundland and Labrador Department of Health and Community Services Provincial Blood Coordinating Program PLATELET GUIDANCE DOCUMENT Office of Administrative Responsibility Director, Regional
Government of Newfoundland and Labrador Department of Health and Community Services Provincial Blood Coordinating Program PLATELET GUIDANCE DOCUMENT Office of Administrative Responsibility Director, Regional
Hematology Emergencies: Problems with Platelets
 Hematology Emergencies: Problems with Platelets Christian Cable, MD, FACP Associate Professor of Medicine Division of Hematology & Oncology Texas A&M HSC College of Medicine Scott & White Healthcare Fundamentals
Hematology Emergencies: Problems with Platelets Christian Cable, MD, FACP Associate Professor of Medicine Division of Hematology & Oncology Texas A&M HSC College of Medicine Scott & White Healthcare Fundamentals
Session 1 Topics. Vascular Phase of Hemostasis. Coagulation Pathway. Action of Unfractionated Heparin. Laboratory Monitoring of Anticoagulant Therapy
 ~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (NovoSeven RT) Reference Number: CP.PHAR.220 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Medicaid, HIM-Medical Benefit Coding Implications Revision Log See Important
Clinical Policy: (NovoSeven RT) Reference Number: CP.PHAR.220 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Medicaid, HIM-Medical Benefit Coding Implications Revision Log See Important
Emergency and Perioperative Hemostasis Testing: Which Assays Provide Helpful Information. Wayne Chandler, MD Laboratory Medicine Seattle Children s
 Emergency and Perioperative Hemostasis Testing: Which Assays Provide Helpful Information Wayne Chandler, MD Laboratory Medicine Seattle Children s Emergency Hemostasis Testing Patients actively bleeding
Emergency and Perioperative Hemostasis Testing: Which Assays Provide Helpful Information Wayne Chandler, MD Laboratory Medicine Seattle Children s Emergency Hemostasis Testing Patients actively bleeding
New factor concentrates on the way to the market
 New factor concentrates on the way to the market ISCB, Copenhagen, 1 September 2015 John R. Hess, MD, MPH, FACP, FAAAS Professor of Laboratory Medicine and Hematology Medical Director, Transfusion Service,
New factor concentrates on the way to the market ISCB, Copenhagen, 1 September 2015 John R. Hess, MD, MPH, FACP, FAAAS Professor of Laboratory Medicine and Hematology Medical Director, Transfusion Service,
REGIONAL AUDIT OF PLASMA PRODUCTS 2016
 REGIONAL AUDIT OF PLASMA PRODUCTS 2016 Background: In 2010, the East of England RTC carried out an audit of the use of Fresh Frozen Plasma (FFP) in adult patients. With the introductions of trauma networks
REGIONAL AUDIT OF PLASMA PRODUCTS 2016 Background: In 2010, the East of England RTC carried out an audit of the use of Fresh Frozen Plasma (FFP) in adult patients. With the introductions of trauma networks
LABORATORY APPROCH TO THE BLEEDING PATIENT
 Anne Winkler, MD Emory University School of Medicine, Atlanta Georgia Assistant Professor, Pathology & Laboratory Medicine Medical Director, Transfusion Service, Grady Health System Assistant Director,
Anne Winkler, MD Emory University School of Medicine, Atlanta Georgia Assistant Professor, Pathology & Laboratory Medicine Medical Director, Transfusion Service, Grady Health System Assistant Director,
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides.
 These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
Aim. To provide basic knowledge on the processing, testing and issue of blood donations by NHSBT
 From Donor To Door Aim To provide basic knowledge on the processing, testing and issue of blood donations by NHSBT At the end of this session you will be aware of: The stages of processing, testing and
From Donor To Door Aim To provide basic knowledge on the processing, testing and issue of blood donations by NHSBT At the end of this session you will be aware of: The stages of processing, testing and
Massive Haemorrhage J Davies B Ferguson
 Massive Haemorrhage J Davies B Ferguson What is Massive Haemorrhage (MH)? Difficult to apply rules as to how much blood loss defines a major haemorrhage. Easier to define how the patient s condition is
Massive Haemorrhage J Davies B Ferguson What is Massive Haemorrhage (MH)? Difficult to apply rules as to how much blood loss defines a major haemorrhage. Easier to define how the patient s condition is
Laboratory investigation in the Bleeding Patient. Dr Craig Taylor Consultant Haematologist May 2016
 Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015
 + Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
+ Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
STANDARD BLOOD PRODUCTS AND SERVICES
 STANDARD BLOOD PRODUCTS AND SERVICES Policy NHP reimburses contracted providers for the medically necessary administration (transfusion) of blood and standard blood products. Prerequisites Authorization,
STANDARD BLOOD PRODUCTS AND SERVICES Policy NHP reimburses contracted providers for the medically necessary administration (transfusion) of blood and standard blood products. Prerequisites Authorization,
Coagulopathy Case-2. Andy Nguyen, M.D. 2009
 Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
Disseminated Intravascular Coagulation: Laboratory Support for Management and Treatment
 Disseminated Intravascular Coagulation: Laboratory Support for Management and Treatment Virginia R. Fisher, BS, MT(ASCP), 1 Mary K. Scott, BS, MLS(ASCP) CM, 1 Christine A. Tremblay, BS, MLS(ASCP) CM, 1
Disseminated Intravascular Coagulation: Laboratory Support for Management and Treatment Virginia R. Fisher, BS, MT(ASCP), 1 Mary K. Scott, BS, MLS(ASCP) CM, 1 Christine A. Tremblay, BS, MLS(ASCP) CM, 1
IMPORTANCE OF COAGLUOPATHIES IN COMPANION ANIMALS
 74 IMPORTANCE OF COAGLUOPATHIES IN COMPANION ANIMALS Urs Giger School of Veterinary Medicine, University of Pennsylvania, Philadelphia, USA Practical Tools to Approach Bleeding Patients Urs Giger, Dipl.
74 IMPORTANCE OF COAGLUOPATHIES IN COMPANION ANIMALS Urs Giger School of Veterinary Medicine, University of Pennsylvania, Philadelphia, USA Practical Tools to Approach Bleeding Patients Urs Giger, Dipl.
Disclosure. Hemophilia: The Royal Treatment. Objectives. Background. History of Hemophilia. Epidemiology 1/4/2018
 Disclosure Hemophilia: The Royal Treatment Nikki Heeren, PharmD PGY1 Resident Avera McKennan Hospital I have had no financial relationship over the past 12 months with any commercial sponsor with a vested
Disclosure Hemophilia: The Royal Treatment Nikki Heeren, PharmD PGY1 Resident Avera McKennan Hospital I have had no financial relationship over the past 12 months with any commercial sponsor with a vested
Massive Haemorrhage P Donnelly B Ferguson
 Massive Haemorrhage P Donnelly B Ferguson What is Massive Haemorrhage (MH)? Difficult to apply rules as to how much blood loss defines a major haemorrhage. Easier to define how the patient s condition
Massive Haemorrhage P Donnelly B Ferguson What is Massive Haemorrhage (MH)? Difficult to apply rules as to how much blood loss defines a major haemorrhage. Easier to define how the patient s condition
CLOTTING FACTORS, COAGULANT BLOOD PRODUCTS & OTHER HEMOSTATICS
 CLOTTING FACTORS, COAGULANT BLOOD PRODUCTS & OTHER HEMOSTATICS Protocol: PHA027 Effective Date: February 1, 2019 Table of Contents Page BENEFIT CONSIDERATIONS... 1 COVERAGE RATIONALE... 2 US FOOD AND DRUG
CLOTTING FACTORS, COAGULANT BLOOD PRODUCTS & OTHER HEMOSTATICS Protocol: PHA027 Effective Date: February 1, 2019 Table of Contents Page BENEFIT CONSIDERATIONS... 1 COVERAGE RATIONALE... 2 US FOOD AND DRUG
Component Preparation, Manufacturing and Modifications
 Component Preparation, Manufacturing and Modifications Mahdokht Parsi, MPH, MT(ASCP) Director of Operation, Immunohematology & Genomics Mparsi@nybc.org Current Practices in Transfusion Medicine 1 NEW YORK
Component Preparation, Manufacturing and Modifications Mahdokht Parsi, MPH, MT(ASCP) Director of Operation, Immunohematology & Genomics Mparsi@nybc.org Current Practices in Transfusion Medicine 1 NEW YORK
Type of intervention Treatment; secondary prevention. Economic study type Cost-effectiveness analysis.
 Coagulation disorders induced by L-asparaginase: correction with and without fresh-frozen plasma Glasmacher A, Kleinschmidt R, Unkrig C, Mezger J, Scharf R E Record Status This is a critical abstract of
Coagulation disorders induced by L-asparaginase: correction with and without fresh-frozen plasma Glasmacher A, Kleinschmidt R, Unkrig C, Mezger J, Scharf R E Record Status This is a critical abstract of
Cryoprecipitate audit within six centres in New Zealand.
 Cryoprecipitate audit within six centres in New Zealand. Final Report Audit data collated by: Rachel Donegan : Auckland Rebecca Charman: Manukau Christopher Corkery : Hamilton Catherine Hammond :Wellington
Cryoprecipitate audit within six centres in New Zealand. Final Report Audit data collated by: Rachel Donegan : Auckland Rebecca Charman: Manukau Christopher Corkery : Hamilton Catherine Hammond :Wellington
The Coagulation Workup In The Office Setting
 CAA Conference alm Springs 2012 The Coagulation Workup In The Office Setting CAA Conference alm Springs, October 2012 Robert Miller, A-C Henoch-Schoenlein urpura 1 CAA Conference alm Springs 2012 2 CAA
CAA Conference alm Springs 2012 The Coagulation Workup In The Office Setting CAA Conference alm Springs, October 2012 Robert Miller, A-C Henoch-Schoenlein urpura 1 CAA Conference alm Springs 2012 2 CAA
Disclosures. I have received research funding from: I have received consulting fees/honoraria from: Novo Nordisk CSL-Behring Boehringer Ingelheim
 Test Disclosures I have received research funding from: Novo Nordisk CSL-Behring Boehringer Ingelheim I have received consulting fees/honoraria from: Novo Nordisk CSL-Behring Baxter The Medicines Company
Test Disclosures I have received research funding from: Novo Nordisk CSL-Behring Boehringer Ingelheim I have received consulting fees/honoraria from: Novo Nordisk CSL-Behring Baxter The Medicines Company
Use of ROTEM from the Laboratory Perspective. A/Prof David Roxby SA Pathology
 Use of ROTEM from the Laboratory Perspective A/Prof David Roxby SA Pathology What s the Problem? Constant changes in treatment recommendations Lack of good evidence to guide practice Variations in clinical
Use of ROTEM from the Laboratory Perspective A/Prof David Roxby SA Pathology What s the Problem? Constant changes in treatment recommendations Lack of good evidence to guide practice Variations in clinical
These slides and the data they contain are the sole property of the author(s) of the slide set.
 These slides and the data they contain are the sole property of the author(s) of the slide set. Reproduction or distribution of the content of the slides or the data they contain requires the prior, specific
These slides and the data they contain are the sole property of the author(s) of the slide set. Reproduction or distribution of the content of the slides or the data they contain requires the prior, specific
Factor VIII Concentrate Factor IX Complex (Coagulation Factors, II, VII, IX, X) Concentrate
 Factor VIII Concentrate Factor IX Complex (Coagulation Factors, II, VII, IX, X) Concentrate Application for retention on the WHO Model List From: Plasma Protein Therapeutics Association (PPTA) 1. Summary
Factor VIII Concentrate Factor IX Complex (Coagulation Factors, II, VII, IX, X) Concentrate Application for retention on the WHO Model List From: Plasma Protein Therapeutics Association (PPTA) 1. Summary
CLOTTING FACTORS AND COAGULANT BLOOD PRODUCTS
 UnitedHealthcare Commercial Medical Benefit Drug Policy CLOTTING FACTORS AND COAGULANT BLOOD PRODUCTS Policy Number: 2018D0047K Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Medical Benefit Drug Policy CLOTTING FACTORS AND COAGULANT BLOOD PRODUCTS Policy Number: 2018D0047K Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
Subject: Clotting Factors and Coagulant Blood Products
 09-J0000-34 Original Effective Date: 03/15/01 Reviewed: 04/11/18 Revised: 03/15/19 Subject: Clotting Factors and Coagulant Blood Products THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
09-J0000-34 Original Effective Date: 03/15/01 Reviewed: 04/11/18 Revised: 03/15/19 Subject: Clotting Factors and Coagulant Blood Products THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
Blood essentials. 16 Nursing made Incredibly Easy! March/April 2013
 Blood essentials One unit of whole blood yields many components that are used to support life-threatening conditions. Managing blood transfusions requires knowledge of blood products and practice guidelines
Blood essentials One unit of whole blood yields many components that are used to support life-threatening conditions. Managing blood transfusions requires knowledge of blood products and practice guidelines
Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation
 Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation Ayesha Ather, PharmD, BCPS College of Pharmacy, Adjunct Assistant Professor University of Kentucky Faculty Disclosure I have
Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation Ayesha Ather, PharmD, BCPS College of Pharmacy, Adjunct Assistant Professor University of Kentucky Faculty Disclosure I have
Transfus Med Hemother 2009;36:
 Transfus Med Hemother 2009;36:419 436 7 Procoagulators 7.1 Fibrinogen 7.1.1 Preparation, Quality Criteria 7.1.2 Active Constituents 7.1.3 Physiological Function 7.1.4 Application 7.1.4.1 Congenital Fibrinogen
Transfus Med Hemother 2009;36:419 436 7 Procoagulators 7.1 Fibrinogen 7.1.1 Preparation, Quality Criteria 7.1.2 Active Constituents 7.1.3 Physiological Function 7.1.4 Application 7.1.4.1 Congenital Fibrinogen
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency Evaluation of Medicines for Human Use London, 29 July 2004 CPMP/BPWG/1089/00 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON THE CLINICAL INVESTIGATION OF PLASMA
European Medicines Agency Evaluation of Medicines for Human Use London, 29 July 2004 CPMP/BPWG/1089/00 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON THE CLINICAL INVESTIGATION OF PLASMA
Adv Pathophysiology Unit 4 Page 1 of 10. Learning Objectives for this file:
 Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
Improving Outcomes of Cardiac Surgery with a Point-of-Care Based Transfusion Algorithm
 Improving Outcomes of Cardiac Surgery with a Point-of-Care Based Transfusion Algorithm Summer Syed (local PI) Keyvan Karkouti Deputy Anesthesiologist-in-Chief, Toronto General Hospital, University Health
Improving Outcomes of Cardiac Surgery with a Point-of-Care Based Transfusion Algorithm Summer Syed (local PI) Keyvan Karkouti Deputy Anesthesiologist-in-Chief, Toronto General Hospital, University Health
Haemostasis. The function of haemostasis is: to prevent blood loss from injured vessels. to stop bleeding. to prevent thrombosis
 Haemostasis Haemostasis The function of haemostasis is: to prevent blood loss from injured vessels to stop bleeding to prevent thrombosis Haemostasis blood endothelium basement membrane subendothelium
Haemostasis Haemostasis The function of haemostasis is: to prevent blood loss from injured vessels to stop bleeding to prevent thrombosis Haemostasis blood endothelium basement membrane subendothelium
Coagulation. Coagulation Limited CGL, CGDF Surveys & Anatomic Pathology Education Programs. Coagulation 117
 www.cap.org Coagulation Analytes/procedures in bold type are regulated for proficiency testing by the Centers for Medicare & Medicaid Serviced (CMS). Coagulation Limited CGL, CGDF Analyte CGL CGDF New
www.cap.org Coagulation Analytes/procedures in bold type are regulated for proficiency testing by the Centers for Medicare & Medicaid Serviced (CMS). Coagulation Limited CGL, CGDF Analyte CGL CGDF New
Obstetrical (OB) Hemorrhage Guidelines
 Obstetrical (OB) Hemorrhage Guidelines This document has been prepared by the Puget Sound Blood Center Transfusion Safety and Patient Blood Management Department to provide information necessary to obtain
Obstetrical (OB) Hemorrhage Guidelines This document has been prepared by the Puget Sound Blood Center Transfusion Safety and Patient Blood Management Department to provide information necessary to obtain
Biotechnology of Human Plasma-Derived Medicines in Scope of Collaboration Perspectives within The Central European Initiative
 Biotechnology of Human Plasma-Derived Medicines in Scope of Collaboration Perspectives within The Central European Initiative Dr Vadim Sentchouk PHARMLAND LLC Deputy General Director PLASMAPHARM LLC General
Biotechnology of Human Plasma-Derived Medicines in Scope of Collaboration Perspectives within The Central European Initiative Dr Vadim Sentchouk PHARMLAND LLC Deputy General Director PLASMAPHARM LLC General
2017 AABB Annual Meeting On-Demand SAM Sessions
 2017 AABB Annual Meeting On-Demand SAM Sessions The following 14 SAM sessions from the 2017 AABB Annual Meeting are eligible for up to 17.75 SAM eligible credits. The number of credits is based on the
2017 AABB Annual Meeting On-Demand SAM Sessions The following 14 SAM sessions from the 2017 AABB Annual Meeting are eligible for up to 17.75 SAM eligible credits. The number of credits is based on the
General News. Product Notes. Instrument Notice HELENA SALES FORCE TO: FROM: SUBJECT: HELENA POINT OF CARE ROUND-UP/US DOMESTIC DATE: 9/1/2009
 TO: FROM: SUBJECT: HELENA SALES FORCE DATE: 9/1/2009 General News HELENA POINT OF CARE ROUND-UP/US DOMESTIC We have concluded a very large meeting with the AACC in Chicago. The leads have been processed
TO: FROM: SUBJECT: HELENA SALES FORCE DATE: 9/1/2009 General News HELENA POINT OF CARE ROUND-UP/US DOMESTIC We have concluded a very large meeting with the AACC in Chicago. The leads have been processed
Common Inherited Bleeding Disorders
 CAA 2015 Annual Conference Common Inherited Bleeding Disorders Bob Miller, A October 8, 2015 VWF has two jobs Loosely bound to protect FVIII and tether to site of injury All other coagulation factors also
CAA 2015 Annual Conference Common Inherited Bleeding Disorders Bob Miller, A October 8, 2015 VWF has two jobs Loosely bound to protect FVIII and tether to site of injury All other coagulation factors also
The World Health Assembly Resolution on availability, safety and quality of blood products (WHA 63.12) Adopted May 2010
 The World Health Assembly Resolution on availability, safety and quality of blood products (WHA 63.12) Adopted May 2010 Dr Ana Padilla Blood Products & related Biologicals Essential Medicines and Pharmaceutical
The World Health Assembly Resolution on availability, safety and quality of blood products (WHA 63.12) Adopted May 2010 Dr Ana Padilla Blood Products & related Biologicals Essential Medicines and Pharmaceutical
TAYSIDE GUIDE TO MASSIVE TRANSFUSION/BLOOD LOSS
 HTC 11/02 TAYSIDE GUIDE TO MASSIVE TRANSFUSION/BLOOD LOSS This local guide should be used in conjunction with the guidelines published by the British Committee for Standards in Haematology. Definition:
HTC 11/02 TAYSIDE GUIDE TO MASSIVE TRANSFUSION/BLOOD LOSS This local guide should be used in conjunction with the guidelines published by the British Committee for Standards in Haematology. Definition:
BLOOD COMPONENT THERAPY
 BLOOD COMPONENT THERAPY Original Article by: Dr Lara Herbert, Dr Rob Price, Royal Devon and Exeter Hospital, UK INTRODUCTION Blood products are any therapeutic substances that are prepared from human blood.
BLOOD COMPONENT THERAPY Original Article by: Dr Lara Herbert, Dr Rob Price, Royal Devon and Exeter Hospital, UK INTRODUCTION Blood products are any therapeutic substances that are prepared from human blood.
Celluvative. Cellular Therapies Redefined. A portfolio of products and services brought to you by: Saving lives today. Improving life tomorrow.
 Cellular Therapies Redefined A portfolio of products and services brought to you by: Saving lives today. Improving life tomorrow. cell u va tive / sel-yoo-vā-tiv/ noun 1. a partnership between BloodCenter
Cellular Therapies Redefined A portfolio of products and services brought to you by: Saving lives today. Improving life tomorrow. cell u va tive / sel-yoo-vā-tiv/ noun 1. a partnership between BloodCenter
Surgical Adhesives in Facial Plastic Surgery
 Surgical Adhesives in Facial Plastic Surgery Dean M. Toriumi, Victor K. Chung, Quintin M. Cappelle University of Illinois at Chicago Chicago, IL Supplement to Toriumi DM, Chung VK, Cappelle QM. Surgical
Surgical Adhesives in Facial Plastic Surgery Dean M. Toriumi, Victor K. Chung, Quintin M. Cappelle University of Illinois at Chicago Chicago, IL Supplement to Toriumi DM, Chung VK, Cappelle QM. Surgical
GUIDELINES FOR IDENTIFICATION AND INDICATION OF BLOOD COMPONENTS AND BLOOD PRODUCTS.
 GUIDELINES FOR IDENTIFICATION AND INDICATION OF BLOOD COMPONENTS AND BLOOD PRODUCTS. Hur sluta röka cold turkey 1. Policy Statement The Regional Health Authorities should develop policies that: 1.1 Provide
GUIDELINES FOR IDENTIFICATION AND INDICATION OF BLOOD COMPONENTS AND BLOOD PRODUCTS. Hur sluta röka cold turkey 1. Policy Statement The Regional Health Authorities should develop policies that: 1.1 Provide
Common Inherited Coagulation Disorders. Inherited Coagulation Disorders. All coagulation factors and platelets in circulation (unactivated)
 Common Inherited Coagulation Disorders Bob Miller, A 2017 Inherited Coagulation Disorders Brief review of coagulation Disorders related to platelet dysfunction (not the acquired thrombocytopenias) Disorders
Common Inherited Coagulation Disorders Bob Miller, A 2017 Inherited Coagulation Disorders Brief review of coagulation Disorders related to platelet dysfunction (not the acquired thrombocytopenias) Disorders
Critical Quality Attributes for Blood Products. Tim Lee, Ph.D. OBRR/CBER/FDA 12 January 2009 WCBP
 Critical Quality Attributes for Blood Products Tim Lee, Ph.D. OBRR/CBER/FDA 12 January 2009 WCBP 1 Disclaimer The views expressed during this presentation are my own and may not be those of the FDA 2 Blood
Critical Quality Attributes for Blood Products Tim Lee, Ph.D. OBRR/CBER/FDA 12 January 2009 WCBP 1 Disclaimer The views expressed during this presentation are my own and may not be those of the FDA 2 Blood
TSOAC Case Study 1. Question. TSOAC Case Study 1 Continued
 TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
Pharmacology Lecture 5. Anticoagulants
 Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Hematotoxin producing snakes in Thailand พญ.ม ชฌ มา รอดเช อ พญ.อ สร ย หาญอ ท ยร ศม
 Hematotoxin producing snakes in Thailand พญ.ม ชฌ มา รอดเช อ พญ.อ สร ย หาญอ ท ยร ศม Hematotoxin producing snakes Pit vipers (Crotalinae) Malayan pit viper (Calloselasma rhodostoma) Green pit viper (Trimeresurus
Hematotoxin producing snakes in Thailand พญ.ม ชฌ มา รอดเช อ พญ.อ สร ย หาญอ ท ยร ศม Hematotoxin producing snakes Pit vipers (Crotalinae) Malayan pit viper (Calloselasma rhodostoma) Green pit viper (Trimeresurus
Coagulation Laboratory: Methods, Standards & Cost Effective Testing Part 1
 Coagulation Laboratory: Methods, Standards & Cost Effective Testing Part 1 Donna D. Castellone, MS, MT (ASCP) SH Clinical Project Manager Hematology and Hemostasis Siemens Healthcare Diagnostics Disclosures
Coagulation Laboratory: Methods, Standards & Cost Effective Testing Part 1 Donna D. Castellone, MS, MT (ASCP) SH Clinical Project Manager Hematology and Hemostasis Siemens Healthcare Diagnostics Disclosures
ABO, Rh, HLA Antibodies Issues with Whole Blood NANCY M. DUNBAR, MD MEDICAL DIRECTOR, BLOOD BANK DARTMOUTH-HITCHCOCK MEDICAL CENTER, LEBANON, NH, USA
 ABO, Rh, HLA Antibodies Issues with Whole Blood NANCY M. DUNBAR, MD MEDICAL DIRECTOR, BLOOD BANK DARTMOUTH-HITCHCOCK MEDICAL CENTER, LEBANON, NH, USA The Appeal of Whole Blood WHOLE BLOOD IN EXSANGUINATING
ABO, Rh, HLA Antibodies Issues with Whole Blood NANCY M. DUNBAR, MD MEDICAL DIRECTOR, BLOOD BANK DARTMOUTH-HITCHCOCK MEDICAL CENTER, LEBANON, NH, USA The Appeal of Whole Blood WHOLE BLOOD IN EXSANGUINATING
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS
 Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
