Self-injectable, infused and oral specialty drugs
|
|
|
- Jane Booker
- 6 years ago
- Views:
Transcription
1 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Aetna Specialty Pharmacy and the University of Virginia Health Plan Specialty Pharmacy Basic Health Drug List Self-injectable, infused and oral specialty drugs XX.XX.XXX.X (X/16)
2 You may only purchase specialty drugs through UVA Specialty Pharmacy or Aetna Specialty Pharmacy. Drugs purchased at any other pharmacy will not be covered. Please review your plan documents for more about the requirements and limitations of your pharmacy benefits and insurance plan. What is a specialty drug? Specialty drugs treat complex, chronic conditions that often require support by a nurse or pharmacist during treatment.because of the complex therapy needed, a pharmacist or nurse should check in with you often during your treatment. These drugs may be injected, infused or taken by mouth. They may need to be refrigerated. To get started with Aetna Specialty Pharmacy, call ASRX ( ) or TDD: ASRX ( ). Or visit Or call the University of Virginia Health Plan Specialty Pharmacy Key NPL National precertification * Drug may not be available through Aetna Specialty Pharmacy. Precertification Bold New QL ST NPS Quantity limit applies Step therapy applies Non-preferred specialty drug Health benefits and health insurance plans are offered, administered and/or underwritten by Aetna Health Inc., Aetna Health of California Inc., Aetna Health Insurance Company of New York, Aetna Health Insurance Company and/or Aetna Life Insurance Company (Aetna). In Florida, by Aetna Health Inc. and/or Aetna Life Insurance Company. In Maryland, by Aetna Health Inc., 151 Farmington Avenue, Hartford, CT Each insurer has sole financial responsibility for its own products. Aetna Pharmacy Management refers to an internal business unit of Aetna Health Management, LLC.
3 Antineoplastic agents Antineoplastics (oral) bexarotene capecitabine temozolomide tretinoin QL QL QL AFINITOR ST AFINITOR DIS BOSULIF ST CAELSA * COMETRIQ ERIVEDGE FARYDAK GILOTRIF * GLEEVEC HYCAMTIN IBRANCE ICLUSIG ST IMBRUVICA INLYTA ST IRESSA JAKAFI * LENVIMA * LYNPARZA MEKINIST NEXAVAR ST POMALYST PURIXAN ST REVLIMID SYCEL ST STIVARGA SUTENT TAFINLAR TARCEVA TARGRETIN TASIGNA ST TEMODAR THALOMID TYKERB VOTRIENT ST XELODA QL XALKORI * ZELBORAF ST ZOLINZA ZYDELIG ZYKADIA QL Antineoplastics hormonal agents leuprolide ELIGARD FASLODEX FIRMAGON LUPANETA LUON LUON DEPOT TRELSTAR LA Antineoplastics miscellaneous ACTIMMUNE ALFERON N INTRON A IRESSA TRELSTAR DEPOT TRELSTAR MIX VANTAS XTANDI * ST ZOLADEX ZYTIGA LU DEP-PED SYLATRON TARGRETIN Gel VALCHLOR NPS Blood products modifiers volume expanders Anti-inhibitor coagulant complex FEIBA NF FEIBA VH Blood-clotting factor VIIa (recombinant) NOVOSEVEN NOVOSEVEN RT Blood-clotting factor VIII (human) ALPHANATE CORIFACT HEMOFIL M HUMATE-P KOATE-DVI MONOCLATE-P WILATE Blood-clotting factor VIII (recombinant) ADVATE ELOCTATE HELIXATE FS IXINITY KOGENATE FS NOVOEIGHT RECOMBINATE XYNTHA Blood-clotting factor IX (nonrecombinant) ALPHANINE SD MONONINE OFILNINE Blood-clotting factor IX (recombinant) ALOLIX BEBULIN VH BENEFIX IXINITY
4 Blood-clotting factor XIII (recombinant) TRETTEN Blood-clotting complex KCENTRA Fibrinogen concentrate (human) RIASTAP NPL RIXUBIS Hematopoietic growth factors ARANESP EPOGEN GRANIX LEUKINE MIRCERA NEULASTA Hereditary angioedema BERINERT CINRYZE * FIRAZYR NEUMEGA NEUPOGEN NPLATE OCRIT OMACTA ZARXIO KALBITOR * RUCONEST * Paroxysmal nocturnal hemoglobinuria Cardiovascular system SOLIRIS Hypertension VECAMYL ST Inherited homozygous familial hypercholesterolemia Inherited heterozygous familial hypercholesterolemia JUXTAPID* ST KYNAMRO ST REPATHA QL ST ALUENT QL ST REPATHA QL ST Orthostatic hypotension NORTHERA ST Pulmonary hypertension agents epoprostenol * ADCIRCA sildenafil QL QL ST QL ST ADEMPAS FLOLAN * LETAIRIS OPSUMIT ORENITRAM QL ST REMODULIN * QL REVATIO QL ST TRACLEER TYVASO * VELETRI * VENTAVIS * Central nervous system Analgesics nonnarcotic IALT Anticonvulsants GABA modulators SABRIL * Huntington s disease chorea tetrabenazine XENAZINE *
5 Multiple sclerosis agents glatopa AMPYRA AUBAGIO AVONEX ST BETASERON COPAXONE 20 mg ST COPAXONE 40 mg QL ST ST EXTAVIA ST QL ST GILENYA LEMTRADA PLEGRIDY REBIF TECFIDERA TYSABRI QL ST QL ST QL ST ST Dermatological agents Antineoplastic-alkylating agents VALCHLOR Gel * ST Antipsoriatics COSENTYX ST ENBREL HUMIRA KINERET ST OTEZLA QL OTREXUP ST RASUVO ST REMICADE SIMPONI STELARA ST Endocrine system Acromegaly octreotide SANDOSTATIN SANDOSTATIN LAR SIGNIFOR LAR * SOMATULINE SOMAVERT Congenital sucrase-isomaltase deficiency SUCRAID * Corticotropin ACTHAR HP Cushing s disease SIGNIFOR KORLYM Diagnostic drugs THYROGEN Fabry disease FABRAZYME Gaucher disease CERDELGA CEREZYME ELELYSO * ST VIV ST ZAVESCA * Growth factors, insulin-like INCRELEX Growth hormone agents GENOTROPIN ST HUMATROPE ST NORDITROPIN ST NUTROPIN ST NUTROPIN AQ ST NUTROPIN AQ NUSPIN OMNITROPE SAIZEN ST SEROSTIM ST ZOMACTON ST ZORBTIVE Hereditary tyrosinemia ORFADIN * Homocystinuria CYSTADANE ST
6 Hormone replacement progestins MAKENA Hunter syndrome ELAASE * Hyperammonemia phenylbutyrate AMMONUL BUPHENYL Hyperparathyroidism doxercalciferol paricalcitol HECTOROL SENSIPAR ZEMPLAR Hypoparathyroidism NATPARA * QL Leptin deficiency MYALEPT QL LHRH/GnRH agonist analog pituitary suppressants SUPELIN LA SYNAREL Morquio A syndrome VIMIZIM Mucopolysaccharidosis I ALDURAZYME Mucopolysaccharidosis VI NAGLAZYME Phenylketonuria KUVAN * Pompe disease LUMIZYME MYOZYME Vasopressin receptor antagonists SAMSCA * Gastrointestinal system Bile acid synthesis disorders CHOLBAM * Crohn s disease CIMZIA ST ENTYVIO ST HUMIRA REMICADE Short bowel syndrome GATTEX * QL Infections and infestations Antiretrovirals fusion inhibitors FUZEON Antivirals cytomegalovirus (CMV) agents cidofovir foscarnet ganciclovir valganciclovir CYTOGAM CYTOVENE FOSCAVIR VALCYTE VALCYTE SOL VISTIDE
7 Antivirals hepatitis agents adefovir entecavir lamivudine ribapak ribasphere ribavirin BARACLUDE COPEGUS DAKLINZA EPIVIR HBV HARVONI HEPSERA I NFERGEN OLYSIO QL ST ST QL ST PEGASYS PEGINTRON REBETOL SOVALDI TECHNIVIE TYZEKA VIEKIRA ST ZEPATIER QL ST QL ST NPS Musculoskeletal system Bone-modifying agents ibandronate (inj only) pamidronate zoledronic acid FORTEO GANITE NPL OLIA RECLAST XGEVA ZOMETA Enzymes XIAFLEX Gout KRYSTEXXA Interleukin-1beta blockers ILARIS * Interleukin-1 blockers ARCALYST * Neuromuscular blocking agent neurotoxins BOTOX DYSPORT XEOMIN Osteoarthritis EUFLEXXA GEL-ONE INJ HYALGAN MONOVISC ST ST Rheumatoid arthritis ACTEMRA ST ACTEMRA SC CIMZIA ST ENBREL HUMIRA KINERET ST ORENCIA ST ST ORTHOVISC SUPARTZ ST SYNVISC ST SYNVISC ONE OTREXUP ST RASUVO ST REMICADE SIMPONI SIMPONI ARIA XELJANZ ST ST QL ST Ophthalmic agents Macular degeneration EYLEA LUCENTIS NPS NPL NPS NPL MACUGEN NPL VISUDYNE Macular edema OZURDEX Vitreomacular adhesion JETREA Respiratory tract agents Alpha-proteinase inhibitors ARALAST ARALAST NP GLASSIA * OLASTIN * OLASTIN-C * ZEMAIRA *
8 Antiasthmatic monoclonal antibodies XOLAIR Cystic fibrosis colistimethate sodium tobramycin neb sol BETHKIS NEB CAYSTON * COLY-MYCIN M KALYDECO * ORKAMBI * PULMOZYME TOBI TOBI podhaler Idiopathic pulmonary fibrosis ESBRIET OFEV Respiratory syncytial virus monoclonal antibodies SYNAGIS QL Tuberculosis SIRTURO ST Therapeutic nutrients vitamins minerals electrolytes Mineral supplements ferric gluconate FERRIOX FERRLECIT VENOFER Toxicologic agents Alcohol dependence VIVITROL Antidotes deferoxamine mesylate DESFERAL EXJADE JADENU Vaccines, toxoids and biologics Immune globulin CMV CYTOGAM Immune globulin immune disorders ADAGEN BIVIGAM CARIMUNE NANOFILTERED FLEBOGAMMA GAMASTAN S/D GAMMAGARD GAMMAGARD S/D GAMMAKED GAMMAPLEX GAMUNEX GAMUNEX-C HIZENTRA HYQVIA OCTAGAM IVIGEN VIVAGLOBIN Immune globulin hepatitis B HEPAGAM B HYPERHEP B NABI-HB Immune globulin rabies HYPERRAB S/D IMOGAM RABIES
9 Immune globulin Rh isoimmunization HYPERRHO S/D MICRHOGAM ULTRA-FILTERED RHOGAM ULTRA-FILTERED PLUS RHOPHYLAC WINRHO SDF Immune globulin tetanus HYPERTET S/D Miscellaneous Cystinosis CYSTARAN * OCYSBI ST Immunosuppressive agents azathioprine (inj only) cyclosporine gengraf mycophenolic acid mycophenolate mofetil sirolimus tacrolimus ASTAGRAF ATGAM CELLCEPT MYFORTIC NEORAL NULOJIX OGRAF RAPAMUNE SANDIMMUNE SIMULECT THYMOGLOBULIN ZORTRESS Narcolepsy XYREM * Primary periodic paralysis KEVEYIS * Systemic lupus erythematosus agents BENLYSTA Urea cycle disorder RAVICTI * Anxiolytics, sedatives, hypnotics miscellaneous HETLIOZ Parkinson's disease DUOPA * ST Wilson's disease Alpha-1 blockers phenoxybenzamine CUIMINE SYINE THIOLA DIBENZYLINE
10 Commercial fully insured members in Louisiana and Texas (except Federal Employee Health Benefit Plan members) who have coverage for medications that are added to or removed from the Aetna Specialty CareRx SM list, national precertification list, precertification safety edit list, precertification list, step-therapy list or quantity limit list, or have quantity limits modified, during the plan year will continue to have those medications covered at the same benefits level under their plan prior to the addition, removal or change, until their plan s renewal date. The term precertification means the utilization review process to determine whether the requested service, procedure, prescription drug or medical device meets the company s clinical criteria for coverage. It does not mean precertification as defined by Texas law, as a reliable representation of payment of care or services to fully insured HMO and PPO members. In accordance with state law, fully insured commercial California HMO members (except Federal Employee Health Benefit Plan members) who are receiving coverage for medications that are added to the precertification or step-therapy lists will continue to have those medications covered, for as long as the treating physician continues prescribing them, provided that the drug is appropriately prescribed and is considered safe and effective for treating the enrollee s medical condition. In accordance with state law, fully insured commercial Connecticut PPO members (except Federal Employee Health Benefit Plan members) who are receiving coverage for medications that are added to the precertification or step-therapy lists will continue to have those medications covered for as long as the treating physician prescribes them, provided the drug is medically necessary and more medically beneficial than other covered drugs. Nothing in this section shall preclude the prescribing provider from prescribing another drug covered by the plan that is medically appropriate for the enrollee, nor shall anything in this section be construed to prohibit generic drug substitutions. This material is for information only. Health benefits and health insurance plans contain exclusions and limitations. Not all health services are covered. See plan documents for a complete description of benefits, exclusions, limitations and conditions of coverage. Providers are independent contractors and are not agents of Aetna. Provider participation may change without notice. Aetna does not provide care or guarantee access to health services. Aetna Specialty Pharmacy refers to Aetna Specialty Pharmacy, LLC, a licensed pharmacy subsidiary of Aetna Inc. that operates through specialty pharmacy prescription fulfillment. Information is believed to be accurate as of the production date; however, it is subject to change. For more information about Aetna plans, refer to Policy forms issued in OK include: HMO OK COC-5 09/07, HMO/OK GA-3 11/01, HMO OK POS RIDER 08/07, GR-23 and/or GR-29/GR-29N Aetna Inc. XX.XX.XXX.X (X/16)
Please scroll down for list of drugs
 Posted on NaviNet Plan Central page 12-7-2015 IMPORTANT NOTICE REGARDING DRUG COVERAGE AND PEBTF MEMBERS: CERTAIN SPECIALTY MEDICATIONS EXCLUDED FROM MEDICAL BENEFIT FOR PEBTF PATIENTS Highmark administers
Posted on NaviNet Plan Central page 12-7-2015 IMPORTANT NOTICE REGARDING DRUG COVERAGE AND PEBTF MEMBERS: CERTAIN SPECIALTY MEDICATIONS EXCLUDED FROM MEDICAL BENEFIT FOR PEBTF PATIENTS Highmark administers
Please scroll down for list of drugs
 Posted on NaviNet Plan Central page 1-7-2016 REMINDER: IMPORTANT NOTICE REGARDING DRUG COVERAGE AND PEBTF MEMBERS: CERTAIN SPECIALTY MEDICATIONS EXCLUDED FROM MEDICAL BENEFIT FOR PEBTF PATIENTS Highmark
Posted on NaviNet Plan Central page 1-7-2016 REMINDER: IMPORTANT NOTICE REGARDING DRUG COVERAGE AND PEBTF MEMBERS: CERTAIN SPECIALTY MEDICATIONS EXCLUDED FROM MEDICAL BENEFIT FOR PEBTF PATIENTS Highmark
The Specialty Drug Program provides care management services to your members, including:
 Aetna Better Health is managed through CVS Health Specialty Pharmacy. The Specialty pharmacies fill prescriptions and ship drugs for complex medical conditions, including multiple sclerosis, rheumatoid
Aetna Better Health is managed through CVS Health Specialty Pharmacy. The Specialty pharmacies fill prescriptions and ship drugs for complex medical conditions, including multiple sclerosis, rheumatoid
Applies to members in the Aetna Value, Value Plus SM plan and Premier formularies
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Aetna Specialty Drug List Applies to members in the Aetna Value, Value Plus SM plan and Premier formularies
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Aetna Specialty Drug List Applies to members in the Aetna Value, Value Plus SM plan and Premier formularies
Applies to members in the Aetna Premier Plus formulary
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Aetna Specialty Drug List Applies to members in the Aetna Premier Plus formulary You may fill these drugs
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Aetna Specialty Drug List Applies to members in the Aetna Premier Plus formulary You may fill these drugs
April 2015 NALC Specialty Pharmacy Drug List Providing one of the broadest offerings of specialty pharmaceuticals in the industry
 NALC Specialty Pharmacy Drug List Providing one of the broadest offerings of specialty pharmaceuticals in the industry The NALC Specialty Pharmacy Drug List is a guide of medications available through
NALC Specialty Pharmacy Drug List Providing one of the broadest offerings of specialty pharmaceuticals in the industry The NALC Specialty Pharmacy Drug List is a guide of medications available through
Specialty Drug List. For members with the Aetna Standard Plan 2018 Aetna Specialty Drug List (5/18)
 Specialty Drug List For members with the Aetna Standard Plan 2018 Aetna Specialty Drug List 05.02.409.1 (5/18) How to use this guide You may fill these drugs at an in-network specialty pharmacy, like Aetna
Specialty Drug List For members with the Aetna Standard Plan 2018 Aetna Specialty Drug List 05.02.409.1 (5/18) How to use this guide You may fill these drugs at an in-network specialty pharmacy, like Aetna
Prior Authorization Drug List
 Prior Authorization Drug List This is a list of drugs that require Prior Authorization before coverage is provided. If you are prescribed a medication that requires Prior Authorization, your physician
Prior Authorization Drug List This is a list of drugs that require Prior Authorization before coverage is provided. If you are prescribed a medication that requires Prior Authorization, your physician
Specialty drug coverage
 Specialty drug coverage For members with the Aetna Value plan, Value Plus plan and Premier plan 2017 Aetna Specialty Drug List 54.03.439.1 C (7/17) aetna.com You may get your first fill of these drugs
Specialty drug coverage For members with the Aetna Value plan, Value Plus plan and Premier plan 2017 Aetna Specialty Drug List 54.03.439.1 C (7/17) aetna.com You may get your first fill of these drugs
Specialty drug coverage
 Specialty drug coverage For members with the Aetna Premier Plus plan 2018 Aetna Specialty Drug List 05.03.429.1 E (9/17) aetna.com You may fill these drugs at an in-network specialty pharmacy, like Aetna
Specialty drug coverage For members with the Aetna Premier Plus plan 2018 Aetna Specialty Drug List 05.03.429.1 E (9/17) aetna.com You may fill these drugs at an in-network specialty pharmacy, like Aetna
Specialty drug coverage
 Specialty drug coverage For members with the Aetna Value plan, Value Plus plan and Premier plan 2018 Aetna Specialty Drug List 05.03.439.1 H (9/17) aetna.com You may get your first fill of these drugs
Specialty drug coverage For members with the Aetna Value plan, Value Plus plan and Premier plan 2018 Aetna Specialty Drug List 05.03.439.1 H (9/17) aetna.com You may get your first fill of these drugs
Specialty drug. coverage
 Ut labo. Mil mo blabore Specialty drug ssumque conet officim. coverage For members with the Aetna Premier Plus plan Aetna Specialty Drug List aetna.com You may get your first fill of these drugs at any
Ut labo. Mil mo blabore Specialty drug ssumque conet officim. coverage For members with the Aetna Premier Plus plan Aetna Specialty Drug List aetna.com You may get your first fill of these drugs at any
January 2018 Updated 12/01/2017 Advanced Control Specialty Formulary
 January 2018 Updated 12/01/2017 Advanced Control Specialty Formulary The CVS Caremark Advanced Control Specialty Formulary is a guide within select therapeutic categories for clients, plan members and
January 2018 Updated 12/01/2017 Advanced Control Specialty Formulary The CVS Caremark Advanced Control Specialty Formulary is a guide within select therapeutic categories for clients, plan members and
Advanced Control Specialty Formulary
 Advanced Control Specialty Formulary July 2018 Updated 05/09/2018 The CVS Caremark Advanced Control Specialty Formulary is a guide within select therapeutic categories for clients, plan members and health
Advanced Control Specialty Formulary July 2018 Updated 05/09/2018 The CVS Caremark Advanced Control Specialty Formulary is a guide within select therapeutic categories for clients, plan members and health
Specialty drug coverage
 Specialty drug coverage For members with the Aetna Value plan, Value Plus plan and Premier plan Aetna Specialty Drug List aetna.com You may get your first fill of these drugs at any in-network specialty
Specialty drug coverage For members with the Aetna Value plan, Value Plus plan and Premier plan Aetna Specialty Drug List aetna.com You may get your first fill of these drugs at any in-network specialty
encourages correct prescription drug use for a particular diagnosis, promotes the safe use of prescription drugs, and helps reduce drug costs.
 Prior Authorization Your health plan participates in a Prior Authorization (PA) program for specific prescription drugs. This means that Caremark must review certain information provided by your doctor
Prior Authorization Your health plan participates in a Prior Authorization (PA) program for specific prescription drugs. This means that Caremark must review certain information provided by your doctor
BB&T Prior Authorization Program Drug List
 BB&T Prior Authorization Program Drug List Prior authorization programs are designed to support BB&T prior authorization and medical exception initiatives. Prior authorization and medical exceptions apply
BB&T Prior Authorization Program Drug List Prior authorization programs are designed to support BB&T prior authorization and medical exception initiatives. Prior authorization and medical exceptions apply
MedStar Select Pharmacy Services
 Pharmacy Services 1 MedStar Select Pharmacy Services Table of Contents At a Glance..page 2 Obtaining Prior Authorization for Medically Covered Medications..page 2 Pharmacy Services 2 At a Glance Welcome
Pharmacy Services 1 MedStar Select Pharmacy Services Table of Contents At a Glance..page 2 Obtaining Prior Authorization for Medically Covered Medications..page 2 Pharmacy Services 2 At a Glance Welcome
Medical Specialty Drug List
 Neighborhood Health Plan Medical Specialty Drug List UPDATES FOR ALL NHP MEMBERS Novologix PA HCPCS HCPCS Description Drug Name 8/14/2017 J3262 Injection, tocilizumab, 1 Actemra 1/1/2018 J2504 Injection,
Neighborhood Health Plan Medical Specialty Drug List UPDATES FOR ALL NHP MEMBERS Novologix PA HCPCS HCPCS Description Drug Name 8/14/2017 J3262 Injection, tocilizumab, 1 Actemra 1/1/2018 J2504 Injection,
Specialty Drug coverage reviews
 Specialty Drug coverage reviews Specialty drugs requiring prior authorization 2018 Aetna Standard plan 05.03.488.1 C (4/18) aetna.com The drugs on this list require prior authorization* review under the
Specialty Drug coverage reviews Specialty drugs requiring prior authorization 2018 Aetna Standard plan 05.03.488.1 C (4/18) aetna.com The drugs on this list require prior authorization* review under the
Specialty. Drug. coverage reviews
 Call to action small copy (especially related to mobile apps). Hendani adionse rferum faceatis incte voluptassi aut maximpe rumquid ebita- Call out bold Call out light Contact information, Specialty call
Call to action small copy (especially related to mobile apps). Hendani adionse rferum faceatis incte voluptassi aut maximpe rumquid ebita- Call out bold Call out light Contact information, Specialty call
Pharmacy Services Table of Contents
 Pharmacy Services Table of Contents At a Glance..page 2 Obtaining ly Covered Medications..page 2 Pharmacy Services 2 At a Glance Welcome to MedStar Pharmacy Services. MedStar Pharmacy Services partners
Pharmacy Services Table of Contents At a Glance..page 2 Obtaining ly Covered Medications..page 2 Pharmacy Services 2 At a Glance Welcome to MedStar Pharmacy Services. MedStar Pharmacy Services partners
How to search for a Pharmacy or Drug using the Express Scripts website
 How to search for a Pharmacy or Drug using the Express Scripts website You are able to look for a participating pharmacy or a particular drug using the following website: https://host1.medcohealth.com/consumer/site/openenrollment?accesscode=natplsnaprf14&pagename=oeinfo
How to search for a Pharmacy or Drug using the Express Scripts website You are able to look for a participating pharmacy or a particular drug using the following website: https://host1.medcohealth.com/consumer/site/openenrollment?accesscode=natplsnaprf14&pagename=oeinfo
Essential Health Benefits Standard Specialty PA and QL List July 2016
 Anti-infectives Antiretrovirals, HIV SELZENTRY (maraviroc) Cardiology Antilipemic Pulmonary Arterial Hypertension Central Nervous System Anticonvulsants Depressant Neurotoxins Parkinson's Sleep Disorder
Anti-infectives Antiretrovirals, HIV SELZENTRY (maraviroc) Cardiology Antilipemic Pulmonary Arterial Hypertension Central Nervous System Anticonvulsants Depressant Neurotoxins Parkinson's Sleep Disorder
Specialty Pharmacy Drug List
 Specialty Pharmacy Drug List Prescription Solutions Specialty Pharmacy Our Specialty Pharmacy provides patients with comprehensive and coordinated delivery and support services related to high-cost oral
Specialty Pharmacy Drug List Prescription Solutions Specialty Pharmacy Our Specialty Pharmacy provides patients with comprehensive and coordinated delivery and support services related to high-cost oral
Pharmacy Services Table of Contents
 Pharmacy Services Table of Contents At a Glance..page 2 Obtaining ly Covered Medications..page 2 Pharmacy Services 2 At a Glance Welcome to MedStar Select Pharmacy Services. MedStar Select Pharmacy Services
Pharmacy Services Table of Contents At a Glance..page 2 Obtaining ly Covered Medications..page 2 Pharmacy Services 2 At a Glance Welcome to MedStar Select Pharmacy Services. MedStar Select Pharmacy Services
National Preferred Formulary Prior Approval List As of: 09/25/2018
 National Preferred Formulary Prior Approval List As of: 09/25/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
National Preferred Formulary Prior Approval List As of: 09/25/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
Injection, factor viii (antihemophilic factor, recombinant) Afstyla AvMed Novologix. Sildenafil citrate, 25 mg Revatio Novologix Novologix
 90284 or J1559 90378 J0129 MEDICATIONAUTHORIZATIONWORKFLOWFORDRUGSTHATREQUIREPRIOR-AUTHORIZATION (06/9/17) BASEDONLOCATIONWHEREDRUGWILLBEADMINISTERED J-code Medication Drug Name Immune globulin (SCIg),
90284 or J1559 90378 J0129 MEDICATIONAUTHORIZATIONWORKFLOWFORDRUGSTHATREQUIREPRIOR-AUTHORIZATION (06/9/17) BASEDONLOCATIONWHEREDRUGWILLBEADMINISTERED J-code Medication Drug Name Immune globulin (SCIg),
Current Trends in Specialty Pharmacy Management. priorityhealth.com
 Current Trends in Specialty Pharmacy Management A little background Priority Health members fill about 25,000 prescriptions every day We spend over $1,250,000 a day on prescriptions Over 80% of all prescriptions
Current Trends in Specialty Pharmacy Management A little background Priority Health members fill about 25,000 prescriptions every day We spend over $1,250,000 a day on prescriptions Over 80% of all prescriptions
National Preferred Formulary Prior Approval List As of: 10/22/2018
 National Preferred Formulary Prior Approval List As of: 10/22/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
National Preferred Formulary Prior Approval List As of: 10/22/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
CLOTTING FACTOR REPLACEMENT THERAPY
 CLOTTING FACTOR REPLACEMENT THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage
CLOTTING FACTOR REPLACEMENT THERAPY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage
MEDICATION AUTHORIZATION WORKFLOW FOR DRUGS THAT REQUIRE PRIOR-AUTHORIZATION (03/23/18) BASED ON LOCATION WHERE DRUG WILL BE ADMINISTERED
 J9264 Injection, paclitaxel protein-bound particles, 1 mg ABRAXANE J3262 Injection, tocilizumab, 1 mg ACTEMRA J0800 Injection, corticotropin, up to 40 units ACTHAR HP J9042 Injection, brentuximab vedotin,
J9264 Injection, paclitaxel protein-bound particles, 1 mg ABRAXANE J3262 Injection, tocilizumab, 1 mg ACTEMRA J0800 Injection, corticotropin, up to 40 units ACTHAR HP J9042 Injection, brentuximab vedotin,
BRAND NAME GENERIC NAME THERAPEUTIC CLASS DISEASE STATE ENDOCRINE AND METABOLIC AGENTS - Acthar HP 80UNIT/ML Corticotropin
 Products listed below may be covered under your Specialty Pharmacy benefit. To receive coverage for Specialty Products, drugs must be dispensed through select contracted specialty pharmacy network providers.
Products listed below may be covered under your Specialty Pharmacy benefit. To receive coverage for Specialty Products, drugs must be dispensed through select contracted specialty pharmacy network providers.
National Preferred Formulary Prior Approval List As of: 11/08/2018
 National Preferred Formulary Prior Approval List As of: 11/08/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
National Preferred Formulary Prior Approval List As of: 11/08/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
Essential Health Benefits Standard Specialty PA and QL List April 2015
 Anti-infectives Antiretrovirals, Hepatitis B BARACLUDE (entecavir) BARACLUDE (entecavir) Soln 630 ml/30days HEPSERA (adefovir) TYZEKA (telbivudine ) Antiretrovirals, HIV FUZEON (enfuvirtide) 60 vials or
Anti-infectives Antiretrovirals, Hepatitis B BARACLUDE (entecavir) BARACLUDE (entecavir) Soln 630 ml/30days HEPSERA (adefovir) TYZEKA (telbivudine ) Antiretrovirals, HIV FUZEON (enfuvirtide) 60 vials or
FirstCare Medical Pharmacy Prior Authorization Requirements
 90378 palivizumab SYNAGIS ANTIVIRAL MONOCLONAL C9257 bevacizumab 0.25mg AVASTIN J0129 abatacept ORENCIA SELECTIVE COSTIMULATION MODULATORS J0135 adalimumab HUMIRA ANALGESICS ANTI-INFLAMMATORY J0178 aflibercept
90378 palivizumab SYNAGIS ANTIVIRAL MONOCLONAL C9257 bevacizumab 0.25mg AVASTIN J0129 abatacept ORENCIA SELECTIVE COSTIMULATION MODULATORS J0135 adalimumab HUMIRA ANALGESICS ANTI-INFLAMMATORY J0178 aflibercept
HCPCS CODE. HEMOPHILIA, VON WILLEBRAND DISEASE, & RELATED BLEEDING DISORDERS Advate J7192 J7186
 Drugs Requiring Prior Authorization. Non-Covered Drugs May Be Covered Under Part D (For Part D Determinations Contact Molina Medicare Pharmacy at extension 179796). DRUG BRAND NAMES BY CONDITION HCPCS
Drugs Requiring Prior Authorization. Non-Covered Drugs May Be Covered Under Part D (For Part D Determinations Contact Molina Medicare Pharmacy at extension 179796). DRUG BRAND NAMES BY CONDITION HCPCS
Pharmacy Services Table of Contents
 Pharmacy Services Table of Contents At a Glance..page 2 Obtaining Prior Authorization for Medically Covered Medications..page 2 Prior Authorization List page 3 Pharmacy Services 2 At a Glance Welcome to
Pharmacy Services Table of Contents At a Glance..page 2 Obtaining Prior Authorization for Medically Covered Medications..page 2 Prior Authorization List page 3 Pharmacy Services 2 At a Glance Welcome to
Health. bulletin. Important: Formulary Drug Removals DECEMBER 2017
 P.O. Box 16688 Phoenix, Arizona 85011 (888) 331-0222 www.svckairoshealthaz.org DECEMBER 2017 Health bulletin Some people look forward to the holidays all year, while others see the holiday season approaching
P.O. Box 16688 Phoenix, Arizona 85011 (888) 331-0222 www.svckairoshealthaz.org DECEMBER 2017 Health bulletin Some people look forward to the holidays all year, while others see the holiday season approaching
2018 Product Catalog Winter issue
 Pharmacies McKesson Plasma and Biologics LLC 218 Product Catalog Winter issue Contact us: 877.625.2566 mpb@mckesson.com www.mckesson.com/mpb Welcome to the McKesson Plasma and Biologics LLC Winter 218
Pharmacies McKesson Plasma and Biologics LLC 218 Product Catalog Winter issue Contact us: 877.625.2566 mpb@mckesson.com www.mckesson.com/mpb Welcome to the McKesson Plasma and Biologics LLC Winter 218
First Name Last Name Patient Gender. Patient DOB Patient Phone # Alternative Phone # City State Zip code. Prescriber Name Contact Name Contact Phone #
 Hemophilia Product Prior Authorization Form Please complete this form in its entirety and provide relevant progress notes and/or bleeding diaries and fax to 1-888-656-0841 or call 1-800-424-7892. All lab
Hemophilia Product Prior Authorization Form Please complete this form in its entirety and provide relevant progress notes and/or bleeding diaries and fax to 1-888-656-0841 or call 1-800-424-7892. All lab
HCPCS DESCRIPTION/GENERIC NAME
 2013 Molina Healthcare/Molina Medicare/Healthy Advantage Codification List Effective: 2/1/2013 Revised: xx/xx/xxxx Disclaimer: Codes are subject to change based on National coding guidelines, CMS, UT State
2013 Molina Healthcare/Molina Medicare/Healthy Advantage Codification List Effective: 2/1/2013 Revised: xx/xx/xxxx Disclaimer: Codes are subject to change based on National coding guidelines, CMS, UT State
sa EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Prior Authorization of Drugs sa EFFECTIVE DATE: 06 01 2018 POLICY LAST UPDATED: 11 20 2018 OVERVIEW This policy documents drugs that are covered under the member s Commercial medical
Medical Coverage Policy Prior Authorization of Drugs sa EFFECTIVE DATE: 06 01 2018 POLICY LAST UPDATED: 11 20 2018 OVERVIEW This policy documents drugs that are covered under the member s Commercial medical
2006 Focus on Specialty Pharmacy
 TrendsRx Focus on Specialty Pharmacy Biotech and specialty pharmaceuticals offer groundbreaking medical advances in the treatment of complex illnesses. These products are high cost, but have made the most
TrendsRx Focus on Specialty Pharmacy Biotech and specialty pharmaceuticals offer groundbreaking medical advances in the treatment of complex illnesses. These products are high cost, but have made the most
Prior Authorization and Voluntary Preservice Determination Requests for Certain Pharmacy Drugs
 October 2016 Prior Authorization and Voluntary Preservice Determination Requests for Certain Pharmacy Drugs Important Changes We want to let you know that on November 14, 2016, we will change prior authorization
October 2016 Prior Authorization and Voluntary Preservice Determination Requests for Certain Pharmacy Drugs Important Changes We want to let you know that on November 14, 2016, we will change prior authorization
Ambrisentan (Letairis) Drugs LETAIRIS. Covered Uses All FDA-approved indications not otherwise excluded from Part D. Exclusion Criteria Pregnancy
 Ambrisentan (Letairis) LETAIRIS Pregnancy 1 apomorphine (Apokyn) APOKYN 2 Apremilast (Otezla) OTEZLA, OTEZLA STARTER ORAL TABLETS,DOSE PACK 10 MG (4)-20 MG (4)-30 MG (47) 3 Aprepitant (Emend) aprepitant
Ambrisentan (Letairis) LETAIRIS Pregnancy 1 apomorphine (Apokyn) APOKYN 2 Apremilast (Otezla) OTEZLA, OTEZLA STARTER ORAL TABLETS,DOSE PACK 10 MG (4)-20 MG (4)-30 MG (47) 3 Aprepitant (Emend) aprepitant
National Preferred Formulary Prior Approval List As of: 12/31/2018
 National Preferred Formulary Prior Approval List As of: 12/31/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
National Preferred Formulary Prior Approval List As of: 12/31/2018 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
Clotting Disorder Therapy
 Last Review Date: October 13, 2017 Number: MG.MM.PH.25b Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: October 13, 2017 Number: MG.MM.PH.25b Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
National Preferred Formulary Prior Approval List As of: 1/17/2019
 National Preferred Formulary Prior Approval List As of: 1/17/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
National Preferred Formulary Prior Approval List As of: 1/17/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) Trade Name Class Prior Authorization Program KYMRIAH (CAR-T)
Prior Authorization Drug List
 Prior Authorization Drug List Most prescriptions are filled right away when you take them to the pharmacy. But some drugs need to be reviewed by your health plan before they re covered. This process is
Prior Authorization Drug List Most prescriptions are filled right away when you take them to the pharmacy. But some drugs need to be reviewed by your health plan before they re covered. This process is
Drugs Requiring Prior Authorization Effective
 Drugs Requiring Prior Authorization Effective 3 1 2012 Disclaimer: Codes are subject to change based on National coding guidelines, CMS, UT State Medicaid benefits, and MHU PA review Guide. Only covered
Drugs Requiring Prior Authorization Effective 3 1 2012 Disclaimer: Codes are subject to change based on National coding guidelines, CMS, UT State Medicaid benefits, and MHU PA review Guide. Only covered
Ambrisentan (Letairis) Drugs LETAIRIS. Covered Uses All FDA-approved indications not otherwise excluded from Part D. Exclusion Criteria Pregnancy
 Ambrisentan (Letairis) LETAIRIS Pregnancy 1 apomorphine (Apokyn) APOKYN 2 Apremilast (Otezla) OTEZLA, OTEZLA STARTER ORAL TABLETS,DOSE PACK 10 MG (4)-20 MG (4)-30 MG (47) 3 Aprepitant (Emend) aprepitant
Ambrisentan (Letairis) LETAIRIS Pregnancy 1 apomorphine (Apokyn) APOKYN 2 Apremilast (Otezla) OTEZLA, OTEZLA STARTER ORAL TABLETS,DOSE PACK 10 MG (4)-20 MG (4)-30 MG (47) 3 Aprepitant (Emend) aprepitant
TREND REPORT 2017 EIGHTH EDITION
 MAGELLAN RX MANAGEMENT MEDICAL PHARMACY TREND REPORT 2017 EIGHTH EDITION Table of Contents 01 Introduction 02 Executive Summary 04 Medical Pharmacy Overview 06 Medical Pharmacy Trend Drivers 12 Medical
MAGELLAN RX MANAGEMENT MEDICAL PHARMACY TREND REPORT 2017 EIGHTH EDITION Table of Contents 01 Introduction 02 Executive Summary 04 Medical Pharmacy Overview 06 Medical Pharmacy Trend Drivers 12 Medical
Standard Specialty PA and QL List October 2014
 Anti-infectives Antiretrovirals, Hepatitis B BARACLUDE (entecavir) BARACLUDE (entecavir) Soln 630 ml/30days HEPSERA (adefovir) TYZEKA (telbivudine ) Antiretrovirals, HIV FUZEON (enfuvirtide) 60 vials or
Anti-infectives Antiretrovirals, Hepatitis B BARACLUDE (entecavir) BARACLUDE (entecavir) Soln 630 ml/30days HEPSERA (adefovir) TYZEKA (telbivudine ) Antiretrovirals, HIV FUZEON (enfuvirtide) 60 vials or
The following is a summary of the medical services prior authorization changes effective January 1, 2019:
 PROVIDER MEMO To: From: Date: Subject: Santa Clara Family Health Plan Providers Utilization Management December 27, 2018 2019 Dear Providers, Santa Clara Family Health Plan (SCFHP) has made some changes
PROVIDER MEMO To: From: Date: Subject: Santa Clara Family Health Plan Providers Utilization Management December 27, 2018 2019 Dear Providers, Santa Clara Family Health Plan (SCFHP) has made some changes
Prior Authorization (PA) List
 Prior Authorization (PA) List It is recommended to verify benefits and authorization requirements prior to services being received. Category Services Comments Acute Care Hospital Elective/Urgent/Emergent
Prior Authorization (PA) List It is recommended to verify benefits and authorization requirements prior to services being received. Category Services Comments Acute Care Hospital Elective/Urgent/Emergent
Standard Specialty PA and QL List July 2015
 Anti-infectives Antiretrovirals, Hepatitis B BARACLUDE (entecavir) BARACLUDE (entecavir) Soln 630 ml/30days HEPSERA (adefovir) TYZEKA (telbivudine ) Antiretrovirals, HIV FUZEON (enfuvirtide) 60 vials or
Anti-infectives Antiretrovirals, Hepatitis B BARACLUDE (entecavir) BARACLUDE (entecavir) Soln 630 ml/30days HEPSERA (adefovir) TYZEKA (telbivudine ) Antiretrovirals, HIV FUZEON (enfuvirtide) 60 vials or
CODE GENERIC NAME TRADE
 CODE GENERIC NAME TRADE 90281 Immune globulin, IM 90283 Immune globulin IgIV 90284 Immune globulin 100mg SQ SCIg 90378 Palivizumab 50mg Synagis C9014 Cerliponase alfa Brineura C9015 C 1 esterase inhibitor
CODE GENERIC NAME TRADE 90281 Immune globulin, IM 90283 Immune globulin IgIV 90284 Immune globulin 100mg SQ SCIg 90378 Palivizumab 50mg Synagis C9014 Cerliponase alfa Brineura C9015 C 1 esterase inhibitor
Specialty medicine: Pearls from the PBMI conference, Scottsdale, Arizona Dr. Elsa Badenhorst
 Specialty medicine: Pearls from the PBMI conference, Scottsdale, Arizona 2012 Dr. Elsa Badenhorst The Magic Bullet Paul Ehrlich (1854-1915) if a compound could be made that selectively targeted a diseasecausing
Specialty medicine: Pearls from the PBMI conference, Scottsdale, Arizona 2012 Dr. Elsa Badenhorst The Magic Bullet Paul Ehrlich (1854-1915) if a compound could be made that selectively targeted a diseasecausing
PHARMACY TIMES BY IEHP PHARMACEUTICAL SERVICES DEPARTMENT November 20, 2013
 PHARMACY TIMES BY IEHP PHARMACEUTICAL SERVICES DEPARTMENT November 20, 2013 We would like to inform you of the following changes to the 2013 IEHP that were approved by the Pharmacy and Therapeutics Subcommittee
PHARMACY TIMES BY IEHP PHARMACEUTICAL SERVICES DEPARTMENT November 20, 2013 We would like to inform you of the following changes to the 2013 IEHP that were approved by the Pharmacy and Therapeutics Subcommittee
2018 Prior Authorization
 2018 Prior Authorization FID 18088 Prior Authorization ACTEMRA Products Affected Actemra INJ 162MG/0.9ML PA Details Age Other 1 ACTIMMUNE Products Affected Actimmune PA Details Age Other 2 ADEMPAS Products
2018 Prior Authorization FID 18088 Prior Authorization ACTEMRA Products Affected Actemra INJ 162MG/0.9ML PA Details Age Other 1 ACTIMMUNE Products Affected Actimmune PA Details Age Other 2 ADEMPAS Products
National Preferred Formulary Prior Approval List As of: 04/01/2019
 National Preferred Formulary Prior Approval List As of: 04/01/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) KYMRIAH (CAR-T) ADOPTIVE IMMUNOTHERAPY CUSTOM LUXTURNA (gene
National Preferred Formulary Prior Approval List As of: 04/01/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) KYMRIAH (CAR-T) ADOPTIVE IMMUNOTHERAPY CUSTOM LUXTURNA (gene
National Preferred Formulary Prior Approval List As of: 03/25/2019
 National Preferred Formulary Prior Approval List As of: 03/25/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) KYMRIAH (CAR-T) ADOPTIVE IMMUNOTHERAPY CUSTOM LUXTURNA (gene
National Preferred Formulary Prior Approval List As of: 03/25/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) KYMRIAH (CAR-T) ADOPTIVE IMMUNOTHERAPY CUSTOM LUXTURNA (gene
Subject: Site of Care Policy. Effective Date: 01/2019 DESCRIPTION
 Subject: Site of Care Policy Effective Date: 01/2019 DESCRIPTION In an effort to minimize out-of-pocket costs for OSU Health Plan members and to improve cost efficiencies for the overall health care system,
Subject: Site of Care Policy Effective Date: 01/2019 DESCRIPTION In an effort to minimize out-of-pocket costs for OSU Health Plan members and to improve cost efficiencies for the overall health care system,
ANSWER. The committee considers: Food and Drug Administration (FDA) approved indications. Manufacturer s package labeling instructions
 clinically sound medication use Prior Authorization QW hy do I need a prior authorization for some ANSWER medications? Some medications must be authorized for coverage because they re only approved or
clinically sound medication use Prior Authorization QW hy do I need a prior authorization for some ANSWER medications? Some medications must be authorized for coverage because they re only approved or
National Preferred Formulary Prior Approval List As of: 04/01/2019
 National Preferred Formulary Prior Approval List As of: 04/01/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) KYMRIAH (CAR-T) ADOPTIVE IMMUNOTHERAPY CUSTOM LUXTURNA (gene
National Preferred Formulary Prior Approval List As of: 04/01/2019 Helpful Tip: To search for a specific drug, use the find feature (Ctrl + F) KYMRIAH (CAR-T) ADOPTIVE IMMUNOTHERAPY CUSTOM LUXTURNA (gene
All of Colorado HealthOP's networks use the Cigna Performance product for our prescription drug coverage.
 All of Colorado HealthOP's networks use the Cigna Performance product for our prescription drug coverage. Please see the Cigna Specialty Pharmacy Drug List below for the speciality prescription drug list
All of Colorado HealthOP's networks use the Cigna Performance product for our prescription drug coverage. Please see the Cigna Specialty Pharmacy Drug List below for the speciality prescription drug list
Clinical Policy: Ocrelizumab (Ocrevus) Reference Number: CP.PHAR.335 Effective Date: Last Review Date: 05.18
 Clinical Policy: (Ocrevus) Reference Number: CP.PHAR.335 Effective Date: 04.01.17 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Ocrevus) Reference Number: CP.PHAR.335 Effective Date: 04.01.17 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Plasma Protein Products: Why we do what we do. Peter Saunders Associate Director, National Operations April 24, 2015
 Plasma Protein Products: Why we do what we do Peter Saunders Associate Director, National Operations April 24, 2015 Outline Introduction Background and Regulations Business Cycle Product Selection Process
Plasma Protein Products: Why we do what we do Peter Saunders Associate Director, National Operations April 24, 2015 Outline Introduction Background and Regulations Business Cycle Product Selection Process
CLOTTING FACTORS, COAGULANT BLOOD PRODUCTS & OTHER HEMOSTATICS
 CLOTTING FACTORS, COAGULANT BLOOD PRODUCTS & OTHER HEMOSTATICS Protocol: PHA027 Effective Date: February 1, 2019 Table of Contents Page BENEFIT CONSIDERATIONS... 1 COVERAGE RATIONALE... 2 US FOOD AND DRUG
CLOTTING FACTORS, COAGULANT BLOOD PRODUCTS & OTHER HEMOSTATICS Protocol: PHA027 Effective Date: February 1, 2019 Table of Contents Page BENEFIT CONSIDERATIONS... 1 COVERAGE RATIONALE... 2 US FOOD AND DRUG
San Francisco Health Service System
 San Francisco Health Service System Pharmacy Trends Board Forum: November 10, 2016 Prepared by: Aon s Pharmacy Point of View We Believe Getting patients to the RIGHT drug at the RIGHT channel for the RIGHT
San Francisco Health Service System Pharmacy Trends Board Forum: November 10, 2016 Prepared by: Aon s Pharmacy Point of View We Believe Getting patients to the RIGHT drug at the RIGHT channel for the RIGHT
UBCM Conference. Joanne Jung, BScPharm Director, Pharmacy Services Mar 10, 2016
 UBCM Conference Joanne Jung, BScPharm Director, Pharmacy Services Mar 10, 2016 Agenda Drug Landscape Private drug plan trends Cost drivers Specialty Drugs Drug Trends Top Therapeutic Classes Drug Plan
UBCM Conference Joanne Jung, BScPharm Director, Pharmacy Services Mar 10, 2016 Agenda Drug Landscape Private drug plan trends Cost drivers Specialty Drugs Drug Trends Top Therapeutic Classes Drug Plan
Clinical Policy: Teriflunomide (Aubagio) Reference Number: CP.PHAR.262 Effective Date: Last Review Date: 05.18
 Clinical Policy: (Aubagio) Reference Number: CP.PHAR.262 Effective Date: 08.01.16 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Aubagio) Reference Number: CP.PHAR.262 Effective Date: 08.01.16 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Aubagio) Reference Number: CP.PHAR.262 Effective Date: 07.01.18 Last Review Date: 05.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Aubagio) Reference Number: CP.PHAR.262 Effective Date: 07.01.18 Last Review Date: 05.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end of this policy
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Ocrevus) Reference Number: CP.PHAR.335 Effective Date: 07.01.18 Last Review Date: 05.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Ocrevus) Reference Number: CP.PHAR.335 Effective Date: 07.01.18 Last Review Date: 05.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end of this policy
INDUSTRY OUTLOOK SPECIALTY DRUG REPORT
 INDUSTRY OUTLOOK SPECIALTY DRUG REPORT INDUSTRY OUTLOOK FOR SPECIALTY DRUGS: Specialty drugs are classified in the specialty category when they require special handling, specific administration techniques
INDUSTRY OUTLOOK SPECIALTY DRUG REPORT INDUSTRY OUTLOOK FOR SPECIALTY DRUGS: Specialty drugs are classified in the specialty category when they require special handling, specific administration techniques
The Evolving Role Of Prescription Benefit Managers
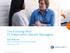 The Evolving Role Of Prescription Benefit Managers Steve Miller, MD Senior Vice President & Chief Medical Officer November 1, 2016 1 Prescription drugs: A growing share of U.S. healthcare spend Net spending
The Evolving Role Of Prescription Benefit Managers Steve Miller, MD Senior Vice President & Chief Medical Officer November 1, 2016 1 Prescription drugs: A growing share of U.S. healthcare spend Net spending
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Tysabri) Reference Number: CP.CPA.206 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Commercial Coding Implications Revision Log See Important Reminder at the end
Clinical Policy: (Tysabri) Reference Number: CP.CPA.206 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Commercial Coding Implications Revision Log See Important Reminder at the end
Prior Authorization Form
 5/2/2017 Prior Authorization Form INTOTAL HEALTH PLAN (SPC) Multiple Sclerosis MMT SGM This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
5/2/2017 Prior Authorization Form INTOTAL HEALTH PLAN (SPC) Multiple Sclerosis MMT SGM This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
Subject: Clotting Factors and Coagulant Blood Products
 09-J0000-34 Original Effective Date: 03/15/01 Reviewed: 04/11/18 Revised: 03/15/19 Subject: Clotting Factors and Coagulant Blood Products THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
09-J0000-34 Original Effective Date: 03/15/01 Reviewed: 04/11/18 Revised: 03/15/19 Subject: Clotting Factors and Coagulant Blood Products THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
Continued Development of Approved Biological Drugs
 Continued Development of Approved Biological Drugs A Quantitative Study of Additional Indications Approved Postlaunch in the United States White Paper December 2007 Maya Said Charles-André Brouwers Peter
Continued Development of Approved Biological Drugs A Quantitative Study of Additional Indications Approved Postlaunch in the United States White Paper December 2007 Maya Said Charles-André Brouwers Peter
CODE GENERIC NAME TRADE
 CODE GENERIC NAME TRADE 90281 Immune globulin, IM 90283 Immune globulin IgIV 90284 Immune globulin 100mg SQ SCIg 90378 Palivizumab 50mg Synagis A9503 Ibritumomab tiuxetan Zevalin A9606 Radium Ra 223 dichloride
CODE GENERIC NAME TRADE 90281 Immune globulin, IM 90283 Immune globulin IgIV 90284 Immune globulin 100mg SQ SCIg 90378 Palivizumab 50mg Synagis A9503 Ibritumomab tiuxetan Zevalin A9606 Radium Ra 223 dichloride
Pharmacy Benefit Drug Trends and Pipeline. Casey Robinson, PharmD, MBA, Cigna Pharmacy Management
 Pharmacy Benefit Drug Trends and Pipeline Casey Robinson, PharmD, MBA, Cigna Pharmacy Management Disclosure and Conflict of Interest Dr. Robinson declares no conflicts of interest, real or apparent, and
Pharmacy Benefit Drug Trends and Pipeline Casey Robinson, PharmD, MBA, Cigna Pharmacy Management Disclosure and Conflict of Interest Dr. Robinson declares no conflicts of interest, real or apparent, and
Pharmacy Benefit Drug Trends and Pipeline Casey Robinson, PharmD, MBA, Cigna Pharmacy Management
 Pharmacy Benefit Drug Trends and Pipeline Casey Robinson, PharmD, MBA, Cigna Pharmacy Management Disclosure and Conflict of Interest Pharmacist Objectives Dr. Robinson declares no conflicts of interest,
Pharmacy Benefit Drug Trends and Pipeline Casey Robinson, PharmD, MBA, Cigna Pharmacy Management Disclosure and Conflict of Interest Pharmacist Objectives Dr. Robinson declares no conflicts of interest,
Approval of a drug under this criteria document does not ensure full coverage of the drug.
 Department of Origin: Pharmacy Department(s) Affected: Integrated Healthcare Services and Pharmacy 09/13/18 Pharmacy Criteria Document: Biologics for Psoriatic Arthritis: infliximab, Orencia, and Simponi
Department of Origin: Pharmacy Department(s) Affected: Integrated Healthcare Services and Pharmacy 09/13/18 Pharmacy Criteria Document: Biologics for Psoriatic Arthritis: infliximab, Orencia, and Simponi
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Betaseron, Extavia) Reference Number: CP.CPA.331 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Commercial Coding Implications Revision Log See Important Reminder
Clinical Policy: (Betaseron, Extavia) Reference Number: CP.CPA.331 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Commercial Coding Implications Revision Log See Important Reminder
2018 Medical Drug Authorization List. Updated: April 1, 2018
 2018 Medical Drug Authorization List Updated: April 1, 2018 Health First Commercial Plans, Inc. is doing business under the name of Florida Hospital Care Advantage. Florida Hospital Care Advantage does
2018 Medical Drug Authorization List Updated: April 1, 2018 Health First Commercial Plans, Inc. is doing business under the name of Florida Hospital Care Advantage. Florida Hospital Care Advantage does
MS Injectable Drugs
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: MS Injectable Drugs Page: 1 of 5 Last Review Date: November 30, 2018 MS Injectable Drugs Description
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: MS Injectable Drugs Page: 1 of 5 Last Review Date: November 30, 2018 MS Injectable Drugs Description
Indranil Bagchi, Ph.D. Vice President, Market Access Specialty Care, Pfizer CADTH SYMPOSIUM May 6, 2013
 Characterizing the value of orphan drugs in an HTA environment Indranil Bagchi, Ph.D. Vice President, Market Access Specialty Care, Pfizer CADTH SYMPOSIUM May 6, 2013 Agenda Background Regulatory Approval
Characterizing the value of orphan drugs in an HTA environment Indranil Bagchi, Ph.D. Vice President, Market Access Specialty Care, Pfizer CADTH SYMPOSIUM May 6, 2013 Agenda Background Regulatory Approval
Five Drugs With Price Increases During 2016
 Five Drugs With Price Increases During 2016 #1 May Surprise You! Pharmaceutical price hikes have raised concerns about the affordability of critical and often life-saving medications, sparking debate,
Five Drugs With Price Increases During 2016 #1 May Surprise You! Pharmaceutical price hikes have raised concerns about the affordability of critical and often life-saving medications, sparking debate,
Premium Prior Authorization
 Premium Prior Authorization Some medications must be authorized for coverage because they re only approved or effective in treating specific illnesses, they cost more or they may be prescribed for conditions
Premium Prior Authorization Some medications must be authorized for coverage because they re only approved or effective in treating specific illnesses, they cost more or they may be prescribed for conditions
Specialty Pharmacy 101
 Specialty Pharmacy 101 The Landscape of Specialty Pharmacy Services DATE: October 27, 2011 NAME: TITLE: Clinical Pharmacist, Serve You Agenda Define specialty pharmacy Examine market trends and current
Specialty Pharmacy 101 The Landscape of Specialty Pharmacy Services DATE: October 27, 2011 NAME: TITLE: Clinical Pharmacist, Serve You Agenda Define specialty pharmacy Examine market trends and current
Prior Authorization (PA) List for: Fully Insured Plans Effective and Current as of: January 1, 2017 Phone: or
 Prior Authorization (PA) List for: Fully Insured Plans Effective and Current as of: January 1, 2017 Phone: 877.449.2884 or 859.335.3737 It is recommended to verify benefits and authorization requirements
Prior Authorization (PA) List for: Fully Insured Plans Effective and Current as of: January 1, 2017 Phone: 877.449.2884 or 859.335.3737 It is recommended to verify benefits and authorization requirements
CLOTTING FACTORS AND COAGULANT BLOOD PRODUCTS
 UnitedHealthcare Commercial Medical Benefit Drug Policy CLOTTING FACTORS AND COAGULANT BLOOD PRODUCTS Policy Number: 2018D0047K Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Medical Benefit Drug Policy CLOTTING FACTORS AND COAGULANT BLOOD PRODUCTS Policy Number: 2018D0047K Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
There may be thousands of orphan diseases, but some of
 Orphan Drug Markets Established Orphan Disease Markets: Innovators Wanted Meaningful product differentiation is required for new drugs to enjoy the rapid clinical development and commercial success that
Orphan Drug Markets Established Orphan Disease Markets: Innovators Wanted Meaningful product differentiation is required for new drugs to enjoy the rapid clinical development and commercial success that
Approval of a drug under this criteria document does not ensure full coverage of the drug.
 Criteria Document: Reference #: PC/B016 Page: 1 of 4 and Therapeutics Quality PRODUCT APPLICATIO: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne
Criteria Document: Reference #: PC/B016 Page: 1 of 4 and Therapeutics Quality PRODUCT APPLICATIO: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne
2018 Medical Drug Authorization List. Updated: January 1, 2018
 2018 Medical Drug Authorization List Updated: January 1, 2018 Health First Commercial Plans, Inc. and Health First Insurance, Inc. are both doing business under the name of Health First Health Plans. Health
2018 Medical Drug Authorization List Updated: January 1, 2018 Health First Commercial Plans, Inc. and Health First Insurance, Inc. are both doing business under the name of Health First Health Plans. Health
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Betaseron, Extavia) Reference Number: CP.PHAR.256 Effective Date: 08.01.16 Last Review Date: 05.18 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at
Clinical Policy: (Betaseron, Extavia) Reference Number: CP.PHAR.256 Effective Date: 08.01.16 Last Review Date: 05.18 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at
