Thoracoscopic lobectomy for benign disease ± a single centre study on 64 cases q
|
|
|
- Meagan Roberts
- 6 years ago
- Views:
Transcription
1 European Journal of Cardio-thoracic Surgery 20 (2001) 443±448 Thoracoscopic lobectomy for benign disease ± a single centre study on 64 cases q Alberto Weber, Uz Stammberger, Ilhan Inci, Ralph A. Schmid, Andre Dutly, Walter Weder* Division of Thoracic Surgery, University Hospital, Raemistrasse 100, CH-8091 Zurich, Switzerland Received 10 October 2000; received in revised form 14 March 2001; accepted 19 March 2001 Abstract Objective: Chronic lung infection is the main indication for lobectomy in benign pulmonary disease and may be technically demanding due to in ammatory changes such as adhesions, lymph node enlargement and neovascularization. The role of the thoracoscopic operation in these indications is yet ill-de ned. Methods: We retrospectively analyzed the results of patients who underwent thoracoscopic lobectomy (TL) between 1992 and June 1999 and compared this study group with patients who underwent open lobectomy (OL), all for benign disease. Data were not normally distributed, therefore, the median and range is given and nonparametric statistical analysis was applied. Results: A total of 117 lobectomies for benign disease (64 TL) were analyzed. Indications included bronchiectasis (36 TL; 18 OL), chronic infections (13 TL; eight OL), tuberculosis ( ve TL; 15 OL), emphysema ( ve TL; one OL), AV-malformations (two TL; one OL), severe haemoptysis (four OL), and others (three TL; six OL). Twelve conversions to thoracotomy were necessary due to severe adhesions. One patient in the open lobectomy group died within 30 days postoperative. Drainage time was 5.0 (1±32) days in TL and 6.0 (3±21) days in OL, hospital stay was 8.5 (4±41) days and 10.0 (5±52) days, respectively. Blood loss was 0 (0±2000) ml in TL and 300 (0±6000) ml in OL.Operation time for thoracoscopic lobectomies signi cantly decreased from 2.5 (1±6) h for cases between 1992 and 1997 (n ˆ 49) to 1.5 (0.5±2.5) h for recent cases (n ˆ 15) (P, 0:01). In addition, a trend towards less blood loss was noted (100 (0±2000) ml vs. 0 (0±400) ml; P ˆ 0:06). Drainage time and hospital stay did not differ signi cantly. Conclusions: Thoracoscopic lobectomy in chronic in ammatory disease can be performed safely in selected patients, especially with bronchiectasis. Conversion rate to thoracotomy is low. Operation time with this approach declined signi cantly over time. q 2001 Elsevier Science B.V. All rights reserved. Keywords: Video-assisted-thoracoscopic-surgery; Lobectomy; Benign-lung-disease 1. Introduction q Presented at the 14th Annual Meeting of the European Association for Cardio-thoracic Surgery, Frankfurt, Germany, October 7±11, * Corresponding author. Tel.: ; fax: address: walter.weder@chi.usz.ch (W. Weder). Advances in video-assisted thoracoscopic surgery (VATS) instruments, imaging technology and surgical techniques have promoted a rapid increase in the number and variety of operations performed using this technique. Several clinical series demonstrated that VATS had similar ef cacy to open thoracotomy while providing the bene ts of decreased pain-related morbidity, functional disability and hospital stay [1±7]. Successful implementation of this goal has made VATS the preferred approach to the diagnosis and treatment of many thoracic disease processes. The technical feasibility of major lung resections using VATS have been shown by several surgeons [8±17]. However reports in the literature on thoracoscopic anatomic lung resections were almost exclusively devoted to the treatment of early bronchogenic carcinoma with few exceptions (Table 1). VAT lobectomy for benign lung disease has been speci cally addressed by Yim [15] reporting on ten cases. Chronic lung infection is the main indication for lobectomy in benign pulmonary disease and therefore may be technically demanding due to acute and chronic in ammatory changes such as adhesions, lymph node enlargement and increased bleeding due to neovascularization. The role of the thoracoscopic operation in these situations is yet illde ned. Herein, we report our experience with 64 patients treated with VATS lobectomy for benign lung disease in order to de ne indications and limits. 2. Material and methods From January 1992 to June 1999, 117 patients underwent lobectomy for benign disease at our institution. Among them, 64 selected patients underwent a VAT-lobectomy /01/$ - see front matter q 2001 Elsevier Science B.V. All rights reserved. PII: S (01)
2 444 A. Weber et al. / European Journal of Cardio-thoracic Surgery 20 (2001) 443±448 Table 1 Major published series of video-assisted thoracic surgical lobectomy and pneumonectomy [17] a Reference No. Cancer Benign Mortality (%) Length of stay Lewis & Caccavale (1998) Yim et al. (1998) (0.4) 6.8 Kasada et al. (1998) (0.8) NA Hermansson et al. (1998) Walker et al. (1996) (2) 7.2 Roviaro et al. (1998) (0.5) NA McKenna et al. (1998) (0.5) 4.6 Weber et al Total (0.6) 5.28 a No., number of patients. NA, not available. and 53 patients a conventional open lobectomy after informed consent was obtained. Selection criteria included symptomatic patients who had failed medical treatment, continued to have productive cough, hemoptysis and failure to thrive. In some instances patients were admitted on an emergency basis for acute hemoptysis. All patients received routine chest X-ray and a high resolution computed tomograph scanning of the thorax while the majority underwent a bronchoscopy. In all elective cases pulmonary function was determined by spirometry. In cases of respiratory limitation a perfusion lung scan was added. Patients were selected for VATS if they were under stable cardio-pulmonary conditions and the procedure was planned as an elective operation. In cases with evidence for severe parenchymal and or pleural scarring on CT scan we directly performed an open procedure. This selection was based on the surgeon's judgement. Patient characteristics, type of lobectomies and indications are shown in Tables 2 and 3. After induction of general anaesthesia with a double lumen endotracheal tube, the patient is placed in a full lateral decubitus position with the upper arm suspended on a crossbar. In VATS procedures, a collapse of the lung was achieved with unilateral lung ventilation, and the rst 10 mm trocar was introduced in the sixth (for upper lobe), seventh (for middle and lower lobes) or eighth (lung sequestration, heavy scarring on the diaphragm) intercostal space on the midaxillary line. The optical instrument with a 308 lens and videocamera (Wolf CCT- Endocam 5370) attached was introduced, the cavity was carefully explored and the feasibility of a videoscopic procedure was con rmed. The operating trocars were then inserted under direct endoscopic control, usually in the fourth, fth or sixth intercostal space (Fig. 1). We use three 10 mm trocars and one or two 5/6 mm trocars. All preparations are done through the inserted trocars and at the end of the procedure the lobe is removed in a plastic bag from the enlarged ventral trocar port (6±8 cm). In thoracoscopic lobectomy with minithoracotomy we use two 10 mm trocars and one 5 mm trocar, followed by the union of two trocar ports with the result of an anteriolateral minithoracotomy (8±10 cm) without rib cutting. In this method some of the preparations are done through the minithoracotomy incision. The hilar dissection is done as in open lobectomy. This included the individual isolation of vessels and bronchus. Dissection was performed using electrocoagulating endoscissors or endoswabs, for blunt dissection. All major pulmonary arteries and veins were transected using endoscopic stapling devices (Endo GIA-30-Autosuture). Lobar bronchi were closed by a linear stapling device (TLH-30 or the ET 45 B, Ethicon). Incomplete ssures were divided by using a stapler (ET 45, Ethicon).The lung Table 2 Characteristics of the study groups a VATS/1992Ð1999 n ˆ 64 Open lobectomy n ˆ 53 VATS/ n ˆ 15 Sex 36 F/28 M 25 F/28 M 11 F/4 M Age (mean) 54.5 (20Ð81) 47.1 (17±82) 51.8 (36Ð75) Type of lobectomy n % n % n % RUL ML RLL LUL LLL a F, female; LLL, left lower lobectomy; LUL, left upper lobectomy; M, male; ML, middle lobectomy; RLL, right lower lobectomy; RUL, right upper lobectomy; VATS, video-assisted thoracoscopic surgery.
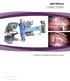
3 Table 3 Indications according to the groups a A. Weber et al. / European Journal of Cardio-thoracic Surgery 20 (2001) 443± VATS/1992Ð1999 Open lobectomy VATS/ Disease n % n % n % Bronchiectasis Chronic lung infections Tuberculosis Emphysema 5 1 AV-malformations 2 1 Severe hemoptysis 0 4 Lung sequestration 3 3 Others 0 3 a n, number of patients. specimen was then placed in a plastic bag for removal through a minithoracotomy incision. At the end of the procedure, usually two chest tubes were inserted through the trocar incisions and connected to a closed chest tube drainage system with suction of 225 cm H 2 O. We reviewed all data of the studied patients for indication, surgical technique, conversion rate from VATS to open lobectomy, resected lobe, operation time, blood loss, drainage time, hospital stay, early postoperative morbidity and mortality. We especially evaluated VATS lobectomies which were carried out in the last 2 years and compared them with those performed in the early phase Statistical analysis Data were analyzed with Mann±Whitney U-test. All values are expressed as median and range. A P value less than 0.05 was considered signi cant. 3. Results In 76 cases we intended to perform a video-assisted thoracoscopic lobectomy. This procedure was successfully Fig. 1. (1) Main trocar port for camera; (2) operating trocar (exchangeable for camera); (3) operating trocar (exchangeable for camera); (4) lung forceps (5 mm); (5) lung forceps (5 mm). completed in 64 patients. In 12 cases the thoracoscopic approach (15.3%) had to be converted to a antero-lateral thoracotomy because of either dense adhesions, massive in ammatory lymph node enlargement with neovascularization or a closed ssure. The conversion rate to thoracotomy between 1992 and 1997 was 15.8% and was comparable with the second phase performed between 1998 and 1999 (10.2%). There was no emergency conversion thoracotomy due to a major bleeding. In 17 of 64 cases an early minithoracotomy of 8±10 cm. was necessary to ease the dissection of in ammatory changes. In the other cases the minithoracotomy (6±8 cm) was done at the end to harvest the resected lung specimen. There was no hospital death in the VATS group. One patient in the open lobectomy group died within 30 days postoperatively due to multiorgan failure after an emergency operation because of massive hemoptysis. A total of 17 patients underwent an urgent operation because of hemoptysis and all of them were managed with a standard lobectomy. Of these, four patients with massive bleeding had an emergency operation. Operation time, blood loss, drainage time and hospital stay for VATS lobectomy were lower compared to open thoracotomy, but the differences did not reach statistical signi cancy. However operation time signi cantly decreased for VATS lobectomy between 1998 and June 1999 compared to those between 1992 and 1997 (P ˆ 0:01). In addition, a trend towards less blood loss, fewer drainage time and hospital stay was noted (Table 4). Twelve patients (18.7%) of the VATS lobectomy group and 23 (43.4%) of the open lobectomy group experienced nonfatal complications. Prolonged parenchymal stulas (.7 days) developed in six cases among VATS (9.3%) and ve cases among open lobectomy patients (9.4%). One patient (1.5%) developed a hemothorax in the VATS group compared to seven (13.2%) patients after open lobectomy. After VATS lobectomy 3 patients (4.7%) required reoperation, all for control of pneumothorax caused by parenchymal stulas. In the open lobectomy group seven patients (13.2%) required reoperation for control of hemothorax or prolonged air leak. Postoperative pneumonia developed in three patients (4.7%) after video-assisted procedure and eight
4 446 A. Weber et al. / European Journal of Cardio-thoracic Surgery 20 (2001) 443±448 Table 4 Operative and postoperative results of the groups VATS/1992±1999 Open lobectomy VATS/ Operating time, hours Median Range 0.5±6 1±4 0.5±2.5 Blood loss, ml Median Range 0±2000 0±6000 0±400 Drainage time, days Median Range 1±32 3±21 1±9 Hospital stay, days Median Range 4±41 5±52 4±16 (15%) after standard thoracotomy. Postoperative cardiac arrhythmias, occurred in two of VATS and three of open lobectomy cases. Overall complication rate was reduced to 10% among the last twenty VATS patients. 4. Discussion There have been several reports testifying the technical feasibility of video-assisted thoracoscopic major lung resections [9±14]. In the early 1990s, dif culties were due to the lack of adequate thoracoscopic instrumentation [10]. As predicted by Giudicelli [8], thanks to advances in videoendoscopic instrumentation and endosurgical techniques, the indications of video-assisted lobectomy have been extended to a larger patient population in the last few years. Results of published series of VATS lobectomy and pneumonectomy [17] showed favourable results compared with a thoracotomy (Table 1). In these series, complications occurred in 10.0±21.9%. Conversion from VATS to thoracotomy was necessary in 0±19.5% of patients. Overall, 119 of 1120 operations were converted to thoracotomy (11.6%). Most commonly, oncologic reasons prompted the conversion. Approximately 30% of the conversions to thoracotomy were for nononcologic reasons, such as pleural symphysis. A direct comparison between these two groups is rather dif cult because of the heterogeneity of the patients characteristics. However, there are major differences between anatomic resections of benign or malignant disease through minimal access. The existing literature is mostly devoted to the treatment of early bronchogenic carcinoma [15] (Table 1). Yim and co-workers [15] discussed for the rst time VATS lobectomies speci cally for benign disease in ten cases. They reported three major differences compared to resection for malignant disease. First, adequacy of tumor clearance is not relevant. Second, in ammatory changes may render dissection more dif cult especially in certain disease like tuberculosis. Third, while tumor seeding is a concern in malignant neoplasms, wound infection is a concern in resections for an infectious disease. Roviaro and co-workers [10] stated that all benign pulmonary disease can be explored thoracoscopically, but the feasibility of resection depends on the local anatomic situation especially adhesions. They described that in the setting of in ammatory pathologic conditions such as purulent bronchiectasis, dissection of the pulmonary vessels within the ssure may be very dif cult if there were dense adhesions or enlarged lymph nodes, especially calci ed. In our experience we found that the severity of adhesions to the chest wall, the hilum and especially in the ssure, typically seen in in ammatory disease is the key limiting factor for a safe VATS lobectomy. It necessitates patience for the surgeon to complete the operation by VATS. Adhesions have to be dissected stepwise to safely explore the relevant anatomy. Destroyed lobes mainly after tuberculosis with or without aspergillosis were all directed to open lobectomy due to these dif culties. It is not surprising that prolonged air leaks were the major morbidity both after VATS as well as open lobectomy for in ammatory disease. However wound infections were not seen in trocar sites nor in the thoracotomy. In our series the conversion rate from VATS to thoracotomy was 15.3%. We consider this not as a failure rather than a safety measure. All these patients suffered from extended adhesions with chronic in ammatory changes, except for one patient with a large arterio-venous malformation of the middle lobe. Among the VATS lobectomy group, 50% of patients with tuberculosis had to be managed with an open lobectomy nally. Considering the subgroup of patients operated on for bronchiectasis and undergoing middle lobe resection between 1998 and 1999, conversion rate fell to 6.25% (10.3% for the whole group). Furthermore, for these the overall complication rate was only 10% and the operation time was signi cantly shorter. In addition there was no mortality and a trend towards less blood loss, shorter drainage time and hospital stay was achieved. Twelve patients (18.7%) of the VATS lobectomy group experienced nonfatal complications. This is comparable to the data in a collected review were the complication rate
5 A. Weber et al. / European Journal of Cardio-thoracic Surgery 20 (2001) 443± was between 10±22% (Table 1). We did not perform an emergency conversion to thoracotomy, which happened in ten cases within studies. In the VATS group middle and lower left lobectomies were most often performed. These are technically easier than upper lobectomies, especially on the left side [12,18± 20]. However all other possible lobectomies were also performed safely, but in less number. A trend to mainly middle and lower lobectomy was seen in the last 2 years with more than 90%. This corroborates a more selective disease- and localization-related indication for videoassisted thoracoscopic management of benign diseases. More than 2/3 of our bronchiectasis patients were successfully treated with a video-assisted thoracoscopic lobectomy. Segmentectomy may be the surgical treatment of choice in situations with well-localized bronchiectasis [22]. However all of these were done as open procedures. On the contrary, all type of lobectomies, independent from the technical dif culties, were carried out by a standard thoracotomy. Compared with VATS, more upper lobes were resected where tuberculosis is more likely to be localized [21]. Only in ve selected cases of tuberculosis VATS lobectomy was successfully completed. Dense adhesions and calci ed lymph nodes, led to a high conversion rate to thoracotomy (50%). In addition, in patients with known or presumed tuberculosis, with extensive intraparenchymal scarring, the question of malignancy is often present. Therefore, the management of these individuals, must be adjusted. Between 1998 and 1999, all patients with tuberculosis were directed to standard thoracotomy for lobectomy. Our results suggest that video assisted thoracoscopic lobectomy in chronic in ammatory diseases can be performed safely in selected patients, especially with bronchiectasis. Radiological signs of severe scarring and adhesions on CT scan indicates the need of thoracotomy. Beside adequate selection, the growing experience of the surgeon has an important impact on the outcome [7]. Since our patients were pleased with the rapid postoperative recovery and the favorable cosmetic result, it became the surgical treatment of choice for these indications. References [1] Landreneau RJ, Hazelrigg SR, Mack MJ, Dowling RD, Burke D, Gavlick J, Perrino MK, Ritter PS, Bowers CM, DeFino J. Postoperative pain-related morbidity: video-assisted thoracic surgery versus thoracotomy. Ann Thorac Surg 1993;56(6):1285±1289. [2] Landreneau RJ, Mack MJ, Hazelrigg SR, Naunheim K, Dowling RD, Ritter P, Magee MJ, Nunchuck S, Keenan RJ, Ferson PF. Prevalence of chronic pain after pulmonary resection by thoracotomy or VATS. J Thorac Cardiovasc Surg 1994;107(4):1079±1086. [3] Landreneau RJ, Wiechmann RJ, Hazelrigg SR, Mack MJ, Keenan RJ, Ferson PF. Effect of minimally invasive thoracic surgical approaches on acute and chronic postoperative pain. Chest Surg Clin N Am 1998;8(4):891±906. [4] Hazelrigg SR, Landreneau RJ, Boley TM, Priesmeyer M, Schmaltz RA, Nawarawong W, Johnson JA, Walls JT, Curtis JJ. The effect of muscle sparing versus standard posterolateral thoracotomy on pulmonary function, muscle strength, and postoperative pain. J Thorac Cardiovasc Surg 1991;101(3):394±401. [5] Hazelrigg SR, Nunchuck SK, LoCicero J. Video assisted thoracic surgery study group data. Ann Thorac Surg 1993;56(5):1039±1044. [6] Nakata M, Saedi H, Yokoyama N, Kurita A, Takiyama W, Takashima S. Pulmonary function after lobectomy: video-assisted thoracic surgery versus thoracotomy. Ann Thorac Surg 2000;70:938±941. [7] Stammberger U, Steinacher C, Hillinger S, Schmid RA, Kinsbergen T, Weder W. Early and long-term complaints following videoassisted thoracoscopic surgery: evaluation in 173 patients. Eur J Cardio-thorac Surg 2000;18(1):7±11. [8] Giudicelli R, Thomas P, Lonjon T, Jacques R, Morati N, Ottomani R, Fuentes PA, Shennib H, Noirclerc M. Video-assisted minithoracotomy versus muscle-sparing thoracotomy for performing lobectomy. Ann Thorac Surg 1994;58:712±718. [9] Lewis RJ. The role of video-assisted thoracic surgery for carcimoma of the lung: wedge resection to lobectomy by simultaneous individual stapling. Ann Thorac Surg 1993;56:762±768. [10] Roviaro G, Varoli F, Rebuffat C, Vergani C, D'Hoore A, Scalambra SM, Maciocco M, Grignani F. Major pulmonary resections: pneumonectomies and lobectomies. Ann Thorac Surg 1993;56:779±783. [11] Walker WS, Carnochan FM, Pugh GC. Toracoscopic pulmonary lobectomy: early operative experience and preliminary clinical results. J Thorac Cardiovasc Surg 1993;106:1111±1117. [12] Kirby TJ, Mack MJ, Landreneau RJ. Initial experience with video assisted thoracoscopic lobectomy. Ann Thorac Surg 1993;56:1248± [13] McKenna RJ. Lobectomy by video-assisted thoracic surgery with mediastinal node sampling for lung cancer. J Thorac Cardiovasc Surg 1994;107:879±882. [14] Yim APC, Ho JKS. Video assisted thoracoscopic lobectomy a word of caution. Aust NZ J Surg 1995;65:438±441. [15] Yim APC, Ko K, Ma C, Chau W, Kyaw K. Thoracoscopic lobectomy for benign diseases. Chest 1996;109:554±556. [16] McKenna RJ. VATS lobectomy with mediastinal node sampling or dissection. Chest Surg Clin N Am 1995;4:223. [17] McKenna RJ. Video-assisted thoracic surgery for wedge resection, lobectomy, and pneumonectomy. In: Shields TW, LoCicero III J, Ponn RB, editors. General thoracic surgery. Philadelphia: Lippincott Williams and Wilkins, pp. 455±462. [18] Lin JC, Landreneau RJ. Instruments and techniques of video-assisted thoracic surgery. In: Shields TW, LoCicero III J, Ponn RB, editors. General thoracic surgery. Philadelphia: Lippincott Williams & Wilkins, pp. 439±453. [19] Kirby TJ, Rice TW. Thoracoscopic lobectomy. Ann Thorac Surg 1993;56:784±786. [20] Stamatis G, Fechner S. Die videothoracoskopische Lobektomie. Chirurg 1996;67:425±435. [21] Shields TW, Pomerantz M. Pulmonary Tuberculosis and other mycobacterial infections of the lung. (Chapter 85 A and B). In: Shields TW, LoCicero III J, Ponn RB, editors. General thoracic surgery. Philadelphia: Lippincott Williams & Wilkins, pp. 1053±1075. [22] Ris HB, Stocker JM, Im Hof V. Lungenabszesse und Bronchiektasen. Schweiz Med Wochenschr 1999;129:547±555. Appendix A. Conference discussion Dr H.B. Ris (Lausanne, Switzerland): You did most of your operations for bronchiectasis, and, as far as I understood, most of these bronchiectases were localized in the lower lobes. Why have you not considered a segmentectomy? Usually the bronchiectases are situated in the basal segments leaving a nice and voluminous superior segment and I always nd it a pity to sacri ce this segment. Could you comment on that, please?
6 448 A. Weber et al. / European Journal of Cardio-thoracic Surgery 20 (2001) 443±448 Dr Weber: We also agree that segmentectomy has to be considered for bronchiectasis, but for well-localized bronchiectasis only. In these cases, bronchiectases weren't as localized, so lobectomy couldn't be avoided. Dr P. Thomas (Marseille, France): In Marseille we have strictly the same gures that you showed. I have a question regarding what you call your standard thoracotomy. Do you use a muscle-sparing thoracotomy, and, if so, do you note any difference between video-assisted minithoracotomy and a standard muscle-sparing thoracotomy? Dr Weber: Our standard thoracotomy is an anterolateral thoracotomy with rib cutting. We did not study the difference in regard of pain etc. between the two groups. Dr Thomas: In your opinion, what is the main bene t of VATS surgery for lobectomy, for major pulmonary resection in the setting of benign disease? Dr Weber: We can say at this point that the patient's opinion is really important. All of them prefer this approach. The patient's comfort after the operation is much better. It has been also reported that compared to open thoracotomy, this technique compares favorably to it. Dr G. Cardillo (Rome, Italy): You have treated three patients with lung sequestration by VATS. Did you know the diagnosis before surgery? Do you think that sequestration is a safe indication for VATS? Dr Weber: In these cases the diagnosis was expected from the CT scan. It was in a few cases and it was safe. They were all intrapulmonary sequestration. Dr Ris: Walter, do you want to comment on that? Dr W. Weder (Zurich, Switzerland): Indeed VATS lobectomy for lung sequestration may be a critical issue. First you must anticipate the diagnosis from the CT scan; otherwise, your preparation above the diaphragm could lead to a major bleeding by injuring the aberrant artery. In these three cases we completed all procedures by VATS. The artery was nicely seen and safely divided by a stapler. In three other cases they were done by open thoracotomy. All of them were started by VATS, but because of dense adhesions the isolation of the artery was not safe. We converted at times to an open procedure just for safety reasons. So I think it depends very much on the wound and quality of adhesions during surgery. Dr El-Sayed (Khartoum, Sudan): Who was performing the thoracotomies, the standard thoracotomies? From your slide they were taking 2.5 h as opposed to 2 h in VATS. So were the standard thoracotomies being performed by junior trainees, for example? Dr Weber: I think Professor Weder should answer this question. Dr W. Weder: As we already pointed out, we cannot compare the VATS group with the open group, because in the open group we selected all emergency cases or cases with severe adhesions, for example patients with severely destructed lobes from tuberculosis. So you cannot compare these two groups with each other because the indications were slightly different. On the other hand, all VATS lobectomies were done by the senior author and open cases by trainees as well.
Thoracoscopic Pneumonectomy. 10 th Annual Masters in Minimally Invasive Thoracic Surgery
 Thoracoscopic Pneumonectomy 10 th Annual Masters in Minimally Invasive Thoracic Surgery September 22-23, 2017 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery, Duke University
Thoracoscopic Pneumonectomy 10 th Annual Masters in Minimally Invasive Thoracic Surgery September 22-23, 2017 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery, Duke University
Transition from two-three port to uniportal approach in videoassisted thoracoscopic surgery lobectomy: a multicentre comparative study
 Original Article Page 1 of 6 Transition from two-three port to uniportal approach in videoassisted thoracoscopic surgery : a multicentre comparative study Tanel Laisaar 1, Ákos Kocsis 2, Aleksandras Bagajevas
Original Article Page 1 of 6 Transition from two-three port to uniportal approach in videoassisted thoracoscopic surgery : a multicentre comparative study Tanel Laisaar 1, Ákos Kocsis 2, Aleksandras Bagajevas
Technique of uniportal VATS major pulmonary resections
 Surgical Technique Technique of uniportal VATS major pulmonary resections Eva Fieira Costa 1, María Delgado Roel 1, Marina Paradela de la Morena 2, Diego Gonzalez-Rivas 1, Ricardo Fernandez-Prado 1, Mercedes
Surgical Technique Technique of uniportal VATS major pulmonary resections Eva Fieira Costa 1, María Delgado Roel 1, Marina Paradela de la Morena 2, Diego Gonzalez-Rivas 1, Ricardo Fernandez-Prado 1, Mercedes
Is the learning curve for video-assisted thoracoscopic lobectomy affected by prior experience in open lobectomy?
 Interactive CardioVascular and Thoracic Surgery 21 (2015) 108 113 doi:10.1093/icvts/ivv090 Advance Access publication 15 April 2015 BEST EVIDENCE TOPIC THORACIC Cite this article as: Okyere S, Attia R,
Interactive CardioVascular and Thoracic Surgery 21 (2015) 108 113 doi:10.1093/icvts/ivv090 Advance Access publication 15 April 2015 BEST EVIDENCE TOPIC THORACIC Cite this article as: Okyere S, Attia R,
Teaching uniportal video-assisted thoracic surgery in Rome
 Teaching Uniportal VATS in Rome Teaching uniportal video-assisted thoracic surgery in Rome Elisa Meacci, Dania Nachira, Maria Teresa Congedo, Stefano Margaritora Department of Thoracic Surgery, A.Gemelli
Teaching Uniportal VATS in Rome Teaching uniportal video-assisted thoracic surgery in Rome Elisa Meacci, Dania Nachira, Maria Teresa Congedo, Stefano Margaritora Department of Thoracic Surgery, A.Gemelli
Management of complications by uniportal video-assisted thoracoscopic surgery
 Surgical Technique Management of complications by uniportal video-assisted thoracoscopic surgery Ricardo Fernández Prado 1,2, Eva Fieira Costa 1, María Delgado Roel 1, Lucía Méndez Fernández 1, Marina
Surgical Technique Management of complications by uniportal video-assisted thoracoscopic surgery Ricardo Fernández Prado 1,2, Eva Fieira Costa 1, María Delgado Roel 1, Lucía Méndez Fernández 1, Marina
LOBECTOMY. Solutions for minimally invasive thoracic surgery
 LOBECTOMY Solutions for minimally invasive thoracic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Dual Console Dual console capability allows an additional surgeon
LOBECTOMY Solutions for minimally invasive thoracic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Dual Console Dual console capability allows an additional surgeon
European questionnaire on the clinical use of video-assisted thoracoscopic surgery
 https://helda.helsinki.fi European questionnaire on the clinical use of video-assisted thoracoscopic surgery Cao, Christopher 2018-09 Cao, C, Frick, A E, Ilonen, I, McElnay, P, Guerrero, F, Tian, D H,
https://helda.helsinki.fi European questionnaire on the clinical use of video-assisted thoracoscopic surgery Cao, Christopher 2018-09 Cao, C, Frick, A E, Ilonen, I, McElnay, P, Guerrero, F, Tian, D H,
Technological aids in uniportal video-assisted thoracoscopic surgery
 Review Article on Thoracic Surgery Technological aids in uniportal video-assisted thoracoscopic surgery Sonia Raquelline Roque Cañas 1,2, Alonso José Oviedo Argueta 1,2, Ching Feng Wu 2, Diego Gonzalez-Rivas
Review Article on Thoracic Surgery Technological aids in uniportal video-assisted thoracoscopic surgery Sonia Raquelline Roque Cañas 1,2, Alonso José Oviedo Argueta 1,2, Ching Feng Wu 2, Diego Gonzalez-Rivas
Interventional radiology suite or hybrid operating room: Which is the best for lung nodule localization?
 Accepted Manuscript Interventional radiology suite or hybrid operating room: Which is the best for lung nodule localization? Robert B. Cameron PII: S0022-5223(18)31813-0 DOI: 10.1016/j.jtcvs.2018.06.063
Accepted Manuscript Interventional radiology suite or hybrid operating room: Which is the best for lung nodule localization? Robert B. Cameron PII: S0022-5223(18)31813-0 DOI: 10.1016/j.jtcvs.2018.06.063
New stapling devices in robotic surgery
 rief Report on Thoracic Surgery New stapling devices in robotic surgery Domenico Galetta 1, Monica Casiraghi 1, lessandro Pardolesi 1, lessandro orri 1, Lorenzo Spaggiari 1,2 1 Division of Thoracic Surgery,
rief Report on Thoracic Surgery New stapling devices in robotic surgery Domenico Galetta 1, Monica Casiraghi 1, lessandro Pardolesi 1, lessandro orri 1, Lorenzo Spaggiari 1,2 1 Division of Thoracic Surgery,
During pulmonary resection surgeons occasionally. Use of Three-Dimensional Computed Tomographic Angiography of Pulmonary Vessels for Lung Resections
 Use of Three-Dimensional Computed Tomographic Angiography of Pulmonary Vessels for Lung Resections Shun-ichi Watanabe, MD, Kazunori Arai, MD, Toshio Watanabe, MD, Wataru Koda, MD, and Hiroshi Urayama,
Use of Three-Dimensional Computed Tomographic Angiography of Pulmonary Vessels for Lung Resections Shun-ichi Watanabe, MD, Kazunori Arai, MD, Toshio Watanabe, MD, Wataru Koda, MD, and Hiroshi Urayama,
Prevention & Management of Intra-op Challenges. Shanda H. Blackmon, M.D., M.P.H., FACS Associate Professor, Thoracic Surgery, Mayo Clinic
 VATS Lobectomy Prevention & Management of Intra-op Challenges Shanda H. Blackmon, M.D., M.P.H., FACS Associate Professor, Thoracic Surgery, Mayo Clinic Duke Masters of Minimally Invasive Thoracic Surgery,
VATS Lobectomy Prevention & Management of Intra-op Challenges Shanda H. Blackmon, M.D., M.P.H., FACS Associate Professor, Thoracic Surgery, Mayo Clinic Duke Masters of Minimally Invasive Thoracic Surgery,
Multiportal video-assisted thoracic surgery, uniportal videoassisted thoracic surgery and minimally invasive open chest surgery selection criteria
 Review Article on Thoracic Surgery Multiportal video-assisted thoracic surgery, uniportal videoassisted thoracic surgery and minimally invasive open chest surgery selection criteria William Guido Guerrero
Review Article on Thoracic Surgery Multiportal video-assisted thoracic surgery, uniportal videoassisted thoracic surgery and minimally invasive open chest surgery selection criteria William Guido Guerrero
Robotic surgery, video-assisted thoracic surgery, and open surgery for early stage lung cancer: comparison of costs and outcomes at a single institute
 Original Article Robotic surgery, video-assisted thoracic surgery, and open surgery for early stage lung cancer: comparison of costs and outcomes at a single institute Pierluigi Novellis 1, Edoardo Bottoni
Original Article Robotic surgery, video-assisted thoracic surgery, and open surgery for early stage lung cancer: comparison of costs and outcomes at a single institute Pierluigi Novellis 1, Edoardo Bottoni
Cost analysis of VATS approaches
 Review Article Page 1 of 6 Cost analysis of VATS approaches Alessandro Brunelli Department Thoracic Surgery, St. James s University Hospital, Leeds, UK Correspondence to: Dr. Alessandro Brunelli. Department
Review Article Page 1 of 6 Cost analysis of VATS approaches Alessandro Brunelli Department Thoracic Surgery, St. James s University Hospital, Leeds, UK Correspondence to: Dr. Alessandro Brunelli. Department
Video-assisted thoracoscopic surgery lobectomy using the caudal approach : results and evolution
 Original Article on Thoracic Surgery Video-assisted thoracoscopic surgery lobectomy using the caudal approach : results and evolution Giampiero Dolci, Alessio Campisi, Domenica Giunta, Stefano Congiu,
Original Article on Thoracic Surgery Video-assisted thoracoscopic surgery lobectomy using the caudal approach : results and evolution Giampiero Dolci, Alessio Campisi, Domenica Giunta, Stefano Congiu,
Simple covering technique in thoracoscopic bullectomy for spontaneous pneumothorax
 Surgical Technique Simple covering technique in thoracoscopic bullectomy for spontaneous pneumothorax Manabu Yasuda 1, Ryoichi Nakanishi 2, Masataka Mori 1, Syuhei Ashikari 1, Tsunehiro Oyama 1, Takeshi
Surgical Technique Simple covering technique in thoracoscopic bullectomy for spontaneous pneumothorax Manabu Yasuda 1, Ryoichi Nakanishi 2, Masataka Mori 1, Syuhei Ashikari 1, Tsunehiro Oyama 1, Takeshi
Uniportal video-assisted thoracic surgery for pneumothorax and blebs/bullae
 Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for pneumothorax and blebs/bullae Luca Bertolaccini 1, Alessandro Pardolesi 2, Jury Brandolini 2, Piergiorgio Solli 3 1 Department
Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for pneumothorax and blebs/bullae Luca Bertolaccini 1, Alessandro Pardolesi 2, Jury Brandolini 2, Piergiorgio Solli 3 1 Department
Troubleshooting Video-Assisted Thoracic Surgery Lobectomy
 Troubleshooting Video-Assisted Thoracic Surgery Lobectomy Todd L. Demmy, MD, Ted A. James, MD, Scott J. Swanson, MD, Robert J. McKenna, Jr, MD, and Thomas A. D Amico, MD Departments of Thoracic Surgery
Troubleshooting Video-Assisted Thoracic Surgery Lobectomy Todd L. Demmy, MD, Ted A. James, MD, Scott J. Swanson, MD, Robert J. McKenna, Jr, MD, and Thomas A. D Amico, MD Departments of Thoracic Surgery
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Cameron D. Wright, MD PII: S0022-5223(18)31749-5 DOI: 10.1016/j.jtcvs.2018.06.017 Reference: YMTC 13140 To appear in: The Journal of Thoracic and Cardiovascular Surgery Received Date:
Accepted Manuscript Cameron D. Wright, MD PII: S0022-5223(18)31749-5 DOI: 10.1016/j.jtcvs.2018.06.017 Reference: YMTC 13140 To appear in: The Journal of Thoracic and Cardiovascular Surgery Received Date:
Uniportal video-assisted thoracic surgery: the Middle East experience
 Original Article dedicated to the 3rd International VATS Course in Berlin Uniportal video-assisted thoracic surgery: the Middle East experience Firas Abu Akar 1, Diego Gonzalez-Rivas 2, Mahmoud Ismail
Original Article dedicated to the 3rd International VATS Course in Berlin Uniportal video-assisted thoracic surgery: the Middle East experience Firas Abu Akar 1, Diego Gonzalez-Rivas 2, Mahmoud Ismail
Why should we prefer the single port access thoracic surgery?
 Commentary on Thoracic Surgery Why should we prefer the single port access thoracic surgery? Luca Bertolaccini, Alberto Terzi, Andrea Viti Thoracic Surgery Unit, Sacro Cuore Don Calabria Research Hospital
Commentary on Thoracic Surgery Why should we prefer the single port access thoracic surgery? Luca Bertolaccini, Alberto Terzi, Andrea Viti Thoracic Surgery Unit, Sacro Cuore Don Calabria Research Hospital
VATS Lobectomy. Prevention & Management of Intra-op Events. Shanda H. Blackmon, M.D., M.P.H., FACS
 VATS Lobectomy Prevention & Management of Intra-op Events Shanda H. Blackmon, M.D., M.P.H., FACS Duke Masters of Minimally Invasive Thoracic Surgery, 2015 2014 MFMER slide-1 Disclosure I have no Disclosures
VATS Lobectomy Prevention & Management of Intra-op Events Shanda H. Blackmon, M.D., M.P.H., FACS Duke Masters of Minimally Invasive Thoracic Surgery, 2015 2014 MFMER slide-1 Disclosure I have no Disclosures
Update on three-dimensional image reconstruction for preoperative simulation in thoracic surgery
 Original Article Update on three-dimensional image reconstruction for preoperative simulation in thoracic surgery Toyofumi F. Chen-Yoshikawa, Hiroshi Date Department of Thoracic Surgery, Kyoto University,
Original Article Update on three-dimensional image reconstruction for preoperative simulation in thoracic surgery Toyofumi F. Chen-Yoshikawa, Hiroshi Date Department of Thoracic Surgery, Kyoto University,
Samer Kanaan, MD Pacific Thoracic Surgery
 Samer Kanaan, MD Pacific Thoracic Surgery PN 1000710-US Rev D C 8/14 6/15 Table of Contents Vision Presentation Clinical Data da Vinci Xi PN 1000710-US Rev D 1/15 6/15 Adoption of VATS Lobectomy * in the
Samer Kanaan, MD Pacific Thoracic Surgery PN 1000710-US Rev D C 8/14 6/15 Table of Contents Vision Presentation Clinical Data da Vinci Xi PN 1000710-US Rev D 1/15 6/15 Adoption of VATS Lobectomy * in the
Innovative Technology
 Innovative Technology and instrumentation Shanda H. Blackmon, M.D., M.P.H., FACS Duke Masters of Minimally Invasive Thoracic Surgery 2016 2014 MFMER slide-1 Disclosure I have no Disclosures 2014 MFMER
Innovative Technology and instrumentation Shanda H. Blackmon, M.D., M.P.H., FACS Duke Masters of Minimally Invasive Thoracic Surgery 2016 2014 MFMER slide-1 Disclosure I have no Disclosures 2014 MFMER
CT Guided Electromagnetic Navigational Bronchoscopy
 CT Guided Electromagnetic Navigational Bronchoscopy Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Chief Thoracic Surgery, Chief Medical Officer
CT Guided Electromagnetic Navigational Bronchoscopy Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Chief Thoracic Surgery, Chief Medical Officer
PROGRAMME. Claudio LOTTENBERG President United Health Group Brazil. Dominique GOSSOT Institut Mutualiste Montsouris Paris, France
 PROGRAMME Claudio LOTTENBERG President United Health Group Brazil Jacques MARESCAUX President, IRCAD University of Strasbourg, France Armando MELANI Americas Medical City Rio de Janeiro, Brazil Dominique
PROGRAMME Claudio LOTTENBERG President United Health Group Brazil Jacques MARESCAUX President, IRCAD University of Strasbourg, France Armando MELANI Americas Medical City Rio de Janeiro, Brazil Dominique
Robotic thoracic surgery in inflammatory and infective diseases
 Perspective Robotic thoracic surgery in inflammatory and infective diseases Ali Zamir Khan 1, Sangeeta Khanna 2, Narendra Agarwal 1, Kamran Ali 1 1 Department of Minimally Invasive Thoracic Surgery, 2
Perspective Robotic thoracic surgery in inflammatory and infective diseases Ali Zamir Khan 1, Sangeeta Khanna 2, Narendra Agarwal 1, Kamran Ali 1 1 Department of Minimally Invasive Thoracic Surgery, 2
Computed tomography guided microcoil localization for pulmonary small nodules and ground-glass opacity prior to thoracoscopic resection
 Original Article Computed tomography guided microcoil localization for pulmonary small nodules and ground-glass opacity prior to thoracoscopic resection Xizhao Sui*, Hui Zhao*, Feng Yang, Ji-Lun Li, Jun
Original Article Computed tomography guided microcoil localization for pulmonary small nodules and ground-glass opacity prior to thoracoscopic resection Xizhao Sui*, Hui Zhao*, Feng Yang, Ji-Lun Li, Jun
Image-guided video-assisted thoracoscopic surgery for small ground glass opacities: a case series
 Original Article on Thoracic Surgery Image-guided video-assisted thoracoscopic surgery for small ground glass opacities: a case series Hsin-Yueh Fang, Yin-Kai Chao, Ming-Ju Hsieh, Chih-Tsung Wen, Pei-Hsuan
Original Article on Thoracic Surgery Image-guided video-assisted thoracoscopic surgery for small ground glass opacities: a case series Hsin-Yueh Fang, Yin-Kai Chao, Ming-Ju Hsieh, Chih-Tsung Wen, Pei-Hsuan
Intra-Operative Thoracoscopic Assisting Techniques
 Intra-Operative Thoracoscopic Assisting Techniques S.Scott Balderson PA-C Clinical Instructor, Duke Surgical Physician Assistant Residency Division of Thoracic Surgery Thoracic Oncology Program Duke Comprehensive
Intra-Operative Thoracoscopic Assisting Techniques S.Scott Balderson PA-C Clinical Instructor, Duke Surgical Physician Assistant Residency Division of Thoracic Surgery Thoracic Oncology Program Duke Comprehensive
12VIDEO-ASSISTED THORACOSCOPIC PROCEDURES
 2016 Strasbourg University /FRANCE 12VIDEO-ASSISTED AND THORACOSCOPIC PROCEDURES Course directors [ D. Gossot F ] [ W. Walker UK ] March 3-5 Advanced Course 1 12 VIDEO-ASSISTED AND THORACOSCOPIC PROCEDURES
2016 Strasbourg University /FRANCE 12VIDEO-ASSISTED AND THORACOSCOPIC PROCEDURES Course directors [ D. Gossot F ] [ W. Walker UK ] March 3-5 Advanced Course 1 12 VIDEO-ASSISTED AND THORACOSCOPIC PROCEDURES
Computed Tomography-Guided Bronchoscopy
 Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 229-232 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 229-232 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
Disclosures. Role of the Pulmonologist in a Multidisciplinary Thoracic Program. Introduction. Access. None. Access
 Role of the Pulmonologist in a Multidisciplinary Thoracic Program Disclosures None Ken Y. Yoneda, M.D. Professor of Medicine Division of Pulmonary and Critical Care University of California, Davis VA Northern
Role of the Pulmonologist in a Multidisciplinary Thoracic Program Disclosures None Ken Y. Yoneda, M.D. Professor of Medicine Division of Pulmonary and Critical Care University of California, Davis VA Northern
The Journal of THORACIC AND CARDIOVASCULAR SURGERY GENERAL THORACIC SURGERY. Volume 109 Number4 April 1995
 Volume 109 Number4 April 1995 The Journal of THORACIC AND CARDIOVASCULAR SURGERY GENERAL THORACIC SURGERY SIMULTANEOUSLY STAPLED LOBECTOMY: A SAFE TECHNIQUE FOR VIDEO- ASSISTED THORACIC SURGERY Currently,
Volume 109 Number4 April 1995 The Journal of THORACIC AND CARDIOVASCULAR SURGERY GENERAL THORACIC SURGERY SIMULTANEOUSLY STAPLED LOBECTOMY: A SAFE TECHNIQUE FOR VIDEO- ASSISTED THORACIC SURGERY Currently,
Necrotizing pneumonia is characterized by a consolidated
 Intrathoracic Vacuum-Assisted Management of Persistent and Infected Pleural Spaces Giorgio M. Aru, MD, Nicholas B. Jew, Curtis G. Tribble, MD, and Walter H. Merrill, MD Division of Cardiothoracic Surgery,
Intrathoracic Vacuum-Assisted Management of Persistent and Infected Pleural Spaces Giorgio M. Aru, MD, Nicholas B. Jew, Curtis G. Tribble, MD, and Walter H. Merrill, MD Division of Cardiothoracic Surgery,
Current Management of Empyema
 Current Management of Empyema George W. Holcomb, III, M.D., MBA Surgeon-in-Chief/Senior Vice-President Children s Mercy Hospital Kansas City, Missouri Thoracoscopic Operations Children s Mercy Experience
Current Management of Empyema George W. Holcomb, III, M.D., MBA Surgeon-in-Chief/Senior Vice-President Children s Mercy Hospital Kansas City, Missouri Thoracoscopic Operations Children s Mercy Experience
Pulmonary Nodule Localization - Best Method. Jay M. Lee, M.D. Chief and Associate Professor Division of Thoracic Surgery, UCLA
 Pulmonary Nodule Localization - Best Method Jay M. Lee, M.D. Chief and Associate Professor Division of Thoracic Surgery, UCLA 1 Localization of pulmonary nodules Lung cancer screening has lead to frequent
Pulmonary Nodule Localization - Best Method Jay M. Lee, M.D. Chief and Associate Professor Division of Thoracic Surgery, UCLA 1 Localization of pulmonary nodules Lung cancer screening has lead to frequent
What makes the technology unique?
 The VirtuoSaph Endoscopic Vein Harvesting System is designed to elevate standards for patient safety, conduit quality, and ergonomics. When developing the VirtuoSaph System, Terumo spent significant resources
The VirtuoSaph Endoscopic Vein Harvesting System is designed to elevate standards for patient safety, conduit quality, and ergonomics. When developing the VirtuoSaph System, Terumo spent significant resources
Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/endobronchial-ultrasoundguided-transbronchial-needle-aspiration/4014/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/endobronchial-ultrasoundguided-transbronchial-needle-aspiration/4014/
Cite this article as:
 doi: 10.21037/acs.2018. 11.10 Cite this article as: Stamenkovic S, Slight RD. Resource implications of robotic thoracic surgery: what are the wider issues?. doi: 10.21037/acs.2018.11.10 This is a PDF file
doi: 10.21037/acs.2018. 11.10 Cite this article as: Stamenkovic S, Slight RD. Resource implications of robotic thoracic surgery: what are the wider issues?. doi: 10.21037/acs.2018.11.10 This is a PDF file
During the past 20 years, the trend has been to make
 Early Experience With Robotic Lung Resection Results in Similar Operative Outcomes and Morbidity When Compared With Matched Video- Assisted Thoracoscopic Surgery Cases Brian E. Louie, MD, Alexander S.
Early Experience With Robotic Lung Resection Results in Similar Operative Outcomes and Morbidity When Compared With Matched Video- Assisted Thoracoscopic Surgery Cases Brian E. Louie, MD, Alexander S.
EDITO. First International Conference - Sublobar resections for lung cancer Programme. Dear Colleagues,
 EDITO Dear Colleagues, The treatment of early-stage lung carcinomas is rapidly evolving. During the last years, we have progressively moved from pulmonary lobectomies considered until recently as the gold
EDITO Dear Colleagues, The treatment of early-stage lung carcinomas is rapidly evolving. During the last years, we have progressively moved from pulmonary lobectomies considered until recently as the gold
Get a Closer Look. Continuing Support
 Get a Closer Look Terumo s Centers of Excellence bring together clinicians interested in evaluating Terumo s endoscopic vein harvesting products and experienced clinicians already successfully using them.
Get a Closer Look Terumo s Centers of Excellence bring together clinicians interested in evaluating Terumo s endoscopic vein harvesting products and experienced clinicians already successfully using them.
TOP MISSED CONCEPTS: CPC
 1 TOP MISSED CONCEPTS: CPC 2018 AMA Disclaimer CPT copyright 2017 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are
1 TOP MISSED CONCEPTS: CPC 2018 AMA Disclaimer CPT copyright 2017 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are
UNIQUE CHALLENGES DEMAND MEANINGFUL INNOVATIONS. Specialty stapling and advanced energy solutions for thoracic surgeons
 UNIQUE CHALLENGES DEMAND MEANINGFUL INNOVATIONS. Specialty stapling and advanced energy solutions for thoracic surgeons OUR JOB IS TO MAKE YOURS EASIER. TO HELP YOU SAVE MORE LIVES. Having the right tools
UNIQUE CHALLENGES DEMAND MEANINGFUL INNOVATIONS. Specialty stapling and advanced energy solutions for thoracic surgeons OUR JOB IS TO MAKE YOURS EASIER. TO HELP YOU SAVE MORE LIVES. Having the right tools
Sample page. Anesthesia Services An essential coding, billing and reimbursement resource for anesthesiology and pain management CODING & PAYMENT GUIDE
 CODING & PAYMENT GUIDE 2019 Anesthesia Services An essential coding, billing and reimbursement resource for anesthesiology and pain management Power up your coding optum360coding.com Contents Getting Started
CODING & PAYMENT GUIDE 2019 Anesthesia Services An essential coding, billing and reimbursement resource for anesthesiology and pain management Power up your coding optum360coding.com Contents Getting Started
Superficial Endobronchial Lung Cancer: Radiologic-Pathologic Correlation
 Superficial Endobronchial Lung Cancer: Radiologic-Pathologic Correlation Nae Jin Han, MD 1 Koun-Sik Song, MD 1 Kyung Hee Lee, MD 1 Joon Beom Seo, MD 1 Jin Seong Lee, MD 1 Tae-Hwan Lim, MD 1 Gil Hyun Kang,
Superficial Endobronchial Lung Cancer: Radiologic-Pathologic Correlation Nae Jin Han, MD 1 Koun-Sik Song, MD 1 Kyung Hee Lee, MD 1 Joon Beom Seo, MD 1 Jin Seong Lee, MD 1 Tae-Hwan Lim, MD 1 Gil Hyun Kang,
Use of an electrothermal bipolar tissue sealing system in lung surgery
 European Journal of Cardio-thoracic Surgery 29 (2006) 226 230 www.elsevier.com/locate/ejcts Use of an electrothermal bipolar tissue sealing system in lung surgery Mario Santini a, *, Giovanni Vicidomini
European Journal of Cardio-thoracic Surgery 29 (2006) 226 230 www.elsevier.com/locate/ejcts Use of an electrothermal bipolar tissue sealing system in lung surgery Mario Santini a, *, Giovanni Vicidomini
Operative Considerations for the Thoracoscopic Surgery Team
 Operative Considerations for the Thoracoscopic Surgery Team S.Scott Balderson PA-C Clinical Instructor, Duke Surgical Physician Assistant Residency Division of Thoracic Surgery Thoracic Oncology Program
Operative Considerations for the Thoracoscopic Surgery Team S.Scott Balderson PA-C Clinical Instructor, Duke Surgical Physician Assistant Residency Division of Thoracic Surgery Thoracic Oncology Program
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Surgical Advantages of Selective Unilateral Ventilation
 Surgical Advantages of Selective Unilateral Ventilation Richard E. Wood, M.D., Donovan Campbell, M.D., Maruf A. Razzuk, M.D., Donald L. Paulson, M.D., and Harold C. Urschel, Jr., M.D. ABSTRACT Two hundred
Surgical Advantages of Selective Unilateral Ventilation Richard E. Wood, M.D., Donovan Campbell, M.D., Maruf A. Razzuk, M.D., Donald L. Paulson, M.D., and Harold C. Urschel, Jr., M.D. ABSTRACT Two hundred
Evolving from conventional video-assisted thoracoscopic lobectomy to uniportal: the story behind the evolution
 Perspective Evolving from conventional video-assisted thoracoscopic lobectomy to uniportal: the story behind the evolution Diego Gonzalez-Rivas 1,2, Eva Fieira 1, Maria Delgado 1, Lucía Mendez 1, Ricardo
Perspective Evolving from conventional video-assisted thoracoscopic lobectomy to uniportal: the story behind the evolution Diego Gonzalez-Rivas 1,2, Eva Fieira 1, Maria Delgado 1, Lucía Mendez 1, Ricardo
Robotic lobectomy for lung cancer: evolution in technique and technology
 European Journal of Cardio-Thoracic Surgery 46 (2014) 626 631 doi:10.1093/ejcts/ezu079 Advance Access publication 9 March 2014 ORIGINAL ARTICLE Robotic lobectomy for lung cancer: evolution in technique
European Journal of Cardio-Thoracic Surgery 46 (2014) 626 631 doi:10.1093/ejcts/ezu079 Advance Access publication 9 March 2014 ORIGINAL ARTICLE Robotic lobectomy for lung cancer: evolution in technique
Interlobar fixation using TachoSil : a novel technique
 Original Article Interlobar fixation using TachoSil : a novel technique Alfonso Fiorelli, Roberto Scaramuzzi, Saveria Costanzo, Antonio Volpicelli, Mario Santini Thoracic Surgery Unit, Second University
Original Article Interlobar fixation using TachoSil : a novel technique Alfonso Fiorelli, Roberto Scaramuzzi, Saveria Costanzo, Antonio Volpicelli, Mario Santini Thoracic Surgery Unit, Second University
Gelatin-Resorcinol Formaldehyde-Glutaraldehyde Glue for Sealing Pulmonary Air Leaks During Thoracoscopic Operation
 Gelatin-Resorcinol Formaldehyde-Glutaraldehyde Glue for Sealing Pulmonary Air Leaks During Thoracoscopic Operation Hiroaki Nomori, MD, Hirotoshi Horio, MD, Shojiroh Morinaga, MD, and Keiichi Suemasu, MD
Gelatin-Resorcinol Formaldehyde-Glutaraldehyde Glue for Sealing Pulmonary Air Leaks During Thoracoscopic Operation Hiroaki Nomori, MD, Hirotoshi Horio, MD, Shojiroh Morinaga, MD, and Keiichi Suemasu, MD
ADHESIVE SEALANT BIOMATERIALS
 ADHESIVE SEALANT BIOMATERIALS Technical Bulletin David Mandley PhD Tissuemed Ltd. Performance of a Novel Adhesive Film (TissuePatch TM 3) compared with commercially available Products in the resolution
ADHESIVE SEALANT BIOMATERIALS Technical Bulletin David Mandley PhD Tissuemed Ltd. Performance of a Novel Adhesive Film (TissuePatch TM 3) compared with commercially available Products in the resolution
Uniportal VATS Course
 FACULTY Thomas Damico Chief, Thoracic surgery department. Duke University medical Center. US Gaetano Rocco Chief.Thoracic surgery department. National Cancer Institute. Italy Calvin NG Consultant surgeon.
FACULTY Thomas Damico Chief, Thoracic surgery department. Duke University medical Center. US Gaetano Rocco Chief.Thoracic surgery department. National Cancer Institute. Italy Calvin NG Consultant surgeon.
Accepted Manuscript. Tag, You re It! Finding and Treating Early Lung Cancers in a Single Setting. Ngoc-Quynh Chu, MD, Yolonda L.
 Accepted Manuscript Tag, You re It! Finding and Treating Early Lung Cancers in a Single Setting Ngoc-Quynh Chu, MD, Yolonda L. Colson, MD, PhD PII: S0022-5223(18)33512-8 DOI: https://doi.org/10.1016/j.jtcvs.2018.12.069
Accepted Manuscript Tag, You re It! Finding and Treating Early Lung Cancers in a Single Setting Ngoc-Quynh Chu, MD, Yolonda L. Colson, MD, PhD PII: S0022-5223(18)33512-8 DOI: https://doi.org/10.1016/j.jtcvs.2018.12.069
A New Technological Approach to Nonanatomical Pulmonary Resection: Saline Enhanced Thermal Sealing
 A New Technological Approach to Nonanatomical Pulmonary Resection: Saline Enhanced Thermal Sealing Anthony P. C. Yim, MD, Erino A. Rendina, MD, Stephen R. Hazelrigg, MD, Louis T. C. Chow, MD, Tai-Wai Lee,
A New Technological Approach to Nonanatomical Pulmonary Resection: Saline Enhanced Thermal Sealing Anthony P. C. Yim, MD, Erino A. Rendina, MD, Stephen R. Hazelrigg, MD, Louis T. C. Chow, MD, Tai-Wai Lee,
Surgical Management of Empyema. Mr Nadeem Haider Paediatric Surgeon Christchurch Hospital
 Surgical Management of Empyema Mr Nadeem Haider Paediatric Surgeon Christchurch Hospital History A person with empyemata shall die on 14 th day unless something favourable supervene" would rather die at
Surgical Management of Empyema Mr Nadeem Haider Paediatric Surgeon Christchurch Hospital History A person with empyemata shall die on 14 th day unless something favourable supervene" would rather die at
Multidrug-resistant tuberculosis (MDR-TB) refers to
 Pulmonary Resection in the Treatment of Multidrug-Resistant Tuberculosis: A Retrospective Study of 56 Cases Haifeng Wang, MM, Hongsheng Lin, MM, and Gening Jiang, MD Department of Thoracic Surgery, Shanghai
Pulmonary Resection in the Treatment of Multidrug-Resistant Tuberculosis: A Retrospective Study of 56 Cases Haifeng Wang, MM, Hongsheng Lin, MM, and Gening Jiang, MD Department of Thoracic Surgery, Shanghai
Nonintubated uniportal thoracoscopic surgery for resection of lung lesions
 Original Article Nonintubated uniportal thoracoscopic surgery for resection of lung lesions Wan-Ting Hung 1, Hsao-Hsun Hsu 1, Ming-Hui Hung 2, Pei-Yin Hsieh 3, Ya-Jung Cheng 2, Jin-Shing Chen 1,4 1 Division
Original Article Nonintubated uniportal thoracoscopic surgery for resection of lung lesions Wan-Ting Hung 1, Hsao-Hsun Hsu 1, Ming-Hui Hung 2, Pei-Yin Hsieh 3, Ya-Jung Cheng 2, Jin-Shing Chen 1,4 1 Division
Single-Port Thoracic Surgery: A New Direction
 Korean J Thorac Cardiovasc Surg 2014;47:327-332 Review ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) http://dx.doi.org/10.5090/kjtcs.2014.47.4.327 Single-Port Thoracic Surgery: A New Direction Calvin
Korean J Thorac Cardiovasc Surg 2014;47:327-332 Review ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) http://dx.doi.org/10.5090/kjtcs.2014.47.4.327 Single-Port Thoracic Surgery: A New Direction Calvin
Cost-Benefit Performance of Robotic Surgery Compared with Video-Assisted Thoracoscopic Surgery under the Japanese National Health Insurance System
 Ann Thorac Cardiovasc Surg 2015; 21: 95 101 Online May 16, 2014 doi: 10.5761/atcs.oa.14-00076 Original Article Cost-Benefit Performance of Surgery Compared with Video-Assisted Thoracoscopic Surgery under
Ann Thorac Cardiovasc Surg 2015; 21: 95 101 Online May 16, 2014 doi: 10.5761/atcs.oa.14-00076 Original Article Cost-Benefit Performance of Surgery Compared with Video-Assisted Thoracoscopic Surgery under
Specimen Retrieval Systems
 Specimen Retrieval Systems All-in-One Introducer Style Specimen Bags Laparoscopic Solutions: Specimen Retrieval Bag The GeniStrong TM Bag is an easy-to-use retrieval system designed to temporarily contain
Specimen Retrieval Systems All-in-One Introducer Style Specimen Bags Laparoscopic Solutions: Specimen Retrieval Bag The GeniStrong TM Bag is an easy-to-use retrieval system designed to temporarily contain
The evolution of minimally invasive thoracic surgery: implications for the practice of uniportal thoracoscopic surgery
 Review Article The evolution of minimally invasive thoracic surgery: implications for the practice of uniportal thoracoscopic surgery Alan D. L. Sihoe Division of Cardiothoracic Surgery, Department of
Review Article The evolution of minimally invasive thoracic surgery: implications for the practice of uniportal thoracoscopic surgery Alan D. L. Sihoe Division of Cardiothoracic Surgery, Department of
Shun-Mao Yang 1,2, Wei-Chun Ko 3, Ling-Hsuan Meng 4, Li-Wei Chen 2, Kun-Hsien Lin 3, Yueh-Lun Liu 3, Shao-En Sun 3, Huan-Jang Ko 1.
 Original Article Page 1 of 8 Single-stage hybrid localization: a combination of bronchoscopic lung mapping followed by post-mapping computed tomographic reconstruction and additional transthoracic needle
Original Article Page 1 of 8 Single-stage hybrid localization: a combination of bronchoscopic lung mapping followed by post-mapping computed tomographic reconstruction and additional transthoracic needle
A Retrospective Database Analysis
 CHEST Original Research LUNG CANCER In-hospital Clinical and Economic Consequences of Pulmonary Wedge Resections for Cancer Using Video-Assisted Thoracoscopic Techniques vs Traditional Open Resections
CHEST Original Research LUNG CANCER In-hospital Clinical and Economic Consequences of Pulmonary Wedge Resections for Cancer Using Video-Assisted Thoracoscopic Techniques vs Traditional Open Resections
Asian perspectives in thoracic surgery: clinical innovation in Taiwan
 Review Article Asian perspectives in thoracic surgery: clinical innovation in Taiwan Chao-Yu Liu 1,2, Chen-Sung Lin 2,3, Chia-Chuan Liu 4 1 Division of Thoracic Surgery, Department of Surgery, Far Eastern
Review Article Asian perspectives in thoracic surgery: clinical innovation in Taiwan Chao-Yu Liu 1,2, Chen-Sung Lin 2,3, Chia-Chuan Liu 4 1 Division of Thoracic Surgery, Department of Surgery, Far Eastern
The gold standard for mediastinal lymph node staging is
 Endobronchial Ultrasound Traves D. Crabtree, MD The gold standard for mediastinal lymph node staging is mediastinoscopy. Standard mediastinoscopy or video mediastinoscopy provides access to levels 2R,
Endobronchial Ultrasound Traves D. Crabtree, MD The gold standard for mediastinal lymph node staging is mediastinoscopy. Standard mediastinoscopy or video mediastinoscopy provides access to levels 2R,
Small Nodule Localization. Bernard Park, M.D. Attending Surgeon, Thoracic Service Memorial Sloan Kettering Cancer Center
 Small Nodule Localization Bernard Park, M.D. Attending Surgeon, Thoracic Service Memorial Sloan Kettering Cancer Center Disclosures Intuitive Surgical: honoraria Medtronic: consulting Image guidance in
Small Nodule Localization Bernard Park, M.D. Attending Surgeon, Thoracic Service Memorial Sloan Kettering Cancer Center Disclosures Intuitive Surgical: honoraria Medtronic: consulting Image guidance in
Harvesting a New Standard of Care
 Harvesting a New Standard of Care The handoff. Be confident what you re passing along is of the highest quality. What do you need to deliver the optimal conduit? Is it knowing that you controlled hemostasis?
Harvesting a New Standard of Care The handoff. Be confident what you re passing along is of the highest quality. What do you need to deliver the optimal conduit? Is it knowing that you controlled hemostasis?
Coding and Billing Guide
 To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
Disclosure. Industry-sponsored grants. Consultant. Research Collaboration. Educational and research grants from Olympus Medical Systems Corp.
 Image Guided Surgery Kazuhiro Yasufuku MD, PhD Director, Interventional Thoracic Surgery Program Associate Professor of Surgery, University of Toronto Division of Thoracic Surgery, Toronto General Hospital
Image Guided Surgery Kazuhiro Yasufuku MD, PhD Director, Interventional Thoracic Surgery Program Associate Professor of Surgery, University of Toronto Division of Thoracic Surgery, Toronto General Hospital
In the last 15 years, video-assisted thoracic surgery (VATS)
 Single-Port Video-Assisted Thoracic Surgery (Uniportal) in the Routine General Thoracic Surgical Practice Gaetano Rocco, MD, FRCS(Ed), FETCS In the last 15 years, video-assisted thoracic surgery (VATS)
Single-Port Video-Assisted Thoracic Surgery (Uniportal) in the Routine General Thoracic Surgical Practice Gaetano Rocco, MD, FRCS(Ed), FETCS In the last 15 years, video-assisted thoracic surgery (VATS)
Coding and Billing Guide
 To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
Lung cancer may present either as a parenchymal. Utility of Transbronchial Needle Aspiration in the Diagnosis of Endobronchial Lesions*
 Utility of Transbronchial Needle Aspiration in the Diagnosis of Endobronchial Lesions* Asok Dasgupta, MBBS, Prasoon Jain, MBBS, MD; Omar A Minai, MBBS; Sunder Sandur, MD; Yvonne Meli, RN; Alejandro C.
Utility of Transbronchial Needle Aspiration in the Diagnosis of Endobronchial Lesions* Asok Dasgupta, MBBS, Prasoon Jain, MBBS, MD; Omar A Minai, MBBS; Sunder Sandur, MD; Yvonne Meli, RN; Alejandro C.
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Laparoscopic vs open nephrectomy in 210 consecutive patients: outcomes, cost, and changes in practice patterns Kercher K W, Heniford B T, Matthews B D, Smith T I, Lincourt A E, Hayes D H, Eskind L B, Irby
Laparoscopic vs open nephrectomy in 210 consecutive patients: outcomes, cost, and changes in practice patterns Kercher K W, Heniford B T, Matthews B D, Smith T I, Lincourt A E, Hayes D H, Eskind L B, Irby
Coding and Billing Guide
 To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
Specimen Retrieval Solutions
 Specimen Retrieval Solutions All-in-One Introducer Style Specimen Bags Laparoscopic Solutions: Specimen Retrieval Bag The GeniStrong TM Bag is an easy-to-use retrieval system designed to temporarily contain
Specimen Retrieval Solutions All-in-One Introducer Style Specimen Bags Laparoscopic Solutions: Specimen Retrieval Bag The GeniStrong TM Bag is an easy-to-use retrieval system designed to temporarily contain
Original Article. Introduction
 doi: 10.5761/atcs.oa.17-00094 Original Article Cost-Benefit Performance Simulation of Robot-Assisted Thoracic Surgery As Required for Financiall Viability under the 2016 Revised Reimbursement Paradigm
doi: 10.5761/atcs.oa.17-00094 Original Article Cost-Benefit Performance Simulation of Robot-Assisted Thoracic Surgery As Required for Financiall Viability under the 2016 Revised Reimbursement Paradigm
DA VINCI Xi SINGLE-SITE TECHNOLOGY SOLUTIONS FOR SINGLE-INCISION SURGERY
 DA VINCI Xi SINGLE-SITE SOLUTIONS FOR SINGLE-INCISION SURGERY TECHNOLOGY DA VINCI Xi SINGLE-SITE TECHNOLOGY AT INTUITIVE SURGICAL, WE STRIVE TO MAKE SURGERY MORE EFFECTIVE, LESS INVASIVE, AND EASIER ON
DA VINCI Xi SINGLE-SITE SOLUTIONS FOR SINGLE-INCISION SURGERY TECHNOLOGY DA VINCI Xi SINGLE-SITE TECHNOLOGY AT INTUITIVE SURGICAL, WE STRIVE TO MAKE SURGERY MORE EFFECTIVE, LESS INVASIVE, AND EASIER ON
Recent developments in uniportal VATS in Asia and beyond
 Review Article on Thoracic Surgery Page 1 of 6 Recent developments in uniportal VATS in Asia and beyond Peter S. Y. Yu, Calvin S. H. Ng Division of Cardiothoracic Surgery, Department of Surgery, The Chinese
Review Article on Thoracic Surgery Page 1 of 6 Recent developments in uniportal VATS in Asia and beyond Peter S. Y. Yu, Calvin S. H. Ng Division of Cardiothoracic Surgery, Department of Surgery, The Chinese
Endobronchial Valves. Description
 Section: Surgery Effective Date: July 15, 2015 Subject: Endobronchial Valves Page: 1 of 10 Last Review Status/Date: June 2015 Endobronchial Valves Description Endobronchial valves are synthetic devices
Section: Surgery Effective Date: July 15, 2015 Subject: Endobronchial Valves Page: 1 of 10 Last Review Status/Date: June 2015 Endobronchial Valves Description Endobronchial valves are synthetic devices
Median Sternotomy Closure Utilizing Platelet Concentrate BIOLOGICS
 Median Sternotomy Closure Utilizing Platelet Concentrate BIOLOGICS This brochure is for International use only. It is not for distribution in the United States. The Surgical Procedure: Median Sternotomy
Median Sternotomy Closure Utilizing Platelet Concentrate BIOLOGICS This brochure is for International use only. It is not for distribution in the United States. The Surgical Procedure: Median Sternotomy
Coding and Billing Guide
 To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
To control prolonged air leaks of the lung or significant air leaks likely to become prolonged following lobectomy, segmentectomy and LVRS Coding and Billing Guide This guide is intended to provide coding
Thoracoscopic stapler-based bidirectional segmentectomy for posterior basal segment (S10) and its variants
 Surgical Technique Thoracoscopic stapler-based bidirectional segmentectomy for posterior basal segment (S10) and its variants Masaaki Sato, Tomonori Murayama, Jun Nakajima Department of Thoracic Surgery,
Surgical Technique Thoracoscopic stapler-based bidirectional segmentectomy for posterior basal segment (S10) and its variants Masaaki Sato, Tomonori Murayama, Jun Nakajima Department of Thoracic Surgery,
Intra-Operative Thoracoscopic Assisting Techniques
 Intra-Operative Thoracoscopic Assisting Techniques S.Scott Balderson PA-C Clinical Instructor, Duke Surgical Physician Assistant Residency Division of Thoracic Surgery Thoracic Oncology Program Duke Comprehensive
Intra-Operative Thoracoscopic Assisting Techniques S.Scott Balderson PA-C Clinical Instructor, Duke Surgical Physician Assistant Residency Division of Thoracic Surgery Thoracic Oncology Program Duke Comprehensive
From full thoracotomy to uniportal video-assisted thoracic surgery: lessons learned
 Review Article on Thoracic Surgery From full thoracotomy to uniportal video-assisted thoracic surgery: lessons learned Eliseo Passera 1, Gaetano Rocco 2 1 Department of Thoracic Surgery, Humanitas Gavazzeni
Review Article on Thoracic Surgery From full thoracotomy to uniportal video-assisted thoracic surgery: lessons learned Eliseo Passera 1, Gaetano Rocco 2 1 Department of Thoracic Surgery, Humanitas Gavazzeni
The occurrence of prolonged alveolar air leaks (AAL)
 Randomized Controlled Trial of a Synthetic Sealant for Preventing Alveolar Air Leaks After Lobectomy Henri L. Porte, MD, Thomas Jany, MD, Rias Akkad, MD, Massimo Conti, MD, Patricia A. Gillet, MD, Anne
Randomized Controlled Trial of a Synthetic Sealant for Preventing Alveolar Air Leaks After Lobectomy Henri L. Porte, MD, Thomas Jany, MD, Rias Akkad, MD, Massimo Conti, MD, Patricia A. Gillet, MD, Anne
Pre-operative localization of solitary pulmonary nodules with computed tomography-guided hook wire: report of 181 patients
 Hanauer et al. Journal of Cardiothoracic Surgery (2016) 11:5 DOI 10.1186/s13019-016-0404-4 RESEARCH ARTICLE Pre-operative localization of solitary pulmonary nodules with computed tomography-guided hook
Hanauer et al. Journal of Cardiothoracic Surgery (2016) 11:5 DOI 10.1186/s13019-016-0404-4 RESEARCH ARTICLE Pre-operative localization of solitary pulmonary nodules with computed tomography-guided hook
Bipolar sealing devices in video-assisted thoracic surgery
 Review Article on Thoracic Surgery Bipolar sealing devices in video-assisted thoracic surgery Filippo Longo 1, Pierfilippo Crucitti 1, Fabio Quintarelli 1, Raffaele Rocco 1, Giuseppe Mangiameli 1, Gaetano
Review Article on Thoracic Surgery Bipolar sealing devices in video-assisted thoracic surgery Filippo Longo 1, Pierfilippo Crucitti 1, Fabio Quintarelli 1, Raffaele Rocco 1, Giuseppe Mangiameli 1, Gaetano
ARTEMIS. A telemanipulator for cardiac surgery q
 European Journal of Cardio-thoracic Surgery 16 (Suppl. 2) (1999) S106±S111 www.elsevier.com/locate/ejcts ARTEMIS. A telemanipulator for cardiac surgery q Hermann Rininsland* Karlsruhe Research Centre,
European Journal of Cardio-thoracic Surgery 16 (Suppl. 2) (1999) S106±S111 www.elsevier.com/locate/ejcts ARTEMIS. A telemanipulator for cardiac surgery q Hermann Rininsland* Karlsruhe Research Centre,
Robotics in general thoracic surgery procedures
 Review Article on Thoracic Surgery Robotics in general thoracic surgery procedures M. Jawad Latif, Bernard J. Park Thoracic Surgery Service, Memorial Sloan Kettering Cancer Center, New York, NY, USA Contributions:
Review Article on Thoracic Surgery Robotics in general thoracic surgery procedures M. Jawad Latif, Bernard J. Park Thoracic Surgery Service, Memorial Sloan Kettering Cancer Center, New York, NY, USA Contributions:
Disclosure. Industry-sponsored grants. Research Collaboration. Consultant. Educational and research grants from Olympus Corporation
 Image Guided Surgery Kazuhiro Yasufuku MD, PhD Director of Endoscopy, University Health Network Director, Interventional Thoracic Surgery Program Associate Professor of Surgery, University of Toronto Division
Image Guided Surgery Kazuhiro Yasufuku MD, PhD Director of Endoscopy, University Health Network Director, Interventional Thoracic Surgery Program Associate Professor of Surgery, University of Toronto Division
Intraoperative ultrasonographic localization of pulmonary ground-glass opacities
 Kondo et al General Thoracic Surgery Intraoperative ultrasonographic localization of pulmonary ground-glass opacities Ryoichi Kondo, MD, PhD, a Kazuo Yoshida, MD, PhD, a Kazutoshi Hamanaka, MD, a Masahiro
Kondo et al General Thoracic Surgery Intraoperative ultrasonographic localization of pulmonary ground-glass opacities Ryoichi Kondo, MD, PhD, a Kazuo Yoshida, MD, PhD, a Kazutoshi Hamanaka, MD, a Masahiro
Laparoscopic Bowel Surgery. Dr. G. Mapeso Sept 14, 2007 Summer School Thunder Bay Medical Society
 Laparoscopic Bowel Surgery Dr. G. Mapeso Sept 14, 2007 Summer School Thunder Bay Medical Society Challenges and Barriers Acquisition of Skills Laparoscopic Bowel Data and Experience Technique (How I do
Laparoscopic Bowel Surgery Dr. G. Mapeso Sept 14, 2007 Summer School Thunder Bay Medical Society Challenges and Barriers Acquisition of Skills Laparoscopic Bowel Data and Experience Technique (How I do
