V Activated Platelet. vwf. IXa VIII. Inhibition path. VIIa PAI-1 TFPI. Quick Guide To Haemostasis
|
|
|
- Clifford Newton
- 6 years ago
- Views:
Transcription
1 IIa PC AT II APC P V PS APC Va Xa AT Activated Platelet X vwf AT IXa VIIIa APC PS VIII IX Inhibition path Xa TFPI VIIa TF AT PAI-1 APC PS Xa Quick Guide To Haemostasis R
2 Screening assays in Haemostasis Anticoagulant therapy monitoring (1): Vitamin K antagonists Anticoagulant therapy monitoring (2): Heparin Assays for other anticoagulant therapy (3) isseminated Intravascular Coagulation (IC) Thrombophilia -imer assay for the exclusion of venous thromboembolism (VT) Lupus anticoagulants / Antiphospholipid antibodies For more information, visit our website at
3 Screening assays in Haemostasis 1) Questionnaire l Personal and familial history l Treatments l iseases l Clinical symptoms 2) Physical examination 3) Pre-operative Haemostasis screening assays l Prothrombin time (PT) n Screening test for the extrinsic and common pathways of coagulation (factors II, V, VII, X). Limited sensitivity to fibrinogen. n Usual normal ranges: sec (may vary between reagents, please refer to manufacturer s insert) l Activated Partial Thromboplastin Time (aptt) n Screening test for the intrinsic and common coagulation pathways of coagulation (factors VIII, IX, XI, XII, V and II). Limited sensitivity to fibrinogen. n May be normal in some forms of von Willebrand disease n Usual normal range: ratio patient/reference 1.2 l Thrombin time n xploration of fibrin formation n Usual normal range: < 21 seconds (may vary between reagents, please refer to manufacturer s insert) ffects of coagulation factors and protein levels on clotting assays FACTORS NORMAL VALUS MINIMUM LVL FOR LOW BLING RISK INFLUNC OF COAGULATION TSTS 2 PT 3 aptt 4 TT 5 XII % - N N XI % 20-30% N N VIII % 30-40% N N IX % 30-40% N N VII % 10-20% N N X % 30-40% N V % 30-40% N II % 30-40% N Fibrinogen 2-4 g/l g/l N or N or VWF % 40% N N or N Antithrombin % - N N N Protein C % - N N N Protein S % 6 - N N N 1. Approximate level in the case of a single factor deficiency. These levels may vary according to different clinical settings, e.g. haemophiliacs undergoing surgery will require higher levels of FVIII 2. Results vary as a function of sensitivity of reagents and single or multiple factor levels 3. PT: Prothrombin Time 4. aptt: activated Partial Thromboplastin Time 5. TT: Thrombin time 6. Sex and age-dependent
4 Screening assays in Haemostasis l Fibrinogen level n Quantitative assay of fibrinogen level n Usual normal range: 2-4 g/l ( mg/dl) n levated fibrinogen levels are observed in inflammatory syndrome (acute or chronic) l Platelet count n Number of circulating platelets n Usual normal range: G/L 4) Screening assays for isseminated Intravascular Coagulation (IC) PT, aptt and fibrinogen levels, as well as -imers, are generally abnormal in acute IC but may be normal during chronic and subacute IC. These screening tests are thus of limited specificity and sensitivity for the diagnosis of IC (see section on IC). Recent studies suggest that fibrin monomer may constitute early and more specific markers of IC. 5) Screening assays for thrombophilia l There are as yet no global tests available to explore all thrombophilia factors. l First-line activity assays are required for monitoring of inhibitors (see Thrombophilia section). 6) Screening tests for Lupus Anticoagulants (LA) l The screening assays are phospholipid-dependent function tests. At least two different tests are required for detection of LA (see Lupus Anticoagulants section). Bibliography: l Simple coagulation tests survival prediction in patients with septic shock. Lissalde Lavigne G et al. J Thromb Haemost 2008, 6: l Guidelines for the diagnosis and management of IC. Levi M. et al. Br J Haematol, 2009, 145, 1:24-33 l IC diagnosed based on the Japanese association for acute medicine criteria is a dependant continuum to overt IC in patient with sepsis. Gando S. et al. Thromb Res, 2009, 123, 5: l Conduites pratiques en hémostase, Charles Marc Samama, LFB monograph, 1996 l Hémostase & thrombose, La Simare éditions impression, 1994 l Hemostasis, a case oriented approach,. A. Triplett, Igaku-Shoin Medical publishers, 1985 l Recommandations pour une juste prescription des examens d hémostase en pratique médicale courante, M. Gouault-Heilmann, STV, 2006; vol.18, No1, pages l Laboratory Techniques in Thrombosis - A Manual, Second revised edition of the CAT Assay Procedures, Jespersen J, Bertina RM, Haverkate F, 1999, pages 1-308
5 Anticoagulant therapy monitoring (1) Oral anticoagulant therapy with vitamin K antagonists (VKA*) l Vitamin K antagonists reduce synthesis of both vitamin K-dependent coagulation factors (factors II, VII, IX, X) and some proteins (Protein C and Protein S). The deficiency in factors II, VII, IX and X induced by the absorption of vitamin K antagonists results in prolongation of PT and of aptt. l The Prothrombin Time is the reference test of choice for monitoring of vitamin K antagonist therapy. It is expressed as a coagulation time, using the ratio between the patient and a control, or as % prothrombin time, leading to wide inter-laboratory result variability due to the use of different analysers/reagents combination. In order to standardise the results obtained for patients on vitamin K antagonists, results are expressed as INR. l PT results expressed as INR (International Normalized Ratio) n The INR is the ratio of PT to the power ISI (International Sensitivity Index). It represents the ratio of PT that would have been obtained if an international thromboplastin reference material had been used for the test. n The ISI is a value calculated for each batch of thromboplastin reagent and varies according to the type of analyser used. ISI values are specific for pairs of reagents and instruments. The international recommendations suggest the use of a reagent with an ISI value of less than 1.7. n The control time is the geometric mean of PT values measured on at least 20 fresh plasma samples from healthy subjects (with no pathology or treatment that might interfere with coagulation). ISI Patient Time (sec) INR = ( ) Control Time (sec) l Anticoagulant therapy monitoring n Heparin followed by vitamin K antagonists l Monitoring of treatment with vitamin K antagonists with the INR (using a reagent insensitive to heparin at therapeutic doses) l Monitoring of heparin treatment - aptt (indicates the combined effect of vitamin K antagonists and unfractionated heparin) - Specific anti-xa assay (specific monitoring of anti-xa activity) l Treatment with heparin and vitamin K antagonists may be given concomitantly for 4 to 5 days until the desired therapeutic range is achieved in terms of INR (i.e. two consecutive INR of two consecutive days unchanged and in the therapeutic range). n Stable patients on vitamin K antagonists treatment The INR value should be checked weekly then monthly, and more frequently in the event of a dose change, unbalanced assay results or suspected interference by other factors. *Antivitamins K or vitamin K antagonists
6 Anticoagulant therapy monitoring (1) l N.B.: n Wide inter-patient variability n Interferences due to: l Other treatments (many drugs can interfere with vitamin K antagonists) l Other diseases l Food and drinks rich in vitamin K l Recommended therapeutic ranges (expressed in INR) INICATION INR ACCP 1, BCSH 2, GHT 3 Range Target Prophylaxis of venous thrombosis. Treatment for deep venous thrombosis (VT) and pulmonary embolism (P). Cardiac valve disease. Myocardial infarction. Atrial fibrillation. Antiphospholipid syndrome associated with recurrent VT or additionnal risk factors ACCP: American College of Chest Physicians 2 BCSH: British Committee for Standards in Haematology 3 GHT: Groupe d tude sur l Hémostase et la Thrombose Bibliography: l Guidelines on oral anticoagulation (warfarin): third edition update. Baglin T.P., Keeling.M., Watson H.G. for the British Commitee for Standards in Haemotalogy. Br J Haematol, 2005; 132: l vidence-based Management of Anticoagulant Therapy. Antithrombotic Therapy and Prevention of Thrombosis, 9th d: American College of Chest Physicians vidence-based Clinical Practice Guidelines. Holbrook A., Schulman S., Witt.M., Vandvik P.O., Fish J., Kovacs M.J., Svensson P.J, Veenstra.L., Crowther M., Guyatt G.H. Chest, 2012; 141: 152S-184S
7 Anticoagulant therapy monitoring (2) Unfractionated Heparin monitoring Unfractionated heparin (UFH) is a heterogeneous mix of polysaccharide chains of variable molecular weight. One-third of the chains have a pentasaccharide pattern that has a strong binding affinity to Antithrombin. Molecular weight: 2,000 to 40,000 alton (average: 15,000). They are used for both therapeutic and prophylactic therapy l Limitation: n Short half-life, dose-dependent n Non-specific binding n Random dose-response effect n Major bleeding risk l Sample collection and treatment: n A standardised protocol should be followed for the collection and processing of the samples. n Collection: tube containing an anticoagulant - sodium citrate 0.105/0.109 M or CTA (Citrate, Theophylline, Adenosine, ipyridamole). n Centrifugation within an hour of collection. n Stability at +20 C: 2 hours in a citrate tube or 4 hours in a CTA tube l Assays: n aptt l Widely used for monitoring UFH treatment but sensitive to certain coagulation abnormalities (deficiency or specific coagulation disorders, lupus anticoagulant) and to certain drugs such as vitamin K antagonists (during heparin-vka therapy switch) or thrombolytic drugs Note: Therapeutic ranges may vary between reagents n Anti-Xa activity: standardised measurement using an international standard (see Tables 1 and 2) n Platelet count: for the detection of heparin-induced thrombocytopenia (HIT) l HIT, Type II : - Immunoallergic reaction to the drug - Up to 3% of treated patients (1) - Generally occurs after the 5 th day of treatment - Severe thrombocytopenia, followed by life-threatening thrombotic complications n Antithrombin (AT): for the exclusion of antithrombin deficiency in the case of heparin resistance. Bibliography: l (1) Treatment and Prevention of Heparin-Induced Thrombocytopenia. Antithrombotic Therapy and Prevention of Thrombosis, 9 th ed: American College of Chest Physicians vidence-based Clinical Practice Guidelines. Linkins L.A., ans A.L., Moores L.K., Bona R., avidson B.L., Schulman S., Crowther M. Chest, 2012; 141: 495S-530S
8 Anticoagulant therapy monitoring (2) Table 1 : Unfractionated heparin: curative therapeutic range Curative treatment AMINISTRATION MO SAMPLING aptt Ratio* patient/reference Anti-Xa activity continuous intravenous infusion any time after fourth hour of treatment times 0.3 to 0.7 IU/mL discontinuous subcutaneous or intravenous infusion at the midpoint between 2 injections times 0.3 to 0.7 IU/mL Tableau 2 : Unfractionated Heparin: preventive therapeutic range Preventive treatment AMINISTRATION MO SAMPLING aptt Ratio* patient/reference Anti-Xa activity subcutaneous or intravenous infusion at the midpoint between 2 injections times 0.1 to 0.2 IU/mL *The extent of aptt prolongation differs between reagent. It is recommended that every laboratory establish their own aptt therapeutic range according to their own operating procedure
9 Low Molecular Weight Heparin (LMWH) monitoring l Low Molecular Weight Heparin is obtained by enzymatic or chemical depolymerisation of unfractionated heparin. Molecular weight: to altons (mean: a) l Anticoagulant profile: n Ratio of anti-factor Xa / anti-factor IIa activity: - UFH: 1:1 - LMWH: 2 to 5:1 (and more for same LMWH preparation) l Advantages: n More predictable anticoagulant response n Better bioavailability at low doses n Non-dose-dependent clearance n Longer half-life l Tests: n The result of global coagulation tests (aptt) are not correlated with the anticoagulant activity of LMWH n The only tests currently available are those that specifically measure anti-xa activity in plasma n An international standard for LMWH is available n Anti-Xa activity for LMWH dose adjustment should be assayed at least 48 hours after the initial injection (curative treatment) n Monitoring is not necessary during prophylactic treatment (except in the event of renal impairement, weight gain, bleeding or thrombosis risk) n Monitoring is particularly recommended in children and elderly subjects n Platelet count should be measured: - within the first 24h of treatment - thereafter, twice weekly throughout treatment. Bibliography: l Parenteral anticoagulants. Antithrombotic Therapy and Prevention of Thrombosis. 9 th ed: American College of Chest Physicians vidence-based Clinical Practice Guidelines. Garcia.A., Bagin T.P. Witz J., Samama M.M. Chest, 2012; 141: e24s-e43s
10 Table 3: Heparin derivatives (LMWH and fondaparinux) available in France at curative doses in (1, 16, 18) Product Indications osage Peak anti-xa activity Mean values 1 m±sd Overdose threshold 2 APTT prolongation (if measured) LOVNOX (INN enoxaparin) FRAGMIN (INN dalteparin) FRAXIPARIN (INN nadroparin) INNOHP (INN tinzaparin) FRAXOI (INN nadroparin) ARIXTRA (INN fondaparinux) ARIXTRA (INN fondaparinux) LMWH: twice-daily injection regimen: sample taken at peak activity, 3 to 4 h after injection VT with or without P Acute coronary syndrome stablished VT Unstable angina Non-Q-wave myocardial infarction 100 IU/kg/12h (1 mg/kg/12h) 100 to 120 IU/ kg/12h 85 IU/kg/12h 1.20 ± 0.17 IU/mL 0.6 ± 0.25 IU/mL 1.0 ± 0.2 IU/mL LMWH: once-daily injection regimen: sample taken at peak activity, 4 to 6 h after injection stablished VT Non-serious P stablished VT 175 IU/kg/24h 171 IU/kg/24h 0.87 ± 0.15 IU/mL 1.34 ± 0.15 IU/mL IU = International Units VT: eep Vein Thrombosis; P: Pulmonary mbolism INN: International Nonproprietary Name 1 NB: mean values measured in subjects receiving treatment with each LMWH; 2 Threshold values above which dose reduction can be considered; 3 For patients weighing between 50 and 100 kg; 5 mg/24h for patients weighing < 50 kg; 10 mg/24h for patients weighing > 100 kg N 1.0 IU/mL N Moderate prolongation Moderate prolongation Moderate prolongation < 1.5 IU/mL Prolongation < 1.8 IU/mL Fondaparinux: once-daily injection regimen: sample taken at peak activity, 2 to 3 h after injection stablished VT 7.5 mg/24h Non-serious P µg/ml N Acute coronary syndrome 2.5 mg/24h 0.45 µg/ml N Moderate prolongation No prolongation No prolongation
11 Assays for other anticoagulant therapy (3) Replacement therapy monitoring Hirudin - desirudin (Revasc ) A protein produced by the salivary glands of leeches. irect thrombin inhibitor. Recombinant hirudins are currently commercially available. l Indications (depend on drug and country) n Treatment of patients with heparin-induced thrombocytopenia (HIT) n Prevention of thromboembolic complications after orthopaedic surgery (total hip or knee replacement) in patients with a history of HIT l Laboratory tests n Treatment l aptt: there is a direct relationship between the aptt prolongation and the plasma hirudin concentration, except at high concentrations. l carin clotting time l carin chromogenic assay (CA): for the quantitative determination of hirudin and its analogues n Prophylaxis No recommendation for monitoring, except in the case of renal or hepatic failure or combined treatment with oral anticoagulants. anaparoid Sodium (Orgaran ) Mixture of heparan sulphate (~ 84%), dermatane sulphate (~ 12%) and chondroitin sulphate (~ 4%). Molecular weight: approximately altons. Specific inhibitor of factor Xa. l Indications (according to country) n Treatment of patients presenting HIT n Prophylaxis of post-operative deep venous thrombosis following total hip or knee replacement surgery (in patients with a previous history of HIT) l Laboratory tests n Monitoring not necessary for prophylactic treatments, but recommended for curative treatment. - mild effect on time-based assays (PT and aptt) - anti-xa assays (specific protocol)
12 Assays for other anticoagulant therapy (3) New anticoagulants monitoring Fondaparinux (Arixtra ) Fondaparinux, a pentasaccharide, is a synthetic and selective inhibitor of factor Xa. The administration of this drug is simple: 1 subcutaneous injection per day at a fixed dose regardless of patient characteristics. The half-life varies according to age and is between 17 and 21h, with a peak concentration 2 to 3h after injection l Indications n Prevention of thrombosis in orthopaedic surgery n Prevention of thrombosis in high-risk abdominal surgery n Prevention of thromboembolic events in patients at risk and bedridden for an acute medical problem (cardiac failure, respiratory problems, etc) n Curative treatment of acute deep venous thrombosis n Curative treatment of acute pulmonary embolism l Therapeutic dosage n Preventive treatment: 2.5 mg (or 1.5 mg for renal failure patients) / day n Curative treatment: 7.5 mg/day for patients weighing between 50 and 100 kg l Laboratory tests Although no monitoring is officially recommended, certain clinical situations may require a dosage: n Haemorrhagic or thrombotic accidents n Additional surgery n Renal failure n etc. Anti-Xa activity assay with dedicated controls and calibrator for the monitoring of Fondaparinux (STA - Fondaparinux Control and Calibrator) n Measuring range: 0.1 to 2 µg/ml l The assay measuring range covers all doses irect factor Xa inhibitors Rivaroxaban (Xarelto ) - Apixaban (liquis ) Rivaroxaban and apixaban are synthetic direct factor Xa inhibitors. They have a short half-life and are almost immediately bioavailable upon oral administration. There is currently no antidote available. It may be necessary to measure anticoagulant activity in certain patients or in certain clinical situations.
13 l Indications n VT prophylaxis after total knee or hip replacement surgery n Atrial fibrillation n VT and P treatment (rivaroxaban) n Secondary prevention of VT (rivaroxaban) n Acute coronary events, in combination with antiplatelet drugs l Specific test: rivaroxaban anti-xa activity is assayed using specific controls and calibrators (STA -Rivaroxaban Control & Calibrator) l For specific determination of rivaroxaban anticoagulant activity: l Test to be performed 2 to 4 h after latest intake l Working range: 20 to 500 ng/ml irect Thrombin Inhibitors (TIs) TIs (abigatran -Pradaxa -, Argatroban, Bivalirudine, etc) are direct inhibitors of thrombin with varied therapeutic range. They have a short half-life and practically immediate bioavailability. TIs have no antidotes. It may be necessary to measure anticoagulant activity for certain drugs and in certain patients. l Indications (according to drug and country) n Treatment of patients with heparin-induced thrombocytopenia (Argatroban, Bivalirudine ) n Prevention of thrombosis n Prevention of stroke in atrial fibrillation n Prevention of thromboembolic complications following orthopaedic or cardiac surgery. l Laboratory tests n aptt: there is a direct relationship between the aptt prolongation and the TIs concentration in plasma, however: l This test is greatly affected by different variables (presence of lupus anticoagulants, factor deficiencies, etc) and concomitant treatments (vitamin K antagonists, heparin, etc) l The measuring range is unsuitable for TIs l There is poor linearity with high doses of TIs n carin clotting time (CT): this is considered as the reference test, but: l It is dependent on the patient s thrombin and fibrinogen levels. l There is no standardisation n carin chromogenic assay (CA): is a specific and quantitative assay of TIs levels
14
15 isseminated intravascular coagulation (IC) l IC is an acquired syndrome characterised by excessive systemic intravascular activation of coagulation, with no specific site and due to a variety of different causes and origins (ISTH 2001). l iagnosis of IC is based on clinical criteria (presence of underlying disease or specific medical conditions such as septicaemia, trauma, malignant tumour, etc) and laboratory criteria. l There are 2 types of IC: n Compensated or «non-overt» IC n ecompensated or «overt» IC Non-overt IC is defined as IC with no signs of haemorrhage or thrombosis. iagnosis of compensated IC is based primarily on laboratory criteria. Overt IC consists of established, manifest and serious IC. iagnosis is based on a combination of clinical signs and different laboratory tests. Fibrinogen Thrombin Fibrin Monomer Plasmin Plasmin Fibrinogen degradation products (FP) + + FXIII Stabilised fibrin clot Plasmin -imers Fibrin degradation products (FPn) + Solubles complexes = Fibrin monomer + FP Fibrin monomer + FPn Fibrin monomer + fibrinogen
16 iagnosis of IC Clinical diagnosis Clinical signs of IC are either thrombotic signs or haemorrhagic signs, or both at the same time. Patients are classified according to 3 different physiological clinical scoring systems. Laboratory diagnosis There are no laboratory tests truly specific for IC. PT, aptt and fibrinogen are generally abnormal in acute IC, but they may be normal in chronic or subacute IC. These screening tests are thus of limited specificity and sensitivity for diagnosis of IC. Recent studies show assay of fibrin monomers to be an early marker for IC. etermination of IC defined by the ISTH is based on the presence of underlying disorders and on clotting tests, which allow the identification of patients presenting non-overt and overt IC. PRSNC OF AN UNRLYING ISORR ASSOCIAT WITH IC YS: proceed with ISTH overt IC score PT, APTT, Fibrinogen, platelet count, fibrin-related markers NO: stop Score : l Platelet count: > 100 G/L = 0 < 100 G/L = 1 < 50 G/L = 2 l Fibrinolysis: (e.g: -i, FP, FM): No increase = 0 moderate increase = 2 high increase = 3 l PT prolongation: < 3 sec. = 0 3 sec. < PT < 6 sec. = 1 > 6 sec. = 2 l Fibrinogen: > 1 g/l = 0 > 1 g/l = 1 Overall score : 5 compatible with overt-ic (repeat daily) < 5 non-suggestive of overt IC (repeat the next 1-2 days) Bibliography: l isseminated Intravascular Coagulation. Levi M, Cate H. ten. NJM, 1999, l iagnostic Criteria and Laboratory Tests for isseminated Intravascular Coagulation. Kaneko T., Wada H. J. Clin. xp. Hematopathol. 2011; 51: l iagnosis of isseminated Intravascular Coagulation and related consumptive coagulopathies. Mammen F. Caduceus Medical Publishers Inc., Patterson, NY, USA, 1992 l Laboratory diagnosis of IC and activated coagulation. Schmaier AH., IC assessment ABC monography,1989, 2-18 l Towards efinition, Clinical and Laboratory Criteria, and a Scoring System for isseminated Intravascular Coagulation (ISTH), Taylor F.B., Toh C.H., Hoots W.K., Wada H., Levi M., Thromb Haemost, 2001; 86: l iagnostic criteria and laboratory tests for disseminated intravascular coagulation. Kaneko T, Wada H. J. Clin. xp. Hematopathol 2011; 51: 67-76
17 Thrombophilia l Thrombophilia may be defined as the tendency to develop thrombosis: n Hereditary thrombophilia (congenital or juvenile), is a genetically determined tendency to develop venous thrombosis. n Acquired thrombophilia. Classification l Hereditary thrombophilia (congenital) n Associated with a family history of venous thrombosis (in most cases). n Recurrent thrombosis in certain patients. n Not always associated with a clear triggering factor. n Affects young subjects: < 60 years. l Acquired thrombophilia n No associated family history (generally). n Associated with transient triggering event such as: l Traumatic injury. l Pregnancy - in particular during the post-partum period. l Immobilisation (i.e., stasis, long flights, etc). l Post-operative period. l Advanced age (first event > 60 years). n Oestrogen therapy. n Antiphospholipid antibodies. n Can also be associated with other clinical disorders such as: l Cancer. l Heparin-induced thrombocytopenia. iagnostic tests for thrombophilia l Prelimary Screen: n Antithrombin, Protein C, Protein S, resistance to activated Protein C / Factor V Leiden, prothrombin gene mutation, lupus anticoagulants (LA) and antiphospholipid antibodies (APA). l Secondary Screen: n Fibrinogen, homocysteine. n Investigation of fibrinolysis (tpa, etc.) n Assay of factor VIII, etc.
18 Thrombophilia Prevalence in thrombotic subjects CAUSS USUAL VALUS RLATIV RISK PRVALNC Antithrombin % in heterozygous 1-2% in patients patients with VT Protein C % 6 3% in patients with VT % in the Protein S* % 5 in patients general population 2-3% in thrombotic subjects 5% in the general FV leiden 3-5 heterozygous patients population >20% in thrombotic subjects FII genous polymorphism 2-3 heterogenous patients 2% in the uropean population αβ2gp1 + ACL 2.2 *depends on age and sex l Other tests n Other Haemostasis elements. l Sample collection procedure Samples used for confirmation of thrombophilia must be collected at least 3 months after the latest thrombotic event and in accordance with the time limits associated with the test to be performed after the end of treatment. n Samples should not be taken in the following cases: l uring acute episodes of VT/P l uring oral anticoagulant treatment with vitamin K antagonists, PC and PS levels are reduced by 50% and levels of activity are reduced. l It is necessary to wait one month after discontinuation of treatment with vitamin K antagonists before performing Protein C and Protein S assays. l In the case of heparin treatment, which could reduce antithrombin levels l In pregnant women and for up to 3 months after childbirth l In patients on oestrogen therapy until 2 cycles after treatment discontinuation (e.g. contraceptive pills) l In patients treated with L-asparaginase l In patients with nephritic syndrome, hepatic impairment, IC or an inflammatory condition. l In the case of positive screening tests for LA, further screening should be repeated after 12 weeks. Low levels of PC and PS are seen in normal paediatric samples. In tests performed on paediatric samples, normal values for patients of the same age group should be established before the diagnosis is established. Bibliography : l Inherited thrombophilia: part 1. Lane et al. Thromb Haemost. 1996; 76: 651. l High prevalence of antithrombin III, protein C and S deficiency, but not factor V Leiden mutation in venous thrombophilic Chinese patients in Taiwan. Shen MC, Lin JS, Tsay W, Thromb Res. 1997; 87: l Risk factors for venous thrombotic disease. Rosendaal FR. Thromb Haemost. 199; 82: l Protein C and protein S deficiencies are the most important risk factors associated with thrombosis in Chinese venous thrombophilic patients in Taiwan. Thromb Res. 2000; 99: l Management of thrombophilia, Bauer K. A., J Thromb Haemost. 2003; 1: l Screening for thrombophilia: a laboratory perspective, Jennings I., Cooper P., Br J Biomed Sc. 2003; 60: 39-51
19 -imer assay for exclusion of Venous Thrombombolism (VT) l It has been shown that only -imer is of diagnosis value in ruling out deep venous thrombosis or pulmonary embolism. -imer fragments are formed through the degradation of polymerised fibrin by plasmin. N.B.: High levels of -imers do not necessarily imply VT/P since they may be associated with many other causes. levated -imers may also be found in samples: n from pregnant patients n from older subjects n from patients with infection n following traumatic injury n during the post-operative period n from patients with cancer n from hospitalised patients (who generally have a higher baseline -imer level than ambulatory patients) n from patients with inflammatory syndrome l Value of -imers in the diagnosis of deep venous thrombosis: n Negative Predictive Value (NPV) close to 100% n Use of -imers combined with clinical pretest prohability score clinical pretest prohability score (Wells score) l With a score < 2 for patients with suspected VT l With a score 4 for patients with suspected P l May be used for all patients with suspected VT n Non-invasive method n Limits the number of tests required as well as the need for imaging n Improves diagnosis
20 -imer assay for exclusion of Venous Thrombombolism (VT) l Several studies performed with STA -Liatest -i have shown a negative predictive value (NPV) pretty to close to 100% in ambulatory patients using a threshold value for -imers of 500 ng/ml (i.e. 0.5 µg/ml). Clinical validation of STA -Liatest -i in ruling out diagnosis of VT and P. Number of patients Pathologies NPV STA -Liatest -i 386 P 100% 501 P 99.4% 222 P 100% 114 TVP/P 100% Bibliography: l valuation of a new, rapid, and quantitative imer test in patients with suspected pulmonary embolism. Oger. and al., Am. J. Respir. Crit. Care Med. 1998; 158: l Performances of a new, rapid and automated microlatex imer assay for the exclusion of pulmonary embolism in symptomatic outpatients. Reber G. et al., Thromb Haemost. 1998; 80: l imer testing in patients with suspected pulmonary embolism. Comparison of 2 rapid quantitative assays STA Liatest i and vidas ddimer with an LISA. Lecourvoisier C. et al., ASH l Comparative study of 4 new and rapid imer assays to exclude deep venous thrombosis or pulmonary embolism. Breton. et al., Thromb Haemost. 1997; suppl 1 844: 720.
21 Lupus Anticoagulants (LA) / Antiphospholipid antibodies (APA) l Antiphospholipid antibodies are a heterogeneous family of antibodies directed against proteins bound to negatively charged phospholipids. Lupus-type inhibitors belong to this family of antibodies as do anticardiolipin antibodies. The presence of antiphospholipid antibodies is a biological marker for antiphospholipid syndrome (APS). l APS is an autoimmune disease associated with high risk for thrombosis, recurrent spontaneous miscarriage, thrombocytopenia and numerous other clinical manifestations. l Lupus inhibitor is also known as «antiprothrombinase anticoagulant antibody» or «lupus anticoagulant» (LA). n LA is an acquired abnormality affecting between 1 and 5% of the general population. However, only 15 to 20% of these individuals are positive for control testing performed several months afterwards. n In vitro, LA results in prolonged coagulation times in phospholipiddependent tests (e.g. aptt or PT as well as certain APCR tests). iluted Russell s viper venom time (drvvt) is a specific test used for LA screening. n In vivo, LA is associated with a risk of thrombosis that may result in obstetric, neurological stroke, renal or pulmonary complications. l A single test is not sufficient to allow the diagnosis of this syndrome. l In some patients, transient antiphospholipid antibodies may be detected due to infection or to another treatment, despite the absence of any clinical signs. iagnostic decision tree for screening for LA (1) according to ISTH recommendations Screening test Mixing studies Confirmatory test STA -Staclot RVV Screen (drvvt) prolonged time* STA -Staclot RVV Confirm (drvvt) AN PTT-LA (APTT) prolonged time Ratio patient time > 1.2 referent time Patient plasma + Pool Norm no OR Staclot LA (APTT) CT correction CT > 8 sec NR > 1.2 LA Negative Factor assays LA Positive NR: Normalized Ratio; CT: Clotting Time * If OAT patient, mix 1:1 plasma patient - Pool Norm ** according to Rosner Index or ICA calculation (1)
22 Lupus Anticoagulant (LA) / Antiphospholipid antibodies (APA) Laboratory diagnosis iagnosis may only be made on the basis of two types of test: immunological tests with screening for APA and/or coagulation tests specific for LA. The recommendations of the «Scientific Subcommittees of the International Society on Thrombosis and Haemostasis» (ISTH) are as follows: 1) Lupus Anticoagulants (LA) Must be detected in plasma on at least two occasions separated by a minimum interval of 12 weeks: l Screening step: detection of increased coagulation time during a phospholipiddependent test; n At least 2 screening tests must be performed before LA can be ruled out: l The first-line test is the RVV test. l The second-line test consists of sensitised aptt containing silica activator and a low concentration of phospholipids. l Identification step for the presence of a coagulation inhibitor: 50/50 mix of patient + control (a commercially available pool may be used). l Confirmation step indicating that the inhibition is phospholipid-dependent; the selected test contains a high phospholipid concentration. It must be based on the same principle as the screening test. xclusion of associated clotting disorder. 2) Anticardiolipin antibody (acl) (IgG and/or IgM) May be present in serum or plasma, in moderate to high concentrations (e.g. > 40 GPL or MPL, or > 99th percentile), on at least two occasions, separated by a minimum interval of 12 weeks, determined using a standardised LISA method. 3) Anti-ß2 glycoprotein I antibodies (IgG and/or IgM) May be present in serum or plasma (titre > 99th percentile), on one or two occasions, separated by a minimum interval of 12 weeks, determined using a standardised LISA method, in accordance with the recommended operating procedure. Bibliography: l Pengo A, Update of the guidelines for lupus anticoagulant detection. J. Thromb Haemost. 2009; 7: l Miyakis S et al. International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS). J Thromb Haemost. 2006; 4:
23 AT H A M O S T A S I S PAI-1 tpa FP -imer Plasminogen Plasmin Fibrin Fibrinogen IIa TM IIa PC II APC PS V PS APC Va Xa AT Activated Platelet X vwf AT XI IXa VIIIa APC PS VIII AT XIa IX Activation pathways Coagulation Fibrinolysis Xa TFPI VIIa TF AT Inhibition pathways PAI-1 APC PS Xa AT TFPI
24 agencel2r.com iagnostica Stago - All rights reserved - Non-contractual illustration - 07/ Ref For further information, please contact: At the Heart of Haemostasis iagnostica Stago S.A.S. RCS Nanterre B , allée Thérésa Asnières sur Seine France Ph.: +33 (0) Fax: +33 (0) webmaster@stago.com
Hypercoagulation. CP Conference 11/14/2006
 Hypercoagulation CP Conference 11/14/2006 Overview Hypercoagulation: poorly understood phenomena No definite cause is identified in > 40% of cases Three major factors in thrombus formation (Rudolf Virchow,
Hypercoagulation CP Conference 11/14/2006 Overview Hypercoagulation: poorly understood phenomena No definite cause is identified in > 40% of cases Three major factors in thrombus formation (Rudolf Virchow,
UW Medicine Alternative Monitoring for Antithrombotic Agents
 Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
Managing the Risks Associated with Anticoagulant Therapy. Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde
 Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Index. Autoimmune thrombocytopenic purpura (AITP), 100, 102, 105, 108, 187 Automated platelet counters, , 108
 A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
DOAC s and Implications on Laboratory Results. Kandice Kottke-Marchant, MD, PhD Cleveland Clinic
 DOAC s and Implications on Laboratory Results Kandice Kottke-Marchant, MD, PhD Cleveland Clinic Anticoagulants Heparin Low Molecular Weight Heparins enoxaparin, fragmin Heparin pentasaccharide - fondaparinux
DOAC s and Implications on Laboratory Results Kandice Kottke-Marchant, MD, PhD Cleveland Clinic Anticoagulants Heparin Low Molecular Weight Heparins enoxaparin, fragmin Heparin pentasaccharide - fondaparinux
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues
 Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems.
 Test Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems. Karen A. Moffat BEd, MSc, ART, FCSMLS(D) Technical Specialist, Coagulation, HRLMP Assistant Professor, Department of
Test Plasma Testing in the Clinical Coagulation Laboratory: New drugs, new problems. Karen A. Moffat BEd, MSc, ART, FCSMLS(D) Technical Specialist, Coagulation, HRLMP Assistant Professor, Department of
LVHN Scholarly Works. Lehigh Valley Health Network. Joseph G. Ottinger RPh, MS, MBA, BCPS Lehigh Valley Health Network,
 Lehigh Valley Health Network LVHN Scholarly Works Department of Pharmacy Retrospective Evaluation of Delayed Administration of Fondaparinux in Providing Comparable Safety and Efficacy Outcomes in Patients
Lehigh Valley Health Network LVHN Scholarly Works Department of Pharmacy Retrospective Evaluation of Delayed Administration of Fondaparinux in Providing Comparable Safety and Efficacy Outcomes in Patients
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY
 LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
Laboratory Monitoring of Anticoagulation
 Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D.
 New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D. Professor of Cardiovascular Medicine University of Maryland School of Medicine Copyright A.P. Wheeler 2009
New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D. Professor of Cardiovascular Medicine University of Maryland School of Medicine Copyright A.P. Wheeler 2009
Local vasoconstriction. is due to local spasm of the smooth muscle (symp. reflex) can be maintained by platelet vasoconstrictors
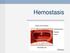 Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
TSOAC Case Study 1. Question. TSOAC Case Study 1 Continued
 TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
Special Coagulation - APC Resistance. DiaPharma Group, Inc. Customer Service: Technical Support:
 Special Coagulation - APC Resistance DiaPharma Group, Inc. Customer Service: 1.800.526.5224 Technical Support:1.800.447.3846 www.diapharma.com 1 Review of Hemostasis Overview Pathways of coagulation, anticoagulation,
Special Coagulation - APC Resistance DiaPharma Group, Inc. Customer Service: 1.800.526.5224 Technical Support:1.800.447.3846 www.diapharma.com 1 Review of Hemostasis Overview Pathways of coagulation, anticoagulation,
Laboratory investigation in the Bleeding Patient. Dr Craig Taylor Consultant Haematologist May 2016
 Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
Lina Al-Lawama. Rama Al-Ashqar. Malik Al-Zohlof
 2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
Clumsy Coagulation Communication
 Clumsy Coagulation Communication Let s Blame the Lab! Lab Clinician Communication Barriers and opportunities Where are the errors made? How do we enhance patient experience? George A Fritsma MS, MLS, Your
Clumsy Coagulation Communication Let s Blame the Lab! Lab Clinician Communication Barriers and opportunities Where are the errors made? How do we enhance patient experience? George A Fritsma MS, MLS, Your
ANTICOAGULANT THERAPY ANTICOAGULANT THERAPY REVISITED Thrombosis is a complication of underaggressive anticoagulant therapy
 ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 07.01.18 Last Review Date: 02.18 Line of Business: Oregon Health Plan Coding Implications Revision Log See Important Reminder at
Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 07.01.18 Last Review Date: 02.18 Line of Business: Oregon Health Plan Coding Implications Revision Log See Important Reminder at
HIBOR. 1st Prophilaxis. Acute phase treatment. Pentasaccharide. Long-term 2ª ACOs UFH LMWH LMWH LMWH. Competitors
 HIBOR Competitors 1st Prophilaxis LMWH Pentasaccharide Long-term Profilaxis treatment 2ª ACOs LMWH Acute phase treatment UFH LMWH Unfractionated heparin (UFH) Discovered by J. Mc Lean in 1916. Later named
HIBOR Competitors 1st Prophilaxis LMWH Pentasaccharide Long-term Profilaxis treatment 2ª ACOs LMWH Acute phase treatment UFH LMWH Unfractionated heparin (UFH) Discovered by J. Mc Lean in 1916. Later named
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Fragmin) Reference Number: CP.PHAR.225 Effective Date: 05.01.16 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Coding Implications Revision Log See Important Reminder
Clinical Policy: (Fragmin) Reference Number: CP.PHAR.225 Effective Date: 05.01.16 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Coding Implications Revision Log See Important Reminder
Coagulation Cascade. TF-VIIa. Tissue Factor + VII. XIIa. Prothrombin. XIa. IXa. VIIIa. Thrombin. XL- Fibrin. XIII Monomer. Fibrinogen.
 Coagulation Cascade Intrinsic Pathway Extrinsic Pathway Contact Activation XIIa XI XIa Prekallikrein HMW Kininogen IX IXa Ca 2+ Anticoagulation proteins: Protein C, Protein S, Antithrombin III, TFPI TF
Coagulation Cascade Intrinsic Pathway Extrinsic Pathway Contact Activation XIIa XI XIa Prekallikrein HMW Kininogen IX IXa Ca 2+ Anticoagulation proteins: Protein C, Protein S, Antithrombin III, TFPI TF
Continuing Education for Pharmacists
 Continuing Education for Pharmacists Oral anticoagulation without protimes: A review of two emerging agents that may come to market. Lindsay Davis, Pharm.D. (Acute Care Pharmacy Resident, Phoenix VA Medical
Continuing Education for Pharmacists Oral anticoagulation without protimes: A review of two emerging agents that may come to market. Lindsay Davis, Pharm.D. (Acute Care Pharmacy Resident, Phoenix VA Medical
Disclosure (s) Relevant financial relationship(s) None Off-label usage None Change in slide set You betcha! (YES!) 2015 MFMER slide-1
 Disclosure (s) Relevant financial relationship(s) None Off-label usage None Change in slide set You betcha! (YES!) 2015 MFMER slide-1 Learning Objectives Explain the concept of thrombophilia Recognize
Disclosure (s) Relevant financial relationship(s) None Off-label usage None Change in slide set You betcha! (YES!) 2015 MFMER slide-1 Learning Objectives Explain the concept of thrombophilia Recognize
PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba
 VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba OVERVIEW Biochemistry of coagulation Pathogenesis of VTE
VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba OVERVIEW Biochemistry of coagulation Pathogenesis of VTE
DOACs: When and how to measure their anticoagulant effect
 DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
Anticoagulation in VTE The Haematologist s Perspective. Dr. M.D. Maina FRCP Edin.
 Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Session 1 Topics. Vascular Phase of Hemostasis. Coagulation Pathway. Action of Unfractionated Heparin. Laboratory Monitoring of Anticoagulant Therapy
 ~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
ANTICOAGULANT THERAPY ANTICOAGULANT THERAPY REVISITED 2005
 ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED Thrombosis is a complication of underaggressive anticoagulant therapy ANTICOAGULANT THERAPY.
 ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY Goals of Therapy PREVENTION OF THROMBOEMBOLISM!!! Stop propagation
ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY Goals of Therapy PREVENTION OF THROMBOEMBOLISM!!! Stop propagation
Platelet Factor IV- Heparin Antibodies. Presenter: Michael J. Warhol, M.D.
 Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
Analysis of the Anticoagulant Market
 MEDICAL DEVICES PHARMACEUTICALS CHEMICALS FOOD & BEVERAGE ELECTRONICS Analysis of the Anticoagulant Market VPG Publications, Consulting, Clients www.vpgcorp.com VPG Market Research Reports www.vpgmarketresearch.com
MEDICAL DEVICES PHARMACEUTICALS CHEMICALS FOOD & BEVERAGE ELECTRONICS Analysis of the Anticoagulant Market VPG Publications, Consulting, Clients www.vpgcorp.com VPG Market Research Reports www.vpgmarketresearch.com
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Commercial, HIM-Medical Benefit, Medicaid Coding Implications Revision Log See
Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Commercial, HIM-Medical Benefit, Medicaid Coding Implications Revision Log See
Activated Protein C Resistance vs Factor V Leiden assay: Which is the most cost effective?
 Activated Protein C Resistance vs Factor V Leiden assay: Which is the most cost effective? Rajiv K. Pruthi, M.B.B.S Co-Director, Special Coagulation Laboratory & Director, Mayo Comprehensive Hemophilia
Activated Protein C Resistance vs Factor V Leiden assay: Which is the most cost effective? Rajiv K. Pruthi, M.B.B.S Co-Director, Special Coagulation Laboratory & Director, Mayo Comprehensive Hemophilia
Drugs used in Thromboembolic Disease. Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014
 Drugs used in Thromboembolic Disease Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014 Drugs used in Thromboembolic Disease Anticoagulants: Heparin. Oral anticoagulants.
Drugs used in Thromboembolic Disease Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014 Drugs used in Thromboembolic Disease Anticoagulants: Heparin. Oral anticoagulants.
Pharmacology Lecture 5. Anticoagulants
 Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Antithrombotic Therapies: Parenteral Agents
 Antithrombotic Therapies: Parenteral Agents Christine A. Sorkness, Pharm.D. Professor of Pharmacy & Medicine (CHS) UW School of Pharmacy Clinical Pharmacist, Anticoagulation Clinic, Wm S. Middleton VA
Antithrombotic Therapies: Parenteral Agents Christine A. Sorkness, Pharm.D. Professor of Pharmacy & Medicine (CHS) UW School of Pharmacy Clinical Pharmacist, Anticoagulation Clinic, Wm S. Middleton VA
Personal Disclosure. The Coagulation Cascade. Learning Objectives. Unfractionated Heparin (UFH): Mechanism of Action. Heparin: Mechanism of Action
 Personal Disclosure Heparin/Low Molecular Weight Heparin and Fondaparinux Pharmacology and Pharmacotherapy Mary Jane E. Mattern PharmD Pharmacist William W. Backus Hospital There are no actual or potential
Personal Disclosure Heparin/Low Molecular Weight Heparin and Fondaparinux Pharmacology and Pharmacotherapy Mary Jane E. Mattern PharmD Pharmacist William W. Backus Hospital There are no actual or potential
Heparin-Induced Thrombocytopenia and New Anticoagulants
 Heparin-Induced Thrombocytopenia and New Anticoagulants September 2004 Elizabeth M. Van Cott, MD Massachusetts General Hospital Boston MA College of American Pathologists 2004. Materials are used with
Heparin-Induced Thrombocytopenia and New Anticoagulants September 2004 Elizabeth M. Van Cott, MD Massachusetts General Hospital Boston MA College of American Pathologists 2004. Materials are used with
General Principles of. Hemostasis. Kristine Krafts, M.D.
 General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
New Anticoagulants Linda Liu, M.D.
 Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
LOW MOLECULAR WEIGHT HEPARIN THE STANDARD VALUE
 LOW MOLECULAR WEIGHT HEPARIN THE STANDARD VALUE ANASTASIOS V. KOROMPILIAS, MD ORTHOPAEDIC DEPARTMENT, MEDICAL SCHOOL UNIVERSITY OF IOANNINA, IOANNINA, GREECE MAJOR ORTHOPAEDIC SURGERY POSTOPERATIVE CLASSIFIED
LOW MOLECULAR WEIGHT HEPARIN THE STANDARD VALUE ANASTASIOS V. KOROMPILIAS, MD ORTHOPAEDIC DEPARTMENT, MEDICAL SCHOOL UNIVERSITY OF IOANNINA, IOANNINA, GREECE MAJOR ORTHOPAEDIC SURGERY POSTOPERATIVE CLASSIFIED
THE NOVEL ORAL ANTICOAGULANTS
 IDEAL ANTITHROMBOTIC AGENT THE NOVEL ORAL ANTICOAGULANTS Kristin Jochmans MD, PhD Dienst Hematologie - Universitair Ziekenhuis Brussel Efficacious (in arterial and venous disease) Safe (no toxicity low
IDEAL ANTITHROMBOTIC AGENT THE NOVEL ORAL ANTICOAGULANTS Kristin Jochmans MD, PhD Dienst Hematologie - Universitair Ziekenhuis Brussel Efficacious (in arterial and venous disease) Safe (no toxicity low
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS
 Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
Reverse the New Anticoagulants? Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care University Medical Center Brackenridge / Dell Seton Medical Center at the University of Texas
Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity
 Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity Abhishek Gulati What is enoxaparin? Low molecular weight heparin anticoagulant Used to minimise the
Linking in silico and in vitro experiments to identify and evaluate a biomarker for enoxaparin activity Abhishek Gulati What is enoxaparin? Low molecular weight heparin anticoagulant Used to minimise the
argatroban, 100mg/ml, concentrate for solution for infusion (Exembol) SMC No. (812/12) Mitsubishi Pharma Europe Ltd
 argatroban, 100mg/ml, concentrate for solution for infusion (Exembol) SMC No. (812/12) Mitsubishi Pharma Europe Ltd 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment
argatroban, 100mg/ml, concentrate for solution for infusion (Exembol) SMC No. (812/12) Mitsubishi Pharma Europe Ltd 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment
Clexane pre-filled syringes 150mg/ml in syringe sizes equating to the following doses: 120mg and 150mg. Page 1 of 8
 Low Molecular Weight Heparins (LMWH) Shared Care Guideline for the use of Enoxaparin and Dalteparin in the Treatment and Prophylaxis of Venous Thromboembolism Introduction Low Molecular Weight Heparins
Low Molecular Weight Heparins (LMWH) Shared Care Guideline for the use of Enoxaparin and Dalteparin in the Treatment and Prophylaxis of Venous Thromboembolism Introduction Low Molecular Weight Heparins
Coagulopathy Case-2. Andy Nguyen, M.D. 2009
 Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides.
 These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
Hemostasis/Thrombosis IV
 Hemostasis/Thrombosis IV Antithrombotic Therapy Antithrombotic Therapy Mainstay of battle against thromboembolic disease Hot area of new drug research Cannot inhibit clot formation without increased risk
Hemostasis/Thrombosis IV Antithrombotic Therapy Antithrombotic Therapy Mainstay of battle against thromboembolic disease Hot area of new drug research Cannot inhibit clot formation without increased risk
Managing Coagulation Abnormalities Linda Liu, M.D.
 Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
Novel Anti-coagulant Agents. David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan
 Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Laboratory Testing Issues for Protein C, Protein S and Antithrombin Assays
 Laboratory Testing Issues for Protein C, Protein S and Antithrombin Assays Richard A. Marlar Ph.D. University of Oklahoma THSNA Meeting- Chicago, IL April 14-16, 2016 DISCLOSURE Richard A. Marlar, PhD
Laboratory Testing Issues for Protein C, Protein S and Antithrombin Assays Richard A. Marlar Ph.D. University of Oklahoma THSNA Meeting- Chicago, IL April 14-16, 2016 DISCLOSURE Richard A. Marlar, PhD
ISIS PHARMACEUTICALS. ISIS-FXI Rx Program Update. Webcast December 8, 2014
 ISIS PHARMACEUTICALS ISIS-FXI Rx Program Update Webcast December 8, 2014 Introduction Stan Crooke, M.D., Ph.D. CEO and Chairman, Isis Pharmaceuticals 2 Forward Looking Language Statement This presentation
ISIS PHARMACEUTICALS ISIS-FXI Rx Program Update Webcast December 8, 2014 Introduction Stan Crooke, M.D., Ph.D. CEO and Chairman, Isis Pharmaceuticals 2 Forward Looking Language Statement This presentation
Coagulation Mechanisms Dr. Nervana Bayoumy
 Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Update on the Direct Oral Anticoagulants (DOACs)
 Update on the Direct Oral Anticoagulants (DOACs) J. Randle Adair DO, PhD Internal Medicine New Mexico Cancer Center & Co-Chair, Anticoagulation Subcommittee Presbyterian Healthcare Services (PHS) Attending,
Update on the Direct Oral Anticoagulants (DOACs) J. Randle Adair DO, PhD Internal Medicine New Mexico Cancer Center & Co-Chair, Anticoagulation Subcommittee Presbyterian Healthcare Services (PHS) Attending,
a unit of Dr Bharat S Mody Director Chief Arthroplasty Surgeon Centre for Knee & Hip Surgery Dr Pankaj Patni Orthopaedic Surgeon Dr Sunil Dewangan
 Centre for Knee & Hip Surgery Arthroscopy a unit of Arthroplasty Dr Bharat S Mody Director Chief Arthroplasty Surgeon Dr Sunil Dewangan Dr Prakash Tekwani Dr Rahul Khanna Dr Pankaj Patni Orthopaedic Surgeon
Centre for Knee & Hip Surgery Arthroscopy a unit of Arthroplasty Dr Bharat S Mody Director Chief Arthroplasty Surgeon Dr Sunil Dewangan Dr Prakash Tekwani Dr Rahul Khanna Dr Pankaj Patni Orthopaedic Surgeon
Coagulation Laboratory: Methods, Standards & Cost Effective Testing Part 1
 Coagulation Laboratory: Methods, Standards & Cost Effective Testing Part 1 Donna D. Castellone, MS, MT (ASCP) SH Clinical Project Manager Hematology and Hemostasis Siemens Healthcare Diagnostics Disclosures
Coagulation Laboratory: Methods, Standards & Cost Effective Testing Part 1 Donna D. Castellone, MS, MT (ASCP) SH Clinical Project Manager Hematology and Hemostasis Siemens Healthcare Diagnostics Disclosures
Please note that the uses described in the following page(s) have not been approved or cleared by FDA, with respect to the described assay or test.
 Please note that the uses described in the following page(s) have not been approved or cleared by FDA, with respect to the described assay or test. In the US, the product is intended For Research Use Only.
Please note that the uses described in the following page(s) have not been approved or cleared by FDA, with respect to the described assay or test. In the US, the product is intended For Research Use Only.
Clotting tests. June 2009 V Diagnostica Stago - All right reserved
 7 Clotting tests June 2009 V2 Reagents Technologies Clotting tests Chromogenic assays Enzyme Immuno Assays (ELISA) Latex Immuno Assays (LIA) Latex slide agglutination Flow cytometry 2 Clotting tests Samples
7 Clotting tests June 2009 V2 Reagents Technologies Clotting tests Chromogenic assays Enzyme Immuno Assays (ELISA) Latex Immuno Assays (LIA) Latex slide agglutination Flow cytometry 2 Clotting tests Samples
iccnet CHSA Clinical Protocol - HEPARIN
 Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
In Hospital Bleeding Management
 In Hospital Bleeding Management Geno J Merli, MD, MACP, FSVM, FHM Professor Medicine & Surgery Co-Director Jefferson Vascular Center Sidney Kimmel Medical College Thomas Jefferson University Hospitals
In Hospital Bleeding Management Geno J Merli, MD, MACP, FSVM, FHM Professor Medicine & Surgery Co-Director Jefferson Vascular Center Sidney Kimmel Medical College Thomas Jefferson University Hospitals
Marcia L. Zucker, Ph.D. ZIVD LLC
 Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 Picture courtesy of Helena Laboratories 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway
Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 Picture courtesy of Helena Laboratories 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway
Laboratory Investigation of Challenging Cases. Laura A. Worfolk, Ph.D Scientific Director, Coagulation
 Laboratory Investigation of Challenging Cases Laura A. Worfolk, Ph.D Scientific Director, Coagulation Coagulation Cascade XII XIIa XI HMWK/Prekallikrein XIa VII Injury IX X IXa VIII Xa X TF TF/VIIa Prothrombin
Laboratory Investigation of Challenging Cases Laura A. Worfolk, Ph.D Scientific Director, Coagulation Coagulation Cascade XII XIIa XI HMWK/Prekallikrein XIa VII Injury IX X IXa VIII Xa X TF TF/VIIa Prothrombin
Venous thromboembolism (VTE) Can Biomarkers Help to Guide Duration of Therapy After VTE? New Chest Guidelines 2016
 Venous thromboembolism (VTE) Can Biomarkers Help to Guide Duration of Therapy After VTE? Marlene Grenon, MD Associate Professor of Surgery University of California San Francisco UCSF Vascular Surgery Symposium
Venous thromboembolism (VTE) Can Biomarkers Help to Guide Duration of Therapy After VTE? Marlene Grenon, MD Associate Professor of Surgery University of California San Francisco UCSF Vascular Surgery Symposium
Scottish Medicines Consortium
 Scottish Medicines Consortium fondaparinux, 2.5mg/0.5ml, solution for injection (Arixtra ) No. (287/06) GlaxoSmithKline 7 July 2006 The Scottish Medicines Consortium has completed its assessment of the
Scottish Medicines Consortium fondaparinux, 2.5mg/0.5ml, solution for injection (Arixtra ) No. (287/06) GlaxoSmithKline 7 July 2006 The Scottish Medicines Consortium has completed its assessment of the
3 : 34. Pankaj Manoria, P C Manoria, Bhopal
 3 : 34 Newer Antithrombins and anticoagulants Introduction Thrombosis is a leading cause of morbidity and mortality but for decades, anticoagulant therapy has usually consisted of unfractionate heparin
3 : 34 Newer Antithrombins and anticoagulants Introduction Thrombosis is a leading cause of morbidity and mortality but for decades, anticoagulant therapy has usually consisted of unfractionate heparin
Marilyn Johnston Hemostasis Reference Laboratory Hamilton,Ontario
 Marilyn Johnston Hemostasis Reference Laboratory Hamilton,Ontario None Discovered in 1916 Named from the Latin word for liver, hepar 1939, heparin requires a plasma cofactor First used in humans in 1940
Marilyn Johnston Hemostasis Reference Laboratory Hamilton,Ontario None Discovered in 1916 Named from the Latin word for liver, hepar 1939, heparin requires a plasma cofactor First used in humans in 1940
Apheresis Anticoagulant Removal. Oluwatoyosi Onwuemene, MD MS May 6th, 2017
 Apheresis Anticoagulant Removal Oluwatoyosi Onwuemene, MD MS May 6th, 2017 Talk Outline Case presentation Factors associated with drug removal TPE s effects on hematologic parameters Anticoagulant properties
Apheresis Anticoagulant Removal Oluwatoyosi Onwuemene, MD MS May 6th, 2017 Talk Outline Case presentation Factors associated with drug removal TPE s effects on hematologic parameters Anticoagulant properties
Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015
 + Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
+ Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
Diagnosing Haemostasis PRODUCT CATALOG
 Diagnosing Haemostasis PRODUCT CATALOG CONTENTS MTI COAGULATION ANALYZER MT1C- Single Channel Semi Automated Coagulation Analyzer MT4C- Four Channel Semi Automated Coagulation Analyzer Bera - New Generation
Diagnosing Haemostasis PRODUCT CATALOG CONTENTS MTI COAGULATION ANALYZER MT1C- Single Channel Semi Automated Coagulation Analyzer MT4C- Four Channel Semi Automated Coagulation Analyzer Bera - New Generation
Physician Orders - Adult
 Physician Orders - Adult attach patient label here Title: Direct Thrombin Inhibitor (DTI) Protocol Orders Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy
Physician Orders - Adult attach patient label here Title: Direct Thrombin Inhibitor (DTI) Protocol Orders Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy
Bayer R&D Investor Day 2005
 Science For A Better Life HealthCare Bayer R&D Investor 25 December 8, 25 London Bayer R&D Investor 25 BAY 59-7939: A Novel, ral, Direct Factor Xa Inhibitor Frank Misselwitz Head of Therapeutic Area Cardiovascular,
Science For A Better Life HealthCare Bayer R&D Investor 25 December 8, 25 London Bayer R&D Investor 25 BAY 59-7939: A Novel, ral, Direct Factor Xa Inhibitor Frank Misselwitz Head of Therapeutic Area Cardiovascular,
Introduction Hemostasis: Tourniquet Test & Bleeding Time. Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO
 Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
Venous Thromboembolism Prophylaxis after Major Elective Orthopedic Surgery
 Venous Thromboembolism Prophylaxis after Major Elective Orthopedic Surgery Tony Wan, MD, FRCPC Clinical Instructor, Division of General Internal Medicine Department of Medicine, University of British Columbia
Venous Thromboembolism Prophylaxis after Major Elective Orthopedic Surgery Tony Wan, MD, FRCPC Clinical Instructor, Division of General Internal Medicine Department of Medicine, University of British Columbia
The novel anticoagulants: entering a new era. BOUNAMEAUX, Henri. Abstract
 Article The novel anticoagulants: entering a new era BOUNAMEAUX, Henri Abstract During the past five decades, anticoagulant therapy has consisted of rapidly acting parenteral drugs (unfractionated heparin
Article The novel anticoagulants: entering a new era BOUNAMEAUX, Henri Abstract During the past five decades, anticoagulant therapy has consisted of rapidly acting parenteral drugs (unfractionated heparin
Anticoagulant therapy has historically consisted. A pharmacologic overview of current and emerging anticoagulants
 A pharmacologic overview of current and emerging anticoagulants EDITH A. NUTESCU, PHARMD; NANCY L. SHAPIRO, PHARMD; AIMEE CHEVALIER, PHARMD; AND ALPESH N. AMIN, MD, MBA ABSTRACT For over 50 years, anticoagulant
A pharmacologic overview of current and emerging anticoagulants EDITH A. NUTESCU, PHARMD; NANCY L. SHAPIRO, PHARMD; AIMEE CHEVALIER, PHARMD; AND ALPESH N. AMIN, MD, MBA ABSTRACT For over 50 years, anticoagulant
2 Thomas G. DeLoughery
 Tests of Hemostasis and Thrombosis 2 Thomas G. DeLoughery A routine laboratory test once well-established is often slavishly adhered to, with little further thought about how it originated, why it is done
Tests of Hemostasis and Thrombosis 2 Thomas G. DeLoughery A routine laboratory test once well-established is often slavishly adhered to, with little further thought about how it originated, why it is done
Haemostasis Reagents product list 2018
 Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch Product # ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Product name
Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch Product # ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Product name
Using TEG in the ED, OR, and ICU. Don H. Van Boerum, MD, FACS
 Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
ENOXAPARIN AHFS??? Class: Low molecular weight heparin (LMWH).
 ENOXAPARIN AHFS??? Class: Low molecular weight heparin (LMWH). Indications: Prevention and treatment of deep vein thrombosis, pulmonary embolism, thrombophlebitis migrans, disseminated intravascular coagulation
ENOXAPARIN AHFS??? Class: Low molecular weight heparin (LMWH). Indications: Prevention and treatment of deep vein thrombosis, pulmonary embolism, thrombophlebitis migrans, disseminated intravascular coagulation
Perioperative management of patients on warfarin requiring elective surgery Dr K Boyd, Mrs S Doyle
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Perioperative management of patients on warfarin requiring elective surgery Dr K Boyd, Mrs S Doyle Haematology Acute Date Uploaded:
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Perioperative management of patients on warfarin requiring elective surgery Dr K Boyd, Mrs S Doyle Haematology Acute Date Uploaded:
Antithrombosis Management for Pediatric VAD and Beyond
 Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
Laboratory Monitoring of Unfractionated Heparin Therapy
 1 PATHOLOGY & LABORATORY MEDICINE December, 2015 Laboratory Monitoring of Unfractionated Heparin Therapy On November 18, 2015, the Thrombosis and Hemostasis Laboratory transitioned from the aptt to the
1 PATHOLOGY & LABORATORY MEDICINE December, 2015 Laboratory Monitoring of Unfractionated Heparin Therapy On November 18, 2015, the Thrombosis and Hemostasis Laboratory transitioned from the aptt to the
Sysmex Educational Enhancement and Development No
 SEED Haematology Sysmex Educational Enhancement and Development No 3 2014 The Thrombin Time test and Reptilase test what is their role in coagulation testing? The purpose of this newsletter is to provide
SEED Haematology Sysmex Educational Enhancement and Development No 3 2014 The Thrombin Time test and Reptilase test what is their role in coagulation testing? The purpose of this newsletter is to provide
Effect of Direct Thrombin Inhibitors, Bivalirudin, Lepirudin, and Argatroban, on Prothrombin Time and INR Values
 Coagulation and Transfusion Medicine / DIRECT THROMBIN INHIBITOR EFFECT ON INR Effect of Direct Thrombin Inhibitors, Bivalirudin, Lepirudin, and Argatroban, on Prothrombin Time and INR Values Robert C.
Coagulation and Transfusion Medicine / DIRECT THROMBIN INHIBITOR EFFECT ON INR Effect of Direct Thrombin Inhibitors, Bivalirudin, Lepirudin, and Argatroban, on Prothrombin Time and INR Values Robert C.
The Role Of Point of Care Coagulation Testing (POCCT) in Patient Blood Management. Elham Khalaf Adeli
 The Role Of Point of Care Coagulation Testing (POCCT) in Patient Blood Management Elham Khalaf Adeli Overview PBM, bleeding management, Coagulation POC Testing Review of laboratory conventional coagulation
The Role Of Point of Care Coagulation Testing (POCCT) in Patient Blood Management Elham Khalaf Adeli Overview PBM, bleeding management, Coagulation POC Testing Review of laboratory conventional coagulation
Understanding the Hazards of Heparin
 Understanding the Hazards of Heparin 1 Contact Hours First Published: March 31, 2012 Course Revised: May, 2018 Course Expires: May 31, 2021 Reproduction and distribution of these materials is prohibited
Understanding the Hazards of Heparin 1 Contact Hours First Published: March 31, 2012 Course Revised: May, 2018 Course Expires: May 31, 2021 Reproduction and distribution of these materials is prohibited
Haemostasis. The function of haemostasis is: to prevent blood loss from injured vessels. to stop bleeding. to prevent thrombosis
 Haemostasis Haemostasis The function of haemostasis is: to prevent blood loss from injured vessels to stop bleeding to prevent thrombosis Haemostasis blood endothelium basement membrane subendothelium
Haemostasis Haemostasis The function of haemostasis is: to prevent blood loss from injured vessels to stop bleeding to prevent thrombosis Haemostasis blood endothelium basement membrane subendothelium
Laboratory testing for Direct Oral Anticoagulants (DOACs): Are we ready?
 The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 12, Issue 1 January 2017 Editorial note: In this topical update, Dr Rock Leung reviews the testing strategy
The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 12, Issue 1 January 2017 Editorial note: In this topical update, Dr Rock Leung reviews the testing strategy
DOACs Can Be Reversed!
 1 DOACs Can Be Reversed! AC Forum 14 th National Conference April 21, 2017 Adam Cuker, MD, MS Perelman School of Medicine University of Pennsylvania 2 Full disclosures (last 12 months) Research support
1 DOACs Can Be Reversed! AC Forum 14 th National Conference April 21, 2017 Adam Cuker, MD, MS Perelman School of Medicine University of Pennsylvania 2 Full disclosures (last 12 months) Research support
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs
 Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom
 If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom Heparin Discovered 1916, commercial available 1935 Heparin Is there an alternative, not really
If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom Heparin Discovered 1916, commercial available 1935 Heparin Is there an alternative, not really
Automated Coagulation Analyser product list 2018
 Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Automated Coagulation
Milan Analytica AG Baslerstrasse 15 4310 Rheinfelden www.milananalytica.ch ** = Smaller Kit Format specifically designed for Helena C-1/2/4/AC-4 ^ = For use with Helena C-1/2/4/AC-4 Automated Coagulation
Guideline on core SmPC for human fibrinogen products
 23 July 2015 EMA/CHMP/BPWP/691754/2013 Rev 1 Committee for Medicinal Products for Human Use (CHMP) Draft Agreed by Blood Products Working Party 27 November 2013 Adoption by CHMP for release for consultation
23 July 2015 EMA/CHMP/BPWP/691754/2013 Rev 1 Committee for Medicinal Products for Human Use (CHMP) Draft Agreed by Blood Products Working Party 27 November 2013 Adoption by CHMP for release for consultation
DRUG NAME : Clexane (enoxaparin) Pre-Filled Syringes
 NHS ONEL & Barking, Havering & Redbridge University Hospitals Trust Shared Care Guidelines DRUG NAME : Clexane (enoxaparin) Pre-Filled Syringes DOCUMENT TO BE SCANNED INTO ELECTRONIC RECORDS AS AND FILED
NHS ONEL & Barking, Havering & Redbridge University Hospitals Trust Shared Care Guidelines DRUG NAME : Clexane (enoxaparin) Pre-Filled Syringes DOCUMENT TO BE SCANNED INTO ELECTRONIC RECORDS AS AND FILED
Basic coagulation applications and case studies
 Basic coagulation applications and case studies Jing Jin Clinical laboratory Scientist (MLS, ASCP) - Coagulation/Hematology Stanford University Hospital and Clinics 1 Agenda Overview about 3 major phases
Basic coagulation applications and case studies Jing Jin Clinical laboratory Scientist (MLS, ASCP) - Coagulation/Hematology Stanford University Hospital and Clinics 1 Agenda Overview about 3 major phases
New Anticoagulants. Kenneth A. Bauer
 New Anticoagulants Kenneth A. Bauer Traditional anticoagulant drugs, including unfractionated heparin and warfarin, have several limitations. New anticoagulants have been developed that target a single
New Anticoagulants Kenneth A. Bauer Traditional anticoagulant drugs, including unfractionated heparin and warfarin, have several limitations. New anticoagulants have been developed that target a single
Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation
 Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation Ayesha Ather, PharmD, BCPS College of Pharmacy, Adjunct Assistant Professor University of Kentucky Faculty Disclosure I have
Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation Ayesha Ather, PharmD, BCPS College of Pharmacy, Adjunct Assistant Professor University of Kentucky Faculty Disclosure I have
Procedure for the prescribing and administration of Low Molecular Weight Heparins
 Procedure for the prescribing and administration of Low Molecular Weight Heparins Author: Lilian Baxendale Designation: Pharmacist Version: 1c Date: March 2013 Date Approved: 17 th May 2013 Approved By:
Procedure for the prescribing and administration of Low Molecular Weight Heparins Author: Lilian Baxendale Designation: Pharmacist Version: 1c Date: March 2013 Date Approved: 17 th May 2013 Approved By:
