Hematology. Presented by: Karen Marzlin DNP, RN, CCNS, CCRN, CMC Cynthia WebnerDNP, RN, CCNS, CCRN, CMC CNEA / Key Choice 1.
|
|
|
- Darren Banks
- 5 years ago
- Views:
Transcription
1 Hematology Presented by: Karen Marzlin DNP, RN, CCNS, CCRN, CMC Cynthia WebnerDNP, RN, CCNS, CCRN, CMC 2012 CNEA / Key Choice 1 Just a Thought Link your roots deeply into whatever task you are doing, for commitment and enthusiasm transform monotony into freshness and routine into joy and discovery
2 Hematology and Immunology Overview 3 Assessment of Hematological System CBC RBC WBC HG HCT Platelets Retriculocyte Count Serum Iron Ferritin Transferrin Total Iron Binding Capacity PT PTT INR 4 2
3 Bone Marrow Production of: Hematologic System Erythrocytes Leukocytes Granulocytes Agranulocytes Thrombocytes 5 Hematologic System Spleen (Red Pulp) Stores and releases RBCs 100 cc in response to SNS Filtering and destruction of damaged or old erythrocytes Pitting Catabolizes hemoglobin / iron returned to bone marrow Storage and release of platelets Destruction of damaged platelets Spleen (white pulp) Production of lymphocytes 6 3
4 Hematologic System Liver Filtering of blood from GI tract Conversion of bilirubin (destruction of RBCs) to bile Detoxification of toxic substances that enter blood Manufacturing of some clotting factors and of thrombin Storage of blood Storage of iron 7 Hematologic System Lymphatic system Lymph Composition Lymphocytes, granulocytes, macrophages, enzymes, antibodies Deficient in platelets and fibrinogen Function Returns excess interstitial fluid (hormones) to blood Returns protein and fat from GI tract Lymph circulation Capillaries larger than blood capillaries Ducts drain to subclavian vein Lymph Nodes Function Filter / allow WBCs to phagocytosize bacteria 8 4
5 Blood Hematologic System Plasma 55% of total blood volume Blood Cells Erythrocytes Stoma location of hemoglobin attachment / contains antigens that determine blood type Reticulocytes immature red blood cells / elevated in hemorrhage» 1 to 4 days to mature Leukocytes 9 Hematologic System Erythrocytes Function Oxygen transport Acid base balance Types Erythropoiesis Secreted by kidney Stimulate bone marrow Destruction Liver and spleen remove damaged RBCs Hemoglobin / iron returned to bone marrow Leukocytes Cytokines Protein hormones Synthesized by leukocytes Granulocytes Neutrophils Eosinophils Basophils Agranulocytes Mononuclear phagocytes Lymphocytes
6 Hematologic System Granulocytes (polymorphic nucluer) Active phagocytes Neutrophils (40-80% of WBC mass) leave blood vessel and migrate through tissues and search for microroganism or old body cells (engulf, kills and digest them: phagocytosis). Dies after phagocytosis producing pus. Bands are immature neutrophils; increase in bands in acute infection is a shift to the left Segmented neutrophils are mature Eosinophils most important during parasytic infection and allergic rx (0-5% of WBCs) Basophils (0-2%) allergic rxs, no phagocytosis Agranulocytes Mononuclear phagocytes (monocytes) differentiate into macrophages as they migrate into tissues, macrophages not measured in WBC count; involved in removal of mutant cancer cells Lymphocytes (10-40% of WBC mass) all involved in immunity 11 Immune System Innate (natural) Immunity Macrophages Neurtophiles Eosinophiles Basophiles Mast Cells Natural killer cells Aquired (adapted) Immunity B Lymphocytes IgG IgA IgM IgE IgD T Lymphocytes T Helper cells (T4 Cells) T Cytotoxic cells T Memory cells T Supressor cells (T8 Cells)
7 Immune System B Cells (Antibodies) (Humeral Immunity) Originate in bone marrow Stored in the lymph Released in the blood Functions Neutralizing bacterial toxins and viruses Promoting phagocytosis Activating component of the inflammatory response T Cells (Cell Mediated Immunity) Originate in the thymus 13 Coagulation
8 Thrombus Formation 15 Another Look at Thrombus
9 Clot Formation Clotting Cascade Intrinsic Initiated by vascular injury and direct exposure to collagen From initiation to a clot is 2-6 minutes Measured by APTT Extrinsic pathways Initiated by endothelial release of tissue factor From initiation to clot is 15 to 20 seconds Measured by Protime A clot can be produced by activation of either the intrinsic or extrinsic pathway. 17 The Clotting Cascade The Common Pathway Prothrombin is converted to thrombin Thrombin permits fibrinogen to be converted to fibrin Result is fibrin stable clot (red clot) This fibrin stable clot is cause of STEMI MI
10 The Clotting Cascade 19 The Role of Platelets
11 The Role of Platelets Platelet aggregation can be large enough to form a platelet plug or a white clot that seals a damaged vessel This white clot is primary culprit in unstable angina 21 The Role of Platelets Platelets release components necessary for the clotting process in the Intrinsic Pathway Platelets contain a fibrin stabilizing factor which is important in the final stage of the Common Pathway prior to stable clot formation
12 The Role of Platelets Platelets cross link with fibrinogen via the GP IIb/IIIa receptors to form a fibrin mesh which gives a clot more substance 23 Drugs Used to Alter Clotting Fibrinolytics Anticoagulants Antiplatelets
13 Fibrinolytics: Physiology After a clot is formed blood or tissue plasminogen activators changes plasminogen to plasmin Plasmin works to lyse fibrin clots and degrade circulating fibrinogen therefore producing fibrin split products Fibrin split products further inhibit fibrin formation This occurs spontaneously to produce reperfusion, however generally this falls outside window of opportunity to limit damage Fibrinolytics speed up this process by providing tissue plasminogen activator 25 Fibrinolytics Streptokinase (Kabikinase, Streptase) bolus followed by infusion, non weight based Urokinase (Abbokinase) bolus followed by infusion, weight based Alteplase,tPa (Activase) (Tissue Plasminogen Activator) no bolus, non weight based APSAC (anisoylated plasminogen streptokinase activator complex) (Retaplase) Retavase double bolus injection; non weight based Tenecteplase (TKNase) - single bolus; weight based
14 Contraindications for Fibrinolytic Therapy Absolute Active internal bleeding Suspected aortic dissection Known intracranial neoplasm History of any hemorrhagic CVA Any cerebral vascular event within the year 27 Contraindication for Fibrinolytic Therapy Relative Prolonged or traumatic CPR > 10 minutes Severe hypertension > 180 / 110 Chronic severe hypertension History prior CVA or other intracranial pathology Recent trauma or other major surgery Noncompressible vascular punctures Recent internal bleeding Prior exposure for Streptokinase or APSAC Known bleeding disorder or current INR >
15 Anticoagulants Unfractionated Heparin Low Molecular Weight Heparin Direct Thrombin Inhibitors Factor Xa Inhibitors Warfarin (Coumadin) 29 A Closer Look at Heparin Prevents conversion of prothrombin to thrombin by binding to antithrombin III Antithrombin III naturally inhibits thrombin; when heparin binds with it the inhibition is increased 1000 times Neutralizes the clotting capabilities of thrombin Works in the intrinsic and common pathway Also Inhibits platelets (thrombin is most potent platelet stimulator) Anticoagulation is almost instant ½ life relatively short Antidote: Protamine 1 mg per 100 units
16 More About Heparin aptt (activated partial thromboplastin time) is used to monitor effectiveness and safety Goal is aptt 1.5 Xs the control Weight based heparin dosing reaches goal 90% of time compared to 77% with standard therapy Baseline aptt, PT/INR, platelets and CBC Increased bleeding can occur with renal failure Heparin has dual clearance mechanism but greater effect on platelet function than LMWH 31 Complications of Heparin Bleeding Mild thrombocytopenia Mild thrombocytopenia occurs in 10-20% of patients Severe thrombocytopenia occurs in 1-2% of patients Platelet aggregation resulting in venous or arterial thrombosis Determining patients at risk is unpredictable Generally occurs 5 to 10 days after initiation of heparin DC heparin if platelets fall below 100,000 Severe thrombocytopenia is due to an immune response (HITTS) No additional heparin including line flushes
17 More on HIT Heparin dependent platelet activating antibodies Recognize a self protein (platelet factor 4: PF4) that is bound to heparin This results in platelet activation and increased thrombin generation 33 A Closer Look at Low Molecular Weight Heparin Low Molecular Weight Heparin (Lovenox) Enoxaprin, dalteparin, tinzaparin, and nadroparin Smaller in size Antithrombin by inhibiting factor Xa Causes less inactivation of thrombin and less inhibition of platelets and less bleeding than standard heparin Does not significantly influence bleeding time Anti Xa levels can be drawn 4 hours after SQ dose Renal failure results in increased risk of bleeding because LMWH is renally cleared Special dosing for chronic renal insufficiency with enoxaparin
18 Benefit of Low Molecular Weight Heparin over Unfractionated Heparin More predictable anticoagulant response Lower incidence of heparin induced thrombocytopenia Lower incidence of osteoporosis No need to monitor APTT Less platelet activation Can be self administered with Sub Q administration ½ life 4-6 hours Protamine reverses 60% of drug effect 35 Administration of Enoxaparin Full length of 27 gauge ½ needle (prepackaged) should be injected Skin fold held until needle withdrawn Use anterolateral or posterorlateral walls of abdomen Rotate sites frequently Do not massage site Prevention of DVT 30 mg BID or 40 mg daily 40 mg daily in most situations Venous thrombosis / DVT 1mg/kg BID or 1.5 mg/kg daily depending of specific circumstances Unstable Angina / NSTEMI (or as adjunct in STEMI) 1 mg/kg BID IV dosing can be used in STEMI Embolism with Atrial Fib 1 mg/kg BID Dosing adjustments are required in several renal impairment
19 Direct Thrombin Inhibitor Indicated for patients with HITTS Approved in Non STEMI guidelines and for PCI Ability to inactivate fibrin bound thrombin Less binding to plasma proteins, therefore more reliable anticoagulation effect Examples Lipirudin and desirudin (hirudin) Argatroban Bivalirudin* (Angiomax) 37 Synthetic Factor Xa Inhibitor Fondaparinux (Arixtra) Used for venous thromboembolism and PE Approved for DVT prophylaxis in certain surgical patients Recently approved and added to NonSTEMI Guidelines Cannot be used as sole anticoagulant during PCI Neutralizes Factor Xa and interrupts the clotting cascade Does not inhibit thrombin No reported HIT Sub Q injection Once daily dosing (fixed dose can cover a range of body weights lower dose for low body weight) Contraindicated in severe renal dysfunction No laboratory monitoring No antidote (Recombinant factor VIIa can help reverse anticoagulation effect)
20 A Closer Look at Coumadin Inhibits the synthesis of prothrombin. Acts indirectly through the liver by altering the synthesis of vitamin K dependent factors in the extrinsic pathway. The vitamin K dependent factors are left biologically inactive. It takes 4-5 days to reach a therapeutic level. Can have initial transient hypercoagulable state Must be overlapped with heparin 39 More About Coumadin PT (prothrombin time monitored to evaluate effectiveness and safety) PT problems with standardization of anticoagulation intensity INR (International Normalized Ratio) relates the patients PT to the intensity of actual coagulation. Dosing Start with 5mg per day Loading doses not recommended PT / INR daily until therapeutic level reached Dosage may need adjusted after 4-6 days due to individual sensitivity PT / INR twice weekly for 2 weeks and weekly for two months PT / INR every 4-6 weeks after dose stable
21 More About Coumadin Goal for INR of is adequate in most situations INR of is goal for mechanical prosthetic valves and prevention of recurrent MI Chronic condition require lifelong therapy Acute conditions (PE, DVT) usually require at least six months of therapy 41 Nursing Considerations with Coumadin Many many drugs interact with coumadin to alter PT Consistency in diet is important especially with known high vitamin K foods (green vegetables) Antidote: Vitamin K Fresh frozen plasma if severe hemorrhage Recombinant factor VIIa is also an option for life threatening bleeding Patient compliance is critical
22 Dabigatran Oral direct thrombin (factor IIa) inhibitor Is a prodrug (dabigatranetexilate) that is converted in liver to active form Peak plasma levels in 1.5 hours; half-life hours Eliminated mostly by kidneys (reduced dose for moderate renal failure, not recommended in severe renal failure) No known reversal agent Predictable dose-response relationship so no lab monitoring of coagulation status needed Dose: 110 mg PO bid (shown not inferior to warfarin) or 150 mg PO bid (shown superior to warfarin) 43 Dabigatran Study results compared to warfarin: Rate of bleeding less than warfarin with 110 mg dose and about the same with 150 mg dose of dabigatran One area of concern GI Bleed Hemorrhagic stroke significantly lower with dabigatran Indicated for reduction of stroke in patients with AF at intermediate or high risk of stroke. Specific patient considerations Can t or won t comply with warfarin monitoring requirements Have inconsistent response to warfarin Take multiple medications that can interact with warfarin
23 Rivaroxaban Oral direct factor Xa inhibitor Maximum plasma level in 3 hours Half-life 4-9 hours (up to 12 hrs if > 75 years old) Dose 10 mg PO daily Few drug interactions Excreted by kidneys (contraindicated in severe renal failure) Predictable dose-response relationship so no lab monitoring needed Approved firstly in Europe and Canada for prevention of VTE after hip and knee surgery 45 Rivaroxaban ROCKET AF Double-blind randomized trial 14,264 patients with nonvalvular atrial fibrillation (at increased risk for stroke) Rivaroxaban (at a daily dose of 20 mg) or doseadjusted warfarin. P<0.001 for noninferiority of rivaroxaban no significant between-group difference in the risk of major bleeding, although intracranial and fatal bleeding occurred less frequently in the rivaroxaban group
24 GP IIb/ IIIa Inhibitors Antiplatelet Drugs ADP Antagonists Thromboxane A 2 Inhibitor 47 A Closer Look at Antiplatelet Drugs: GP IIb/IIIa Inhibitors GP IIb/IIIa Inhibitors Eptifibitide (Integrelin) Tirofiban (Aggrastat) Abciximab (Repro) Inhibit the glycoprotein protein IIb/IIIa receptors which platelets and fibrinogen bind with to form the fibrin mesh
25 More about GP IIb / IIIa Inhibitors Glycoprotein 2b / 3a receptors are most abundant protein on the platelet surface. It is tightly packed on the platelet surface with about 80,000 receptors per platelet. Primary receptor for platelet aggregation. Fibrinogen links to these receptors and simultaneously binds receptors on two separate platelets. Platelet cross-linking occurs leading to platelet aggregation. 49 A Closer Look at ADP Inhibitors: A Type of Thienopyridine Clopidogrel (Plavix) Prasugrel (Effient) Inhibit ADP which is released by platelets. ADP enhances adhesiveness and aggregation of platelets by activating GPIIb/ IIIa receptors. Concern with Proton Pump Inhibitors Resistance concern Triton TIMI 38 Inhibit ADP which is released by platelets. ADP enhances adhesiveness and aggregation of platelets by activating GPIIb/ IIIa receptors. Greater anti-ischemic protection (compared to clopidogrel) Increased bleeding risk Not able to use with prior stroke or TIA, small body size, or advanced age Able to give with PPIs
26 Ticagrelor (Brillinta) Better anti-ischemic effect compared to clopidogrel No significant increase in major bleeding PLATO trial Faster onset and shorter duration than clopidogrel(known as reversible mode of action) BID dosing is a potential concern for compliance Although shorter ½ life recommendation to be held 5 days before surgery. Cannot be given with more than 100 mg ASA daily. 51 ASA A Closer Look at Aspirin Inhibits Thromboxane A2 which is released with vascular injury. Platelet reactivity is diminished. Also inhibits the endothelium s production of prostaglandin I 2 which decreases platelet aggregation and induces vasodilation. Caution with asthma
27 Pathophysiology 53 Disseminated Intravascular Coagulation (DIC ) A syndrome characterized by thrombus formation and hemorrhage secondary to over stimulation of the normal coagulation process and resultant consumption of clotting factors and platelets
28 DIC Etiology Always secondary (Massive transfusion, vascular disorders, infection, sepsis, trauma) Pathophysiology Paradox Bleeding after clotting Results of clotting Clotting causes ischemia, tissue necrosis and micro clots Results of bleeding Bleeding causes loss of hemoglobin and 02 carrying capacity Fibrinolysis Fibrin split products act as anticoagulants (interfere with platelet function and thrombin) 55 DIC Diagnostics Platelet count < 150,000 PT > 40 sec PTT > 70 sec Thrombin time > 15 sec Fibrinogen level (decrease by 50% or < 200) Antithrombin III (decreased) Fibrin split products (usually > 40) D Dimer > 250 D Dimer more specific end product of fibrin degredation Protamine sulfate test: Strongly positive Added to plasma to see if fibrin strands form, if + there is an excessive amount of thrombin
29 DIC Treatment Only effective treatment: Underlying Cause System management Heparin (PTT) rarely if thrombosis is going to lead to mortality Clotting Factors (downside) Platelets FFP Hemostatic cofactors VitK and Folic Acid Amicar** Antifibrinolytic agent Only if primary fibrinolysis is present; otherwise fatal Thrombin gauze, ice packs, pressure dressings Complications 57 Immune Thrombocytopenic Purpura Pathophysiology: Platelets are coated with autoantibodies to platelet membrane antigens this results in splenic sequestration platelets are removed by phagocytosis by macrophages. Life span of platelets are shortened Typical autoantibody is immunoglobulin G (IgG) Binds with platelet GP
30 Immune Thrombocytopenic Purpura Spleen is major organ of involvement Platelet autoantibodies are formed in the white pulp Mononuclear macrophages in the red pulp destroy the affected platelets 59 Thrombocytopenic Purpura Other Causes Systemic lupus erythematosus Acute or chronic leukemia. Myelodysplastic syndrome, particularly in patients older than 60 years. Post viral illness HIV Drug reaction Major Nursing Goal Maintain safe environment
31 Thrombocytopenic Purpura Platelets less than 100,000 / mm 3 Petecchiae Ecchymosis Epitaxis Bleeding gums Menorrhagia GI Bleeding Platelets less than 20,000 / mm 3 Severe GI hemorrhage Severe GU hemorrhage Cerebral hemorrhage 61 Final Thought Learning is a journey Each new discovery leads to a better understanding of previously learned information and opens the opportunity for unlimited future discoveries
Hemostasis/Thrombosis IV
 Hemostasis/Thrombosis IV Antithrombotic Therapy Antithrombotic Therapy Mainstay of battle against thromboembolic disease Hot area of new drug research Cannot inhibit clot formation without increased risk
Hemostasis/Thrombosis IV Antithrombotic Therapy Antithrombotic Therapy Mainstay of battle against thromboembolic disease Hot area of new drug research Cannot inhibit clot formation without increased risk
Lina Al-Lawama. Rama Al-Ashqar. Malik Al-Zohlof
 2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
2 Lina Al-Lawama Rama Al-Ashqar Malik Al-Zohlof Anticoagulant drugs Recap Last lecture we were talking about antiplatelet drugs, we mentioned 5 drugs : Aspirin which is used alone with patents that have
Pharmacology Lecture 5. Anticoagulants
 Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Pharmacology Lecture 5 Anticoagulants General overview Anti-thrombotic Drugs Antiplatlets Anticoagulants Fibrinolytics Anticoagulants Indirect Thrombin Inhibitors Anti-thrombotic effect is exerted by interaction
Session 1 Topics. Vascular Phase of Hemostasis. Coagulation Pathway. Action of Unfractionated Heparin. Laboratory Monitoring of Anticoagulant Therapy
 ~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
~~Marshfield Labs Presents~~ Laboratory Monitoring of Anticoagulant Therapy Session 1 of 4 Session 1 Topics Review of coagulation and the vascular phase of hemostasis Unfractionated heparin Low molecular
ANTICOAGULANT THERAPY ANTICOAGULANT THERAPY REVISITED Thrombosis is a complication of underaggressive anticoagulant therapy
 ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED 2004 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
Bivalirudin (Angiomax ) vs. Heparin during Peripheral Vascular Interventions: Which is Better and How to Decide?
 Bivalirudin (Angiomax ) vs. Heparin during Peripheral Vascular Interventions: Which is Better and How to Decide? Vinod Nair MD FACC FSCAI Cardiovascular Ins6tute of the South, Houma Financial Disclosure:
Bivalirudin (Angiomax ) vs. Heparin during Peripheral Vascular Interventions: Which is Better and How to Decide? Vinod Nair MD FACC FSCAI Cardiovascular Ins6tute of the South, Houma Financial Disclosure:
Local vasoconstriction. is due to local spasm of the smooth muscle (symp. reflex) can be maintained by platelet vasoconstrictors
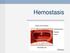 Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Hemostasis Hemostasis ( hemo =blood; sta= remain ) is the stoppage of bleeding, which is vitally important when blood vessels are damaged. Following an injury to blood vessels several actions may help
Adv Pathophysiology Unit 4 Page 1 of 10. Learning Objectives for this file:
 Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
Adv Pathophysiology Unit 4 Page 1 of 10 Learning Objectives for this file: Topics include structure & function of: 1. Coagulation process platelets, clotting factors 2. Coagulation cascade formation of
UW Medicine Alternative Monitoring for Antithrombotic Agents
 Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
Tags: monitoring alternative monitoring SUMMARY OF ANTICOAGULATION LAB TESTS AT UWMedicine Description Order Code Specimen Collection Availability Turn-Around Time Anti Xa Based Tests antixa for heparin
Drugs used in Thromboembolic Disease. Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014
 Drugs used in Thromboembolic Disease Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014 Drugs used in Thromboembolic Disease Anticoagulants: Heparin. Oral anticoagulants.
Drugs used in Thromboembolic Disease Munir Gharaibeh, MD, PhD, MHPE Department of Pharmacology Faculty of Medicine October 2014 Drugs used in Thromboembolic Disease Anticoagulants: Heparin. Oral anticoagulants.
Veins Valves prevent engorgement and backflow. Baroreceptor reflex. Veins returning blood
 Veins have large radii and low resistance. Walls are thin, not elastic Most blood volume is in veins Veins returning blood Veins Valves prevent engorgement and backflow Sympathetic NS constricts veins
Veins have large radii and low resistance. Walls are thin, not elastic Most blood volume is in veins Veins returning blood Veins Valves prevent engorgement and backflow Sympathetic NS constricts veins
Heparin Induced Thrombocytopenia. Heparin Induced Thrombocytopenia. Heparin Induced Thrombocytopenia. Temporal Aspects.
 Heparin Induced Eric Kraut, MD Professor of Internal Medicine The Ohio State University Medical Center Heparin Induced Heparin induced thrombocytopenia occurs in up to 5 % of patients receiving unfractionated
Heparin Induced Eric Kraut, MD Professor of Internal Medicine The Ohio State University Medical Center Heparin Induced Heparin induced thrombocytopenia occurs in up to 5 % of patients receiving unfractionated
Physiology Unit 3 HEMATOLOGY
 Physiology Unit 3 HEMATOLOGY In Physiology Today Hematocrit Percentage of blood volume that is erythrocytes 45% in men 42% in women Average blood volume in is 5 L Plasma Large amounts of organic/inorganic
Physiology Unit 3 HEMATOLOGY In Physiology Today Hematocrit Percentage of blood volume that is erythrocytes 45% in men 42% in women Average blood volume in is 5 L Plasma Large amounts of organic/inorganic
ANEMIA. Oral iron. IV iron gluconate (order set #233)
 PREVENTION ANEMIA Oral iron IV iron gluconate (order set #233) TRANSEXAMIC ACID Efficacy of IV TXA in Reducing Blood Loss After Elective C-section: Prospective, Randomized, Double-blind, Placebo Controlled
PREVENTION ANEMIA Oral iron IV iron gluconate (order set #233) TRANSEXAMIC ACID Efficacy of IV TXA in Reducing Blood Loss After Elective C-section: Prospective, Randomized, Double-blind, Placebo Controlled
Managing Coagulation Abnormalities Linda Liu, M.D.
 Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
Managing Coagulation Abnormalities Professor UCSF Dept of Anesthesia UC SF 1 Difficult Task Coagulation Abnormalities 30 minutes Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban UC SF 2 UC
Update on the Direct Oral Anticoagulants (DOACs)
 Update on the Direct Oral Anticoagulants (DOACs) J. Randle Adair DO, PhD Internal Medicine New Mexico Cancer Center & Co-Chair, Anticoagulation Subcommittee Presbyterian Healthcare Services (PHS) Attending,
Update on the Direct Oral Anticoagulants (DOACs) J. Randle Adair DO, PhD Internal Medicine New Mexico Cancer Center & Co-Chair, Anticoagulation Subcommittee Presbyterian Healthcare Services (PHS) Attending,
Managing the Risks Associated with Anticoagulant Therapy. Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde
 Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Managing the Risks Associated with Anticoagulant Therapy Steve McGlynn Specialist Principal Pharmacist (Cardiology) NHS Greater Glasgow and Clyde Background Identified as high risk medicines Wide range
Ch 13: Blood. What does blood do? Transport: Regulation: Protection:
 Ch 13: Blood What does blood do? Transport: Regulation: Protection: SLOs Describe the composition of plasma and list the major functions of plasma proteins. Map hematopoiesis, starting from a pluripotent
Ch 13: Blood What does blood do? Transport: Regulation: Protection: SLOs Describe the composition of plasma and list the major functions of plasma proteins. Map hematopoiesis, starting from a pluripotent
Continuing Education for Pharmacists
 Continuing Education for Pharmacists Oral anticoagulation without protimes: A review of two emerging agents that may come to market. Lindsay Davis, Pharm.D. (Acute Care Pharmacy Resident, Phoenix VA Medical
Continuing Education for Pharmacists Oral anticoagulation without protimes: A review of two emerging agents that may come to market. Lindsay Davis, Pharm.D. (Acute Care Pharmacy Resident, Phoenix VA Medical
ANTICOAGULANT THERAPY ANTICOAGULANT THERAPY REVISITED 2005
 ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY One of most common treatments in hospital & out 2 nd most
ANTICOAGULANT THERAPY REVISITED Thrombosis is a complication of underaggressive anticoagulant therapy ANTICOAGULANT THERAPY.
 ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY Goals of Therapy PREVENTION OF THROMBOEMBOLISM!!! Stop propagation
ANTICOAGULANT THERAPY REVISITED 2005 or, Which one(s) of these (#$%$#!@#^) drugs should be the one(s) I use, and for what? ANTICOAGULANT THERAPY Goals of Therapy PREVENTION OF THROMBOEMBOLISM!!! Stop propagation
Veins Valves prevent engorgement and backflow. Baroreceptor reflex. Veins returning blood
 Veins have large radii and low resistance. Walls are thin, not elastic Most blood volume is in veins Veins returning blood Veins Valves prevent engorgement and backflow Sympathetic NS constricts veins
Veins have large radii and low resistance. Walls are thin, not elastic Most blood volume is in veins Veins returning blood Veins Valves prevent engorgement and backflow Sympathetic NS constricts veins
Coagulation Mechanisms Dr. Nervana Bayoumy
 Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Coagulation Mechanisms Dr. Nervana Bayoumy Associate Professor Department of Physiology Objectives At the end of this lecture you should be able to: 1. Recognize the different clotting factors 2. Understand
Index. Autoimmune thrombocytopenic purpura (AITP), 100, 102, 105, 108, 187 Automated platelet counters, , 108
 A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
A Accuracy, 6, 7, 15, 46, 52, 53, 61, 75, 100, 143, 144, 149, 166, 176, 178 Acquired coagulation disorders, 111 115 Acquired platelet disorders, 99 108 ACT. See Activated clotting time (ACT) Activated
New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D.
 New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D. Professor of Cardiovascular Medicine University of Maryland School of Medicine Copyright A.P. Wheeler 2009
New Insights into the Diagnosis & Management of Venous Thromboembolism (VTE) Michael Miller, M.D. Professor of Cardiovascular Medicine University of Maryland School of Medicine Copyright A.P. Wheeler 2009
Using TEG in the ED, OR, and ICU. Don H. Van Boerum, MD, FACS
 Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
Using TEG in the ED, OR, and ICU Don H. Van Boerum, MD, FACS Trauma Surgeon, Director of Surgical Critical Care, Co-Director of Shock Trauma ICU, Intermountain Medical Center, Intermountain Healthcare
Antithrombotic Therapies: Parenteral Agents
 Antithrombotic Therapies: Parenteral Agents Christine A. Sorkness, Pharm.D. Professor of Pharmacy & Medicine (CHS) UW School of Pharmacy Clinical Pharmacist, Anticoagulation Clinic, Wm S. Middleton VA
Antithrombotic Therapies: Parenteral Agents Christine A. Sorkness, Pharm.D. Professor of Pharmacy & Medicine (CHS) UW School of Pharmacy Clinical Pharmacist, Anticoagulation Clinic, Wm S. Middleton VA
The Cardiovascular System: Blood
 The Cardiovascular System: Blood The Functions of Blood General Overview Provides a system for rapid transport within the body Nutrients Hormones Waste products Respiratory gases Cells & Blood Components
The Cardiovascular System: Blood The Functions of Blood General Overview Provides a system for rapid transport within the body Nutrients Hormones Waste products Respiratory gases Cells & Blood Components
Anticoagulation in VTE The Haematologist s Perspective. Dr. M.D. Maina FRCP Edin.
 Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Anticoagulation in VTE The Haematologist s Perspective Dr. M.D. Maina FRCP Edin. Disclosures None The coagulation process that leads to haemostasis involves a complex set of reactions involving approximately
Hematology Emergencies: Problems with Platelets
 Hematology Emergencies: Problems with Platelets Christian Cable, MD, FACP Associate Professor of Medicine Division of Hematology & Oncology Texas A&M HSC College of Medicine Scott & White Healthcare Fundamentals
Hematology Emergencies: Problems with Platelets Christian Cable, MD, FACP Associate Professor of Medicine Division of Hematology & Oncology Texas A&M HSC College of Medicine Scott & White Healthcare Fundamentals
Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015
 + Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
+ Management of Bleeding in the Anticoagulated Patient Short Snappers CSIM 2015 Elizabeth Zed, MD, FRCPC October 17, 2015 + Disclosures Off label use of PCC and apcc will be discussed My centre participates
Platelet type bleeding: (vwd) - Petechiae, purpura, ecchymoses, bruising - Menorrhagia, hematuria, occult GI bleed - Gingival bleeding, epistaxis
 1 Nadanotes.com 2 Nadanotes.com 3 Nadanotes.com Platelet type bleeding: (vwd) - Petechiae, purpura, ecchymoses, bruising - Menorrhagia, hematuria, occult GI bleed - Gingival bleeding, epistaxis Clotting
1 Nadanotes.com 2 Nadanotes.com 3 Nadanotes.com Platelet type bleeding: (vwd) - Petechiae, purpura, ecchymoses, bruising - Menorrhagia, hematuria, occult GI bleed - Gingival bleeding, epistaxis Clotting
iccnet CHSA Clinical Protocol - HEPARIN
 Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
Name: iccnet CHSA Clinical Protocol - HEPARIN This clinical guideline or clinical protocol is based on a review of best practice evidence and expert opinion. It is intended to guide practice and does not
Physician Orders - Adult
 Physician Orders - Adult attach patient label here Title: Direct Thrombin Inhibitor (DTI) Protocol Orders Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy
Physician Orders - Adult attach patient label here Title: Direct Thrombin Inhibitor (DTI) Protocol Orders Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY
 LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
LABORATORY APPROACH TO BLEEDING DISORDERS DR NISHANTH PG 1 ST YEAR DEPARTMENT OF PATHOLOGY 1 WHEN IS THE LAB REQUIRED TO INVESTIGATE FOR A POSSIBLE BLEEDING DISORDER? Clinically suspected bleeding tendency
If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom
 If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom Heparin Discovered 1916, commercial available 1935 Heparin Is there an alternative, not really
If not heparin for bypass then what? Dr Tony Moriarty Consultant Cardiac Anaesthetist Birmingham United Kingdom Heparin Discovered 1916, commercial available 1935 Heparin Is there an alternative, not really
Manual of Interventional Cardiology
 770 Manual of Interventional Cardiology Table 34.5. Comparison of Low-Molecular-Weight Heparins to Unfractionated Heparin Characteristic Unfractionated Heparin LMW Heparins Composition Heterogenous mixture
770 Manual of Interventional Cardiology Table 34.5. Comparison of Low-Molecular-Weight Heparins to Unfractionated Heparin Characteristic Unfractionated Heparin LMW Heparins Composition Heterogenous mixture
Novel Anti-coagulant Agents. David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan
 Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Novel Anti-coagulant Agents David G Hovord BA MB BChir FRCA Clinical Assistant Professor University of Michigan Objectives Provide an overview of the normal coagulation, including perioperative testing
Laboratory Monitoring of Anticoagulation
 Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
Michael Smith, Pharm. D., BCPS, CACP East Region Pharmacy Clinical Manager Hartford HealthCare Learning Objectives Explain the role of common laboratory tests used in monitoring of anticoagulation therapy.
Laboratory investigation in the Bleeding Patient. Dr Craig Taylor Consultant Haematologist May 2016
 Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
Laboratory investigation in the Bleeding Patient Dr Craig Taylor Consultant Haematologist May 2016 Introduction Bleeding is common May consume significant resources Crossmatched blood Lab results may be
New Anticoagulants Linda Liu, M.D.
 Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
Difficult Task New Anticoagulants Professor UCSF Dept of Anesthesia 15 minutes! Emphasis on 2 new oral anticoagulants Dabigatran Rivaroxaban Relation to anesthesia Rapid reversal Regional anesthesia UC
TSOAC Case Study 1. Question. TSOAC Case Study 1 Continued
 TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
TSOAC Case Study 1 An otherwise healthy 56-year-old man presents to the emergency department with left leg pain and swelling for the last 3 days. Compression ultrasonography confirms left common femoral
General Principles of. Hemostasis. Kristine Krafts, M.D.
 General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
General Principles of Hemostasis Kristine Krafts, M.D. Hemostasis is a balancing act! pro-ting plugs up holes in blood vessels anti-ting keeps ting under control Pro-Clotting Pro-Clotting vessels platelets
Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation
 Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation Ayesha Ather, PharmD, BCPS College of Pharmacy, Adjunct Assistant Professor University of Kentucky Faculty Disclosure I have
Pharmacotherapy Management in Patients with Extracorporeal Membrane Oxygenation Ayesha Ather, PharmD, BCPS College of Pharmacy, Adjunct Assistant Professor University of Kentucky Faculty Disclosure I have
Coagulopathy Case-2. Andy Nguyen, M.D. 2009
 Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
Coagulopathy Case-2 Andy Nguyen, M.D. 2009 CLINICAL HISTORY A 42 year-old man brought to the emergency room with severe burn. Patient was rescued by firemen in a serious fire. He had been found unconscious
Coagulation in perspective: Blood management. Objectives
 Coagulation in perspective: Blood management Julie Wegner, PhD jawrbl@gmail.com Objectives To gain a basic understanding of the following: 1. Coagulation components and processes Why patients bleed. 2.
Coagulation in perspective: Blood management Julie Wegner, PhD jawrbl@gmail.com Objectives To gain a basic understanding of the following: 1. Coagulation components and processes Why patients bleed. 2.
Chapter 19b Blood, cont d
 Chapter 19b Blood, cont d White Blood Cells WBCs account for less than 1% of blood volume. There are two major histological categories of WBCs the granulocytes and the agranulocytes. GRANULOCYTES are Basophils,
Chapter 19b Blood, cont d White Blood Cells WBCs account for less than 1% of blood volume. There are two major histological categories of WBCs the granulocytes and the agranulocytes. GRANULOCYTES are Basophils,
Omar A. Elkashef, MD
 DVT Prophylaxis in Orthopedic Surgery By Omar A. Elkashef, MD Kasr Al- aini About VTE Venous thromboembolism encompasses deep vein thrombosis (DVT) and pulmonary embolism VTE is common and PE is a potentially
DVT Prophylaxis in Orthopedic Surgery By Omar A. Elkashef, MD Kasr Al- aini About VTE Venous thromboembolism encompasses deep vein thrombosis (DVT) and pulmonary embolism VTE is common and PE is a potentially
ROZAIMAH ZAIN-HAMID. Department of Pharmacology and Therapeutics Faculty of Medicine, Universitas Sumatera Utara
 ROZAIMAH ZAIN-HAMID Department of Pharmacology and Therapeutics Faculty of Medicine, Universitas Sumatera Utara Drugs Used in Disorders of Coagulation Fibrinolytic drugs Anti-thrombotic thrombotic drugs
ROZAIMAH ZAIN-HAMID Department of Pharmacology and Therapeutics Faculty of Medicine, Universitas Sumatera Utara Drugs Used in Disorders of Coagulation Fibrinolytic drugs Anti-thrombotic thrombotic drugs
Hypercoagulation. CP Conference 11/14/2006
 Hypercoagulation CP Conference 11/14/2006 Overview Hypercoagulation: poorly understood phenomena No definite cause is identified in > 40% of cases Three major factors in thrombus formation (Rudolf Virchow,
Hypercoagulation CP Conference 11/14/2006 Overview Hypercoagulation: poorly understood phenomena No definite cause is identified in > 40% of cases Three major factors in thrombus formation (Rudolf Virchow,
Heparin-Induced Thrombocytopenia and New Anticoagulants
 Heparin-Induced Thrombocytopenia and New Anticoagulants September 2004 Elizabeth M. Van Cott, MD Massachusetts General Hospital Boston MA College of American Pathologists 2004. Materials are used with
Heparin-Induced Thrombocytopenia and New Anticoagulants September 2004 Elizabeth M. Van Cott, MD Massachusetts General Hospital Boston MA College of American Pathologists 2004. Materials are used with
Platelet Factor IV- Heparin Antibodies. Presenter: Michael J. Warhol, M.D.
 Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
Platelet Factor IV- Heparin Antibodies Presenter: Michael J. Warhol, M.D. Learning Objectives Describe the mechanism of interaction between Heparin and Platelet Factor 4 Review the chemistry of Heparin
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides.
 These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
These handouts are only meant as a guide while you follow the presentation on the screen. Sometimes the speaker will change some of the slides. If you would like the 1 slide per page handouts, please ask
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Fragmin) Reference Number: CP.PHAR.225 Effective Date: 05.01.16 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Coding Implications Revision Log See Important Reminder
Clinical Policy: (Fragmin) Reference Number: CP.PHAR.225 Effective Date: 05.01.16 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Coding Implications Revision Log See Important Reminder
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues
 Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Evaluation of Complex Coagulation Cases: Case-Based Illustrations of Important Issues Kristi J. Smock, MD Associate Professor of Pathology University of Utah Health Sciences Center Medical Director, Hemostasis/Thrombosis
Direct anticoagulation therapy
 Direct anticoagulation therapy Pan-Arab Meeting & Saudi Society of Hematology Dr Ihab Alhemaidi MBBS MRCP(Lond UK) FRCPath. Fellow of the Royal Society of Medicine Consultant Adult hematology/bmt Section
Direct anticoagulation therapy Pan-Arab Meeting & Saudi Society of Hematology Dr Ihab Alhemaidi MBBS MRCP(Lond UK) FRCPath. Fellow of the Royal Society of Medicine Consultant Adult hematology/bmt Section
PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba
 VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba OVERVIEW Biochemistry of coagulation Pathogenesis of VTE
VENOUS THROMBOEMBOLISM PROPHYLAXIS IN THE ORTHOPEDIC PATIENT: Martin H. Ellis MD Hematology Institute and Blood Bank Meir Medical Center Kfar Saba OVERVIEW Biochemistry of coagulation Pathogenesis of VTE
3 : 34. Pankaj Manoria, P C Manoria, Bhopal
 3 : 34 Newer Antithrombins and anticoagulants Introduction Thrombosis is a leading cause of morbidity and mortality but for decades, anticoagulant therapy has usually consisted of unfractionate heparin
3 : 34 Newer Antithrombins and anticoagulants Introduction Thrombosis is a leading cause of morbidity and mortality but for decades, anticoagulant therapy has usually consisted of unfractionate heparin
Sign up to receive ATOTW weekly -
 BLOOD PHYSIOLOGY PART 2 ANAESTHESIA TUTORIAL OF THE WEEK 231 11 TH JULY 2011 Dr Karen Hayes Royal Devon & Exeter Correspondence to: kmhayes@hotmail.co.uk QUESTIONS Before continuing, try to answer the
BLOOD PHYSIOLOGY PART 2 ANAESTHESIA TUTORIAL OF THE WEEK 231 11 TH JULY 2011 Dr Karen Hayes Royal Devon & Exeter Correspondence to: kmhayes@hotmail.co.uk QUESTIONS Before continuing, try to answer the
DOACs: When and how to measure their anticoagulant effect
 DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
DOACs: When and how to measure their anticoagulant effect Stavroula Tsiara MD, PhD, FRCP Associate Professor of Internal Medicine University of Ioannina, Greece NOACs NOACs, TSOACs, DOACs (ISTH) Target
Personal Disclosure. The Coagulation Cascade. Learning Objectives. Unfractionated Heparin (UFH): Mechanism of Action. Heparin: Mechanism of Action
 Personal Disclosure Heparin/Low Molecular Weight Heparin and Fondaparinux Pharmacology and Pharmacotherapy Mary Jane E. Mattern PharmD Pharmacist William W. Backus Hospital There are no actual or potential
Personal Disclosure Heparin/Low Molecular Weight Heparin and Fondaparinux Pharmacology and Pharmacotherapy Mary Jane E. Mattern PharmD Pharmacist William W. Backus Hospital There are no actual or potential
Bevyxxa (betrixaban) NEW PRODUCT SLIDESHOW
 Bevyxxa (betrixaban) NEW PRODUCT SLIDESHOW Introduction Brand name: Bevyxxa Generic name: Betrixaban Pharmacological class: Factor Xa inhibitor Strength and Formulation: 40mg, 80mg; caps Manufacturer:
Bevyxxa (betrixaban) NEW PRODUCT SLIDESHOW Introduction Brand name: Bevyxxa Generic name: Betrixaban Pharmacological class: Factor Xa inhibitor Strength and Formulation: 40mg, 80mg; caps Manufacturer:
Antithrombosis Management for Pediatric VAD and Beyond
 Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
Antithrombosis Management for Pediatric VAD and Beyond Christina VanderPluym M.D. Director of Ventricular Assist Device and Cardiac Antithrombosis Program Boston Children s Hospital, USA Disclosures I
Bayer R&D Investor Day 2005
 Science For A Better Life HealthCare Bayer R&D Investor 25 December 8, 25 London Bayer R&D Investor 25 BAY 59-7939: A Novel, ral, Direct Factor Xa Inhibitor Frank Misselwitz Head of Therapeutic Area Cardiovascular,
Science For A Better Life HealthCare Bayer R&D Investor 25 December 8, 25 London Bayer R&D Investor 25 BAY 59-7939: A Novel, ral, Direct Factor Xa Inhibitor Frank Misselwitz Head of Therapeutic Area Cardiovascular,
Introduction Hemostasis: Tourniquet Test & Bleeding Time. Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO
 Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
Introduction Hemostasis: Tourniquet Test & Bleeding Time Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran LOGO Hemostasis A series of reactions that function to stop bleeding, maintaining
b. No intercellular fibers 1. Intracellular fluid (ICF) -- 2/3 of total 2. Extracellular fluids (ECF) 1/3 of total
 INTRODUCTION 2013 William A. Olexik Concept A. Tissue 1. Connective 2. Exceptional a. Only liquid tissue b. No intercellular fibers 3. Part of cardiovascular system B. Body Fluid 1. Intracellular fluid
INTRODUCTION 2013 William A. Olexik Concept A. Tissue 1. Connective 2. Exceptional a. Only liquid tissue b. No intercellular fibers 3. Part of cardiovascular system B. Body Fluid 1. Intracellular fluid
Analysis of the Anticoagulant Market
 MEDICAL DEVICES PHARMACEUTICALS CHEMICALS FOOD & BEVERAGE ELECTRONICS Analysis of the Anticoagulant Market VPG Publications, Consulting, Clients www.vpgcorp.com VPG Market Research Reports www.vpgmarketresearch.com
MEDICAL DEVICES PHARMACEUTICALS CHEMICALS FOOD & BEVERAGE ELECTRONICS Analysis of the Anticoagulant Market VPG Publications, Consulting, Clients www.vpgcorp.com VPG Market Research Reports www.vpgmarketresearch.com
Overview of Anatomy and Physioloy II Second Year Students
 University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad, Ph.D. Asaad Ismail Ahmad, Ph.D. Electrolyte and
University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad, Ph.D. Asaad Ismail Ahmad, Ph.D. Electrolyte and
Understanding the Hazards of Heparin
 Understanding the Hazards of Heparin 1 Contact Hours First Published: March 31, 2012 Course Revised: May, 2018 Course Expires: May 31, 2021 Reproduction and distribution of these materials is prohibited
Understanding the Hazards of Heparin 1 Contact Hours First Published: March 31, 2012 Course Revised: May, 2018 Course Expires: May 31, 2021 Reproduction and distribution of these materials is prohibited
a unit of Dr Bharat S Mody Director Chief Arthroplasty Surgeon Centre for Knee & Hip Surgery Dr Pankaj Patni Orthopaedic Surgeon Dr Sunil Dewangan
 Centre for Knee & Hip Surgery Arthroscopy a unit of Arthroplasty Dr Bharat S Mody Director Chief Arthroplasty Surgeon Dr Sunil Dewangan Dr Prakash Tekwani Dr Rahul Khanna Dr Pankaj Patni Orthopaedic Surgeon
Centre for Knee & Hip Surgery Arthroscopy a unit of Arthroplasty Dr Bharat S Mody Director Chief Arthroplasty Surgeon Dr Sunil Dewangan Dr Prakash Tekwani Dr Rahul Khanna Dr Pankaj Patni Orthopaedic Surgeon
Vesalius SCALpel : Coagulation. Coagulation
 Vesalius SCALpel : Coagulation Coagulation Clotting tests injury attracts platelets chemoattractants: platelet derived growth factor (PDGF), transforming growth factor beta (TGF beta) platelets release
Vesalius SCALpel : Coagulation Coagulation Clotting tests injury attracts platelets chemoattractants: platelet derived growth factor (PDGF), transforming growth factor beta (TGF beta) platelets release
Cardiovascular (connective tissue)
 Cardiovascular (connective tissue) Blood Connective tissue Blood Proteins 7% Plasma 55% Other solutes 2% Water 91% Erythrocytes ~5.2 million per cubic mm Formed elements 45% Leukocytes ~7 thousand per
Cardiovascular (connective tissue) Blood Connective tissue Blood Proteins 7% Plasma 55% Other solutes 2% Water 91% Erythrocytes ~5.2 million per cubic mm Formed elements 45% Leukocytes ~7 thousand per
ISIS PHARMACEUTICALS. ISIS-FXI Rx Program Update. Webcast December 8, 2014
 ISIS PHARMACEUTICALS ISIS-FXI Rx Program Update Webcast December 8, 2014 Introduction Stan Crooke, M.D., Ph.D. CEO and Chairman, Isis Pharmaceuticals 2 Forward Looking Language Statement This presentation
ISIS PHARMACEUTICALS ISIS-FXI Rx Program Update Webcast December 8, 2014 Introduction Stan Crooke, M.D., Ph.D. CEO and Chairman, Isis Pharmaceuticals 2 Forward Looking Language Statement This presentation
Primary hemostasis. Vascular endothelium Vasoconstriction : local tissue factor, nervous system
 Primary hemostasis Vascular endothelium Vasoconstriction : local tissue factor, nervous system Platelet Plug Platelet Adhesion Platelet Activation Platelet Aggregation Platelet Plug Formation Secondary
Primary hemostasis Vascular endothelium Vasoconstriction : local tissue factor, nervous system Platelet Plug Platelet Adhesion Platelet Activation Platelet Aggregation Platelet Plug Formation Secondary
Apheresis Anticoagulant Removal. Oluwatoyosi Onwuemene, MD MS May 6th, 2017
 Apheresis Anticoagulant Removal Oluwatoyosi Onwuemene, MD MS May 6th, 2017 Talk Outline Case presentation Factors associated with drug removal TPE s effects on hematologic parameters Anticoagulant properties
Apheresis Anticoagulant Removal Oluwatoyosi Onwuemene, MD MS May 6th, 2017 Talk Outline Case presentation Factors associated with drug removal TPE s effects on hematologic parameters Anticoagulant properties
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Commercial, HIM-Medical Benefit, Medicaid Coding Implications Revision Log See
Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 05.01.16 Last Review Date: 02.19 Line of Business: Commercial, HIM-Medical Benefit, Medicaid Coding Implications Revision Log See
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 07.01.18 Last Review Date: 02.18 Line of Business: Oregon Health Plan Coding Implications Revision Log See Important Reminder at
Clinical Policy: (Arixtra) Reference Number: CP.PHAR.226 Effective Date: 07.01.18 Last Review Date: 02.18 Line of Business: Oregon Health Plan Coding Implications Revision Log See Important Reminder at
Hemostasis. by Mohie-Aldien Elsayed
 Hemostasis by Mohie-Aldien Elsayed Hemostasis Hemostasis is defined as the process that maintains the flowing blood in a fluid state and confined to the circulatory system Coagulation prevents excess blood
Hemostasis by Mohie-Aldien Elsayed Hemostasis Hemostasis is defined as the process that maintains the flowing blood in a fluid state and confined to the circulatory system Coagulation prevents excess blood
Manejo de la transfusión de plaquetas. Ileana López-Plaza, MD
 Manejo de la transfusión de plaquetas Ileana López-Plaza, MD Thrombocytopenia Common in ICU setting 25-38% with< 100,000/µL 2-3 % with < 10,000/µL Common etiologies Drug-induced: heparin, antibiotics,
Manejo de la transfusión de plaquetas Ileana López-Plaza, MD Thrombocytopenia Common in ICU setting 25-38% with< 100,000/µL 2-3 % with < 10,000/µL Common etiologies Drug-induced: heparin, antibiotics,
Heparin Induced Thrombocytopenia
 Screen Heparin Induced Thrombocytopenia This course has been awarded one (1) contact hour. This course expires on September 30, 2018. Copyright 2007 by RN.com. All Rights Reserved. Reproduction and distribution
Screen Heparin Induced Thrombocytopenia This course has been awarded one (1) contact hour. This course expires on September 30, 2018. Copyright 2007 by RN.com. All Rights Reserved. Reproduction and distribution
General News. Product Notes
 TO: HELENA POC DISTRIBUTORS FROM: HELENA POINT OF CARE SUBJECT: ROUND-UP/INTERNATIONAL DATE: 8/31/2009 ATTN: ROUNDUP READERS CLINICAL TRIAL SITES NEEDED! As Helena POC continues development of Cascade
TO: HELENA POC DISTRIBUTORS FROM: HELENA POINT OF CARE SUBJECT: ROUND-UP/INTERNATIONAL DATE: 8/31/2009 ATTN: ROUNDUP READERS CLINICAL TRIAL SITES NEEDED! As Helena POC continues development of Cascade
Clinical Policy Guidelines. Management of patients on antithrombotic agents undergoing colonoscopy procedure following positive FOB test.
 NHS GREATER GLASGOW AND CLYDE BOWEL SCREENING PROGRAMME Clinical Policy Guidelines Management of patients on antithrombotic agents undergoing colonoscopy procedure following positive FOB test. Date to
NHS GREATER GLASGOW AND CLYDE BOWEL SCREENING PROGRAMME Clinical Policy Guidelines Management of patients on antithrombotic agents undergoing colonoscopy procedure following positive FOB test. Date to
Hemostasis and Thrombosis
 Hemostasis Hemostasis and Thrombosis Normal hemostasis is a consequence of tightly regulated processes that maintain blood in a fluid state in normal vessels, yet also permit the rapid formation of a hemostatic
Hemostasis Hemostasis and Thrombosis Normal hemostasis is a consequence of tightly regulated processes that maintain blood in a fluid state in normal vessels, yet also permit the rapid formation of a hemostatic
Blood is 55% Plasma (Liquid)
 Blood is 55% Plasma (Liquid) The plasma portion of blood is: 91% Water Maintains blood volume Transports molecules 7% Proteins (ie: clotting proteins, albumin, immunoglobulins ) 2 % Salts, gases (O 2,
Blood is 55% Plasma (Liquid) The plasma portion of blood is: 91% Water Maintains blood volume Transports molecules 7% Proteins (ie: clotting proteins, albumin, immunoglobulins ) 2 % Salts, gases (O 2,
DOAC s and Implications on Laboratory Results. Kandice Kottke-Marchant, MD, PhD Cleveland Clinic
 DOAC s and Implications on Laboratory Results Kandice Kottke-Marchant, MD, PhD Cleveland Clinic Anticoagulants Heparin Low Molecular Weight Heparins enoxaparin, fragmin Heparin pentasaccharide - fondaparinux
DOAC s and Implications on Laboratory Results Kandice Kottke-Marchant, MD, PhD Cleveland Clinic Anticoagulants Heparin Low Molecular Weight Heparins enoxaparin, fragmin Heparin pentasaccharide - fondaparinux
Scottish Medicines Consortium
 Scottish Medicines Consortium fondaparinux, 2.5mg/0.5ml, solution for injection (Arixtra ) No. (287/06) GlaxoSmithKline 7 July 2006 The Scottish Medicines Consortium has completed its assessment of the
Scottish Medicines Consortium fondaparinux, 2.5mg/0.5ml, solution for injection (Arixtra ) No. (287/06) GlaxoSmithKline 7 July 2006 The Scottish Medicines Consortium has completed its assessment of the
Disclaimer: this is a very big topic and coverage will be only superficial.
 Vascular Biology 4 Blood and its components: 1 Disclaimer: this is a very big topic and coverage will be only superficial. 1. Erythrocytes: eat your spinach (or steak). ~8 um diameter, 2 um thickness no
Vascular Biology 4 Blood and its components: 1 Disclaimer: this is a very big topic and coverage will be only superficial. 1. Erythrocytes: eat your spinach (or steak). ~8 um diameter, 2 um thickness no
Clexane pre-filled syringes 150mg/ml in syringe sizes equating to the following doses: 120mg and 150mg. Page 1 of 8
 Low Molecular Weight Heparins (LMWH) Shared Care Guideline for the use of Enoxaparin and Dalteparin in the Treatment and Prophylaxis of Venous Thromboembolism Introduction Low Molecular Weight Heparins
Low Molecular Weight Heparins (LMWH) Shared Care Guideline for the use of Enoxaparin and Dalteparin in the Treatment and Prophylaxis of Venous Thromboembolism Introduction Low Molecular Weight Heparins
Marcia L. Zucker, Ph.D. ZIVD LLC
 Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway X II Xa LMWH & DXaI IIa (thrombin) Hirudin
Marcia L. Zucker, Ph.D. ZIVD LLC 1 Monitoring hemostasis Bleeding Clotting 2 3 Extrinsic Pathway Monitor with ACT / aptt WARFARIN Monitor with PT Common Pathway X II Xa LMWH & DXaI IIa (thrombin) Hirudin
General News. Product Notes. Instrument Notice HELENA SALES FORCE TO: FROM: SUBJECT: HELENA POINT OF CARE ROUND-UP/US DOMESTIC DATE: 9/1/2009
 TO: FROM: SUBJECT: HELENA SALES FORCE DATE: 9/1/2009 General News HELENA POINT OF CARE ROUND-UP/US DOMESTIC We have concluded a very large meeting with the AACC in Chicago. The leads have been processed
TO: FROM: SUBJECT: HELENA SALES FORCE DATE: 9/1/2009 General News HELENA POINT OF CARE ROUND-UP/US DOMESTIC We have concluded a very large meeting with the AACC in Chicago. The leads have been processed
10/8/2013. Drug-induced immune thrombocytopenia (DITP) Clinical aspects
 Richard Aster, MD Blood Center of Wisconsin, Blood Research Institute, Milwaukee, WI Senior Investigator Medical College of Wisconsin Professor, Departments of Medicine & Pathology Drug-induced immune
Richard Aster, MD Blood Center of Wisconsin, Blood Research Institute, Milwaukee, WI Senior Investigator Medical College of Wisconsin Professor, Departments of Medicine & Pathology Drug-induced immune
Marcia L. Zucker, Ph.D. ZIVD LLC
 Marcia L. Zucker, Ph.D. ZIVD LLC 1 Explain why ACTs from different systems are not the same Develop a plan for switching from one ACT system to another Describe why ACT and aptt are not interchangeable
Marcia L. Zucker, Ph.D. ZIVD LLC 1 Explain why ACTs from different systems are not the same Develop a plan for switching from one ACT system to another Describe why ACT and aptt are not interchangeable
Bleeding Emergencies. Gregory W. Hendey, MD, FACEP Professor of Clinical Emergency Medicine UCSF Fresno
 Bleeding Emergencies Gregory W. Hendey, MD, FACEP Professor of Clinical Emergency Medicine UCSF Fresno Objectives To discuss indications and agents used for reversal of coagulopathy To apply those principles
Bleeding Emergencies Gregory W. Hendey, MD, FACEP Professor of Clinical Emergency Medicine UCSF Fresno Objectives To discuss indications and agents used for reversal of coagulopathy To apply those principles
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs
 Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
Factor Concentrates. More is better? Alexander Duncan MD Emory Medical Labs Call from OR! Scenario -1 Patients is bleeding out! Don t ask why, what rate what s been done! We need blood now! What kind of
LVHN Scholarly Works. Lehigh Valley Health Network. Joseph G. Ottinger RPh, MS, MBA, BCPS Lehigh Valley Health Network,
 Lehigh Valley Health Network LVHN Scholarly Works Department of Pharmacy Retrospective Evaluation of Delayed Administration of Fondaparinux in Providing Comparable Safety and Efficacy Outcomes in Patients
Lehigh Valley Health Network LVHN Scholarly Works Department of Pharmacy Retrospective Evaluation of Delayed Administration of Fondaparinux in Providing Comparable Safety and Efficacy Outcomes in Patients
HIBOR. 1st Prophilaxis. Acute phase treatment. Pentasaccharide. Long-term 2ª ACOs UFH LMWH LMWH LMWH. Competitors
 HIBOR Competitors 1st Prophilaxis LMWH Pentasaccharide Long-term Profilaxis treatment 2ª ACOs LMWH Acute phase treatment UFH LMWH Unfractionated heparin (UFH) Discovered by J. Mc Lean in 1916. Later named
HIBOR Competitors 1st Prophilaxis LMWH Pentasaccharide Long-term Profilaxis treatment 2ª ACOs LMWH Acute phase treatment UFH LMWH Unfractionated heparin (UFH) Discovered by J. Mc Lean in 1916. Later named
THE MICHELANGELO OASIS 5 PROGRAM. MichelAngelo : The Creation of Man (Fragment of the Sistine Chapel ceiling- Detail) ( )
 THE MICHELANGELO OASIS 5 PROGRAM MichelAngelo : The Creation of Man (Fragment of the Sistine Chapel ceiling- Detail) (1511-12) Key Steps in Coagulation Pathway Intrinsic pathway Extrinsic pathway 1 Xa
THE MICHELANGELO OASIS 5 PROGRAM MichelAngelo : The Creation of Man (Fragment of the Sistine Chapel ceiling- Detail) (1511-12) Key Steps in Coagulation Pathway Intrinsic pathway Extrinsic pathway 1 Xa
In Hospital Bleeding Management
 In Hospital Bleeding Management Geno J Merli, MD, MACP, FSVM, FHM Professor Medicine & Surgery Co-Director Jefferson Vascular Center Sidney Kimmel Medical College Thomas Jefferson University Hospitals
In Hospital Bleeding Management Geno J Merli, MD, MACP, FSVM, FHM Professor Medicine & Surgery Co-Director Jefferson Vascular Center Sidney Kimmel Medical College Thomas Jefferson University Hospitals
Princess Alexandra Hospital Emergency Department. Clinical Procedure. 1 Introduction
 Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
Princess Alexandra Hospital Emergency Department Clinical Procedure Trauma, Resuscitation Review Officer: Glenn Ryan 1 Introduction Version no: 1 Approval Date: 16/07/2014 Review Date: 16/07/2016 Authority:
