Mehta Hiren R et al. IRJP 2 (4)
|
|
|
- Clifton Green
- 6 years ago
- Views:
Transcription
1 INTERNATIONAL RESEARCH JOURNAL OF PHARMACY ISSN Available online Review Article XIMELAGATRAN: A NEW DIRECT THROMBIN INHIBITOR Mehta Hiren R 1 *, Patel Paresh B 2, Galani Varsha J 2, Patel Kinjal B 3 1 Torrent Research Centre, Near Bhat village, Gandhinagar, Gujarat, India 2 A R Collage of Pharmacy, Vallabh Vidhyanagar, Anand, Gujarat, India 3 K. B. Institute of Pharmaceutical Education and Research Centre, Gandhinagar, Gujarat, India Article Received on:15/02/2011 Revised on:26/03/2011 Approved for publication:15/04/2011 *Hiren Mehta, Torrent Research Centre, Near Bhat village, Gandhinagar , Gujarat, India hirenpharm@rediffmail.com ABSTRACT Venous thromboembolism is a serious illness that affects patient morbidity and mortality and presents a significant management challenge to healthcare providers world-wide. Despite major achievements in the significant reduction of thromboembolic complications, the most common therapies currently used for prevention and treatment of venous thromboembolism heparins and vitamin K antagonists such as warfarin have several limitations. Warfarin sodium is an effective oral anticoagulant drug. However, warfarin has a narrow therapeutic window with significant risks of hemorrhage at therapeutic concentrations. Dosing is difficult and requires frequent monitoring. New oral anticoagulant agents are required to improve current anticoagulant therapy. Furthermore, while warfarin is effective in venous disease, it does not provide more than 60% risk reduction compared with placebo in venous thrombosis prophylaxis and considerably lower risk reduction in terms of arterial thrombosis. Unlike warfarin and heparin, these direct thrombin inhibitors are able to inhibit fibrin-bound thrombin and so produce more effective inhibition of coagulation. Importantly, some members of this class of drugs have been developed for oral administration. Ximelagatran is an oral pro-drug of melagatran, a synthetic small peptidomimetic with direct thrombin inhibitory actions and anticoagulant activity. As an oral agent, ximelagatran has a number of desirable properties including a rapid onset of action, fixed dosing, stable absorption, apparent low potential for medication interactions, and no requirement for monitoring of drug levels or dose adjustment. It has a short plasma elimination half-life of about 4 hours in cases of unexpected hemorrhage or need for reversal. KEY WORDS: Thromboembolism, Anticoagulants, Direct thrombin inhibitors, Ximelagatran. INTRODUCTION Oral anticoagulants have been used in clinical practice for more than 60 years. The most commonly prescribed oral anticoagulant has been warfarin sodium (either Coumadin or Marevan ) or longer-acting coumarin preparations or indanedione derivatives. Warfarin is an effective anticoagulant, but has a narrow therapeutic window with significant risks of hemorrhage at therapeutic drug concentrations. 1 Venous thromboembolism, including deep vein thrombosis and pulmonary embolism, is a serious and potentially fatal condition that places a significant economic burden on healthcare providers. Its annual incidence is approximately 1 in 1000 individuals per year, but this is likely to be an underestimate, because the condition is often asymptomatic, with the first clinical sign being pulmonary embolism, which can be fatal. 2 The risk of developing venous thrombo embolism increases with age, prolonged immobility and major surgery. Therefore, venous thrombo embolism is a particular problem in elderly patients undergoing major orthopaedic surgery. 2,3 Numerous clinical trials have demonstrated that the provision of anticoagulant therapy (oral vitamin K antagonists, parenteral unfractionated heparin [UFH], low molecular- weight heparin [LMWH], or the factor Xa inhibitor fondaparinux) dramatically reduces the postoperative morbidity associated with orthopaedic surgery. 3 The vitamin K antagonists such as warfarin have remained the only oral anticoagulants available since their introduction in Although effective and widely used for a broad range of indications, they have serious limitations. Close monitoring to maintain the international normalized ratio (INR) within a desired range is required to maintain effectiveness and minimize bleeding complications because of the narrow therapeutic range. Also, they have a slow onset of action so therapy must be initiated with a parenteral anticoagulant when a rapid effect is needed. Vitamin K antagonists also have prolonged action after stopping, which creates difficulties in managing bleeding complications or when treatment must be interrupted for invasive procedures. Dosing is complicated by numerous
2 interactions with food and drugs, and marked biological variations in response between patients. 4 Venous thrombi occur as a result of inappropriate plasma coagulation in patients with hypercoagulability or with venous trauma or stasis. Coagulation is dependent on a highly regulated cascade of proteolytic enzymes and cofactors that ultimately leads to the production of an insoluble fibrin network. 2 Two coagulation pathways exist: the intrinsic pathway, which is activated when blood comes into contact with negatively charged surfaces, and the extrinsic pathway, which is activated by the exposure of tissue factor at sites of vascular injury. Both these pathways are linked and converge after the activation of factor X, which then cleaves prothrombin (factor II) to produce thrombin, the final protease in the coagulation cascade. Thrombin cleaves fibrinopeptides A and B from fibrinogen to yield soluble fibrin, which is cross-linked to form insoluble fibrin and a more stable coagulum. 2,4 However, it also has an important effect in feedback amplification of coagulation, as small amounts of thrombin proteolytically activate Factors V and VIII, and this greatly increases their cofactor activities. Thrombin also converts Factor XI to Factor XIa, which activates Factor XIII; this stabilizes fibrin by isopeptide cross-linking. Another important hemostatic effect is proteolytic activation of thrombin-activatable fibrinolysis inhibitor, which inhibits fibrinolysis by cleaving N- terminal lysines from fibrin to limit plasminogen binding. Additionally, thrombin is a potent platelet activator, and it has effects on a variety of vascular cells through activation of specific receptors. Thrombin also has an important anticoagulant effect after binding to the endothelial receptor, thrombomodulin, which enables it to convert Protein C to activated Protein C; this inactivates Factors Va and VIIIa. Therefore, thrombin inhibition may result in a variety of effects including inhibition of coagulation, platelet activation and fibrinolysis. However, it could potentially have a procoagulant effect under some circumstances through reduced formation of activated Protein C, and it may influence vascular responses to injury through blocking cellular effects. 2,4 As discussed earlier, there are several drawbacks to the clinical use of current anticoagulant treatments. In particular, the unpredictable pharmacokinetics of warfarin and heparin and the associated risk of bleeding or under treatment necessitate routine coagulation monitoring. There is, therefore, a clinical need for alternative anticoagulation therapies. Among other properties, the ideal anticoagulant should have a predictable pharmacokinetic profile such that coagulation monitoring is not required. In addition, oral availability is important if new drugs are to be useful as alternatives to warfarin for long-term, outpatient treatment. 5 Thrombin is a particularly attractive target for anticoagulation therapies because of the central part that it plays in the coagulation cascade. Molecules that directly inhibit thrombin have some theoretical advantages over current anticoagulants. For example, neither heparins nor other indirect coagulation inhibitors are active against fibrin bound thrombin. This is important, because fibrin-bound thrombin remains active and promotes continued thrombus growth. Heparin is able to link thrombin to fibrin and so blocks the heparinbinding site on thrombin that is necessary for its interaction with heparin activated antithrombin. Direct thrombin inhibitors, however, have the potential to inhibit fibrin-bound thrombin, as no steric hindrance is present. In addition, direct thrombin inhibitors do not bind to platelet factor 4 (as do heparins) and so do not cause heparin-induced thrombocytopenia. 2 Some other advantages of direct thrombin inhibitors having anticoagulants with improved pharmacological properties, such as suitability for oral administration, a rapid onset of action, and no requirement of anticoagulation monitoring and dose adjustment. 3 INTRODUCTION TO XIMELAGATRAN Ximelagatran (Exanta TM, AstraZeneca) is the first oral direct thrombin inhibitor in advanced clinical development. Based on its promising pharmacological properties, ximelagatran has been the subject of an extensive clinical trial programme, examining its efficacy and safety in several clinical areas for the prevention and treatment of thromboembolic disorders. The clinical trials of ximelagatran for the prevention of VTE following major orthopaedic surgery, in which approximately 60% to 70% of patients received neuraxial anaesthesia has been, investigated both pre-operative and postoperative commencement of anticoagulant dosing. There have been no reports of spinal or epidural haematomas. 3 Ximelagatran is orally active direct thrombin inhibitors. It belongs to ethyl N-[(R)-cyclohexyl-[[(2S)-2-[[4- (hydroxycarbamimidoyl) benzyl]carbamoyl]-1- zetidinyl] carbonyl]methyl] glycinate. Its having molecular formula C 24 H 35 N 5 O 5 and having molecular weight 474 and 429 after conversion into the active metabolite melagatran. 6 MECHANISM OF ACTION After oral administration, ximelagatran is rapidly absorbed and is extensively metabolized to its active form of melagatran via hydrolysis and reduction. Melagatran is a competitive, direct, and reversible inhibitor of clot-bound and free thrombin, which
3 prevents the conversion of fibrinogen to fibrin, thereby inhibiting coagulation (see figure 1). 7 PHARMACODYNAMICS Ximelagatran is an oral prodrug derivative of melagatran, a low-molecular-weight potent direct thrombin inhibitor. 8 Development of the novel, derivatized prodrug approach was essential because melagatran and other active direct thrombin inhibitors exhibit poor intestinal absorption. 9 Ximelagatran undergoes rapid enzymatic conversion to melagatran via 2 intermediates, ethyl-melagatran (from the ethyl ester of melagatran formed by reduction of the hydroxyl group) and hydroxyl-melagatran (the hydroxyamidine of melagatran, formed by hydrolysis of the ethyl group) (see Figure 2). This conversion in vivo probably occurs in several tissues. Enzymatic conversion in vitro occurs in microsomal preparations from the liver, intestinal membrane, and kidney. The highest activity was found in liver mitochondria. Cytochrome P450 (CYP) enzymes are unlikely to be involved in the bioconversion of ximelagatran as no reduction of hydroxylmelagatran was found in preparations of 9 different CYP isoenzymes. The conversion of the intermediates to melagatran occurs rapidly in all ethnic groups including African, Asian, and Caucasian. Hydroxyl-melagatran, as with ximelagatran, is an ineffective thrombin inhibitor (potency ~1% of melagatran) while ethyl-melagatran s anticoagulant activity is the same as melagatran. 1 PHARMACOKINETICS Ximelagatran is an orally active direct thrombin inhibitor. After oral administration, Ximelagatran rapidly converted into its active form melagatran, a potent inhibitor of thrombin that prevents both thrombin activity and generation. 10 Its oral availability is 18% to 25% in its active form, reaching a peak concentration in 1.5 to 2.5 hours. It is only about 15% protein bound, and its halflife is about three hours in healthy patients. 1-2,8-9 However, following oral administration, ximelagatran is rapidly and nearly completely absorbed with a C max of 0.33 hours, and food has little effect on absorption. Ximelagatran is metabolized rapidly with a half-life of unmetabolized ximelagatran of 0.34 hours, and approximately 20% is converted to melagatran with a low interindividual variability in the area under the curve of approximately 20%. Other metabolites include ethylmelagatran and OH-melagatran that form in small amounts and are eliminated rapidly. The t max of melagatran following oral ximelagatran is approximately 2 hours. 1-2,4 Melagatran is primarily excreted in the kidneys (80%), and its half-life is thus prolonged in patients with renal dysfunction. 8 Unlike warfarin and other vitamin K antagonists, ximelagatran has a very wide therapeutic interval that enables it to be administered safely across a wide range of doses without an increased risk of bleeding. It has a predictable and stable pharmacokinetic profile and is unaffected by patient body weight, age, sex, or ethnic origin. 1 The metabolism of melagatran is independent of the hepatic cytochrome P450 system, leading to a low potential for drug interactions. Unlike warfarin, ximelagatran has no known food interactions and does not require coagulation monitoring or dose adjustment. Recent studies have also demonstrated that the pharmacokinetics and pharmacodynamics of oral ximelagatran are unaffected by alcohol or aspirin. 7 Pharmacokinetic Study One study was conducted in healthy volunteers to check the effect of different antibiotics on the pharmacokinetic and pharmacodynamic of the melagatran. To check the effects of amoxicillin, doxycycline, ciprofloxacin, azithromycin, and cefuroxime on the pharmacokinetics and pharmacodynamics of melagatran, the active form of the oral direct thrombin inhibitor ximelagatran, which is a substrate for the P-glycoprotein pump (Pgp) transporter but is not metabolized by the cytochrome P450 (CYP450) enzyme system? Author included total five parallel groups of 16 healthy volunteers received two sequential treatments. The first treatment was a single 36-mg dose of ximelagatran. During the second treatment period, one of the above antibiotics was given on days 1 5 after a washout of at least 2 days. A single 36-mg oral dose of ximelagatran was given on the mornings of days 1 and 5 of the second treatment period. There was no pharmacokinetic interactions were detected between ximelagatran and amoxicillin, doxycycline, or ciprofloxacin as the least-squares geometric mean treatment ratio of ximelagatran with-to-without antibiotic fell within the intervals of for the area under the curve (AUC) and for C max. After coadministration with azithromycin, the least square mean ratio with-to-without antibiotic for AUC of melagatran was 1.60 (90% CI, ) on day 1 and 1.41 (90% CI, ) on day 5. For melagatran C max, the corresponding ratios were 1.63 (90% CI, ) and 1.40 (90% CI, ). After coadministration with cefuroxime, the ratios were 1.23 (90% CI, ) and 1.16 (90% CI, ) for AUC and 1.33 (90% CI, ) and 1.19 (90%CI, ) for C max of melagatran. Co-administration with the antibiotics did not change mean time to C max, half-life, or renal clearance of melagatran. The melagatran plasma concentration-response relationship for activated partial thromboplastin time (APTT) prolongation was not
4 altered by any of the studied antibiotics, but the increased plasma concentrations of melagatran after coadministration of ximelagatran with azithromycin resulted in a minor increase in the mean maximum APTT of about 15%. 11 Authors concluded that the pharmacokinetics of ximelagatran was not affected by amoxicillin, doxycycline, or ciprofloxacin. Melagatran exposure was increased when ximelagatran was co-administered with azithromycin and, to a lesser extent, with cefuroxime. APTT was not significantly altered by any of the antibiotics. 11 In another study was also conducted for doseoptimization, study18 was conducted to determine the superiority and safety of ximelagatran, at doses of 24 mg or 36 mg twice daily, compared with warfarin. That study showed a significant reduction in the prevalence of deep-vein thrombosis, pulmonary embolism, and/or death with no increase in major bleeding with a dose of 36 mg of ximelagatran twice daily compared with adjusted-dose warfarin (p = 0.003). 10 CLINICAL TRIALS The METHRO Trial METHRO I (Melagatran as prophylaxis of thrombosis in orthopaedic surgery), a dose-ranging pilot study, and METHRO II, a phase II study, have found an overall dose-dependent decrease in venographic total and proximal DVT and/or symptomatic PE with increasing doses of ximelagatran melagatran. The METHRO III study compared the use of ximelagatran melagatran with enoxaparin in a randomized study of 2788 patients undergoing major orthopedic surgery. Doses of enoxaparin were 40 mg once daily commencing 12 hours preoperatively then daily for 1 10 days compared with melagatran 3 mg subcutaneously 4 12 hours postoperatively, then ximelagatran 24 mg orally twice daily commencing on day 1 or 2 postoperatively. Over all conclude that the venous thromboembolism occurred in 355/1146 (31.0%) and 306/1122 (27.3%) patients in the ximelagatran and enoxaparin group, respectively, so a difference in risk of 3.7% in favour of enoxaparin (p = 0.053). Bleeding was comparable between the two groups. 12 The EXPRESS Trial The Extended Prophylaxis Evaluation Surgery Study (EXPRESS), a randomized, double-blind, parallel group, placebo controlled trial, consisted of two treatment arms. The study was conducted to evaluate the safety and efficacy of ximelagatran, compared with enoxaparin (Lovenox, Aventis), in preventing VTE after total hip and knee replacement surgery. Patients in one arm of the trial received melagatran 2 mg subcutaneously immediately before surgery and then 3 mg subcutaneously the night after surgery (n = 1,377). The patients continued therapy with oral ximelagatran 24 mg twice daily. Patients in the second arm received enoxaparin 40 mg subcutaneously once daily starting the night before surgery (n = 1,387). Treatment of patients in both arms continued for eight to 11 days. The rate of deep vein thrombosis (DVT) and pulmonary embolism (PE). The overall rate of DVT and PE in the ximelagatran patients (2.3%) was lower than that in the enoxaparin group (6.3%). The total rate of VTE was lower in the ximelagatran arm (20.3%) than in the enoxaparin arm (26.6%). It is interesting that no differences in clinically significant bleeding were reported among the two groups. However, bleeding events were higher in the patients in the ximelagatran arm (3.3%) than those in the enoxaparin arm (1.2%). The authors of the study concluded that subcutaneous melagatran, in combination with oral ximelagatran, was more effective in preventing VTE than enoxaparin alone in patients with total hip or total knee replacement surgery. 1,8 The EXULT Trial The Exanta Used to Lessen Thrombosis (EXULT) study was a multicenter, randomized, double-blind trial consisting of three treatment arms. A total of 2,301 patients underwent total knee replacement surgery. In one group, ximelagatran 24 mg was given twice daily; the patients in the second arm received ximelagatran 36 mg twice daily. Both dosages were initiated on the morning after surgery. A third study arm consisted of patients who received warfarin, initiated during the evening of the day of surgery. The doses in the warfarin arm were titrated to a goal International Normalized Ratio (INR) of 2 to 3. All treatments in each study arm were continued for seven to 12 days. The study endpoints evaluated the incidence of VTE, all causes of mortality, and bleeding. Combined incidences of DVT and PE with all causes of mortality showed that ximelagatran 36 mg twice daily (20.3%) was more effective than warfarin (27.6%). No differences were reported between endpoints that were independently assessed among the three study arms. Bleeding was evaluated, and no major differences were reported among the groups. The bleeding incidence was noted to be associated with the dosage: ximelagatran 24 mg (4.8%), ximelagatran 36 mg (5.3%), and warfarin (4.5%). In conclusion, ximelagatran showed superior effects over traditional warfarin therapy in preventing VTE after total knee replacement. 4,8
5 The THRIVE III Trial The Oral Direct Thrombin Inhibitor, ximelagatran, for Venous Thromboembolism (THRIVE) study, a multicenter, double-blind trial, included 1,233 patients with documented DVT and PE and appropriate anticoagulation therapy for six months duration. This study evaluated the efficacy and safety of ximelagatran in preventing secondary events associated with VTE. Inclusion criteria were based on the receipt of either placebo or ximelagatran 24 mg twice daily for 18 months after the initial six month anticoagulation period. The primary endpoint was the evaluation of any recurrences of VTE. Patients receiving ximelagatran experienced a significantly lower incidence of VTE recurrence than did patients receiving placebo. Bleeding, described as a major hemorrhage, was not significant between study groups. Overall, ximelagatran was safe and effective in preventing the secondary events of VTE. 13 The SPORTIF III and V Trials The Stroke Prevention by Oral Thrombin Inhibitor in Atrial Fibrillation III (SPORTIF III) study was a randomized, open-label, parallel-group trial with blinded event assessment. The trial included 3,407 patients at 259 study centers in 23 countries. SPORTIF V was also a randomized, open-label, parallelgroup trial with a similar design in utilizing double-blind treatment investigation. This trial involved 3,922 patients in 409 North American study centers. For both studies, the primary endpoint was the incidence of all strokes and systemic embolic events among the ximelagatran and warfarin treatment groups. Secondary endpoints included stroke, embolism, myocardial infarction, ischemic stroke, transient ischemic attack (TIA), bleeding, treatment discontinuation, and death. In an intent-to-treat analysis of SPORTIF III, 3,407 patients received ximelagatran 36 mg twice daily and 1,703 received warfarin with an INR of 2 3. A mean follow-up period of 17.4 months demonstrated 40 documented cases of increased risk of stroke and systemic embolism with ximelagatran and 56 cases of increased risk with warfarin. The data confirmed the non-inferiority of ximelagatran over warfarin. In SPORTIF V, patients were followed for a mean of 20 months. The data from this trial also verified the noninferiority of ximelagatran over warfarin. Bleeding was observed in both treatment groups, and the incidence was higher in the ximelagatran group. Patients receiving ximelagatran demonstrated an increase in alanine aminotransferase (ALT) levels greater than three times the upper limits of normal (ULN) (at 6%) compared with the warfarin patients (at %). Liver enzyme concentrations were elevated within the first six months of therapy and decreased with or without drug discontinuation. Long-term safety over 35 days and liver enzyme levels were also evaluated. Liver enzymes of ALT were more than three times the ULN with ximelagatran in contrast to comparator agents with more than twice the ULN of bilirubin. Of nine patients who died, three were in the ximelagatran group. 1,4,8,9 ADVERSE EFFECTS The most common and expected adverse drug event (ADE) associated with ximelagatran is bleeding. Clinical trials have shown that the risk of bleeding associated with ximelagatran is comparable to that of traditional anticoagulants. However, the incidence is reported to be less than with other conventional therapies. Elevations of liver enzymes have also been noted in clinical trials. Within the first two to six months of treatment with ximelagatran, up to 6% of patients had elevated serum ALT levels as high as three times the ULN. However, these levels returned to normal in most of the patients whether or not they continued therapy. Because of the uncertainty of the significance of liver enzyme elevations, authorities have recommended that liver function tests, in particular ALT testing, be performed before the initiation of ximelagatran and every two months thereafter for at least the first six months, then periodically. Recommendations have been implemented to monitor patients clinically, and patients are urged to adhere to protocols in order to prevent possible ADEs. 1,4,8-9,12,13 CONTRAINDICATION Ximelagatran is contraindicated in patients with a history of hypersensitivity to ximelagatran, melagatran, or any of its components. The use of ximelagatran is prohibited in patients with any type of severe, active bleeding. 12 TOLERABILITY Aside from hemorrhage, ximelagatran melagatran has been remarkably free of significant adverse toxicities. Most concern has been placed on the dose-dependent increase in liver enzymes, predominantly elevated ALT, which is usually unaccompanied by clinical sequelae. This has been found in 6% 12% of patients in clinical studies with the biochemical abnormality typically occurring in 1 6 months of therapy, rarely developing after 6 months of treatment. In all clinical studies, patients required monthly screening of liver biochemistry in the first 6 months. The study medication was ceased if ALT exceeded 5 times ULN at any time. If ALT was 3 5 times ULN, more frequent monitoring was performed with 6% of patients overall of increased ALT to > 3 times ULN. Only about one-half of patients discontinued the study as a result of this. With time, the ALT tends to
6 decrease whether or not the drug is discontinued although a small percentage (data unpublished) still has persistent elevation. However, a small percentage of patients became jaundiced (0.4% in the ESTEEM study) or developed symptoms possibly attributable to liver dysfunction. 1 In the METHRO III study, 2 patients suffered MI during the treatment period and 1 succumbed to cardiogenic shock in the follow up period. No such event occurred in the control arm. Cardiomyopathy, ischemic heart disease, and congestive heart failure were causes of 3 deaths in the ximelagatran group in the METHRO II studies. No comments were made by the authors as to potential reasons for these adverse events or their significance. Similar findings regarding MI were not observed in the other clinical studies of ximelagatran. 12 CONCLUSION Venous thromboembolism is a serious condition that requires effective and safe anticoagulation therapy. The current modalities for its prevention and treatment have many limitations, particularly relating to unpredictable pharmacokinetics and pharmacodynamics. Thrombin is a key enzyme in the coagulation cascade and as such is an attractive target for novel anticoagulant therapies. A new class of drugs has been developed that produces direct inhibition of thrombin. Ximelagatran-the first oral direct thrombin inhibitor, is at the most advanced stage of development and its efficacy and safety in venous thromboembolism have been demonstrated in clinical trials. It has a reproducible pharmacokinetic and pharmacodynamic profile, and thus fixed doses can be administered without the need for coagulation monitoring. The characteristics of ximelagatran have led to its investigation in the prevention of venous thromboembolism in patients undergoing major elective orthopaedic surgery, the treatment and long-term secondary prevention of venous thromboembolism, prevention of stroke in patients with atrial fibrillation and prevention of major cardiovascular events after acute myocardial infarction. The new class of direct thrombin inhibitors, particularly orally available, has the potential to achieve considerable improvement in the prevention and treatment of venous thromboembolism. REFERENCES 1. Ho SJ, Brighton TA. Ximelagatran: direct thrombin inhibitor. Vascular Health and Risk Management 2006;2(1): Haas S. Oral Direct Thrombin Inhibition: an Effective and Novel Approach for Venous Thromboembolism. Drugs 2004; 64(1): Rosencher N. Ximelagatran, a new oral direct thrombin inhibitor, for the prevention of venous thromboembolic events in major elective orthopaedic surgery. Efficacy, safety and anaesthetic considerations. Anaesthesia, 2004;59: Francis CW. Ximelagatran: a new oral anticoagulant. Best Practice & Research Clinical Haematology, 2004;17(1): Weitz JI, Crowther MA. New anticoagulants: current status and future potential. Am J Cardiovasc Drugs 2003; 3 (Pt 3): Ximelagatran: Defination. (link: defin ition/ximelagatran) 7. Boosa CJ,Hinton A, Lip GYH. Ximelagatran: A clinical perspective. European Journal of Internal Medicine, 2005; 16: Hilas O, Marzella N. Ximelagatran (Exanta ): A Product Review and Update. February 2005;30(2): Ximelagatran: An oral direct thrombin inhibitor. Indian J Pharmacol, April 2005;37(2): Colwell CL, et al. Oral Direct Thrombin Inhibitor Ximelagatran Compared with Warfarin for the Prevention of Venous Thromboembolism After Total Knee Arthroplasty. The Journal Of Bone & Joint Surgery, October 2005;87-A(10): Dorani H,Schützer KM. et al. Pharmacokinetics and pharmacodynamics of the oral direct thrombin inhibitor ximelagatran co-administered with different classes of antibiotics in healthy volunteers. Eur J Clin Pharmacol, 2007;63: Eriksson BI, Agnelli G et al. Direct thrombin inhibitor melagatran followed by oral ximelagatran in comparison with enoxaparin for prevention of venous thromboembolism after total hip or knee replacement. Thromb Haemost, 2003 Feb;89(2): Brighton TA. The direct thrombin inhibitor melagatran/ximelagatran. Med J Aust 2004;181(8):
7 Figure 1: Mechanism of Action of Ximelagatran Figure 2: Chemical Structure of Ximelagatran and Melagatran
Scottish Medicines Consortium
 Scottish Medicines Consortium fondaparinux, 2.5mg/0.5ml, solution for injection (Arixtra ) No. (287/06) GlaxoSmithKline 7 July 2006 The Scottish Medicines Consortium has completed its assessment of the
Scottish Medicines Consortium fondaparinux, 2.5mg/0.5ml, solution for injection (Arixtra ) No. (287/06) GlaxoSmithKline 7 July 2006 The Scottish Medicines Consortium has completed its assessment of the
Continuing Education for Pharmacists
 Continuing Education for Pharmacists Oral anticoagulation without protimes: A review of two emerging agents that may come to market. Lindsay Davis, Pharm.D. (Acute Care Pharmacy Resident, Phoenix VA Medical
Continuing Education for Pharmacists Oral anticoagulation without protimes: A review of two emerging agents that may come to market. Lindsay Davis, Pharm.D. (Acute Care Pharmacy Resident, Phoenix VA Medical
Bevyxxa (betrixaban) NEW PRODUCT SLIDESHOW
 Bevyxxa (betrixaban) NEW PRODUCT SLIDESHOW Introduction Brand name: Bevyxxa Generic name: Betrixaban Pharmacological class: Factor Xa inhibitor Strength and Formulation: 40mg, 80mg; caps Manufacturer:
Bevyxxa (betrixaban) NEW PRODUCT SLIDESHOW Introduction Brand name: Bevyxxa Generic name: Betrixaban Pharmacological class: Factor Xa inhibitor Strength and Formulation: 40mg, 80mg; caps Manufacturer:
Bayer R&D Investor Day 2005
 Science For A Better Life HealthCare Bayer R&D Investor 25 December 8, 25 London Bayer R&D Investor 25 BAY 59-7939: A Novel, ral, Direct Factor Xa Inhibitor Frank Misselwitz Head of Therapeutic Area Cardiovascular,
Science For A Better Life HealthCare Bayer R&D Investor 25 December 8, 25 London Bayer R&D Investor 25 BAY 59-7939: A Novel, ral, Direct Factor Xa Inhibitor Frank Misselwitz Head of Therapeutic Area Cardiovascular,
LVHN Scholarly Works. Lehigh Valley Health Network. Joseph G. Ottinger RPh, MS, MBA, BCPS Lehigh Valley Health Network,
 Lehigh Valley Health Network LVHN Scholarly Works Department of Pharmacy Retrospective Evaluation of Delayed Administration of Fondaparinux in Providing Comparable Safety and Efficacy Outcomes in Patients
Lehigh Valley Health Network LVHN Scholarly Works Department of Pharmacy Retrospective Evaluation of Delayed Administration of Fondaparinux in Providing Comparable Safety and Efficacy Outcomes in Patients
a unit of Dr Bharat S Mody Director Chief Arthroplasty Surgeon Centre for Knee & Hip Surgery Dr Pankaj Patni Orthopaedic Surgeon Dr Sunil Dewangan
 Centre for Knee & Hip Surgery Arthroscopy a unit of Arthroplasty Dr Bharat S Mody Director Chief Arthroplasty Surgeon Dr Sunil Dewangan Dr Prakash Tekwani Dr Rahul Khanna Dr Pankaj Patni Orthopaedic Surgeon
Centre for Knee & Hip Surgery Arthroscopy a unit of Arthroplasty Dr Bharat S Mody Director Chief Arthroplasty Surgeon Dr Sunil Dewangan Dr Prakash Tekwani Dr Rahul Khanna Dr Pankaj Patni Orthopaedic Surgeon
SYNOPSIS. Clinical Study Report for Study CV Individual Study Table Referring to the Dossier
 Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Individual Study Table Referring to the Dossier (For National Authority Use Only) Name of Active Ingredient: SYNOPSIS Clinical Study
Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Individual Study Table Referring to the Dossier (For National Authority Use Only) Name of Active Ingredient: SYNOPSIS Clinical Study
ANTICOAGULANT THERAPY ANTICOAGULANT THERAPY REVISITED Thrombosis is a complication of underaggressive anticoagulant therapy
 ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
Omar A. Elkashef, MD
 DVT Prophylaxis in Orthopedic Surgery By Omar A. Elkashef, MD Kasr Al- aini About VTE Venous thromboembolism encompasses deep vein thrombosis (DVT) and pulmonary embolism VTE is common and PE is a potentially
DVT Prophylaxis in Orthopedic Surgery By Omar A. Elkashef, MD Kasr Al- aini About VTE Venous thromboembolism encompasses deep vein thrombosis (DVT) and pulmonary embolism VTE is common and PE is a potentially
Clinical Study Synopsis
 Clinical Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website or on the website www.clinicalstudyresults.org hosted by the Pharmaceutical Research and
Clinical Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website or on the website www.clinicalstudyresults.org hosted by the Pharmaceutical Research and
The Lancet Publishes Results from the Landmark Phase III Rivaroxaban Study RECORD2
 News Release Bayer HealthCare AG Corporate Communications 51368 Leverkusen Germany Phone +49 214 30 1 www.news.bayer.com Venous Blood Clot Prevention after Hip Replacement Surgery: The Lancet Publishes
News Release Bayer HealthCare AG Corporate Communications 51368 Leverkusen Germany Phone +49 214 30 1 www.news.bayer.com Venous Blood Clot Prevention after Hip Replacement Surgery: The Lancet Publishes
LOW MOLECULAR WEIGHT HEPARIN THE STANDARD VALUE
 LOW MOLECULAR WEIGHT HEPARIN THE STANDARD VALUE ANASTASIOS V. KOROMPILIAS, MD ORTHOPAEDIC DEPARTMENT, MEDICAL SCHOOL UNIVERSITY OF IOANNINA, IOANNINA, GREECE MAJOR ORTHOPAEDIC SURGERY POSTOPERATIVE CLASSIFIED
LOW MOLECULAR WEIGHT HEPARIN THE STANDARD VALUE ANASTASIOS V. KOROMPILIAS, MD ORTHOPAEDIC DEPARTMENT, MEDICAL SCHOOL UNIVERSITY OF IOANNINA, IOANNINA, GREECE MAJOR ORTHOPAEDIC SURGERY POSTOPERATIVE CLASSIFIED
Lina Al-Lawama. Rama Al-Ashqar. Malik Al-Zohlof
 2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
Clinical Study Synopsis
 Clinical Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website or on the website www.clinicalstudyresults.org hosted by the Pharmaceutical Research and
Clinical Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website or on the website www.clinicalstudyresults.org hosted by the Pharmaceutical Research and
Session 1 Topics. Vascular Phase of Hemostasis. Coagulation Pathway. Action of Unfractionated Heparin. Laboratory Monitoring of Anticoagulant Therapy
 ~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
Managing the Risks Associated with Anticoagulant Therapy. Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde
 Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Direct anticoagulation therapy
 Direct anticoagulation therapy Pan-Arab Meeting & Saudi Society of Hematology Dr Ihab Alhemaidi MBBS MRCP(Lond UK) FRCPath. Fellow of the Royal Society of Medicine Consultant Adult hematology/bmt Section
Direct anticoagulation therapy Pan-Arab Meeting & Saudi Society of Hematology Dr Ihab Alhemaidi MBBS MRCP(Lond UK) FRCPath. Fellow of the Royal Society of Medicine Consultant Adult hematology/bmt Section
UW Medicine Alternative Monitoring for Antithrombotic Agents
 Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
The novel anticoagulants: entering a new era. BOUNAMEAUX, Henri. Abstract
 Article The novel anticoagulants: entering a new era BOUNAMEAUX, Henri Abstract During the past five decades, anticoagulant therapy has consisted of rapidly acting parenteral drugs (unfractionated heparin
Article The novel anticoagulants: entering a new era BOUNAMEAUX, Henri Abstract During the past five decades, anticoagulant therapy has consisted of rapidly acting parenteral drugs (unfractionated heparin
Pharmacology Lecture 5. Anticoagulants
 Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Hemostasis/Thrombosis IV
 Hemostasis/Thrombosis IV Antithrombotic Therapy Antithrombotic Therapy Mainstay of battle against thromboembolic disease Hot area of new drug research Cannot inhibit clot formation without increased risk
Hemostasis/Thrombosis IV Antithrombotic Therapy Antithrombotic Therapy Mainstay of battle against thromboembolic disease Hot area of new drug research Cannot inhibit clot formation without increased risk
DOACs: When and how to measure their anticoagulant effect
 DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
New Anticoagulants. Kenneth A. Bauer
 New Anticoagulants Kenneth A. Bauer Traditional anticoagulant drugs, including unfractionated heparin and warfarin, have several limitations. New anticoagulants have been developed that target a single
New Anticoagulants Kenneth A. Bauer Traditional anticoagulant drugs, including unfractionated heparin and warfarin, have several limitations. New anticoagulants have been developed that target a single
ISIS PHARMACEUTICALS. ISIS-FXI Rx Program Update. Webcast December 8, 2014
 ISIS PHARMACEUTICALS ISIS-FXI Rx Program Update Webcast December 8, 2014 Introduction Stan Crooke, M.D., Ph.D. CEO and Chairman, Isis Pharmaceuticals 2 Forward Looking Language Statement This presentation
ISIS PHARMACEUTICALS ISIS-FXI Rx Program Update Webcast December 8, 2014 Introduction Stan Crooke, M.D., Ph.D. CEO and Chairman, Isis Pharmaceuticals 2 Forward Looking Language Statement This presentation
Bivalirudin (Angiomax ) vs. Heparin during Peripheral Vascular Interventions: Which is Better and How to Decide?
 Bivalirudin (Angiomax ) vs. Heparin during Peripheral Vascular Interventions: Which is Better and How to Decide? Vinod Nair MD FACC FSCAI Cardiovascular Ins6tute of the South, Houma Financial Disclosure:
Bivalirudin (Angiomax ) vs. Heparin during Peripheral Vascular Interventions: Which is Better and How to Decide? Vinod Nair MD FACC FSCAI Cardiovascular Ins6tute of the South, Houma Financial Disclosure:
New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D.
 New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D. Professor of Cardiovascular Medicine University of Maryland School of Medicine Copyright A.P. Wheeler 2009
New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D. Professor of Cardiovascular Medicine University of Maryland School of Medicine Copyright A.P. Wheeler 2009
New Anticoagulants Linda Liu, M.D.
 Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba
 VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba OVERVIEW Biochemistry of coagulation Pathogenesis of VTE
VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba OVERVIEW Biochemistry of coagulation Pathogenesis of VTE
ANTICOAGULANT THERAPY ANTICOAGULANT THERAPY REVISITED 2005
 ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED Thrombosis is a complication of underaggressive anticoagulant therapy ANTICOAGULANT THERAPY.
 ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY Goals of Therapy PREVENTION OF THROMBOEMBOLISM!!! Stop propagation
ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY Goals of Therapy PREVENTION OF THROMBOEMBOLISM!!! Stop propagation
3 : 34. Pankaj Manoria, P C Manoria, Bhopal
 3 : 34 Newer Antithrombins and anticoagulants Introduction Thrombosis is a leading cause of morbidity and mortality but for decades, anticoagulant therapy has usually consisted of unfractionate heparin
3 : 34 Newer Antithrombins and anticoagulants Introduction Thrombosis is a leading cause of morbidity and mortality but for decades, anticoagulant therapy has usually consisted of unfractionate heparin
Anticoagulation in VTE The Haematologist s Perspective. Dr. M.D. Maina FRCP Edin.
 Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Update on the Direct Oral Anticoagulants (DOACs)
 Update on the Direct Oral Anticoagulants (DOACs) J. Randle Adair DO, PhD Internal Medicine New Mexico Cancer Center & Co-Chair, Anticoagulation Subcommittee Presbyterian Healthcare Services (PHS) Attending,
Update on the Direct Oral Anticoagulants (DOACs) J. Randle Adair DO, PhD Internal Medicine New Mexico Cancer Center & Co-Chair, Anticoagulation Subcommittee Presbyterian Healthcare Services (PHS) Attending,
iccnet CHSA Clinical Protocol - HEPARIN
 Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
Novel Anti-coagulant Agents. David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan
 Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Managing Coagulation Abnormalities Linda Liu, M.D.
 Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 07.01.18 Last Review Date: 02.18 Line of Business: Oregon Health Plan Coding Implications Revision Log See Important Reminder at
Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 07.01.18 Last Review Date: 02.18 Line of Business: Oregon Health Plan Coding Implications Revision Log See Important Reminder at
NEW ORAL ANTICOAGULANTS FOR VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE FOOT AND ANKLE
 NEW ORAL ANTICOAGULANTS FOR VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE FOOT AND ANKLE Matthew Q. McCammon, DPM INTRODUCTION Venous thromboembolism (VTE) is a common cause of morbidity and mortality. Each
NEW ORAL ANTICOAGULANTS FOR VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE FOOT AND ANKLE Matthew Q. McCammon, DPM INTRODUCTION Venous thromboembolism (VTE) is a common cause of morbidity and mortality. Each
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Fragmin) Reference Number: CP.PHAR.225 Effective Date: 05.01.16 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Coding Implications Revision Log See Important Reminder
Clinical Policy: (Fragmin) Reference Number: CP.PHAR.225 Effective Date: 05.01.16 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Coding Implications Revision Log See Important Reminder
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Commercial, HIM-Medical Benefit, Medicaid Coding Implications Revision Log See
Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Commercial, HIM-Medical Benefit, Medicaid Coding Implications Revision Log See
Drugs used in Thromboembolic Disease. Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014
 Drugs used in Thromboembolic Disease Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014 Drugs used in Thromboembolic Disease Anticoagulants: Heparin. Oral anticoagulants.
Drugs used in Thromboembolic Disease Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014 Drugs used in Thromboembolic Disease Anticoagulants: Heparin. Oral anticoagulants.
DRUGDEX DRUG EVALUATIONS. This volume has expired. Product will stop functioning in 13 days. Install the current volume now.
 DRUGDEX DRUG EVALUATIONS This volume has expired. Product will stop functioning in 13 days. Install the current volume now. CLINICAL APPLICATIONS ENOXAPARIN COMPARATIVE EFFICACY / EVALUATION WITH OTHER
DRUGDEX DRUG EVALUATIONS This volume has expired. Product will stop functioning in 13 days. Install the current volume now. CLINICAL APPLICATIONS ENOXAPARIN COMPARATIVE EFFICACY / EVALUATION WITH OTHER
Anticoagulant therapy has historically consisted. A pharmacologic overview of current and emerging anticoagulants
 A pharmacologic overview of current and emerging anticoagulants EDITH A. NUTESCU, PHARMD; NANCY L. SHAPIRO, PHARMD; AIMEE CHEVALIER, PHARMD; AND ALPESH N. AMIN, MD, MBA ABSTRACT For over 50 years, anticoagulant
A pharmacologic overview of current and emerging anticoagulants EDITH A. NUTESCU, PHARMD; NANCY L. SHAPIRO, PHARMD; AIMEE CHEVALIER, PHARMD; AND ALPESH N. AMIN, MD, MBA ABSTRACT For over 50 years, anticoagulant
Scottish Medicines Consortium
 Scottish Medicines Consortium fondaparinux sodium, 2.5mg/0.5ml solution for injection, pre-filled syringe (Arixtra ) No. (420/07) GlaxoSmithKline 09 November 2007 The Scottish Medicines Consortium has
Scottish Medicines Consortium fondaparinux sodium, 2.5mg/0.5ml solution for injection, pre-filled syringe (Arixtra ) No. (420/07) GlaxoSmithKline 09 November 2007 The Scottish Medicines Consortium has
Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity
 Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity Abhishek Gulati What is enoxaparin? Low molecular weight heparin anticoagulant Used to minimise the
Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity Abhishek Gulati What is enoxaparin? Low molecular weight heparin anticoagulant Used to minimise the
Local vasoconstriction. is due to local spasm of the smooth muscle (symp. reflex) can be maintained by platelet vasoconstrictors
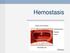 Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 18 January 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 January 2012 ELIQUIS 2.5 mg, film-coated tablets B/10 (CIP code: 419 454-4) B/20 (CIP code: 419 455-0) B/60 (CIP
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 January 2012 ELIQUIS 2.5 mg, film-coated tablets B/10 (CIP code: 419 454-4) B/20 (CIP code: 419 455-0) B/60 (CIP
Analysis of the Anticoagulant Market
 MEDICAL DEVICES PHARMACEUTICALS CHEMICALS FOOD & BEVERAGE ELECTRONICS Analysis of the Anticoagulant Market VPG Publications, Consulting, Clients www.vpgcorp.com VPG Market Research Reports www.vpgmarketresearch.com
MEDICAL DEVICES PHARMACEUTICALS CHEMICALS FOOD & BEVERAGE ELECTRONICS Analysis of the Anticoagulant Market VPG Publications, Consulting, Clients www.vpgcorp.com VPG Market Research Reports www.vpgmarketresearch.com
Physician Orders - Adult
 Physician Orders - Adult attach patient label here Title: Direct Thrombin Inhibitor (DTI) Protocol Orders Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy
Physician Orders - Adult attach patient label here Title: Direct Thrombin Inhibitor (DTI) Protocol Orders Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides.
 These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
Venous thromboembolism (VTE) Can Biomarkers Help to Guide Duration of Therapy After VTE? New Chest Guidelines 2016
 Venous thromboembolism (VTE) Can Biomarkers Help to Guide Duration of Therapy After VTE? Marlene Grenon, MD Associate Professor of Surgery University of California San Francisco UCSF Vascular Surgery Symposium
Venous thromboembolism (VTE) Can Biomarkers Help to Guide Duration of Therapy After VTE? Marlene Grenon, MD Associate Professor of Surgery University of California San Francisco UCSF Vascular Surgery Symposium
This paper reviews the potential cost-effectiveness
 n reports n Cost-Effectiveness of Rivaroxaban After Total Hip or Total Knee Arthroplasty Louis M. Kwong, MD, FACS Abstract Venous thromboembolism (VTE) following joint replacement surgery represents an
n reports n Cost-Effectiveness of Rivaroxaban After Total Hip or Total Knee Arthroplasty Louis M. Kwong, MD, FACS Abstract Venous thromboembolism (VTE) following joint replacement surgery represents an
Oral direct thrombin inhibitors in clinical development
 Journal of Internal Medicine 2003; 254: 322 334 MIISYMPOSIUM Oral direct thrombin inhibitors in clinical development D. GUSTAFSSO From AstraZeneca R&D, Mölndal, Sweden Abstract. Gustafsson D (AstraZeneca
Journal of Internal Medicine 2003; 254: 322 334 MIISYMPOSIUM Oral direct thrombin inhibitors in clinical development D. GUSTAFSSO From AstraZeneca R&D, Mölndal, Sweden Abstract. Gustafsson D (AstraZeneca
New anticoagulants for the prevention and treatment of venous thromboembolism
 REVIEW New anticoagulants for the prevention and treatment of venous thromboembolism Simon J McRae Jeffrey S Ginsberg Department of Medicine, McMaster University, Hamilton, ON, Canada Abstract: Anticoagulant
REVIEW New anticoagulants for the prevention and treatment of venous thromboembolism Simon J McRae Jeffrey S Ginsberg Department of Medicine, McMaster University, Hamilton, ON, Canada Abstract: Anticoagulant
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency London, 19 March 2009 EMEA/CHMP/BMWP/118264/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON NON-CLINICAL AND CLINICAL DEVELOPMENT OF SIMILAR BIOLOGICAL
European Medicines Agency London, 19 March 2009 EMEA/CHMP/BMWP/118264/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON NON-CLINICAL AND CLINICAL DEVELOPMENT OF SIMILAR BIOLOGICAL
CDEC FINAL RECOMMENDATION
 CDEC FINAL RECOMMENDATION APIXABAN (Eliquis Bristol-Myers Squibb Canada and Pfizer Canada) Indication: Venous Thromboembolic Events Recommendation: The Canadian Drug Expert Committee (CDEC) recommends
CDEC FINAL RECOMMENDATION APIXABAN (Eliquis Bristol-Myers Squibb Canada and Pfizer Canada) Indication: Venous Thromboembolic Events Recommendation: The Canadian Drug Expert Committee (CDEC) recommends
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) Draft
 European Medicines Agency Pre-authorisation Evaluation of Medicines for Human Use London, 24 April 2008 EMEA/CHMP/BMWP/118264/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) Draft GUIDELINE
European Medicines Agency Pre-authorisation Evaluation of Medicines for Human Use London, 24 April 2008 EMEA/CHMP/BMWP/118264/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) Draft GUIDELINE
A Pilot Study Comparing Hospital Readmission Rates In Patients Receiving Rivaroxaban or Enoxaparin After Orthopedic Surgery
 A Pilot Study Comparing Hospital Readmission Rates In Patients Receiving Rivaroxaban or Enoxaparin After Orthopedic Surgery Melissa A. Herschman, PharmD, BCPS; Frank S. Rigelsky, PharmD, BCPS; and Sandra
A Pilot Study Comparing Hospital Readmission Rates In Patients Receiving Rivaroxaban or Enoxaparin After Orthopedic Surgery Melissa A. Herschman, PharmD, BCPS; Frank S. Rigelsky, PharmD, BCPS; and Sandra
Antithrombotic Therapies: Parenteral Agents
 Antithrombotic Therapies: Parenteral Agents Christine A. Sorkness, Pharm.D. Professor of Pharmacy & Medicine (CHS) UW School of Pharmacy Clinical Pharmacist, Anticoagulation Clinic, Wm S. Middleton VA
Antithrombotic Therapies: Parenteral Agents Christine A. Sorkness, Pharm.D. Professor of Pharmacy & Medicine (CHS) UW School of Pharmacy Clinical Pharmacist, Anticoagulation Clinic, Wm S. Middleton VA
Timing the First Postoperative Dose of Anticoagulants Lessons Learned From Clinical Trials
 [ Commentary ] Timing the First Postoperative Dose of Anticoagulants Lessons Learned From Clinical Trials Jeremy S. Paikin, MD ; Jack Hirsh, MD ; Noel C. Chan, MBBS ; Jeffrey S. Ginsberg, MD ; Jeffrey
[ Commentary ] Timing the First Postoperative Dose of Anticoagulants Lessons Learned From Clinical Trials Jeremy S. Paikin, MD ; Jack Hirsh, MD ; Noel C. Chan, MBBS ; Jeffrey S. Ginsberg, MD ; Jeffrey
Challenges of VTE Prophylaxis in. Orthopaedics. Prevalence of DVT in Orthopaedic Surgery Without Prophylaxis
 Grand Rounds Scripps Green Hospital May 5, 2010 Challenges of VTE Prophylaxis in Orthopaedics C. W. Colwell, Jr., M.D. At Scripps Clinic Challenges of VTE Prophylaxis in Orthopaedics I have a potential
Grand Rounds Scripps Green Hospital May 5, 2010 Challenges of VTE Prophylaxis in Orthopaedics C. W. Colwell, Jr., M.D. At Scripps Clinic Challenges of VTE Prophylaxis in Orthopaedics I have a potential
UvA-DARE (Digital Academic Repository) Factor XI as target for antithrombotic therapy van Montfoort, M.L. Link to publication
 UvA-DARE (Digital Academic Repository) Factor XI as target for antithrombotic therapy van Montfoort, M.L. Link to publication Citation for published version (APA): van Montfoort, M. L. (2014). Factor XI
UvA-DARE (Digital Academic Repository) Factor XI as target for antithrombotic therapy van Montfoort, M.L. Link to publication Citation for published version (APA): van Montfoort, M. L. (2014). Factor XI
HIBOR. 1st Prophilaxis. Acute phase treatment. Pentasaccharide. Long-term 2ª ACOs UFH LMWH LMWH LMWH. Competitors
 HIBOR Competitors 1st Prophilaxis LMWH Pentasaccharide Long-term Profilaxis treatment 2ª ACOs LMWH Acute phase treatment UFH LMWH Unfractionated heparin (UFH) Discovered by J. Mc Lean in 1916. Later named
HIBOR Competitors 1st Prophilaxis LMWH Pentasaccharide Long-term Profilaxis treatment 2ª ACOs LMWH Acute phase treatment UFH LMWH Unfractionated heparin (UFH) Discovered by J. Mc Lean in 1916. Later named
Oral Dabigatran Etexilate: an Emerging Alternative to Conventional Anticoagulation Therapy
 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-14-2010 Oral Dabigatran Etexilate: an Emerging Alternative to Conventional Anticoagulation
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-14-2010 Oral Dabigatran Etexilate: an Emerging Alternative to Conventional Anticoagulation
argatroban, 100mg/ml, concentrate for solution for infusion (Exembol) SMC No. (812/12) Mitsubishi Pharma Europe Ltd
 argatroban, 100mg/ml, concentrate for solution for infusion (Exembol) SMC No. (812/12) Mitsubishi Pharma Europe Ltd 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment
argatroban, 100mg/ml, concentrate for solution for infusion (Exembol) SMC No. (812/12) Mitsubishi Pharma Europe Ltd 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment
Type of intervention Primary prevention. Economic study type Cost-effectiveness analysis.
 Cost/death averted with venous thromboembolism prophylaxis in patients undergoing total knee replacement or knee arthroplasty Nerurkar J, Wade W E, Martin B C Record Status This is a critical abstract
Cost/death averted with venous thromboembolism prophylaxis in patients undergoing total knee replacement or knee arthroplasty Nerurkar J, Wade W E, Martin B C Record Status This is a critical abstract
Icd code 10 use of low molecular weight heparin
 Icd code 10 use of low molecular weight heparin The Borg System is 100 % Icd code 10 use of low molecular weight heparin ICD -10 is a diagnostic coding system implemented by the World Health Organization.
Icd code 10 use of low molecular weight heparin The Borg System is 100 % Icd code 10 use of low molecular weight heparin ICD -10 is a diagnostic coding system implemented by the World Health Organization.
Evolving Concepts in the Treatment of Venous Thromboembolism: The Role of Factor Xa Inhibitors
 Evolving Concepts in the Treatment of Venous Thromboembolism: The Role of Factor Xa Inhibitors Edith A. Nutescu, Pharm.D., and Cathy M. Helgason, M.D. Anticoagulation is an essential component of the care
Evolving Concepts in the Treatment of Venous Thromboembolism: The Role of Factor Xa Inhibitors Edith A. Nutescu, Pharm.D., and Cathy M. Helgason, M.D. Anticoagulation is an essential component of the care
Personal Disclosure. The Coagulation Cascade. Learning Objectives. Unfractionated Heparin (UFH): Mechanism of Action. Heparin: Mechanism of Action
 Personal Disclosure Heparin/Low Molecular Weight Heparin and Fondaparinux Pharmacology and Pharmacotherapy Mary Jane E. Mattern PharmD Pharmacist William W. Backus Hospital There are no actual or potential
Personal Disclosure Heparin/Low Molecular Weight Heparin and Fondaparinux Pharmacology and Pharmacotherapy Mary Jane E. Mattern PharmD Pharmacist William W. Backus Hospital There are no actual or potential
Enoxaparin sodium 150mg (equivalent to 15,000 IU anti-xa. activity) in 0.2ml water for injections. activity) in 0.4ml water for injections
 1. NAME OF THE MEDICINAL PRODUCT Clexane (Lovenox) Syringes Clexane (Lovenox) Forte Syringes 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Clexane (Lovenox) Syringes (100mg/ml) 20mg Injection 40mg Injection
1. NAME OF THE MEDICINAL PRODUCT Clexane (Lovenox) Syringes Clexane (Lovenox) Forte Syringes 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Clexane (Lovenox) Syringes (100mg/ml) 20mg Injection 40mg Injection
Venous Thromboembolism Prophylaxis after Major Elective Orthopedic Surgery
 Venous Thromboembolism Prophylaxis after Major Elective Orthopedic Surgery Tony Wan, MD, FRCPC Clinical Instructor, Division of General Internal Medicine Department of Medicine, University of British Columbia
Venous Thromboembolism Prophylaxis after Major Elective Orthopedic Surgery Tony Wan, MD, FRCPC Clinical Instructor, Division of General Internal Medicine Department of Medicine, University of British Columbia
Perioperative management of patients on warfarin requiring elective surgery Dr K Boyd, Mrs S Doyle
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Perioperative management of patients on warfarin requiring elective surgery Dr K Boyd, Mrs S Doyle Haematology Acute Date Uploaded:
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Perioperative management of patients on warfarin requiring elective surgery Dr K Boyd, Mrs S Doyle Haematology Acute Date Uploaded:
Study population The study population comprised patients undergoing major hip or knee surgery.
 Pharmacoeconomic analysis of fondaparinux versus enoxaparin for the prevention of thromboembolic events in orthopedic surgery patients Dranitsaris G, Kahn S R, Stumpo C, Paton T W, Martineau J, Smith R,
Pharmacoeconomic analysis of fondaparinux versus enoxaparin for the prevention of thromboembolic events in orthopedic surgery patients Dranitsaris G, Kahn S R, Stumpo C, Paton T W, Martineau J, Smith R,
APC/DTC Briefing Document
 Page 1 London New Drugs Group APC/DTC Briefing Document DABIGATRAN (PRADAXA) FOR THE PREVENTION OF VENOUS THROMBOEMBOLISM Contents Summary 1 Points for consideration 2 Background 3 Hip and knee replacement
Page 1 London New Drugs Group APC/DTC Briefing Document DABIGATRAN (PRADAXA) FOR THE PREVENTION OF VENOUS THROMBOEMBOLISM Contents Summary 1 Points for consideration 2 Background 3 Hip and knee replacement
Coagulation Mechanisms Dr. Nervana Bayoumy
 Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015
 + Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
+ Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
BETRIXABAN TO PREVENT PE, DVT, STROKE: MEDICALLY ILL PATIENTS Samuel Z. Goldhaber, MD Director, Thrombosis Research Group Section Head, Vascular
 BETRIXABAN TO PREVENT PE, DVT, STROKE: MEDICALLY ILL PATIENTS Samuel Z. Goldhaber, MD Director, Thrombosis Research Group Section Head, Vascular Medicine Cardiovascular Division Brigham and Women s Hospital
BETRIXABAN TO PREVENT PE, DVT, STROKE: MEDICALLY ILL PATIENTS Samuel Z. Goldhaber, MD Director, Thrombosis Research Group Section Head, Vascular Medicine Cardiovascular Division Brigham and Women s Hospital
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS
 Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
Inhibitors of propagation of coagulation: factors V and X
 British Journal of Clinical Pharmacology DOI:10.1111/j.1365-2125.2011.04001.x Inhibitors of propagation of coagulation: factors V and X Vincenzo Toschi 1 & Maddalena Lettino 2 1 Department of Hematology
British Journal of Clinical Pharmacology DOI:10.1111/j.1365-2125.2011.04001.x Inhibitors of propagation of coagulation: factors V and X Vincenzo Toschi 1 & Maddalena Lettino 2 1 Department of Hematology
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues
 Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Laboratory Monitoring of Anticoagulation
 Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
Consulted With; Post/Committee/Group Date Haematology Dr Shereen Elshazly (Lead for Anticoagulation) January 2016 Department of Anaesthesia
 Peri-procedural anticoagulation in Adult patients taking Warfarin and novel oral anti-coagulants (NOACS) Clinical Guideline Register No: 16005 Status: Public Developed in response to: Contributes to CQC
Peri-procedural anticoagulation in Adult patients taking Warfarin and novel oral anti-coagulants (NOACS) Clinical Guideline Register No: 16005 Status: Public Developed in response to: Contributes to CQC
Platelet Factor IV- Heparin Antibodies. Presenter: Michael J. Warhol, M.D.
 Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
Anti- THrombosis with Enoxaparin in intubated Adolescents
 Anti- THrombosis with Enoxaparin in intubated Adolescents E. Vincent S. Faustino, MD, MHS October 2017 NHLBI submission S L I D E 0 Research question, central hypothesis and primary aim Research Question
Anti- THrombosis with Enoxaparin in intubated Adolescents E. Vincent S. Faustino, MD, MHS October 2017 NHLBI submission S L I D E 0 Research question, central hypothesis and primary aim Research Question
THE MICHELANGELO OASIS 5 PROGRAM. MichelAngelo : The Creation of Man (Fragment of the Sistine Chapel ceiling- Detail) ( )
 THE MICHELANGELO OASIS 5 PROGRAM MichelAngelo : The Creation of Man (Fragment of the Sistine Chapel ceiling- Detail) (1511-12) Key Steps in Coagulation Pathway Intrinsic pathway Extrinsic pathway 1 Xa
THE MICHELANGELO OASIS 5 PROGRAM MichelAngelo : The Creation of Man (Fragment of the Sistine Chapel ceiling- Detail) (1511-12) Key Steps in Coagulation Pathway Intrinsic pathway Extrinsic pathway 1 Xa
Advances in oral anticoagulation treatment: the safety and efficacy of rivaroxaban in the prevention and treatment of thromboembolism
 352040620712453067AGG TurpieTherapeutic Advances in Hematology 2012 Therapeutic Advances in Hematology Review Advances in oral anticoagulation treatment: the safety and efficacy of rivaroxaban in the prevention
352040620712453067AGG TurpieTherapeutic Advances in Hematology 2012 Therapeutic Advances in Hematology Review Advances in oral anticoagulation treatment: the safety and efficacy of rivaroxaban in the prevention
Development of New Anticoagulants: Present and Future
 Development of New Anticoagulants: Present and Future Job Harenberg, M.D. 1 ABSTRACT Anticoagulant drugs are the most frequently hospital-prescribed compounds in many countries and are used with the intention
Development of New Anticoagulants: Present and Future Job Harenberg, M.D. 1 ABSTRACT Anticoagulant drugs are the most frequently hospital-prescribed compounds in many countries and are used with the intention
Understanding the Hazards of Heparin
 Understanding the Hazards of Heparin 1 Contact Hours First Published: March 31, 2012 Course Revised: May, 2018 Course Expires: May 31, 2021 Reproduction and distribution of these materials is prohibited
Understanding the Hazards of Heparin 1 Contact Hours First Published: March 31, 2012 Course Revised: May, 2018 Course Expires: May 31, 2021 Reproduction and distribution of these materials is prohibited
Changes in coagulation and tissue plasminogen activator after the treatment of cerebral infarction with lumbrokinase
 Clinical Hemorheology and Microcirculation 23 (2000) 213 218 213 IOS Press Changes in coagulation and tissue plasminogen activator after the treatment of cerebral infarction with lumbrokinase Lirong Jin
Clinical Hemorheology and Microcirculation 23 (2000) 213 218 213 IOS Press Changes in coagulation and tissue plasminogen activator after the treatment of cerebral infarction with lumbrokinase Lirong Jin
Adv Pathophysiology Unit 4 Page 1 of 10. Learning Objectives for this file:
 Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
DOACs Can Be Reversed!
 1 DOACs Can Be Reversed! AC Forum 14 th National Conference April 21, 2017 Adam Cuker, MD, MS Perelman School of Medicine University of Pennsylvania 2 Full disclosures (last 12 months) Research support
1 DOACs Can Be Reversed! AC Forum 14 th National Conference April 21, 2017 Adam Cuker, MD, MS Perelman School of Medicine University of Pennsylvania 2 Full disclosures (last 12 months) Research support
THE PHARMA INNOVATION - JOURNAL Dabigatran Etexilate: A Drug Update
 Received: 25-02-2013 Accepted: 26-04-2013 ISSN: 2277-7695 CODEN Code: PIHNBQ ZDB-Number: 2663038-2 IC Journal No: 7725 Vol. 2 Issue 3 2013 Online Available at www.thepharmajournal.com THE PHARMA INNOVATION
Received: 25-02-2013 Accepted: 26-04-2013 ISSN: 2277-7695 CODEN Code: PIHNBQ ZDB-Number: 2663038-2 IC Journal No: 7725 Vol. 2 Issue 3 2013 Online Available at www.thepharmajournal.com THE PHARMA INNOVATION
Antithrombosis Management for Pediatric VAD and Beyond
 Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
EDUCATIONAL COMMENTARY D-DIMER UPDATE
 EDUCATIONAL COMMENTARY D-DIMER UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits see the Continuing
EDUCATIONAL COMMENTARY D-DIMER UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits see the Continuing
Clinical Study Synopsis for Public Disclosure
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis - which is part of
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis - which is part of
New Drug Evaluation: Betrixaban Capsules
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
General Principles of. Hemostasis. Kristine Krafts, M.D.
 General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
Learning Objectives include:
 Organization Frederick Memorial Hospital Solution Title Using Lean to Improve Quality Outcomes DVT Case Study Program/Project Description, including Goals: Hospital Acquired DVTs have become a very serious
Organization Frederick Memorial Hospital Solution Title Using Lean to Improve Quality Outcomes DVT Case Study Program/Project Description, including Goals: Hospital Acquired DVTs have become a very serious
The history of anticoagulation. Mike Greaves [1949-] University of Aberdeen
![The history of anticoagulation. Mike Greaves [1949-] University of Aberdeen The history of anticoagulation. Mike Greaves [1949-] University of Aberdeen](/thumbs/86/93082514.jpg) The history of anticoagulation Mike Greaves [1949-] University of Aberdeen Disclosure I have avoided financial support from the pharmaceutical industry for around 7 years The history of heparin 1916 Heparin
The history of anticoagulation Mike Greaves [1949-] University of Aberdeen Disclosure I have avoided financial support from the pharmaceutical industry for around 7 years The history of heparin 1916 Heparin
